Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
How painful is having a tooth pulled? – (How bad does having an extraction procedure hurt?)
Tooth extraction procedure pain.
Will it hurt when you have your tooth pulled?
No, you don’t have to expect that having your tooth pulled will hurt. But we’d be leading you astray if we said that getting one taken out never did. And that, basically, is what this guide is all about.
- We explain the types of sensations that are usually felt when teeth are extracted.
- Provide details about the always disappointing, hopefully just minor, pain sensations that may be experienced during a patient’s procedure and why they’re felt. (Along with statistics about what percentage of patients have a painful experience.)
- What you and your dentist can do to create a comfortable, trusting environment for your extraction process. One that is as pleasant and pain-free as possible.
(Check out this page’s Table of Contents for a complete list of its topics.)
This guide provides you with the facts you need to know to determine what is normal. That way, if something feels off during your extraction process, you can confidently signal your dentist so they can address your situation immediately. This proactive approach shifts you from passively enduring the procedure to actively guiding it, making for a smoother, more comfortable experience.
What do patients usually feel when they have a tooth pulled?
Here are some of the routine sensations you should expect to experience during the extraction process:
- You may feel the pinch of the needle as your dentist numbs up your teeth and gums.
- You will feel the back-and-forth pressure that’s used to loosen up your tooth until it’s free enough to come out. (It’s important not to confuse this pressure with feeling pain, many patients do.)
But other than those two items, the odds favor that you won’t feel anything else significant during your procedure.
So, patients never feel pain?
No, research studies do show that a small percentage of people report experiencing pain during their extraction procedure. However, this isn’t entirely unexpected.
Each case is, of course, different.
Every patient, their tooth, and their overall case is unique, and as such, some patients will require extra care or additional measures beyond what their dentist initially expected was needed to ensure their comfort during their procedure.
That’s precisely why dentists:
- Test for numbness at the beginning of every patient’s procedure.
- Prearrange an unambiguous “it hurts” signal with their patients so they’re immediately alerted if something has gone amiss.
So, even if pain is felt, what you experience should be just brief and minor. And then, once your dentist knows that additional steps are needed, they can go ahead and proceed with them.
Here are more details about what to expect during your procedure …
What painful events may be felt during an extraction?
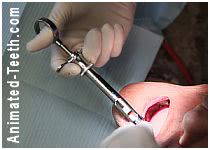
Numbing up a tooth for extraction.
1) Numbing up your tooth.
Both your tooth and its surrounding bone and gum tissue must be numbed up.
What may be different with an extraction as opposed to other dental procedures is that all of the tissues that surround your tooth (its gum and bone tissue) must be anesthetized too. In comparison, for a lot of dental procedures, like routine fillings, just numbing up your tooth may be enough.
That means with an extraction you may end up getting more total shots, and therefore have more potential for feeling needle pricks, than you’ve experienced before. But as far as the way the injections are done, it’s all pretty much the same as with other dental procedures.
Use this link to access our page that explains details about getting dental shots (types of injections, the way they’re given, which hurt the most, etc…). Jump to page.
2) Your dentist testing to see if you do feel pain.
Once your initial round of injections has been completed, there’s no reason why you should expect to feel any pain for the remainder of your extraction procedure.
Having said that, there can be times when this initial round hasn’t numbed up the tooth or its surrounding tissues enough. That’s never the dentist’s intention. It’s just something that statistically can happen.
a) How does a dentist test for numbness?
Since a dentist knows that some percentage of people will need further numbing, they’ll follow a protocol that’s designed to test and evaluate their patient’s status before the work of actually removing their tooth is begun. That way whatever level of pain is felt is kept to a brief, bare minimum.
Here are some of the ways they’ll evaluate and test, with each method explained in greater detail below on this page.
How a dentist checks for numbness before proceeding with an extraction.
Print out this list.
Discuss its points with your dentist.
- i) Asking what “lip signs” (lip numbness) you notice.
- ii) Deliberate finger manipulation of your tooth to test for discomfort.
- iii) Testing your gum tissue for pain response.
