Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
Extraction Aftercare and Recovery – Post-op instructions for the Day After Your Tooth Extraction and Beyond.
Post-extraction aftercare –
Beginning 24 hours after your extraction process, and the days beyond.
Separate from the set of aftercare instructions your dentist gives you for the first 24 hours following your extraction Jump to list. , they’ll also need to provide you with a second set of directions that outline the steps you should take beginning the day following your surgery (24 hours post-op) and beyond.
This second set of directions, which is the subject of this page, will focus on two general areas of concern:
A) Steps that address basic post-extraction aftercare.
This group of instructions focuses on extraction site care. They’ll include things to do that will help to keep conditions for your healing socket as optimal as possible.
For the most part, this aspect of aftercare has to do with how to keep the wound clean, minimizing the potential for wound disruption, and if placed, when to remove stitches.
With simple, routine extractions uncomplicated by post-op side effects, these may be the only instructions that you’ll need to follow.
B) Steps focused on identifying and managing postoperative complications.
This portion of the instructions will provide information about identifying developing postoperative side effects and complications, as well as steps that can be taken to alleviate or manage them.
- Common near-term issues are swelling and bruising, and less frequently persistent bleeding or continued pain.
- Developing complications can include the formation of a dry socket (often characterized by throbbing pain) or bacterial infection.
- Complications usually involving a longer time frame are surfacing bone or tooth fragments or the consequences of procedure-related nerve damage.
FYI: If you’re looking for information for about a particular postoperative issue, use the following Table of Contents for a link that jumps ahead to specific content areas.
Where do our aftercare instructions come from?
In an effort to make our “2nd day and beyond” post-extraction directions as thorough as possible and more complete than available elsewhere, we’ve reviewed post-op instructions published by university-based oral surgery departments. And from those sources, we’ve created the compilation set of instructions found on this page. The sources we’ve used are:
- University of Washington School of Dentistry

- University of Michigan Medicine

- McGill University Division of Oral and Maxillofacial Surgery

- University of Rochester Eastman Institute for Oral Health

Extraction Aftercare Checklist – The day after and beyond.
Customize this list so you’ll know where to start or what to do with these issues.
- Persistent bleeding.
- Pain management.
- Wound management and cleaning.
- Sinus precautions.
- Activities. | Time off.
- Eating, drinking, teeth cleaning.
- Smoking. | Alcohol.
- Antibiotics.
- Managing swelling/bruising.
- Stitches removal.
- Identifying post-op complications.
- Dentist contact info.
Print out. Add notes while reading this page.
You’ll need to check with your dentist and get their OK.
Your first line of support is your dentist.
Every extraction is unique.
Extraction difficulty does matter.
As you would expect, the extent of surgery needed for a tooth extraction can vary widely. And therefore, so will aspects of the healing process that follows.
As a simple comparison, it’s easy to imagine the differences associated with having an impacted wisdom tooth removed (a major surgical event involving a gum tissue flap, bone removal, tooth sectioning and placing stitches) vs. pulling a small lower front tooth.
You’ll need to keep these differences in mind.
As you read through our instructions, keep in mind that in order to make them as complete as possible for all extraction patients, they do include issues, directions and precautions that really won’t apply for the simplest cases.
Following our instructions as written won’t cause you any harm. But doing so may be overkill for your particular situation. Your dentist can help you decide.
This page’s highlights as a video –
Subscribe to our YouTube channel.
Overview – Aftercare steps to take during the period 24 hours after your extraction procedure and the days beyond.
As an introduction, here’s a brief outline of the steps that you’ll need to take starting on day two following your extraction. The links in this section take you to more in-depth instructions and details, either included lower down on this page, or for some topics, on a page on our website dedicated to just that subject.
► Favor your extraction site. (2nd day post-op and beyond)
Avoid any activities during the days that follow your extraction that might disrupt, or even dislodge, the blood clot that’s formed in your tooth’s socket, or disturb your healing wound. This includes:
- Positive and negative pressure events, such as blowing or sucking actions (using a straw, drawing on a cigarette, blowing a musical instrument, etc…). These seemingly benign activities may dislodge the blood clot that’s formed, with its loss resulting in dry socket formation. What’s this complication?
- Making extreme mouth motions, or exploring your extraction site (like with your finger or tongue).
- Allowing the foods that you eat, especially hard or crunchy ones, to drift into the area of your extraction site.
► Needed sinus precautions. (2nd day post-op and beyond)
If you’ve had a back upper tooth removed, avoid situations that create pressure in your sinuses. Don’t blow your nose for several days following your procedure. The same precaution goes for sneezing (if you must sneeze, do so with your mouth open).
◆ Jump ahead to our post-extraction sinus complications section.
► Ways to manage post-surgical swelling. (2nd day post-op and beyond)

With more involved surgeries, a larger amount of diffuse postop facial swelling may occur.
How to minimize the level of swelling that occurs.
Applications should be in cycles of 15 minutes on, followed by 15 minutes off, during waking hours only.
Bringing down swelling.
