Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
Tooth extraction aftercare: Instructions for the first 24 hours after having your tooth pulled.
Tooth extraction aftercare – The first 24 hours.
Once your extraction procedure has been completed, initiating proper aftercare is vital for minimizing post-surgical complications and ensuring a smooth recovery. The first 24 hours are especially critical because the events that occur during this phase set the stage for the healing process that follows. What you do, or don’t do, during this initial period will significantly affect how your recovery progresses in the coming days and weeks.
This guide explains why controlling bleeding and protecting the blood clot that forms are two of the most important goals during the initial 24-hour period. It also outlines steps you can take to minimize postoperative pain and swelling and includes guidelines for eating, drinking, physical activity, and other key concerns. (Check out this page’s Table of Contents for a complete list of its topics.)
FYI: This is the first of two post-extraction instruction sets that you’ll need.
Once your tooth extraction procedure has been completed, your dentist will need to provide you with two sets of aftercare instructions.
- One set will address things to do, and not to do, during the first 24 hours after having your tooth pulled. (That’s the subject of this page.)
- The second set of instructions will outline aftercare during the days following the first 24 hours post-op.
Related pages: Tooth extraction healing timeline. | How can you tell if you’re developing complications?
Where do our instructions come from?
As sources for this page, we read through the post-extraction directions published on the websites of several university-based oral surgery programs. From them, we’ve identified the most frequently mentioned issues pertaining to the first 24 hours post-op and created the composite instructions set that you’ll find on this page.
- University of Washington School of Dentistry

- University of Michigan Medicine

- McGill University Division of Oral and Maxillofacial Surgery

- University of Rochester Eastman Institute for Oral Health

Extraction Aftercare Checklist – The 1st 24 hours post-op.
Customize this list so you’ll know what you’ll do for these issues.
- Controlling bleeding.
- Blood clot protection.
- Sinus precautions.
- Managing numbness.
- Minimizing swelling.
- Managing pain.
- Activities.
- Eating, drinking, teeth cleaning.
- Smoking. | Alcohol.
- Antibiotics.
- Dentist contact info.
Print out. Add notes while reading this page.
What issues are included in our instructions?
We also explain the underlying principles associated with post-extraction directions.
Just follow the links we’ve placed throughout this page for those more in-depth type of details. In some cases, we’ve dedicated entire pages to individual subjects.
Get your dentist’s input and OK.
While we’ve included what we found to be the most frequently given aftercare instructions for the first 24 hours following an extraction, your specific situation may involve special circumstances or concerns.
For this reason, in all cases you should discuss the steps we outline (scroll through our list with your dentist or their staff member on your phone) so they can modify and amend them as they feel is indicated.
Additionally, and once again in all cases, if you feel you have developed complications, including any issues not mentioned on this page, you should never hesitate to contact your dentist. It’s their obligation to address all of your post-op needs.
This page’s highlights as a video –
Subscribe to our YouTube channel.
Postoperative instructions for the first 24 hours following a tooth extraction.
Here’s a concise presentation of our directions. The links in this section then take you to more in-depth details, either found lower down on this page, or for some topics, on a page on our website dedicated to that subject alone.
► Control the bleeding coming from your extraction site. (First 24 hours post-op)
Gauze placed by your dentist.
Your dentist will have placed a folded piece of gauze over your tooth’s socket at the completion of your procedure. You should continue to apply firm pressure to that gauze for the next 30 minutes. Doing so should stop the bleeding from your extraction site.
If bleeding persists.
After following the instructions above, if bleeding continues or at some point restarts, place a fresh piece of moistened gauze over your extraction site and apply firm, constant pressure on it for 30 to 60 minutes. You may need to repeat this process a few times. If after doing so bleeding continues, you should contact your dentist.
What’s normal?
A minor amount of continued bloody ooze coming from your surgical site that tinges your saliva can be expected during the first 24 hours.
◆ Jump ahead to our post-extraction bleeding section for details.
► Protect the blood clot that forms. (First 24 hours post-op)
Do not rinse your mouth during the first 24 hours following your surgery. Avoid vigorous spitting too. These activities may prolong bleeding.
Also, avoid creating positive or negative pressure events (sucking or blowing actions). This includes the use of a straw, the act of smoking, blowing a musical instrument, or activities like blowing up a balloon. Doing so may dislodge or disrupt the socket’s blood clot.
◆ Jump ahead to our protecting the blood clot section for details.
