Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
Does your tooth need a root canal? – Signs & Symptoms
Signs and symptoms that suggest your tooth needs root canal treatment.
With most endodontic cases, there is typically some subtle hint or even a clear sign signaling the need for attention in advance.
- Some of these are common signs and symptoms that individuals experiencing endodontic problems typically notice.
- Others are clinical signs that dentists are trained to recognize but may go unnoticed by patients without guidance on what to look for.
For your knowledge, we’ve created this guide that outlines signs and symptoms you should be able to identify when problems are brewing. And if you do discover something, don’t delay in reporting it to your dentist so they can fully evaluate your situation and make a proper diagnosis.
That’s important to ensure your tooth receives the treatment it requires and before complications arise. In the event that assistance is unavailable, this guide also provides some self-help remedies you might try
Signs and symptoms of needing root canal treatment.
Symptoms you have noticed. What to look for. – It’s frequently the presence of pain, or signs of infection and/or swelling, that first signal to a person that their tooth has a problem.
Your dentist will quiz you about the symptoms you’ve noticed: Type, location, onset, triggers, duration, and what if anything provides relief. Their evaluation will then involve trying to confirm, and possibly even reproduce, what you report.
Clinical signs possibly only obvious to your dentist. What they look for. – Some teeth seem to give little indication that there’s a problem within their nerve space. But to the trained eye, they may be displaying subtle signs that hint that a problem likely exists.
These tip-offs include things like: Individually darkened teeth, evidence of infection or drainage from it, and soft tissue changes.
FYI: Additional testing will be needed. – Once the signs you have noticed have been investigated by your dentists, and possibly confirmed by things they know to look for, further evaluation will be needed. This includes:
- Radiographic evaluation - Root canal signs on X-rays.
- Additional clinical testing - What kinds of tests?
FYI – Since performing endodontic therapy is the needed solution for such a wide variety of problems (acutely inflamed teeth, teeth with dying or dead nerve tissue, cracked teeth, failed initial root canal treatment, etc…), there isn’t just a single set of symptoms that appears in every case where it’s needed.
It’s only after sorting through all of the bits of information they’ve collected, from all available sources, that your dentist can then determine if a root canal, or possibly an entirely different dental procedure, seems to be the appropriate solution.
In some cases, the data that’s been collected may be inconclusive or even conflicting. If so, the patient may need to wait and be reassessed at a later time, or be referred to a specialist endodontist for evaluation.
I) Signs and symptoms that you (the patient) may notice.
Having a toothache or noticing swelling are the most common signs that will first tip off a person that their tooth has an endodontic problem. However, exactly what is experienced will vary greatly, both among cases and during an individual case’s timeline.
Dental abscess.
The set of symptoms that are probably most associated and most feared by patients as a sign that root canal treatment is needed for their tooth are those that occur during an acute tooth flare-up. (In dental terms, referred to as an “acute apical abscess.”)
Acute apical abscess signs and symptoms –
In full form, this condition is characterized by:
- A quick onset.
- Spontaneous pain – pain that occurs on its own, unprovoked.
- Extreme tenderness of the tooth to pressure – like when biting or tapping on it.
- Swelling of associated soft tissues – a sign of the spread of pus from the tooth’s infection.
Despite what a person might fear or be inclined to expect, with many if not most cases, just one or a few of the above symptoms will be experienced. And possibly then, only vaguely.
Also, with some cases, additional or even entirely different signs may be the ones noticed. That’s because what exactly a person does experience will simply depend on the state of pathology that currently exists with the tooth’s nerve/nerve space, and that can be quite varied.
For our discussion about what types of signs or symptoms might be noticed, we’ve addressed each category individually.
a) Pain.
Having a toothache isn’t always one of the first signs that a person notices when their tooth requires root canal therapy. Some teeth that require it never hurt at all. With others, they may hurt for a while and then inexplicably settle down.
But when a cause-and-effect relationship exists between the two, one or more of the following scenarios typically plays out.
Type of pain.