- iv) Easing into the extraction process, so to see how you’re doing.
Of course, each of these last three tests means that you’ll need to have an agreed-upon “it hurts” signal so you can communicate what you feel accurately. Here’s more information …
i) Does your lip feel tingly?
Your dentist knows the specific portions of your mouth that each type of injection they give should numb up. And they’ll quiz you about how these areas feel to see if they have.
For example, before extracting lower back teeth a dentist will usually ask their patient if their lower lip feels tingly. That’s typically a sign that the anesthetic that’s been given has been effective.
But this type of questioning about how things feel is only valid in some situations. For example, the injections used to anesthetize upper back teeth may have been fully effective without causing much change in the way the adjacent lip or cheek tissues feel at all.
ii) Pressing and wiggling on your tooth.
- Since teeth are extracted by way of applying forces to them (via the use of dental instruments such as forceps and elevators How they’re used.), the pressure of this testing somewhat replicates what you’re in store for. If you feel discomfort now, you would during your tooth’s removal too.
- This test also gives you an introduction to the sensation of pressure that you can expect to feel during your procedure.
Being able to distinguish between pressure and pain (and understand that the two are unrelated, see discussion below) is a big deal. There’s nothing more important for the patient to be able to comprehend and differentiate during their extraction procedure than the issue of pain vs. pressure.
iii) Testing your gum tissue.
A dentist knows which areas of your mouth should have been numbed up with the anesthetic they’ve given you. So as a test, it’s common for them to use a pointed dental tool and deliberately poke your gum tissue in those areas, just to make sure you don’t feel anything (other than possibly the pressure involved).
Just so you’re not surprised or confused, we’ll state that where they test may be some distance from the tooth that’s going to be taken out. (For example, they may test your lower lip even though it’s a back lower molar that will be pulled.)
iv) Testing as your extraction gets started.
- One of the first steps of the extraction process involves the dentist using a tool to detach (strip away) the gum tissue surrounding the tooth.
Your dentist will be gentle as they first start to do this, so they can test out how you’re doing. Then once they’ve confirmed that you’re feeling no pain, they’ll continue on with this task in earnest.
- Likewise, when a dentist initially begins the process of loosening up a tooth, they’ll ease into applying full pressure. That way they can look for confirmation from you that all is going well.
Setting up an “it hurts” signal.
Even with all of the checks mentioned above, it’s still possible that your tooth isn’t as numb as it needs to be and you will start to feel some degree of pain (hopefully just minor) as your extraction procedure gets started up.
Creating a trusting relationship by setting up an “it hurts” signal in advance.
Due to the uncertainty of knowing what the patient will feel, it’s basic protocol for a dentist to set up a signal with their patient. A sign that can be used to unambiguously communicate to them that something is amiss, even when you are unable to speak.
- One common signal is simply having the patient raise their hand immediately upon noticing that something isn’t right.
- Even when this motion isn’t in the dentist’s direct line of vision, their peripheral vision will easily notice this type of signal.
The agreement between the dentist and patient should be one where work is stopped upon the signal without hesitation. That way the patient is guaranteed that if something does hurt it’s kept to a minimum and just minor levels.
3) Pain felt during your extraction procedure.
Despite their best efforts, you may discover that your tooth and/or surrounding tissues haven’t yet been numbed up enough. You might notice this as your dentist first tests for adequate numbness before beginning your procedure, or else during the extraction process itself.
How likely is it that your first shots won’t be totally effective in numbing your tooth?
A couple of papers have investigated this topic. And while the numbers they’ve reported may not be entirely reassuring, with just a little explaining you’ll find they aren’t really as bad as they initially seem.
Study: Wong (2001)
Title: Adjuncts to Local Anesthesia: Separating fact from fiction.
This paper reviewed published literature that had evaluated the subject of:
- Numbing up lower molars. (Probably the most challenging teeth to numb, per Nusstein [reference linked above]) …
- … by way of using conventional dental shots. (An inferior alveolar nerve block [“IANB”]. Types of dental injections.)