Once the level of swelling has peaked, moist heat (like a hot water bottle wrapped in a moistened towel) applied to the affected area can help to speed up the rate at which it subsides.
Applications should be made during waking hours in cycles of 20 minutes on, then 20 minutes off. Perform the applications 4 to 5 times a day in groups of several cycles.
◆ Jump ahead to our managing postoperative swelling section.
◆ Jump ahead to our postoperative bruising section.
► Ways to manage postoperative pain. (2nd day post-op and beyond)
Will you experience any pain?
It’s normal and expected that a patient may experience some level of discomfort after their extraction. The usual course of events is one where the pain that’s felt gradually diminishes, day-by-day, with it finally fully resolving after several days to a week.
If instead the pain you feel persists or intensifies (the opposite of progressively diminishing), you should contact your dentist.
Pain control.
For mild to moderate pain, the OTC pain reliever ibuprofen (Advil, Motrin, or generic) can make a good choice. For those who can’t use ibuprofen, acetaminophen (Tylenol or generic) can provide an alternative.
Note: Consult your healthcare professional before taking any medication to confirm that it’s safe and appropriate for your use. Use medications only as directed.
If your dentist anticipates that you may experience severe pain, they will prescribe a pain medication for you (once again, you must follow all of the product’s associated instructions and precautions). At that point where your level of discomfort has begun to diminish, the use of one of the OTC products mentioned above may then prove satisfactory.
If you notice side effects from taking any medication, including skin rash or itching, discontinue its use and contact your dentist immediately.
◆ Jump ahead to our post-extraction pain section.
► If antibiotics have been prescribed. (2nd day post-op and beyond)
- If your dentist feels that the use of an antibiotic is indicated following your extraction, they will provide you with a prescription for one.
- If antibiotics have been prescribed, either prior to or after your surgery, you should take the full course of the medication as directed.
Most extraction cases don’t involve the use of antibiotics. So if one hasn’t been prescribed don’t be alarmed.
If you notice any side effects from taking any medication, including skin rash or itching, discontinue its use and contact your dentist immediately.
◆ Jump ahead to our postoperative antibiotics section.
► Guidelines for eating and drinking. (2nd day post-op and beyond)
During the days immediately following your extraction, it’s important to drink plenty of fluids (6 to 8 glasses of water per day) so your body stays properly hydrated. It’s also important to maintain proper nutrition for your extraction site’s healing process.
Initially you may feel more comfortable eating comparatively softer foods as opposed to hard, crispy or crunchy ones. Maintaining a softer diet is also less likely to result in accidental trauma to your extraction site, and may be easier to eat if you’ve experienced jaw discomfort as a result of your procedure.
Even after more extensive surgeries, you’ll probably be able to return to your normal diet in about a week. Initially, avoid spicy and acidic foods. As your healing process progresses, you can gradually reintroduce foods from your original diet back into your meals.
► Guidelines for post-extraction activities. (2nd day post-op and beyond)
It’s best to avoid strenuous activities (bending, lifting, participating in sports, exercise classes, etc…) on the day immediately following your extraction.
After comparatively more involved surgeries:
- Strenuous activities should be avoided for the next several days, with their resumption eased into as you feel up to them.
- A patient might take 1 to 2 days off from their normal duties, returning to work or school after they feel recovered.
◆ Jump ahead to our sick leave after an extraction page.
► Guidelines about smoking. (2nd day post-op and beyond)
Do not smoke following your extraction. A minimum of 3 days, and preferably 7 days, is generally recommended if total smoking cessation is not possible.
▲ Section references – Politis
► Guidelines about alcoholic beverage consumption. (2nd day post-op and beyond)
You should not consume alcoholic beverages as long as you are taking narcotic (prescription) pain medication, and also some kinds of antibiotics. Generally, alcohol has a negative effect on healing tissues.
◆ Jump ahead to our the effects of alcohol on healing section.
► Guidelines about rinsing. (2nd day post-op and beyond)
Gently rinse your mouth 4 or 5 times per day (including after meals) with warm saltwater. (1/2 teaspoon of salt in an 8-ounce glass of warm water.)
◆ Jump ahead to our post-extraction rinsing section.
► Guidelines about performing oral home care. (2nd day post-op and beyond)
Resume cleaning your teeth as normal but you must be careful to avoid disrupting your surgical site. With larger wounds, be especially careful during the first week.
◆ Jump ahead to our post-extraction oral home care section.
► Extraction site irrigation may be indicated. (2nd day post-op and beyond)
With larger, deeper wounds (like those resulting from impacted wisdom tooth removal), your dentist may ask you to flush your extraction site periodically so to remove accumulated debris. If this is indicated, they will provide you with the needed tools and instructions.
◆ Jump ahead to our extraction site irrigation section.
► Sutures (stitches) management. (2nd day post-op and beyond)
Some surgical procedures require the placement of sutures. If yours has, your dentist will tell you if they are a type that will dissolve away on their own, or if they must be removed. If they will need to be taken out, your dentist will state when that should be. The usual time frame is 7 to 10 days following their placement.
Extreme mouth movements or exploring your wound with your finger or tongue can disrupt stitches. As the swelling in sutured tissues begins to subside, you may notice that your stitches loosen.