- The discomfort can range from sharp and intense to a dull ache. Its level may range from slight to extreme.
Characteristically:
- The pain may include a throbbing component (feels like it has its own heartbeat).
- Its character may change (lessen or intensify) as you change your posture (stand up, bend over, lie down, etc…).
- The discomfort may be severe enough that it wakes you when sleeping.
Onset and duration.
- Depending on how long the underlying condition has existed, some level of discomfort may have presented itself intermittently before (previous days, weeks, months). In other cases, this will be the person’s first painful experience.
Characteristically:
- The pain may be spontaneous (hurts on its own, unprovoked) or only triggered in response to a stimulus.
- In cases where the pain is spontaneous, it may be intermittent or continuous.
- If a triggering event is involved, it may be: Chewing or biting pressure, the pressure of pressing or tapping on the tooth, thermal insult (like exposure to hot or cold foods and beverages), or sweets.
Once the triggering stimulus has been removed, rather than disappearing immediately the discomfort frequently lingers (often for 30 seconds or longer). It may then finally fade away, or continue for an extended period of time.
In some cases, heat application will bother the culprit tooth, and cold liquids or ice will settle it down. (Ice application is sometimes used by patients to provide temporary relief.)
- It’s common that over-the-counter analgesics (pain relievers) are ineffective in controlling the pain.
Location.
- It may be quite easy for the patient to identify which tooth hurts. At other times the discomfort may be vague and nondescript.
Characteristically:
- The person may be able to tell which general area is painful but not which tooth.
- The pain may be referred, meaning that the tooth or area that hurts the most is not the one that is the actual source of the problem.
▲ Section references – Germain, Iqbal, Bender
Remember, pain isn’t always a sign that a root canal is needed.
While each of the above scenarios may be an indication that endodontic treatment is needed, there simply isn’t a single set of signs that appear in every case that foretells for sure that it is. In fact, many of the symptoms above can also be an indication of more benign tooth conditions.
Beyond just quizzing you about what you have experienced, your dentist may also try to reproduce events that trigger your discomfort so they can evaluate what you are experiencing firsthand. (See the “testing” section below.)
Even then, while they may have formed a strong opinion about your tooth’s condition, they’ll still wait until they have collected other information before making a final diagnosis.
So, if you experience some type of pain, be concerned and proceed with seeking assistance. But in regard to it absolutely being a sign that a root canal procedure must be performed, there can be other explanations.
Other dental conditions that may cause a toothache.
As a part of their differential diagnosis, your dentist will consider additional conditions that may be the cause of your tooth’s discomfort. They can include:
- Tooth decay, tooth fracture, a cracked tooth, a defective, deep, extensive or new dental restoration, sinus infection, tooth clenching and grinding (bruxism), periodontal (gum) disease, exposed dentin.
If any of these are identified, the dentist will likely initiate treatment aimed at both managing that problem and helping the irritated tooth to settle down. If it doesn’t respond positively, or if reevaluation at a later date identifies the need, performing a root canal procedure may still be required.
b) Gum tenderness, swelling, infection.
With some endodontic cases, the inside of the tooth has become colonized by bacteria. And a symptom of the presence of this infection can be soft tissue swelling in the region of the tooth.
Swelling doesn’t occur in every case where root canal treatment is needed. But when it does, it typically displays one or more of the following characteristics.
Amount of swelling.
- Comparatively minor amounts (swollen gums) – In these cases, the swelling you notice will be inside your mouth, in the soft tissues directly adjacent to your tooth. Besides being enlarged, the tissues will typically have a reddish coloration and be tender to the touch.
- Larger amounts (swollen face) – More extensive swelling can extend into the face and neck.
a) The swelling may take the form of a localized, reddened, pus-filled bump.

A tooth abscess with localized facial swelling.
b) Or may involve a large expanse of diffuse swelling that causes noticeable facial or neck fullness.

A dental abscess that has caused diffuse facial swelling.
Location.