This review concluded that the use of conventional methods (IANB injections) to numb up asymptomatic molars (teeth that weren’t hurting at the time of their extraction) was only successful 69% of the time.
Study: Kanaa (2012)
While this paper focused on a different topic, it contained a section that provided background information about this subject. It cited two studies that placed the effectiveness of initial rounds of anesthesia for lower teeth at 63% and 76%.
Your dentist is quite aware of the possibility of numbing failure.
A person could look at the figures above and have some concerns about how painless their procedure will be. After all, those statistics suggest that about one-fourth to one-third of patients being prepared for a tooth extraction won’t be adequately numbed up after getting their initial injections. [At least with lowers. The numbers are likely higher for upper, usually easier to anesthetize, teeth.]
Don’t think for a second that your dentist doesn’t recognize the potential for this problem. And with all extractions, not just lowers. That’s why they use a protocol laden with evaluation and testing aimed at identifying ahead of time those patients whose situation requires further anesthesia.
Actually, this is the way you want it to be.
As much as you don’t want to feel pain during your extraction procedure, what you also don’t want is for your dentist to initially administer more anesthetic than is reasonably expected to be required. That’s because doing so can lead to complications:
- Administering more than that quantity that was needed to be effective serves no purpose.
- Administering more will require additional shots, some of which might be felt.
- There are limits on the total amount of anesthetic solution that can be safely used with a patient. (Maximum dosages are typically based on the patient’s weight.)
Having expended most of this quantity needlessly can jeopardize the procedure if later on pain control becomes a problem, or if the procedure runs long and the anesthetic that’s already been given begins to wear off.
Numbing up “hot” teeth for extraction can be even more difficult.
The numbers reported above are for numbing up asymptomatic teeth (teeth that weren’t hurting at the time of their extraction).
The more difficult challenge is when dentists numb up “hot” teeth (teeth that are painful because they are experiencing irreversible pulpitis).
- The review of published literature mentioned above (Wong (2001)) determined that only 30% of initial attempts at numbing up extremely sensitive (“hot”) lower molars using conventional methods (IANB injections) were successful.
- Not all studies put this number for “hot” teeth (numbed via initial IANB injections) so low. Research by Zain reported a 63% success rate for lower molars.
 The above-mentioned study by Kanaa (2012) found a success rate of 67% for lower teeth in general, not just molars.
The above-mentioned study by Kanaa (2012) found a success rate of 67% for lower teeth in general, not just molars.
Why these numbers really aren’t so negative.
The variation reported above withstanding, it’s doubtful that any dentist would dispute that numbing up “hot” teeth can be a challenge. And that point alone is where good news lies. It means they’ll know to take extra measures.
All dentists know that the use of adjunct (supplemental, extra) injections can improve the patient’s level of anesthesia (see statistics below). So, any dentist treating a “hot” tooth will know that these techniques are probably needed and therefore will go ahead and take these additional steps right off the bat. After all, your dentist doesn’t want your extraction to hurt any more than you do.
How much can adjunct numbing techniques help?
The Wong (2001) paper mentioned above also reviewed studies that evaluated the use of supplemental techniques with lower molars after an initial round of conventional (IANB) injections had failed.
- For asymptomatic teeth, success rates could be raised from 69% to 97% with the addition of adjunct methods.
- For “hot” teeth, the 30% number reported above could be raised to 83% effective.
That means with just routine discovery (all of the steps we mentioned above that a dentist takes to make sure that their patient really is numb), the vast majority of people can expect to enter the actual work of their extraction process having profound tooth anesthesia.
What happens if pain is felt during an extraction? – What additional steps can be taken?
For those patients who haven’t been adequately numbed up initially and have felt discomfort during their extraction procedure, a dentist has options available to them to resolve the issue. A paper by Nusstein details some of the options that dentists have when managing “hot teeth.”
- In some cases, they may repeat your initial injections.
The goal here is not simply placing more anesthetic solution but instead an additional quantity in a slightly different (more on-target) location in hopes that doing so will create a more profound effect.