◆ Jump ahead to our stitches used with oral surgery section.
► Follow-Up appointments may be needed. (2nd day post-op and beyond)
If your dentist feels that a follow-up appointment is needed, they will tell you. For most extractions, a second visit will not be required. (That does not mean however that you shouldn’t contact your dentist if you have questions or a need.)
The most common exception would be removing stitches. But this is only required if they have been placed, and if they are not a type that will dissolve away on their own.
► Confirm that you have emergency contact information. (2nd day post-op and beyond)
Your dentist should provide you with their emergency contact information. And if you feel that you need their assistance, you should not hesitate to contact them. Providing postoperative care is a part of their obligation (ethical and legal) to you as your treatment provider.
Post-extraction symptoms that may signify developing complications.
- Swelling that increases in size beyond 48 to 72 hours post-op.
- Pain that 2 to 3 days postoperatively shows signs of increasing rather than gradually subsiding.
- A foul mouth taste or odor.
- Your temperature rises above 100.5 degrees (F).
- You notice side effects from medications, including the formation of a rash or itching.
If you experience any of these signs or symptoms, you should contact your dentist so they may evaluate them.
► Managing prolonged bleeding. (2nd day post-op and beyond)
At a point 24 hours after your procedure, the bleeding from your extraction site should have long stopped. Although, you may experience a minor amount of bloody oozing that tinges your saliva for up to 48 hours.
Persistent or renewed bleeding, especially that involving the flow of bright red blood, should be reported to your dentist immediately. The technique of applying pressure to the bleeding site via gauze should be implemented. Directions.
◆ Jump ahead to our complications with bleeding section.
► Managing difficulties with jaw function. (2nd day post-op and beyond)
Following longer or more involved dental surgeries, you may notice tenderness or reduced function in your jaw joint (TMJ). This can usually be explained by:
- Transient inflammation that’s formed in response to trauma that the joint and/or its associated muscles experienced during your procedure.
- The presence of postoperative swelling in the tissues surrounding the TMJ.
Function should gradually return to normal within a week or so.
◆ Jump ahead to our post-extraction complications with jaw movement section.
► Monitor for dry socket formation. (2nd day post-op and beyond)
A dry socket is a relatively common post-extraction complication that’s associated with a disruption of the normal healing process. Symptoms typically include a dull, throbbing pain that doesn’t appear until 3 to 4 days following your procedure, and a foul odor or taste. If you notice these symptoms, you should contact your dentist.
◆ Jump ahead to our dry sockets section.
► Post-extraction chip and fragment management. (2nd day post-op and beyond)
Small tooth chips or bone fragments may work their way to the surface of your extraction site and become apparent when they poke through your gum tissue. The timing of their initial presence can be quite variable, ranging from a few days to several weeks following your procedure.
These bits will often work their way out on their own, or else can be flicked out easily. Larger pieces may need to be removed by your dentist.
◆ Jump ahead to our post-extraction bone and tooth fragments section.
► Monitoring prolonged numbness. (2nd day post-op and beyond)
As a possible post-surgical complication, some patients may notice persistent numbness (paresthesia) following their procedure. (Numbness that extends beyond the 2 to 4 hours post-op period that’s normally expected.) If you do, you should contact your dentist so they can help you monitor your situation.
◆ Jump ahead to our dental paresthesia section.
The remainder of this page’s content reiterates and provides more in-depth details about the issues outlined in our instructions set above. (Many of the links above link down to this section.)
More in-depth details about the above instructions for the period beginning 24 hours after your tooth extraction.
A) Basic post-extraction aftercare – What’s needed?
In most cases, the only care that’s needed during this time frame is just maintaining the extraction site in a manner that helps to promote its healing. Extraction healing timeline.
Routine extraction-site care 24-hours post-op and beyond should include …
- Taking precautions with the wound so it isn’t traumatized or disrupted.
- Keeping the extraction site clean so it has an optimal healing environment.
- Keeping your activities in line with the level of surgery you have experienced.
(This link provides pertinent information and guidelines.)
- If needed, irrigating the socket (only per your dentist’s recommendations).
- If needed, having stitches removed at the proper time.
Print this list so as you read on you can make notes specific to your situation.
B) Managing post-extraction complications – What’s needed?
The other postoperative care that may be needed is managing any complications that develop. This would include conditions such as:
- Prolonged bleeding.
- Swelling.
- Bruising.
- Sinus precautions.
- Continued pain.
- Dry sockets.
- Tooth chips. / Bone fragments.
- Prolonged numbness.
- Muscle / Joint pain.
A) Basic post-extraction aftercare.
1) Avoid creating surgical site disruption.
Favor your extraction site.
You’ll need to avoid activities that might traumatize your extraction area. That’s because …
- They might disrupt or interfere with its healing process.
This would include events that might dislodge or damage any stitches, dressings or tissue flaps that have been placed or positioned.
- The new tissues that form are quite vascular (they contain many fragile blood vessels) and they will bleed easily if provoked.
Limiting post-extraction physical activities.