► Needed sinus precautions. (First 24 hours post-op)
If you’ve had an upper tooth pulled, avoid creating increased pressure situations with your sinuses. Do not blow your nose. If you need to sneeze, do it with your mouth open.
◆ Jump ahead to our sinus precautions section for details.
► How to minimize postop swelling. (First 24 hours post-op)
- Repeated cycles (ice pack/no ice pack) during waking hours only, 15 minutes on followed by 15 minutes off.
- Begin the applications immediately following your procedure.
- Additionally, when lying down keep your head elevated by propping it up with 2 or 3 pillows.
◆ Jump ahead to our post-surgical swelling section for details.
► Ways to manage pain. (First 24 hours post-op)
It’s normal to feel some discomfort coming from your extraction site. Taking pain medication promptly after your procedure and before your numbness has worn off can help to limit the amount you do.
- Ibuprofen (Advil, Motrin, or generic) can make a good choice for controlling mild to moderate post-extraction pain. Or if you cannot use ibuprofen, acetaminophen (Tylenol or generic) can provide an alternative. In all cases, you must stay within the guidelines stated by the product’s manufacturer.
- If your dentist anticipates that your post-op recovery may involve comparatively more severe discomfort, they will prescribe a prescription pain medication for you.
- Avoid taking pain relievers that contain aspirin because their use may lead to more bleeding.
- If you notice side effects from taking any medication, including skin rash or itching, discontinue its use and contact your dentist immediately.
Note: Consult your healthcare professional before taking any medication to confirm that it’s safe and appropriate for your use. Use medications only as directed.
◆ Jump ahead to our post-extraction pain control section for details.
► If antibiotics have been prescribed. (First 24 hours post-op)
If your dentist feels that the use of an antibiotic is indicated, they will give you a prescription for one. If antibiotics have been prescribed (either before or after your surgery), take the full course as directed.
If you notice any side effects from taking any medication, including skin rash or itching, discontinue its use and contact your dentist immediately.
Most extraction cases do not need to involve the use of antibiotics so do not be alarmed if they have not been prescribed for you.
◆ Jump ahead to our post-extraction antibiotics section for details.
► Monitoring postoperative numbness. (First 24 hours post-op)
Expected that the local anesthetic that was administered during your procedure will slowly wear off during the next 2 to 4 hours. While numb, you’ll need to take precautions so you don’t injure yourself. For example:
- Be careful not to bite your lips or tongue. (Children will need to be coached and monitored on this point.)
- Avoid exposing soft tissues (lips, tongue, face, etc…) to harmful hot or cold temperature extremes.
◆ Jump ahead to our precautions with numbness section for details.
► Guidelines about physical activity. (First 24 hours post-op)
You should limit your activities for the rest of the day following your surgery. Avoid bending over, lifting objects, or participating in sports or exercise classes. The best plan is to just relax and get plenty of rest.
When lying down, prop your head up with 2 or 3 pillows. (Doing so will help to minimize bleeding and swelling.)
◆ Jump ahead to our post-extraction activities section for details.
► Guidelines about smoking. (First 24 hours post-op)
Do not smoke. Smoking increases the risk of dry socket formation and other postoperative complications.
◆ Jump ahead to our tooth extractions and smoking section for details.
► Guidelines for eating and drinking. (First 24 hours post-op)
Avoid eating or drinking for the first hour after your surgery (with the exception of liquids needed as an aid with taking medication).
Over the following 24 hours, drink plenty of fluids so you stay properly hydrated. Choosing soft or liquid foods makes it less likely that you’ll traumatize your extraction site when eating. The temperature of foods and beverages you consume should be kept cool, not hot.
◆ Jump ahead to our eating and drinking following an extraction section for details.
► Guidelines about drinking alcohol. (First 24 hours post-op)
Do not consume alcoholic beverages following your surgery. Alcohol consumption is also contraindicated as long as you are taking narcotic pain relievers and some types of antibiotics.
► Oral home care guidelines. (First 24 hours post-op)
Do not rinse your mouth during the first 24 hours following your procedure.
You may clean your teeth on the day of your extraction but you must be careful to avoid your surgical area. For routine cases, stopping a tooth short of either end of your extraction site typically makes a good plan.
◆ Jump ahead to our post-extraction oral home care section for details.
► Make sure you have emergency contact information. (First 24 hours post-op)
More in-depth details about the above instructions –
A) Stopping tooth extraction bleeding.