- Usually, there’s a general relationship between the location of the swelling and the culprit tooth. Although, it’s possible for pus/swelling to travel or extend some distance from the source of its infection. The swelling will occur on the same side of your body as the infected tooth.
Characteristically:
- With intraoral (inside the mouth) swelling that’s relatively minor and localized, the area of enlargement usually lies at a level that approximates the tip of the problem tooth’s root.
- Instead of pronounced swelling, a pimple-like drain for pus may form on your gums (a “gum boil”). We discuss this phenomenon more fully below.
Onset.
While nothing here is uniquely informative:
- The swelling may come and go as days, weeks or even months pass, possibly never disappearing completely.
- It may have presented itself for the first time, with a slow or rapid onset.
Associated symptoms.
- Swelling may be but isn’t always accompanied by the presence of pain. (The pressure associated with the buildup of pus is often what is causing the person’s tooth pain.)
- The area of swelling is characteristically tender to palpation (touch).
- Lymph nodes (like in your neck or under your jaw, on the same side as the infected tooth) may be enlarged or tender.
- If the pus causing the swelling finds a way to vent off (drain), you may notice a bad taste in your mouth. Draining pus can also be the source of foul breath odor.
Characteristically:
- It’s possible that due to infection the tooth feels slightly elevated. (Seems as though it’s been pushed out of its socket some and is taller than its neighboring teeth.)
- To a minor extent, the tooth may also feel slightly more mobile than previously.
▲ Section references – Tronstad
Swelling isn’t always a sign that root canal treatment is needed.
Experiencing swelling doesn’t necessarily mean that you have a tooth that needs endodontic therapy but it does indicate that something is wrong somewhere and its presence should be taken seriously. (While rare, in extreme cases it can become so pronounced as to interfere with your ability to breathe.)
It’s a simple matter to contact your dentist’s office and report what you have experienced. They can then make a decision about what level of attention you require.
When swelling is present a dentist will frequently have their patient start a regimen of oral antibiotics. Since they typically take about 24 hours to have an effect, when you call your dentist even if they don’t feel that you need immediate examination, they may go ahead and prescribe antibiotics for you so you can get started with them.
Ways to distinguish the likely source of your swelling.
In cases where an area of tenderness and swelling is fairly small, the following rules of thumb tend to apply.
- If caused by periodontal (gum) issues, the area is often located alongside the tooth or right at its gum line.
- When caused by an infection inside a tooth, it’s often centered in the region that approximates the tooth’s root tip.
Other dental conditions that may cause swelling.
Your dentist will consider other possible sources of infection during their examination. They can include:
- Periodontal (gum) disease, pericoronitis (most commonly associated with erupting wisdom teeth.
Whatever the source, a dentist will first take steps to manage the swelling so it doesn’t get out of hand. Then at a later point diagnose the actual underlying problem and determine what treatment is required to resolve it.
c) Additional signs.
Malaise (a general feeling of illness or uneasiness) or even fever are possible symptoms that may present themselves when a person has a tooth that requires endodontic therapy.
However, these symptoms on their own are generally considered to be just secondary in nature. (They provide no information about which tooth lies at fault or the underlying nature of its condition.) Other signs will be weighed much more heavily by your dentist when formulating their diagnosis.
d) Frequency and duration of symptoms.
It bears repeating that the nature of any of the signs and symptoms discussed above may change over time. If so, they may either be:
- Transient – Meaning what’s noticed comes and goes on an hour-by-hour, day-to-day, month-to-month basis, or any frequency in between.
- Persistent and continual. – In this case, while possibly not always especially noticeable or intense, the symptoms never totally subside or disappear.
As a partial explanation, symptoms caused by infected teeth frequently wax and wane due to the current level of infection activity.
So now you know. What you may experience can be incredibly varied.
By this point on this page, it should be apparent to you why a dentist’s level of experience and knowledge is so important in their being able to accurately diagnose their patient’s condition.
The range and degree of symptoms possible with root canal cases are so varied and great that there’s nothing simple about interpreting them.