The extent to which you’ll need to limit physical activities during the days that follow your extraction will in part depend of the magnitude of your surgical event.
With simple single-root, single-tooth, extractions, by day three and possibly even on day 2 following your procedure, the concerns associated with performing activities may just be minimal. But with more involved surgical procedures, like the removal of impacted wisdom teeth, not following precautions may lead to complications like renewed bleeding.
Generally, it’s best to avoid strenuous activities (bending, lifting, participating in sports, exercise classes, etc…) on the day immediately following any extraction.
With comparatively more involved surgeries:
- Strenuous activities should be avoided for the next several days, with their resumption eased into as you feel up to them.
- A patient might take 1 to 2 days off from their normal duties, returning to work or school after they feel recovered.
This link leads to our page that discusses Taking time off after extractions. It provides further details and guidelines.
Be cautious with eating.
It makes good sense to shift your eating activities over to the other side of your mouth for a few days. You may find that you do this subconsciously anyway because your extraction site is a little tender.
It’s also not a bad idea to choose relatively softer foods, as opposed to hard or crunchy ones that might inadvertently slip over to the wrong side and jab, poke or otherwise irritate your wound.
Overall, it’s important to maintain proper nutrition and stay well hydrated. Doing so will help you regain your strength, as well as promote more rapid healing. So, if possible, try not to miss any meals. And make sure to drink 6 to 8 glasses of water (roughly two quarts) each day.
Alcoholic beverages.
The metabolism of ethanol leads to the formation of compounds and molecules that can damage healthy tissues. As such, almost all phases of extraction site healing are adversely affected by alcoholic beverage consumption. Therefore, avoidance makes the best plan.
Smoking.
Do not smoke following your extraction. A minimum of 3 days, and preferably 7 days, is generally recommended if total smoking cessation is not possible.
▲ Section references – Politis
Cleaning your teeth.
During the days following your extraction you will need to clean your teeth. Just don’t be too aggressive with your toothbrush or floss.
- With routine extractions, during the first few days following your procedure just do the best that you can. You don’t want to be so vigorous that you risk scraping your wound.
- In the case of surgical extractions it’s best to avoid brushing or flossing in the area of the site altogether for the first 3 days, so not to dislodge any tissue flaps, stitches or dressings that have been positioned or placed.
Over the first several days following your extraction you’ll probably find that if you’re too aggressive with your toothbrush the newly forming tissues in your wound will bleed easily (a small amount of blood, short duration).
▲ Section references – Politis
2) Keep your extraction area clean by rinsing it.
In general, the cleaner you keep your extraction site the quicker it will heal.
- Beginning 24 hours after having your tooth pulled, you can gently rinse the area after meals, snacks and before bed (on average, 4 to 5 times daily).
- Don’t be too vigorous. Doing so may disrupt the blood clot or new tissue that has formed.
Guidelines for extraction-site rinsing.
- Adhere to your dentist’s recommendations.
- Gentle rinsing is usually only begun after 24-hours post-op.
- A routine of after meals and before bed, for several days, is common.
- Avoid using mouthwash.
- Saline solution (saltwater) makes a good choice.
- Vigorous rinsing will disrupt your wound and must be avoided.
- Only “irrigate” your extraction site if instructed to by your dentist.
Print out. Add notes while reading this page.
What should you rinse with?
What does rinsing accomplish?
It’s a way of gently cleansing the wound. This includes the removal of necrotic tissues being sloughed off as part of the healing process, microorganisms, and food and other debris that has accumulated in the area of the wound.
For how many days should you rinse?
As the healing of your wound progresses, the need to rinse it gradually diminishes. Performing your duties for just several days is usually sufficient. However, if your extraction site tends to trap debris, you should extend your routine accordingly so to keep it clean. (Also, see our next section about socket “irrigation.”)
3) Extraction site irrigation.
In cases where a patient’s post-surgical wound is large and/or deep (such as after an impacted wisdom tooth has been removed), food, microorganisms and other debris may tend to accumulate and be difficult to remove just by rinsing. If so, the extraction site may require daily “irrigation.”
This process is used to gently flush away debris that may:
- Interfere with healing.
- Be the source of a foul taste or smell.
- Create an environment that promotes the formation of a secondary bacterial infection.
When should you start irrigating?
You’ll simply need to follow your dentist’s instructions.
- Irrigation isn’t started immediately following your surgery but instead is delayed until at least several days of healing have taken place.
- Once started (per your dentist’s instructions) it’s typically continued for 1 to 2 weeks as the bone healing process starts to fill in and smooth out the divot that was your tooth’s socket. Timeline.
Irrigation technique.
Socket irrigation involves the use of a syringe that has a curved or bent, blunt-ended tip instead of a sharp needle. It’s filled with saline solution (saltwater, 1/2 teaspoon of table salt in one cup of warm water), or even just lukewarm tap water.
The tip is placed at the opening of the tooth socket and the syringe is slowly expressed so its fluid floats accumulated debris to the surface and away. It’s not a forceful activity but instead one that creates a gentle flushing.

If stitches have been placed, ask “if and when” they should be removed.