Immediately after your tooth has been pulled, some amount of bleeding will occur, possibly for some time.
[FYI: Use this link for information about post-extraction bleeding that continues beyond the initial 24-hour period. What to do.]
a) Controlling bleeding with gauze.
In most cases, post-extraction bleeding can be readily controlled, and ultimately stopped, by performing the following routine:
Closing down on gauze is a good way to control extraction site bleeding.

Place firm pressure on the gauze for 45 minutes or longer.
Steps to bring post-extraction bleeding under control.
- Place a clean piece of dampened gauze over the empty tooth socket.
Before putting it in place, roll the gauze up, or better yet, fold it into a small square. (It’s only the portion that rests directly over your wound that plays a role.) If you don’t have any gauze, a piece of clean cloth can be used instead.
- Bite firmly on the gauze for 30 minutes to an hour.
Make sure the wad of gauze is large enough and positioned so that when you bite down on it it applies pressure directly onto your extraction site. (If your teeth come fully together when you close, the gauze may not be receiving much pressure.)
- Repeat cycles of the above, a few may be needed, to finally bring the bleeding fully under control.
Note: Applying pressure over an extended period is the key.
It’s both creating firm pressure and maintaining it continuously over a prolonged period (30 to 60 minutes of application time) that are important factors in getting this technique to work.
- Don’t keep changing the gauze, don’t chew on it, and don’t get started up in a conversation. Just put the gauze in place and continuously close down on it for the full 30 minutes to an hour.
- If at the completion of the application your bleeding has stopped, you can discard the gauze. It is no longer necessary.
b) Controlling bleeding with a tea bag.
Using a damp tea bag can be more effective in bringing bleeding under control than gauze.
One of the components of tea (black tea, the regular stuff you would use to make iced tea) is tannic acid. Tannic acid aids in the formation of blood clots, thus making this method a very effective technique. (Same instructions as above, just substitute the tea bag for the gauze.)
Repeat the process as needed.
Continued bleeding. / Renewed bleeding.
If some bleeding still persists after the completion of a 30 to 60-minute application, then repeat the process above with a fresh piece of gauze or a new tea bag. The same goes if your bleeding once stopped starts up again.
- A few application cycles may be needed. However, after each one you should notice that the amount of flow coming from your extraction site is less and less.
- It’s rare that this technique, especially when a tea bag is used, doesn’t provide a solution. However, if bleeding continues, you should contact your dentist.
What constitutes persistent bleeding?
Every extraction site is expected to have some bleeding associated with it. And this can include some bloody oozing that is normal and may persist for 24 to 48 hours after your surgery.
In all cases where you have questions about the bleeding you’ve noticed, you should contact your dentist. Their questions will help them differentiate between:
- Oozing – A small amount of blood coming from the wound that tinges your saliva. (A little bit of blood in a lot of saliva will seem like a lot of blood.) Or dark red clumps of clotted blood.
- Bleeding – Bright red blood pooling in, or dripping out of, the surgical area within 15 to 20 seconds of removing the gauze.
More to know about post-extraction bleeding …
Clotting aids.
In some cases, your dentist may anticipate that post-operative bleeding will be a concern. If so, they may place some type of clotting aid in your extraction socket.
This might be an absorbable collagen or gelatin dressing (CollaPlug®, Gelfoam®), oxidized cellulose (Surgicel®), microfibrillar collagen (Avitene®), or a similar-purposed product.
From a standpoint of appearance, these products initially look like pieces of foam, sponge, or gauze. Then once moistened with blood and oral fluids, they soften considerably and are easily adapted into the opening of the tooth’s socket. Once placed, they are typically quite visible lying across the socket’s opening.
(Absorb = the process where a person’s body will naturally degrade and then take up the breakdown components of an object.)
You still need to follow standard protocol.
By no means does your dentist having placed a clotting aid in your tooth’s socket lessen your need to follow standard post-op instructions.
Instead, you should recognize that they consider you to be at elevated risk for complications, which makes faithfully following their directions all that more important.
What becomes of the clot?
B) Ensuring that an adequate blood clot forms (and stays) in the tooth socket.
The blood clot that forms in the tooth’s empty socket plays an important role in supporting the healing process that follows, so be careful not to do anything that will dislodge or disrupt it.
Remember, events that occur during this first-24-hours time frame will affect the healing process for days to come. For example, it’s thought that the formation of a dry socket Signs | Symptoms is related to the loss of the original blood clot.