To recap some examples, all of which are resolved via the exact same treatment process (performing root canal treatment):
- With low-grade chronic (long-existing) conditions, the patient may experience essentially no symptoms at all.
- At the other extreme, with acute apical abscess cases, rapid onset, spontaneous (possibly severe) pain, pronounced tissue swelling, and extreme sensitivity to pressure (tapping or biting on the tooth) are all likely to be experienced.
- And of course with all other endodontic cases, what’s experienced can be essentially anything in between.
So if you do notice the kinds of symptoms discussed above, you don’t necessarily have to assume the worst. But they are an indication that your most prudent move is to be checked out by your dentist promptly.
II) Clinical signs of needing a root canal that may only be obvious to your dentist.
Unlike acute flare-ups (acute tooth abscesses) like described above, the deterioration and even ultimate death of a tooth’s pulp tissue (nerve) isn’t always a big event. For example,
- It’s possible and even common for this process to occur without producing any noticeable symptoms at all.
- Or, it may be that the original events surrounding the nerve’s demise may have been so mild, or taken place so long ago, that they’re not remembered.
In either of these situations, it may take your dentist’s keen eye during their clinical examination to discover that unbeknownst to you, your tooth requires endodontic therapy. Here are some of the ways they tell.
a) Minor signs of swelling or inflammation.
Your dentist will look for signs of infection you may have not noticed. The inspection method they’ll use is termed “palpation,” which simply means examination by touch.
Signs you might have overlooked can include areas of tenderness, hardness, fluctuation (fluid-filled tissues), crepitation (areas that make a crackling noise when pressed), and slight tissue enlargement.
They’ll use their fingers and feel alongside the tooth in question. And compare what they feel, and your response to it, to areas involving neighboring teeth or even the same area on the other side of your mouth.
Characteristically, any signs they discover will likely be centered at a level approximating the tip of your problematic tooth’s root. (The point where the infection would be leaking out.)
▲ Section references – Tronstad
b) Recurring or persistent gum boils.
The presence of an infection inside a tooth can result in the formation of a pimple-like bump on the person’s gum tissue. These are frequently found in association with chronic (long-standing) tooth infections but one may form following an acute episode (swelling flare-up) too.
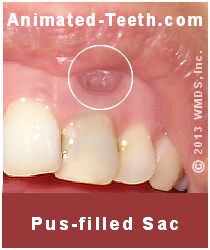
The surface opening of a sinus tract.
Patients often refer to these lesions as “gum boils.” Dentists sometimes use the term “fistulous tracts” but most accurately they are referred to as “sinus tracts.”
Why do they form?
These lesions are literally drains for pus. Instead of it building up inside the bone tissue around your tooth’s root, or in adjacent soft tissues, the tract provides a way for it to vent off totally (into your mouth).
We’ve dedicated an entire page to this topic. You can find it here: What are sinus tracts? Pictures | Diagrams
▲ Section references – Tronstad
A gum boil may go unnoticed.
In cases where the infection inside a tooth remains low-grade, the boil will tend to be small and only have minimal taste coming from it. If so, it’s possible for a person to be totally unaware that it’s there.
Other dental conditions that may result in a sinus tract.
This type of lesion is proof positive that a problem exists but not necessarily that root canal treatment is the needed solution. For example, it’s possible that the source of the infection is a periodontal (gum disease) issue.
c) Individually darkened teeth.
A tooth that’s darker than its neighbors typically indicates that its dental pulp (nerve tissue) has undergone some type of degenerative change.
And it’s often the case, but not always, that these changes have led to a situation where root canal treatment is now needed.
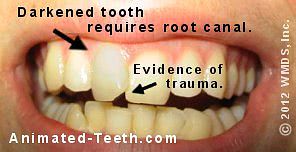
The dark color of this tooth suggests that it needs treatment.
This type of color mismatch is frequently the sole reason why a dentist will suspect that a tooth has a problem and requires root canal therapy.
Things to know.
- Having this phenomenon develop is fairly common with teeth that have experienced some type of traumatic event, like being banged up in an accident (traffic collision, contact sport incident, etc…).