4) Stitches.
Removing stitches is easy and painless.
Non-resorbable stitches are usually removed 7 to 10 days after they were placed. The process of removing them is usually painless and very easy. Here’s how it’s done.
5) Antibiotics.
If your dentist feels that the use of an oral antibiotic is indicated following your extraction, they will provide you with a prescription for one. If antibiotics had been prescribed prior to your extraction procedure, you should continue and take the full course as originally directed.
If you notice any side effects from taking your medication, including skin rash or itching, discontinue its use and contact your dentist immediately.
Use this link for more information about the use of Post-extraction antibiotics.
B) Managing post-tooth extraction complications.
Related page: How can you tell if you’re developing complications?
1) Prolonged bleeding.
From the point when your tooth has first been removed there will be noticeable bleeding from your extraction site. And it can be expected to continue on, possibly for several hours.
But the level of flow that you notice with time should be ever diminishing. And overall, an extraction site’s bleeding can be expected to be well controlled by the end of the first day. (Related content: Extraction-site bleeding – The first 24 hours. What to expect.)
Prolonged/renewed extraction-site bleeding (24-hr post-op and beyond).
- [Bleeding is usually controlled during the first 24-hrs post-op.]
- Minor low-level bloody oozing isn’t uncommon.
- Bleeding on provocation is common and must be avoided.
- Extraction-site bleeding is best controlled by biting on moist gauze for an extended period.
- Advise your dentist of prolonged/renewed bleeding issues.
- An accurate report of bleeding color and quantity aids them in interpreting your condition.
At the point 24 hours after your surgery and beyond, any bleeding you notice should be just minor. As examples:
- You might find a low level of bloody oozing or seepage coming from your extraction area.
- Physical trauma (like that caused by eating, or brushing around or touching your wound) may trigger a minor amount of short-lived bleeding.
If you notice anything more, you should contact your dentist’s office so they can evaluate your status.
In the mean time, biting on gauze like you did during the first day of your surgery (see link above for directions) will help to minimize the amount of bleeding that occurs, and may even provide the needed solution for your situation.
You’ll need to make an accurate report to your dentist.
When trying to evaluate what level of emergency exists, your dentist will need an accurate description of the color and quantity of bleeding that has occurred.
They know that a small amount of blood mixed in with saliva will create a reddish fluid. But this type of pink-colored bleeding is quite different, and represents a far lower quantity of flow, than if the color of the bleeding you’ve noticed is dark red.
Be as accurate as you can when describing what you’ve experienced to your dentist so they’ll know what level of attention you require.
2) Swelling.
Trauma created during the tooth extraction process can cause postoperative swelling. Any swelling that does occurs usually reaches its peak between 24 to 48 hours after your surgery.
(We now cover this subject on its own page: Post-tooth extraction swelling. Prevention | Managment)
3) Bruising.
While somewhat infrequent, some patients will notice facial bruising following their extraction procedure. This is considered a normal postoperative occurrence. Its formation is not a sign of developing infection.
Signs and symptoms.
- It typically follows occurrences of tissue swelling, with the bruising first becoming apparent 2 to 3 days following the person’s extraction procedure.
- Its color can be black, blue, green or even yellow. It often starts off darker, and then transforms and fades as the bruise gradually resolves.
- Characteristically, it just appears on the same side as the person’s extraction. While it most often forms in the tissues that lie over or adjacent to the surgical site, it’s not uncommon for it to also appear in, or migrate (travel) to, other areas. This can include to your eyes or down your neck (with it possibly even sinking down to your chest).
(The size/extent of the bruising is related to the quantity of pooled red blood cells that have oozed from your surgical area. The bruise’s color/intensity is due to the color of these cells and pigments that are released from them as they are broken down by your body. Movement of the bruise occurs as this collection of cells and breakdown products travels along body tissue planes.)
Managing post-extraction bruising.
- Don’t be overly alarmed, bruising is not that uncommon.
- Over time, its shape or positioning may change.
- As healing progresses, its color will fade.
- Full resolution can take 7 to 10 days.
- Moist-heat applications (20 min. on/off), begun 3 to 4 days post-op, can speed up resolution. (See Swelling directions above.)
- Even without treatment, bruising can be expected to resolve uneventfully on its own.
Treatment.
Other things to know.
- Bruises may appear following oral surgery, no matter how gentle the procedure.
- It may be more extensive with elderly patients, or those who take blood thinners (aspirin, anti-inflammatory medications, warfarin [Coumadin]).
4) Sinus precautions.
If you’ve had a back upper tooth removed, avoid activities and situations that create pressure in your sinuses.
For example, don’t blow your nose for several days following your procedure. If you must sneeze, do so with your mouth open. Other events and activities (like playing a musical wind instrument) need to be considered to be risky too. Consult with your dentist about your plans.
What’s the concern?
The bone that comprises the floor of your sinus and the outline of your tooth’s socket may be one and the same in some regions and just paper thin. Excessive pressure differences can rupture this fragile layer and result in what’s termed a sinus communication.
5) Managing post-extraction pain.