- In other instances, some type of supplemental technique might be used. – This could include giving you a shot in an entirely different location or using a different injection method.
You may not feel these additional injections.
How much pain can you expect to feel during your tooth extraction?
Statistics from studies.
We found a couple of studies that evaluated intraoperative pain (discomfort experienced during the extraction process alone).
- Intraoperative pain was generally defined as discomfort that took place after giving the patient the shots needed to numb up their tooth. (Procedure discomfort that followed whatever level of injection pain might have been felt.)
- We’re of the opinion that this definition would include the following scenario: 1) after the tooth had been numbed, 2) the extraction process was begun, 3) pain was felt, 4) additional injections were given, and 5) the extraction process was then resumed and completed.
Research findings.
[Similar to those cited above, the studies discussed here evaluated the extraction of mandibular (lower) teeth using conventional methods (IANB injection), which is probably the most challenging numbing situation.]
Study: Kammerer (2012)
This study asked its 88 subjects who had lower molars removed to rate the level of pain they experienced during their procedure from 0 to 10, with 10 being the worst. The average of the scores reported was between 0 and 1.
Study: Bataineh (2016)
This study evaluated intraoperative pain levels (rated 0 to 100) experienced by 52 patients having lower molars removed.
- On average, the level of injection pain (IANB injection) was rated as 41 (the high end of the mild pain range).
- As for the level of pain experienced during their extraction, 81% of patients reported mild pain, 17% moderate pain and 2% severe pain.
- 89% of subjects reported that the level of discomfort they felt during their procedure was less severe than expected, 11% the same as expected and 0% felt it was greater.
- “… the intense pressure felt by some patients during the extraction, which may be difficult to differentiate from pain …”
Pain vs. pressure is a critically important distinction that the patient must be able to make. We discuss why in our next section below.
Study: Rousseau (2002)
Title: A Comparison of Pain Levels During Pulpectomy, Extractions, and Restorative Procedures.
This study evaluated 50 patients who rated their intraoperative pain from 0 to 100. Some of the extractions involved “hot” teeth. (These are teeth that were painful because they were experiencing irreversible pulpitis. As mentioned above, “hot” teeth are generally more difficult to anesthetize.)
- Preoperatively, the patients rated their level of pain as being 61 (defined as moderate pain).
- Postoperatively the patients were asked to rate their procedure pain. They rated it as 24 (defined as mild pain). (With this study, intraoperative pain was defined as including injection discomfort.)
Why it’s normal to feel pressure during your extraction.
What occurs.
The local anesthetics used in dentistry to numb up teeth and gum tissue are quite effective in inhibiting (conking out) the type of nerve fibers that transmit pain. But they’re not as effective on those that transmit the sensation of pressure.
And because of this, it’s normal and expected that you will feel the pressure, quite possibly a substantial amount of it, that your dentist applies to your tooth with their instruments as they loosen it up during your extraction process.
An explanation why.
The way our bodies are wired is that different types of nerve fibers, each of which transmits a specific type of sensation (pain, pressure, touch, hot and cold, etc…), have different physical characteristics.
And due to these differences (for example, the thickness of the protective insulating sheath that surrounds the nerve), local anesthetics are able to have a more profound effect on some types of fibers as opposed to others.
For the most part, fibers that transmit the sensation of sharp pain (the nerve responds intensely and quickly to painful stimuli) are the type most easily decommissioned by local anesthetic, hence this is the first sensation to be lost.
Following sharp pain is the loss of the ability to feel cold sensations, warmth, touch, and finally pressure, thus explaining why it’s usual and normal for it to be felt during an extraction procedure.
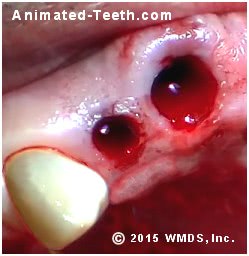
A dentist uses their tools to apply pressure to teeth so they loosen up and can be removed.
How much pressure will you feel?

Comparisons.
As it turns out, that’s a difficult number to find an exact comparison for. We did however discover that regulation basketballs and soccer balls are typically inflated to around 8 psi.