- The change may not manifest itself until some years (even a decade or more) after the original event occurred.
- When it occurs, the tooth may take on a dark yellow, gray, or even black tint. The degree of darkening may be severe or just slight. (Here’s why the darkening occurs. Pictures | Diagrams)
- This process frequently takes place without causing any associated symptoms (pain or swelling).
▲ Section references – Ingle
Tooth discoloration doesn’t always mean that a root canal is needed.
This is, yet again, another sign that by itself does not necessarily mean that root canal therapy is required.
- This same type of discoloration may take place with teeth that have already had successful endodontic treatment. Or it may indicate that some pulp chamber (nerve-space) changes have occurred but at this point no attention is necessary.
- In other instances, the discoloration may be due to the presence of decay, a deteriorated filling, or staining caused by a metal filling.
The color mismatch will remain.
Even after root canal therapy has been completed, the tooth’s staining will remain.
- If after the completion of the tooth’s treatment it requires a dental crown What decides?, then the placement of that restoration can be used to remedy the color mismatch.
- If not, then whitening treatments tooth bleaching may be able to provide a suitable solution.
d) Tooth mobility.
Teeth that have pulpal pathology may display increased mobility (tooth looseness). But considering this issue alone usually isn’t enough to arrive at a valid diagnosis. That’s because other tooth conditions (gum disease, adaptation to the pressure of teeth grinding) can cause increased mobility too.
In making a distinction, if only one tooth seems loose, the cause may be an endodontic one. But if multiple teeth are involved, other causes are more likely involved.
e) Exposure of the tooth’s nerve.
Performing a tooth’s dental procedure sometimes results in an exposure of its nerve. The term “exposure” means that the dentist’s work has made direct contact with the tooth’s pulp chamber and therefore its nerve tissue.

If nerve exposure occurs, endodontic therapy may be needed.
- It’s your dentist’s obligation to notify you that this event has occurred. (Since local anesthesia has been used to numb up your tooth for its procedure, you probably won’t feel the exposure when it happens.)
- They’ll also need to explain whether your tooth requires root canal therapy immediately or if a wait-and-see approach is more appropriate.
With the latter, it’s important to remember what the dentist reported. If your tooth becomes symptomatic later, knowing about the exposure will provide vital information for the dentist diagnosing your situation.
What’s the nerve’s outlook after an exposure has occurred?
With healthy nerves.
The occurrence of the exposure and its associated events may be enough to trigger pulp tissue degeneration and the tooth’s ultimate need for root canal treatment. However, in situations where the tooth’s pulp tissue was healthy at the time of the exposure, the success of a repair made by your dentist may approach 90%. (Tronstad)
With inflamed nerve tissue.
A tooth’s potential for recovery is greatly reduced if its pulp tissue is already inflamed at the time of the exposure (falling to a 30 to 40% chance of success). Unfortunately, this is the usual status of teeth having advanced tooth decay. (Tronstad)
Treatment.
Based on the dentist’s interpretation of the pulp’s status (a factor they can never be 100% certain of because pulpal inflammation is typically asymptomatic), if an exposure has occurred they may feel they must advise their patient that it’s best to go ahead and plan to perform root canal treatment now (a judgment call on their part), so to avoid complications later on. (Such as the patient experiencing a painful tooth abscess, or the tooth’s root canal system undergoing calcification and as a result becoming more difficult to treat).
An attempt at repair can be made via a procedure termed “pulp capping.” It involves:
- Placing a dressing (frequently a layer of calcium hydroxide paste) over the area of the nerve tissue exposure. The tooth’s restoration is then completed.
- The patient may be instructed to take an NSAID medication such as ibuprofen (Avil, Motrin. (Each of these are readily available over-the-counter pain medications.)
NSAIDs (non-steroidal anti-inflammatory drugs) help to limit the nerve tissue’s inflammation reaction to the injury, which can aid in its recovery.
- The tooth’s status must then be monitored periodically for some years following (like during routine dental checkups). The monitoring will need to include an X-ray examination.