Blood clot care and precautions.
As a way of protecting the clot that has formed in your tooth’s socket, during the first 24 hours following your extraction procedure, you should …
Extraction-site blood clot don’ts.
- Avoid vigorous rinsing or spitting. – These activities may dislodge the clot.
- Don’t disturb your extraction site. – Don’t touch or poke at it with your finger. Don’t explore it with your tongue.
- Don’t consume hot liquids and foods. – Hot items, especially liquids like soup, tea, and coffee, tend to dissolve blood clots.
- Minimize air pressure differences. – You should also avoid creating air pressure variations in your mouth, or pressure differences between your mouth and your sinuses (in the case of an upper tooth extraction) because these events may dislodge the blood clot from its socket.
This means you should avoid smoking or using a straw (these activities create suction). Also, don’t blow your nose, or objects like a musical instrument or blowing up a balloon. And if you need to sneeze, sneeze with your mouth open. (See below for more details.)
- Physical activities. – Moderation is key in helping to both control bleeding and avoid renewed bleeding. We discuss physical activity guidelines in greater detail below.
- Postural considerations. – When you sleep or lie down, position yourself so your head is above the level of your heart. Doing so tends to lower your head’s blood pressure level, which when trying to control post-extraction bleeding is a favorable thing.
Toward this goal:
- In bed, prop your head up using an extra pillow, or even 2.
- Rest in a recliner with the head portion of your chair positioned higher than your feet.
Be careful when transitioning from a reclined to upright position. You may find you get lightheaded. Try just sitting up for a minute before slowly getting on up.
C) Swelling may occur.
It’s common and normal for some degree of swelling to occur after having a tooth pulled. The amount that ultimately forms is typically proportional to the extent of the surgery that has taken place. That means:
- After very simple extractions you may notice very little, possibly none.
- With more involved cases (longer, more difficult extractions or the removal of several teeth) you may notice a pronounced enlargement, possibly involving a large portion of your face.
Generally speaking, the amount of swelling that forms can be minimized via the application of ice packs on the outside of your face over the area where your surgery was performed, starting immediately upon the completion of your procedure.
This page provides in-depth details and instructions about this complication: Post-tooth extraction swelling. What to expect. | Management.
D) Sinus considerations.
Avoid blowing your nose.
As mentioned above, in the case where you’ve had an upper back tooth removed (molar, bicuspid) it’s best form to refrain from blowing your nose.
That’s because doing so can create a pressure difference between your mouth (via the recesses of your extracted tooth’s socket) and your sinuses that might be great enough to disrupt what in some cases may be just a paper-thin layer of bone separating the two.
Oroantral communications.
Failing to follow these directions can result in the creation of what’s termed an “oroantral communication” (a direct connection between your mouth and sinus). And the development of one may complicate the healing process. Here’s how.
Other precautions.
Actually, it’s not just avoiding blowing your nose that’s important. You should generally refrain from doing anything that might create a pressure difference, such as:
- Sneezing. If you need to sneeze, do so with your mouth open.
- Avoid sucking on items such as a straw or cigarette.
- If you play a ‘wind’ musical instrument, ask your dentist when it will be OK to resume playing.
E) Precautions with numbness.
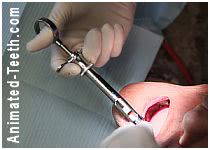
The numbness from your local anesthetic will linger after your procedure.
How long will the numbness last?
You can expect to notice the effects of the anesthetic used for your procedure for some hours following your extraction. The method of injection and the type and formulation of anesthetic solution used are primary determining factors in what you’ll experience.
Studies evaluating the effect of various anesthetic solutions commonly used in dentistry for numbing up lower molars (inferior alveolar nerve block injections) have reported duration times of:
- 2.5 hours (Elbay 2016), 2.5 hours (Managutti 2015), and 3.8 hours (Kammerer 2012). [page references]
- Differences in the duration of numbness among individual patients generally varied from 18 to 35 minutes (plus or minus).
What precautions should you take?
The sensory loss (pain, temperature, and touch) that your postoperative numbness creates can result in accidents. For example …
- You might unknowingly bite your lip or tongue while chewing, possibly even repeatedly.
- You might not be able to test hot (temperature) foods and beverages adequately, which could result in burns.
- Some patients, especially children, may find their numbness a novelty and will bite on, or chew, numbed tissues (lips, cheeks, or tongue). This may result in significant damage.