So if you think in terms of putting one of those balls on the floor and pressing hard enough on it to just slightly indent it, when having an upper front tooth extracted you could expect to feel about twice that much pressure.
What does tooth extraction pain feel like?
How to distinguish between pain and pressure during your extraction.
One common problem that occurs during tooth extractions is that patients sometimes confuse the sensation of pressure with pain.
Extraction pain vs. pressure – How to distinguish between the two.
Print out this list.
Discuss its points with your dentist.
- Some patients may not realize that it’s normal and expected for them to feel pressure, or they may not have anticipated the amount of it involved, and therefore mistake feeling it for experiencing pain.
- Patients may fail to realize that pain characteristically has a sharpness to it whereas pressure does not.
- The patient may incorrectly assume that because they feel increasing levels of pressure they will soon feel pain too.
Remember, these sensations are carried by different types of nerve fibers. Feeling pressure in no way indicates that your fibers that relay pain haven’t been successfully anesthetized (conked out).
Why making a distinction between the two is so important.
Being accurate in your interpretation of what’s going on (feeling sharp or shooting pain vs. pressure) is vital.
That’s because leading your dentist to believe that you are feeling pain instead of just pressure may lead them to needlessly administer more anesthetic.
- As explained above, administering more anesthetic will do absolutely nothing to alleviate the sense of pressure you are feeling.
- Using additional quantities of anesthetic places you at greater risk for complications during your procedure.
- Since only so much anesthetic solution can be given safely (based on the patient’s weight), administering some of this quantity needlessly could mean that little or none is available for use later on during the procedure (if needed).
- Responding to unwarranted patient complaints that have no solution simply draws your dentist’s attention away from the important task at hand (extracting your tooth).
Extraction pain frequently correlates with a patient’s anxiety level.
It’s important for us to mention that research has shown that the level of a patient’s anxiety about their procedure is a predictor of how much pain they will experience during it. This is true for any type of dental work but especially tooth extractions.
Here’s what studies have found:
Study: Fagade (2005)
Title: Intra-operative pain perception in tooth extraction – possible causes.
This paper evaluated 122 patients who had had extractions and found a positive correlation between patient anxiety scores and the level of procedure pain they experienced.
Study: Tickle (2012)
Title: Predictors of pain associated with routine procedures performed in general dental practice.
This study evaluated a group of 451 patients who had varying types of dental work performed (including extractions). Patients rated as “very anxious” were 5 times more likely to report experiencing pain during their procedure.
If you have anxiety about your extraction, make sure to let your dentist know.
A patient’s level of anxiety can be controlled via the use of various sedation techniques administered either before or at the time of their procedure. The decision to employ such methods is both the responsibility of the dentist and the patient.
- The issue should be brought up by the dentist during their pre-extraction examination and the patient’s options explained to them. (We discuss conscious sedation techniques here. Options.)
- The patient must then be willing to admit that they do have apprehensions and be receptive to the dentist’s suggestions and recommendations.
Looking for more information?
Consider one of these topics about the Tooth Extraction Procedure, or choose the “Full Menu” button to see a complete list of Extraction Guides we offer.
Last reviewed: April 23, 2026
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Ahel V, et al. Forces that fracture teeth during extraction with mandibular premolar and maxillary incisor forceps.
Bataineh AB, et al. Patient’s pain perception during mandibular molar extraction with articaine: a comparison study between infiltration and inferior alveolar nerve block.
Fagade 00, et al. Intra-operative pain perception in tooth extraction – possible causes.
Kammerer PW, et al. Comparison of 4% articaine with epinephrine (1:100,000) and without epinephrine in inferior alveolar block for tooth extraction: double-blind randomized clinical trial of anesthetic efficacy.
Kanaa MD, et. al. A Prospective Randomized Trial of Different Supplementary Local Anesthetic Techniques after Failure of Inferior Alveolar Nerve Block in Patients with Irreversible Pulpitis in Mandibular Teeth.