Case failures may be diagnosed 2 to 3, or even more, years after the initial event. (Tronstad) Upon that diagnosis, endodontic therapy must be performed to salvage the tooth.
▲ Section references – Tronstad
Pulp tissue exposures may be planned or unplanned.
a) Unplanned
In most cases, an exposure is an unavoidable, undesired side effect that has occurred as a dentist attempts to repair a cavity. Often, one that ideally should have been treated months or years previously.
b) Planned
In a minority of cases (most of which probably involve dental crown or bridge placement), the exposure may be anticipated due to the amount of tooth structure (dentin and enamel) that’s expected to need to be trimmed away to accommodate the new dental work.
Of these two scenarios, the “unplanned” one is the case where pulp tissue inflammation is more likely not to be an issue, and therefore the success of making a repair is more likely. But whether pulp capping or immediately proceeding with root canal treatment makes the better plan, would simply be a judgment call made by the dentist.
What should you do if you suspect that your tooth needs root canal therapy?
Don’t delay.
If you notice any of the signs and symptoms mentioned on this page, you should establish contact with your dentist’s office and make arrangements to be evaluated and receive treatment in a time frame that they determine is warranted.
Teeth that do require endodontic therapy can be unpredictable, with the consequences of a flare-up (pain, swelling, etc…) possibly being severe.
Don’t make assumptions.
Making a misdiagnosis about their tooth’s status (by way of using website information like this) may deter some people from seeking treatment during that stage when another (simpler, cheaper, and easier) repair might have been possible.
That’s because some people won’t seek treatment promptly if in their mind they think it’s already too late, will cost too much money, or else the idea of having a root canal is too unnerving for them.
Don’t make this mistake. If you have a tooth that’s displaying symptoms, have your dentist evaluate it sooner rather than later. Doing so may make a big difference in what you experience, what type of treatment you require, and its total cost.
If root canal treatment is needed …
In the case where you do have a tooth that seemingly requires endodontic therapy, there’s not a lot, unfortunately, that you can do on your own.
The following video explains what takes place during root canal treatment. It should be obvious to anyone that only a dentist can provide this type of service, so be in touch with yours promptly.
Section highlights as a video –
Note: Dental-Picture-Show’s content and videos have now been absorbed into Animated-Teeth.com.
Self-help measures for root canal pain.
Things you might try …
In the case where you find yourself on your own for a while (can’t make contact with your dentist), there are some things you can try to help to alleviate your symptoms, at least to some degree.
Take it easy with your tooth.
It only makes sense to discontinue any activities that tend to set your tooth off (biting on it, exposing it to hot or cold foods and beverages, etc…).
An OTC pain reliever may help you feel better.
Within the guidelines of the product you choose, you may find that using an over-the-counter pain reliever provides some degree of relief. Ibuprofen (Motrin, Advil) or other NSAIDs (non-steroidal anti-inflammatory drugs) are frequently recommended by dentists for pain control. However, in severe cases, OTC medications are typically found to be ineffective.
Only use medications as directed by their instructions.
As an example of what we mean, placing an aspirin on the gums next to your tooth is ill-advised. An aspirin pill (acetylsalicylic acid) is intended to be a systemic drug (absorbed internally after being swallowed), not a topical one (absorbed through the skin). Placing an aspirin next to your tooth will be ineffective in controlling your tooth’s pain and will cause a chemical burn on your gum tissue.
Try to make contact with your dentist.
Since all dentists know that emergencies do happen, they’ve probably made some type of plan for when their patients experience them. You should call your dentist’s office to see if there’s a message describing the type of assistance they have to offer.
Even just telephone contact with your dentist can be of help.
Sometimes being placed on an antibiotic (and sooner rather than later) can be a big help in limiting what you have to endure. And although a prescription is required, just a phone call to your dentist may be enough to get the ball rolling toward your obtaining one. Since it may take a day or two for the antibiotic to start to produce an effect, your dentist may prescribe a prescription pain reliever for you too.