In regard to this last issue, children must always be monitored during periods of numbness.
F) Controlling extraction-site pain.
The level of discomfort a patient can expect during the first 24 hours following their extraction can be quite variable. For some people, it will be a non-event. For others, it may be quite noticeable.
(FYI: This page discusses pain that extends beyond the initial 24 hours following your procedure. What to expect. | Management.)
Timing your medication.
Quiz your dentist about what to expect. If they feel it’s highly likely that you’ll need to take an analgesic (pain pill), a good plan can be to do so before the local anesthetic used for your procedure has worn off. (That will be tapering down over the next hour or two.)
If discomfort does become an issue, in terms of types of analgesics there are two general classes of medications that are typically used.
a) OTC medications.
For just minor to mild pain, your dentist will probably advise the use of an over-the-counter (non-prescription) analgesic. Commonly used products include acetaminophen (Tylenol®) or ibuprofen (Motrin®, Advil®).
Note: Consult your healthcare professional before taking any medication to confirm that it’s safe and appropriate for your use. Use medications only as directed.
b) Prescription medications.
If a higher level of pain relief is needed, your dentist will likely turn to the use of prescription analgesics.

A narcotic pain reliever may be needed after some extractions.
Precautions with narcotic medications.
- These products tend to cause nausea (upset stomach). This effect can be minimized by taking the medication with milk or food (milkshake, soup, fruit juice, yogurt, mashed potatoes, etc…).
- Taking a narcotic may make you dizzy, drowsy, or groggy. It may also slow down your reflexes or cause you to act strangely.
If you’re taking a narcotic medication, you should let those around you know. You should also limit your activities (driving, operating machinery, etc…).
- Additional common side effects include nausea, vomiting, and constipation.
- You should abstain from drinking alcoholic beverages when taking a narcotic.
Additional precautions.
Make sure that you read and follow all directions and precautions associated with your medication’s use. If you have any questions, you should discuss them with your dentist or pharmacist.
Remember that your product has been prescribed to you for the short-term use of controlling the pain associated with your extraction. Since some products can become habit-forming, their use should be discontinued at the earliest point when pain control is no longer needed.
G) Continue on with prescribed antibiotics.
Any antibiotics prescribed by your dentist should be taken as directed. Historically this has meant “to completion” (the endpoint where all of the medication has finally been taken according to schedule). Doing so may include continuing on even after your tooth has been removed. (Being prescribed a 7-day supply is common.)
Depending on the reason why taking the medication was indicated, under modern prescribing guidelines a common regimen for dental antibiotic usage nowadays involves a variable treatment course of 3 to 7 days, with the medication discontinued 24 hours after a complete resolution of symptoms has occurred.
▲ Section references – Lockhart
FYI: This page explains some reasons for Antibiotic use with extraction cases.
H) Eating and drinking.
Is it OK to eat after having a tooth pulled?
Yes, maintaining proper nutrition is important for both keeping up your strength and providing the nutrients needed for your extraction site’s healing process, so try not to skip any meals.
For the first several days, keep foods away from your surgical area by chewing on the other side. That will help to minimize any chances of disrupting its healing process or allowing debris to collect in it.
Sticking to cool, soft foods makes the right choice after simple extractions. When multiple teeth, multiple extraction sites, or surgical extractions are involved, a liquid diet (supplemental nutrition drinks) may be indicated during the first 24 hours. (See our post-extraction food suggestions below.)
Precautions with eating the day of your extraction (first 24 hours post-op).
- Nutrition is important, so don’t skip meals.
- Avoid beverages during the first hour.
- Wait for your numbness to wear off before eating.
- Avoid hot (in temperature) foods and beverages.
- Choose soft, non-spicy foods.
- Keep food and chewing on the other side of your mouth.
- Maintain adequate fluid intake during the day.
- Avoid consuming alcohol.
How soon after your extraction procedure can you eat?
- Following simple single-tooth extractions, you may be able to return to a fairly normal diet and regular eating habits after just a few days.
- After more involved ones (surgical extractions, the removal of multiple teeth) you may need to favor your extraction site for most of a week as its healing gradually progresses.
What kinds of foods are recommended?
As a general rule, stick to cool, soft foods as opposed to hard, crunchy, or spicy ones after having a tooth pulled. You should also avoid consuming alcoholic or carbonated beverages, or drinking using a straw (the negative pressure might draw the blood clot out of your socket).