It’s not uncommon to experience some level of pain during the first 24 hours following your extraction What’s common. | Management. and for the following few days. But by at least 72 hours postoperatively (the completion of day 3 after your surgery) you should notice that its intensity has begun to subside. In those cases where it hasn’t, you should be in contact with your dentist so they can evaluate your situation.
Pain that persists may be a sign of an underlying problem. One common one is the formation of a dry socket (see next section). Other causes can be: 1) Postoperative infection. 2) Retention of root, bone, or foreign body in the extraction site. 3) Jawbone fracture. 4) Sinus problems. 5) Pain from adjacent teeth. 6) Muscle spasms (see below).
Using oral analgesics –
OTC (nonprescription) pain relievers.
Most extraction procedures that haven’t required additional surgical steps Tissue flap, Bone removal. cause just minor postoperative discomfort. The pain experienced is typically self-limiting and well-managed with over-the-counter (nonprescription, non-narcotic) analgesics.
For those for whom it’s a permissible medication, the OTC pain reliever ibuprofen (Advil, Motrin, or generic) usually makes the best choice. For those who can’t tolerate ibuprofen use, acetaminophen (Tylenol or generic) can provide an alternative.
Note: Consult your healthcare professional before taking any medication to confirm that it’s safe and appropriate for your use. Use medications only as directed.
Prescription pain relievers.
If your dentist anticipates that you may experience severe discomfort, they will prescribe a pain medication for you (frequently a narcotic). Once again, you must follow all of the product’s associated instructions and precautions.
At that point where your level of discomfort has begun to diminish, the use of one of the OTC products mentioned above may then prove satisfactory. If so, it’s wise to do so. It’s fairly commonplace for people with narcotic dependencies to report that their first experience with this class of drugs was following a dental procedure.
Home remedies.
The application of ice packs on the face in the region of a person’s extraction site may help to control their post-procedure discomfort. The steps followed would be similar to using ice packs to minimize post-op swelling. Directions.
The best preventive for dry socket formation is proper blood clot care and protection.
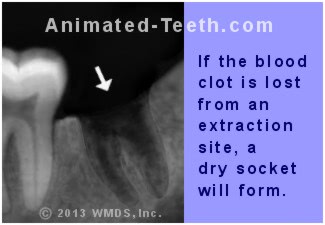
Symptoms of a dry socket include throbbing pain and a foul odor associated with the extraction site.
6) Dry sockets.
We’ve dedicated an entire topic to this subject. You can access it here: Dry sockets – Causes, symptoms and treatments.
7) Bone sequestra and tooth fragments.
Initially after your extraction your tongue may discover hard projections in the area where your tooth was removed. At this point in time they are unlikely to be missed tooth roots but instead the exposed bony walls of your tooth’s socket.
These types of rough projections will typically take care of themselves (smooth out or round over, become covered with new gum tissue) in the days that follow. If not, let your dentist know and they can smooth them for you.
Tooth or bone fragments.
Some patients may discover small bone chips or tooth fragments that have risen to the surface of their extraction site. These bits usually first appear many days, or even several weeks, following the extraction process. We cover this subject in detail here: Post-extraction bone chips & tooth fragments. Causes | Treatment
8) Prolonged numbness (paresthesia).
As a post-surgical complication, some patients may notice persistent numbness following their procedure. Dentists refer to this as paresthesia and it is typically a result of nerve fiber trauma experienced during their extraction procedure.
Following your extraction, you can expect to experience continued numbness for the next 2 to 4 hours, which will finally just fade away. Less frequently, a longer-acting anesthetic may have been used for your case.
If you notice numbness beyond the expected time frame, let your dentist know so they can monitor your situation. In most cases, a patient’s paresthesia is transient, although it may persist for some weeks or months before resolving.
This link discusses this issue in greater detail Dental Paresthesia.
9) Jaw soreness / Muscle spasms.
After your extraction you may experience pain or spasm with the muscles that operate your jaw, or jaw joint soreness. If you do, a number of factors during your extraction process may have helped to cause this:
- Fatigue and irritation associated with prolonged mouth opening.
- Aggravation of a previously existing jaw joint (TMJ) problem.
- Irritation associated with receiving local anesthetic injections (dental “shots”).
Treatment.
You’ll need to seek advice from your dentist for a specific recommendation about what type of treatment is needed. In most cases, it’s directed toward:
- Obtaining muscle relaxation.
- Reducing inflammation of the involved joint or associated muscles.
This is typically accomplished by:
Post-extraction jaw stiffness/spasm checklist.
- Perform 20-minute moist-heat (warm) applications several times per day.
- A course of OTC NSAID medication can aid in reducing pain and inflammation.
- Limited stretching/mobility exercises can assist in regaining function.
- Look for significant improvement over the course of a week.
Management of post-extraction jaw stiffness/spasm.
- Applying warm, moist heat packs (compresses) to the area.
For example, fill a water bottle with warm (not hot) water and then wrap it in a moist dishtowel. Apply to the affected area for 20 minutes. Repeat several times throughout your day.
- Using nonsteroidal anti-inflammatory drugs to minimize pain and reduce inflammation.