Similarly, a physician at an emergency-care facility could initiate this same interim plan.
Home remedy: Try placing ice on your tooth.
In some cases where root canal therapy is needed, during that stage when a tooth has started to produce extended periods of constant pain, chilling it by way of holding a chip of ice, or cold liquid (ice water), against it may provide relief.
This won’t work in all cases and, in fact, may irritate your tooth in some. So, ease into this remedy with testing. But when this solution does work, it can provide much-needed relief until you can receive the treatment you require from your dentist.
FYI – It’s not uncommon for a dentist to have a patient arrive for emergency treatment who has with them a mug of ice water from which they sip at regular intervals so to keep their pain away.
While the dentist must do testing to confirm their suspicions, when seen, this scenario is almost diagnostic of the patient’s tooth’s need for root canal therapy.
In cases where this home remedy works, it’s because the chilling effect of the ice lowers the pain-causing pressure inside the tooth’s nerve space by way of contracting the gases and liquids it contains.
What’s next?
We have more to share about needing a root canal.
Last reviewed: January 18, 2025
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Bender IB. Pulpal Pain Diagnosis— A Review.
Germain L. Differential diagnosis of toothache pain. Part I, odontogenic etiologies.
Ingle JI, et al. Ingle’s Endodontics. Chapter: Periapical Lesions of Endodontic Origin.
Iqbal M, et al. An Investigation Into Differential Diagnosis of Pulp and Periapical Pain: A PennEndo Database Study.
Tronstad L. Clinical Endodontics. Chapter: Oral and Perioral Pain of Endodontic Interest.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
The dentist filled my hurting tooth
I experienced the pain in my left side of the mouth..it was a 2nd tooth from the last that was having a space n cause pain..i went to dentist n he filled the space instead of removing but few hours later the pain started…what will be the solution?
Steven
Reply –
When a patient comes to a dentist with a tooth that aches, (hopefully) their first inclination will be to attempt to “save” the tooth if they think that makes a reasonable approach.
That often involves placing a filling in the hopes that removing the cause of the tooth’s problems (tooth decay usually) will allow it to recuperate and be OK.
What they can never know for certain is how compromised the tooth’s nerve … already was/is/has become …, and it may be that it has been traumatized enough (either by the pathology that caused the tooth’s problems and pain originally, or by the added trauma created while trying to repair the tooth) that it’s nerve tissue can’t recover, or needs more assistance in recovering.
Your solution lies in being in contact with your dentist and letting them continue to evaluate your tooth and symptoms and provide whatever type of treatment they feel is necessary.
This page explains what type of testing they may do, as well as what you may experience that can help to diagnose your condition.
As far as an outcome, one of three things will transpire.
1) Continued efforts by your dentist will assist the tooth’s recovery and it will be fine. (This might include making sure the existing filling is fine, placing a treatment/sedative filling for a while, use of medications to aid the tooth’s healing, … only your dentist can determine what’s indicated.)
2) If not, then your dentist may suggest that having root canal treatment can provide a solution to your situation. Having root canal will remove the damaged/painful/not recovering nerve tissue from your tooth. Afterward, the tooth can be rebuilt, thus returning it to full function.
3) If you decide that you don’t want to have root canal treatment, or your dentist finds a reason why they wouldn’t expect that to be successful, then the tooth should be extracted and replaced with an artificial one.
Good luck. Be in touch with your dentist’s office.
Staff Dentist
Comment –
Tooth pain.
My tooth was aching like two to five months ago .. I visited the dentist and they gave me some tablets but no treatment. But today, a national holiday, I am feeling immense pain in my teeth .what should i do ?
Hari
Reply –
You need the attention of a medical professional. A dentist would be the first choice and the one who could provide definitive treatment (root canal treatment or whatever they determine is required).
There are reasons why the same dentist you consulted with before would make a good choice. They include:
1) Although they were unable to arrive at a diagnosis the first time that they felt confident enough with to base a treatment recommendation on (which isn’t uncommon), they will have documented their findings and impressions in your chart. In cases where a tooth’s current status is still unclear, those historic notes might (but not always) help with forming a diagnosis.