- Soft foodstuffs are less likely to traumatize your extraction site (this is true for both the day of your extraction as well as during the healing process that follows).
- Hot food items (especially soup or coffee but even semi-solid ones) have the potential to dissolve the blood clot that has formed in your tooth’s socket, so they should be avoided during the first 24 hours.
Consider food items like these: pudding, yogurt, jello, mashed potatoes, oatmeal, applesauce, scrambled eggs, pancakes, noodles, (cool) soup, ice cream, milkshakes, and supplemental nutrition drinks.
As the healing of your extraction site progresses, you can start to add foods that have more firmness and texture to your diet.
Drinking dos and don’ts.
It’s important to stay well hydrated. That’s because you’ve lost some bodily fluids during your extraction procedure. You’ll also want to maintain optimal body chemistry for your socket’s healing process.
- Do not consume alcoholic beverages following your surgery. Also, alcohol consumption is contraindicated as long as you are taking narcotic pain relievers, and some types of antibiotics.
- As a best practice, except for taking medication you should delay drinking fluids for 1 hour following your extraction procedure.
- Especially following more involved extractions (difficult procedures, the removal of multiple teeth), drinking 6 to 8 glasses of water per day makes a good idea.
- Simply drink the beverage. Rinsing or similarly disrupting your extraction site with liquids during the first 24 hours should be avoided.
- Liquids should be at room temperature. Hot liquids may tend to dissolve the blood clot that has formed in your extraction site.

Don’t smoke for as many days as you can.
I) Avoid smoking.
We explain the hows and whys of this effect in greater detail in our discussion of smoking as a risk factor for dry sockets. The relationship.
J) Minimizing activities.
During the first 24 hours following your tooth extraction, you’ll want to minimize physical exertion. After all, you’ve just had a surgical procedure performed. Included in this precaution are any activities that might:
- Interfere with controlling the bleeding coming from your extraction site.
- Cause interference with blood clot formation and retention.
- Direct physical strain or disruption toward your wound.
The risk of these complications is often just minimal after very simple extractions (like having an individual small, single-rooted, erupted tooth pulled). However, when multiple teeth have been removed or the patient’s procedure has been an involved one (like removing an impacted wisdom tooth), they can become a substantial concern. Either way, it only makes sense to take precautions.
Activities.
It’s best to avoid strenuous work or exercise. You should also avoid bending over or lifting heavy objects. In general, it’s not a bad idea to just take it easy for the rest of the day following your surgery. Of course, your best judge of what level of activities might be acceptable in light of the kind of procedure you’ve just had would be your dentist, so ask.
(Related page: How much time should you take off from school or work after an extraction? How long?)
K) The first night after your tooth extraction.
Sometime during the first 24 hours after having your tooth pulled, you will of course need to go to bed and get some sleep. In preparation for doing so, there are a couple of points and precautions you should keep in mind.
Have your extraction site’s bleeding under control well in advance of going to bed.
As outlined throughout this page, your primary job on day one following your tooth’s extraction is to take the steps necessary to assist your body in stopping the bleeding from your extraction site and helping to ensure that a proper blood clot forms in your tooth’s socket and remains there.
During your first night’s rest after your extraction, you’ll be asleep and won’t be able to actively participate in any of these steps. Also, leaving gauze in your mouth as you sleep will create a choking hazard.
So, be responsible and follow your dentist’s postoperative instructions (like those found on this page). If you encounter difficulties, be in touch with them. You’ll need to have your bleeding under control before going to sleep.
Sleep with your head elevated slightly.
As mentioned previously on this page, it’s best if you can keep the level of your extraction site above your heart. Doing so tends to lower your head’s blood pressure, and when trying to maintain control of post-extraction bleeding, that’s a favorable thing.
- If you plan to sleep on your side, an easy way to accomplish this is by placing an extra pillow under your head. If possible, rest the side of your face that’s opposite your surgical area against your pillow.
It’s normal that a slight amount of blood may ooze from your wound while you sleep, so placing an old pillow case over your pillow makes a good choice. Or, better yet, place an old towel on it.
- Another option for elevating your head is to sleep on your back inclined against your headboard.
Neither of these positions may be your favorite one. But for this first night following your extraction, there’s a lot to be said for taking precautions. Even if it comes at the expense of a little comfort.
Other things to keep in mind about your first night post-op.
- No rinsing. – As you prepare for bed, you may notice that your mouth doesn’t feel as fresh as you’d like.