Dentists frequently recommend taking ibuprofen (Motrin®, Advil®) continually over the course of a few days (for example, dividing the maximum daily recommended dose of the product [or less] into 4 equal doses, one of which is taken every 6 hours). You’ll need to read and follow all directions, guidelines and warnings that accompany whatever product is utilized.
- Performing stretching exercises to regain jaw function.
Create slow, gentle motions that simply help to regain function as opposed to pushing and stretching limits. For example, perform opening-and-closing and side-to-side motions for 5 minutes, 3 or 4 times a day. Moderate, gentle gum chewing can also be a helpful exercise.
Extreme stretching and excessive or forced testing will tend to trigger continued muscle and joint irritation.
In most cases, a patient’s condition will subside in 5 to 10 days.
Follow-Up Appointments.
If your dentist feels that a follow-up appointment is needed, they will tell you and probably go ahead and appoint you at the completion of your visit.
For most extractions, a second visit will not be required. (That does not mean however that you shouldn’t contact your dentist if you have questions or a need.) The most common exception would be removing stitches. But this is only required if they have been placed, and if they are not a type that will dissolve away on their own. (The topic of suture removal is discussed above.)
Your dentist’s emergency contact information.
At the completion of your appointment, make sure your dentist has given their emergency contact information to you. If you feel that you need their assistance, you should not hesitate to contact them. Providing postoperative care is a part of their obligation (ethical and legal) to you as your treatment provider.
Post-extraction symptoms that may signify developing complications.
- Swelling that increases in size beyond 48 to 72 hours post-op.
- Pain that 2 to 3 days postoperatively shows signs of increasing rather than gradually subsiding.
- A foul mouth taste or odor.
- Your temperature rises above 100.5 degrees (F).
- You notice side effects from medications, including the formation of a rash or itching.
If you experience any of these signs or symptoms, you should contact your dentist so they may evaluate them.
Looking for more information?
Most people who have read this page tend to select one of these pages as their next read: Is your extraction site healing properly? – How to tell. or Normal extraction healing timeline. – What to expect.
If instead you’re looking for more detailed information about a specific postoperative issue or complication, select from this menu: Tooth Extraction Guides.
Last reviewed: April 20, 2026
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
McGill University Department of Oral & Maxillofacial Surgery. Surgical Teeth Extractions Post-Operative Instructions.
Politis C, et al. Wound Healing Problems in the Mouth.
University of Michigan Department of Oral & Maxillofacial Surgery. Tooth Extraction Post-Operative Instructions.
University of Rochester Eastman Institute for Oral Health. Postoperative instructions following dental extraction surgery.
University of Washington Department of Oral & Maxillofacial Surgery. After your oral surgery.
Video transcription.
Hello, welcome to Animated Teeth.com and our discussion of post-extraction instructions that apply to the time period starting 24 hours after having your tooth pulled and then the days beyond. In this video, we’ll highlight some of the more important issues covered on this page.
At this point, now a full day following your procedure, you should find that the bleeding from your extraction site is well controlled. That doesn’t absolutely mean that there won’t be a slight amount of bloody oozing seeping from the area. But what you notice should be drastically different from what took place on day one.
If instead you notice continued or renewed bright red flow, you should let your dentist know. In the meantime, using day one’s technique of applying pressure to the area of bleeding for an extended period of time via a wad of gauze or teabags should be resumed.
Pain may be an issue for some patients during the days following their extraction. However, not everyone will find this to be true.
Your dentist will have an idea of the level of discomfort you’re likely to experience. And at the end of your procedure will most likely discuss over-the-counter pain relievers with you. The use of ibuprofen, also called Motrin or Advil, is frequently recommended. They may also provide you with a prescription pain reliever if they feel that there may be a period when something of that caliber is needed. Keep in mind, all medicines come with directions and warnings, so you’ll need to pay attention to them.
Overall, the general course of events you should notice is one where with each passing day your level of discomfort is ever gradually diminishing. If you find differently, then you’ll need to let your dentist know.
Until your wound’s healing process is well underway, you’ll want to favor your extraction site so not to disrupt it.
Of course, you’ll need to resume eating and drinking so you can maintain proper nutrition and hydration. And maintaining adequate oral hygiene is important too. But as you start to bring these activities back up to speed, always keep in mind the goal of protecting your extraction site.
So, do your eating on the other side of your mouth and choose comparatively softer foods, like having peas, mashed potatoes, and meatloaf as opposed to a meal that includes chips, hard raw vegetables, and meat you have to cut up with a knife.
When cleaning your teeth, especially during the first few days, stop at those at either end of your extraction site. As for keeping your wound clean, your dentist may give you instructions about dislodging debris with gentle rinsing starting a day or two after your procedure.
The new tissues that initially form are fragile and vascular. So, if they do get bumped or scraped, don’t be overly alarmed that they bleed easily. Although, this should just be minor and transient, as well as a warning for you to not do what you just did anymore.
During the first few days of this portion of your recovery period, you’ll need to transition the way you handle swelling that’s taking place. We discuss what you need to do in greatest detail on our separate page that explains the management of post-extraction edema, so look for that.