2) The dentist will have the X-rays they took months ago, which can be compared to current ones taken. Having this multi-month comparison may (but not always) assist them in figuring out what your tooth’s problem is.
[Note: As your health records, you can request that the items above are sent to another dentist.]
3) Since you’ve consulted with them previously, specifically about this tooth, one would hope that your previous dentist would address your situation with some priority.
4) Your previous dentist has a copy of your medical history (which could be updated via phone) and a history of providing you with some type of medication. With those, their previous notes about your tooth, and quizzing you on the phone about your current situation, they might feel comfortable with prescribing medications via telephone before physically examining you. Doing so might give you access (like on a holiday) to needed medications sooner (pain relievers, antibiotics or whatever is indicated).
As the bottom portion of this page discusses, there’s essentially nothing that a person can do on their own to remedy their situation. And often even very little they can do to control their discomfort. You need to give this some priority and seek direct attention from a professional.
Staff Dentist
Comment –
Tooth has crown – can it need a root canal too?
I have a tooth that I had a crown put on. Maybe 8 months ago (the most). Now it has it’s own heartbeat and hurts when I chew on that side. So….is a root canal next?
SB
Reply –
Your symptoms are consistent with that of a tooth that needs root canal treatment. But of course it will take an evaluation by your dentist to know this for sure. You should definitely be in contact with them, and sooner rather than later.
If a root canal is needed, that type of scenario isn’t astoundingly uncommon. We discuss dental-crown-then-root-canal situations here.
Staff Dentist
Comment –
Root canal.
ok so I have a really deep cavity in my left molar. When I was in a couple months ago my dentist told me that if it became painful then he would have to do a root canal, but I just want it extracted instead. A couple days ago I started to feel horrible pain with my tooth and I took a flosser and put it between my teeth, then I discovered that there was a small hole ( you know when you pull out your baby teeth you can stick your finger nail into the bottom of your teeth to help pull it out) and I could stick the flosser under my molar. So I plan to get my molar pulled instead, or should I get a root canal? I’m only 15!
Rhee
Reply –
If your dentist feels that they can salvage your tooth, that is typically the best plan as opposed to extraction. We have a number of sections and pages on our site that discuss various aspects of what you’ll need to think through.
Problems associated with just extracting a tooth and not replacing it.
Methods of replacing an extracted tooth if root canal treatment isn’t chosen.
Root canal vs. dental implant placement.
Staff Dentist
Comment –
Abcessed tooth/ root canal
A week ago I woke from sleep with an explosive pain in face, I looked in mirror, my right side of my face was extremely swollen, eye was swollen shut, lower part of face drooping. This was at 4am, I went to the ER thinking maybe a sinus infection, I was prescribed antibiotics by the doctor…he did no X-rays, did not look in my nose, didn’t look in my mouth. I took the antibiotics for 6 days, still having a great deal of pain, I decided to go to the dentist, after his exam it was determined I have an abcessed tooth, following day he started a root canal, he cleaned the canal, but said I have more infection that didn’t drain, he sealed the tooth and has prescribed amoxicillin, and has scheduled root canal part two in 10 days. Is this common?
VJS
Reply –
Yes, the way your dentist is treating you tooth is commonplace, and it sounds like you’re in good hands with them.
You said they sealed your tooth back up, meaning they’re trying to prevent more bacteria from entering the tooth after cleaning it somewhat.
A sealed tooth might flare up (allow pus to build up like it did before), so they’ve place you on antibiotics to make that event less likely.
They have appointed you for 10 days out, a point after you’ll have stopped taking the antibiotics. That way they’ll know if the tooth is staying quiet on its own accord, or only via the assistance of the antibiotics (a diagnostic test helping them to understand when they can complete the tooth’s treatment).
If perchance you notice problems, especially those similar to what you had before, starting to brew, let them know promptly. Most likely you’ll be fine.
Staff Dentist