It’s of course permissible to drink some water. And you can hold water in your mouth and then just let it flow out. But rinsing this first night, even worse if performed using mouthwash, runs the risk of irritating your surgical site and/or dislodging the blood clot that has formed in your tooth’s socket.
- Keep your medications on schedule. – With some leeway, you want/need to keep on schedule with taking your medications this first night. Even if that means setting an alarm.
The dosing frequency of medications (pain relievers, anti-inflammatory drugs, antibiotics) can play an important role in their effectiveness. Unquestionably, you’ll sleep better if you’re not in pain.
- No ice pack applications while you sleep. – Your first night following your extraction lies within the time frame when ice packs are typically used to minimize postoperative swelling. However, that activity is for waking hours only (see instructions above). Prolonged exposure to cold extremes may cause tissue damage.
- If you’re hungry, have some food before going to bed. – You’ll sleep better if you’re not hungry, so have something soft or liquid, and cool instead of hot, that satisfies your hunger.

Avoid rinsing your extraction site with mouthwash.
L) Cleaning your teeth.
- On the day your tooth has been pulled, it’s best to avoid brushing those teeth that directly border your extraction site. Wherever access isn’t a problem, it’s OK to clean your other teeth.
- During the first day after your extraction, it’s OK to let water or saline solution (1/2 teaspoon of table salt in 1 cup of warm water) roll around in your mouth but rinsing vigorously must be avoided. Doing so might dislodge the blood clot that’s formed in your tooth’s socket.
- Avoid the use of commercial mouthwash or mouth rinse. These products may irritate your extraction site.
M) Emergency contact information.
With the postoperative instructions that your dentist gives you, they should also provide you with their emergency contact information. If you feel you need their assistance, you should not hesitate to contact them. That’s a part of their obligation to you as your treatment provider.
Looking for more information?
With your first-day postop period coming to a close, we’d recommend that you read this page next: Extraction aftercare instructions – 24-hours postop and beyond.
Other pages of interest for many of our readers are these two: Is your extraction site healing properly? – What to look for. or Tooth extraction healing timeline. – What’s normal?
If instead you’re looking for detailed information about any aspect of post-extraction care or potential complications, select from this menu: Tooth Extraction Guides.
Last reviewed: April 20, 2026
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Cohen N, et al. Healing processes following tooth extraction in orthodontic cases.
Lockhart PB, et al. Evidence-based clinical practice guideline on antibiotic use for the urgent management of pulpal- and periapical-related dental pain and intraoral swelling: A report from the American Dental Association.
McGill University Department of Oral & Maxillofacial Surgery. Surgical Teeth Extractions Post-Operative Instructions.
University of Michigan Department of Oral & Maxillofacial Surgery. Tooth Extraction Post-Operative Instructions.
University of Rochester Eastman Institute for Oral Health. Postoperative instructions following dental extraction surgery.
University of Washington Department of Oral & Maxillofacial Surgery. After your oral surgery.
Video transcription.
Hello, welcome to Animated Teeth.com and our discussion of post-extraction instructions for the first 24 hours after having your tooth pulled. Using this video, we’ll point out some of the more important issues we cover on this page and absolutely feel you must be aware.
At the very top of our list are two related items, controlling your extraction site’s bleeding and then protecting the blood clot that has formed.
If you’ve just had a tooth pulled, these two tasks are your primary job today. Period. That’s because the foundation you lay during the first 24 hours following your procedure sets the stage for the healing process that immediately begins.
Messing up these steps will prove to be a nuisance for you today, tend to delay your healing process for some days to come, and possibly even lead to a painful condition called a dry socket, an experience that most people ruefully remember. So, a stitch in time. Well … you know the rhyme.
Despite that belabored warning, doing what you need to do to control your extraction site’s bleeding is typically quite simple, uneventful, and just requires you to keep your mouth closed.
Applying firm pressure to a wound is standard first aid in controlling bleeding. And that applies to wounds in the mouth too.
At the end of your procedure, your dentist will place a wad of gauze on top of your extraction site and then instruct you to bite down on it gently but firmly. They’ll then tell you to hold that pose for the next 30 minutes.
And if you can follow those simple instructions (no yapping, no phone calls, no eating, no drinking), for the next 30 minutes, one of your day’s main tasks will probably already be accomplished.
Of course, even with the best-laid plans issues can arise and sometimes 30 minutes isn’t long enough. And if not, the solution is to do more of the same.