Generally, you can expect the swelling that forms to peak somewhere between 48 and 72 hours following your procedure. Then, from that point on, it should slowly resolve.
So, up until it reaches its maximum, cycles of cold application will help to stymie its formation. After that, cycles of moist heat application will help to bring your swelling down more quickly. If your pattern seems to vary from the norm, let your dentist know.
If any stitches were placed in your wound, and they are a type that will not dissolve away on their own, your dentist will need to remove them. A common time interval to return to their office for this simple service is 7 to 10 days. Look for our additional pages that discuss issues associated with sutures for more details.
Once again, as days pass, the general trend should be one where you notice gradual and continued improvement in your condition. Your pain should be ever diminishing. Your wound filling in and healing over. And after the first two or three days, any swelling starting to subside.
Of course, there are additional things to know, both in terms of dos and don’ts and what to watch out for, so make sure to read through both this page and its linked information.
If you notice anything that seems to vary from your slow march to full and uneventful healing, it could be that some type of complication is involved, a subject we also address on this page. If so, don’t hesitate in contacting your dentist. They’re the one in the best position to interpret your symptoms.
We’ll also point out that, as the provider of your extraction procedure, they have an obligation, and no doubt a strong willingness, in assisting your needs during your healing process that follows. So don’t hesitate to contact them. They’d be disappointed if you didn’t.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
Pain at surgical site.
I made a bony impacted canine surgery where the doctor told me it was not an easy one and a lip repositioning one 7 days ago and the dentist told me that sutures should be taken off 2 weeks after the surgery .At the first 3 days the pain was not that much hard but at day four it started to become very painful and ubearable the pain radiates from my upper jaw at the surgical site to my teeth. I NEED TO KNOW THE REASON AND WHAT IS THE TREATNMENT PLZ ? and a last question is it normal to have swelling at one side of my lip at day 7 ? thank you
Lynn
Reply –
The only question we can give you much of an answer on is the swelling. In most cases, post-extraction swelling should start to subside around day 4. By day 7 it has usually resolved. In all cases, persistent swelling should be evaluated by your dentist.
As far as the cause of your pain, the timing of it and its “radiating pain” nature are reminiscent of a having dry socket. But as far as actually determining what your condition is, once again, you’ll need to consult with your dentist. All dentists expect patients to contact them as complications develop, so you should take advantage of that and let them provide the attention you require.
Staff Dentist
Comment –
Bottom back tooth pulled.
It’s been a week and I have exstream pain it feels like part of the tooth is still in the front is there any way to tell if it’s still in there it was infected when it was pulled and he had to drill to get it out took a very long time the pain is close to being as bad as before it was pulled
TS
Reply –
You need to call your dentist’s office and let them know that you require attention. They’ll figure things out, and take steps that will help to keep you more comfortable in the mean time.
You mention “.. had to drill to get it out took a very long time…”
Difficult, traumatic extraction are more likely to result in dry socket formation. We wouldn’t be surprised if you have developed one. Again, the solution lies with treatment from your dentist.
Staff Dentist
Comment –
Premolar pulled.
Yesterday i had my upper left 1st premolar pulled . I felt alot of pressure on the right upper molars during the process, is that normal? Also today, i’m getting a lot of pain in the left upper canine an 2nd premolar. What should i expect and do?
Alie
Reply –
In all cases, a person should contact their dentist’s office if they have questions or need help. That’s their obligation to you. They expect you to. Their knowing your case history and health history are important factors in determining where the needed solution lies.
“I felt alot of pressure on the right upper molars during the process, is that normal?”
Generally an event involving a tooth on one side of the mouth doesn’t refer sensation to a tooth on the other side of the mouth because the nerves that run to the left and right teeth are independent of each other.
“i’m getting a lot of pain in the left upper canine an 2nd premolar”
It’s common that extraction sites have pain associated with them.
As neighboring teeth, possibly these teeth were inadvertently traumatized as part of the extraction process and are sore for that reason.
You need to contact your dentist. In the case where their direct attention isn’t possible, their recommendation about OTC pain relievers or their calling your pharmacy can usually provide a solution until they can. But as mentioned above, knowing your case and medical history would be important to know.
Staff Dentist
Comment –
After tooth extraction pain.
How long after a tooth extraction is it possible to have “dry socket” pain?
JVL
Reply –
We have a whole series of pages that covers the topic of dry sockets, including how long they may last. We hope your recovery is as speedy as possible.
Staff Dentist
Comment –
After removal of impacted wisdom tooth.
Sir around 1week ago it got extracted. After a short surgery still there is a little swelling n pain n couldn’t open mouth fully how long will it take by tommorw mi sutures will be cut.
Soni Sharma
Reply –
You should go ahead and contact your dentist’s office and report your symptoms. As the only one who knows the specifics of your case, they would be the only one able to give you any sort of specific explanation about what might be expected.
Here’s our page about the normal timeline associated with extraction site healing, and then this page covers symptoms encountered during the healing period following your extraction.
Staff Dentist