Dampen some of the extra gauze your dentist sent you home with, place it on top of your extraction site and bite firmly on it for another 30 minutes, or even an hour. Better yet, instead of gauze use moistened teabags.
After a cycle or two, if you don’t see substantial improvement in your situation, it never hurts to be in touch with your dentist for advice and support. We guarantee you however, the first words out of their mouth will be “have you tried a teabag yet?” So, switch to that sooner rather than later during the process.
The issue of protecting the blood clot that forms is pretty much just as simple. In this case, you just need to take things easy. And not just for this first 24-hour period but really for the next few days too.
As examples, you shouldn’t vigorously rinse your extraction site. And don’t be poking at it with your tongue, finger, or a toothbrush.
Actually, you really need to read through our entire list of do’s and dont’s because there are some activities that can lead to blood clot loss that you might not usually think of. This includes physical exertion, blowing your nose, and even just enjoying a cup of coffee or a bowl of hot soup.
The first 24 hours following your extraction is also a time frame when you can take steps to help to minimize the level of swelling that ultimately forms. We discuss this issue on its own page, so look for that, but generally, today is the day that you’ll begin cycles of ice pack application during your waking hours.
We will point out that swelling isn’t always an issue with all extractions. Sure, patients who have had an impacted wisdom tooth removed will be wise to initiate preventive steps. But for the average routine extraction, whatever swelling occurs will probably just be minimal and probably not noticeable. Ask your dentist what to expect.
Of course, you’ll still be numb after your extraction, and continuing on for the next few hours. That can interfere with your speech, or eating and drinking. But of course, you’re not supposed to be doing those things immediately after your extraction anyway.
Because of their numbness, some people inadvertently bite their lip, possibly even repeatedly. So, be careful, or, very importantly, keep your eye on your child if they’re the one who has had a tooth pulled.
Also, be sure to maintain proper on-off cycles if using an ice pack to minimize swelling. Otherwise, your numbness may keep you from realizing how cold your tissues are getting.
There are additional first-24-hour post-extraction instructions that you should be aware of, so please take the time to read through this page. All of these instructions are important because, like we said at the beginning of this video, they help to set an ideal stage for the healing process that’s starting up. So, take heed.
As one last point, if you have questions or concerns, it’s always appropriate to be in touch with your dentist. They are your healthcare provider, and not just by way of performing your extraction but also in providing you with whatever post-operative care you require. That’s their obligation, and no doubt an aspect of their practice that they take pride in providing. So, make sure to ask for their assistance if you need it.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
I’ve noticed some pain.
I just got my tooth pulled 2 hours ago…I’m feeling a bit of pain, is that bad?
Ashley
Reply –
In all cases, a patient should always feel free to contact their dentist about any concerns that they have. Responding to your needs is a part of their obligation to you as a treatment provider.
It seems possible that what you are experiencing falls within the realm of usual. Here’s what our pages state about post-op pain during the same day of an extraction.
Staff Dentist
Comment –
Worse after tooth extraction.
I had an upper molar removed 7 hours ago the dentist said at the time she was having difficulty extracting the tooth and had to ask her assistant to hold my head while she pushed and pulled eventually it came out successfully. 7 hours later I am suffering extreme pain worse than tooth ache is this normal?
S.C.
Reply –
Your case might be an example of where performing a surgical extraction might have resulted in creating less procedure trauma than performing it conventionally. But that is hindsight now.
With any extraction procedure, postoperative pain is common and not unexpected when it occurs. We discuss the issue of controlling postoperative pain during the first 24 hours here.
Rather than a website, seeking attention from your dentist makes the better plan. Dentists expect that emergencies will happen, especially with difficult extractions, and expect to hear from their patients if their assistance is needed. That is their obligation to you as your treatment provider.
Staff Dentist
Comment –
First day question.
I left my gauze in place for 5 hours. I would change it every hour. I didn’t understand that it was only to be done for an hour or so. Did I hurt my blood clot? It still looks like it’s there.
JS
Reply –
Your post is a little bit unclear (did you or did you not change the gauze each hour). But either way it seems unlikely that you would have done any harm.
The customary instructions are, place the gauze and bite on it (30 minutes to an hour), then repeat that process as needed (to control continued bleeding). What you did would seem to have just ensured that the bleeding was controlled. The extended presence of the gauze probably provided better protection for the forming clot than if it hadn’t been there.
Staff Dentist