Nusstein J, et al. Local Anesthesia Strategies for the Patient With a “Hot” Tooth.
Rousseau WH, et al. A Comparison of Pain Levels During Pulpectomy, Extractions, and Restorative Procedures.
Tickle M, et al. Predictors of pain associated with routine procedures performed in general dental practice.
Wong JK. Adjuncts to Local Anesthesia: Separating fact from fiction.
Zain M, et al. Comparison of Anaesthetic Efficacy of 4% Articaine Primary Buccal Infiltration Versus 2% Lidocaine Inferior Alveolar Nerve Block in Symptomatic Mandibular First Molar Teeth.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
Extraction surgery.
I’m having a surgery in which the dentist will open up my gum to extract a permanent tooth. Obviously, anesthesia will be used. Will I feel much pain?
Rick
Reply –
Your procedure would probably be best described as either a surgical extraction or else the removal of an impacted tooth (akin to removing an impacted wisdom tooth).
Either way, short of any complicating factors [like an active infection (swelling/pain would be an indication) or acutely inflammed pulp (spontaneous pain could be an indication) (see “hot” teeth section above)] there’s no reason to expect that the local anesthetic your dentist uses to numb up your tooth won’t be effective, as it would be for any other tooth (the tooth’s position doesn’t affect which/what surrounding nerves connect with it).
Your procedure might be expected to be more involved than a routine extraction (longer duration, greater surgical difficulty). If so, you and your dentist might consider the use of some method of conscious sedation to help you tolerate your surgery better. But its use has to do with patient management only and not pain control.
Good luck, expect the best.
Staff Dentist
Comment –
Does it hurt getting teeth extracted?
For me it didn’t hurt as much as I thought it would! All they do is they first take a blue type of gel so your mouth will feel numb and tingly after a while. After, they asked me to close my eyes so they can give you the shot and the assistant held out her hand so I could squeeze it if I felt any pain. After that you will feel pressure when they take out the tooth(or teeth) but it doesn’t hurt at all! Finally, they give you a cotton that you bite down on and then your done!!
Aurora
Comment –
My experience.
When i first went to the dentist, i was scared. They put a numbing gel on my gums and told me to close my eyes for the shots. I had 4 shots and they did hurt, it felt really sharp, I have anxiety so as son as i felt the injection pain i was uncontrollably shaking and tears coming out my eyes. After they told me im doing well etc and they pulled out my teeth. I had 2 taken out and the whole procedure took around 10 minutes which was really good.
Alicia
Reply –
You mentioned you were scared about your procedure right right from the start. In hindsight, it seems your experience could have been made more pleasant via the use of some type of sedation technique.
The use of some medications requires some pre-planning, so they aren’t always an option. But a decision to use nitrous oxide (laughing gas) is often made right at the time of the appointment.
Staff Dentist
Comment –
Tooth extraction pain.
I got my tooth extracted a few hours ago. They told me I also had gingivitis.
They numbed my mouth which was good. The extraction was still painful though, I could hear and feel the tooth breaking as they were getting it out of my gum. I shut my eyes tight at those bits, and she kept asking if I were okay,, but I never told her to stop because I wanted to get through with the extraction asap. It hurt more than I thought it would. I have no idea why it hurt though even though they numbed my mouth.
Englan
Reply –
We’re glad for you that your extraction is over and you’re fine.
For people reading this comment we must point out the sentence “she kept asking if I were okay,, but I never told her to stop because I wanted to get through with the extraction asap.”
As we describe at length on this page above, insuring that a person’s extraction process is as pain-free as possible involves communication between the dentist and the patient.
In this situation the dentist was never offered the opportunity to provide additional anesthesia because the need for it was never communicated to them.
Staff Dentist
Comment –
Painless tooth extraction.
I just got a tooth pulled a few hours ago. They rubbed a gel around the tooth and gums . The Dentist walked in to give me injections to numb the area. He gave me two injections never felt them go in. They left the room for a few minutes while the meds took affect. When they came back he tested the area to make sure it was indeed numb. I felt when he poked the gum so they injected me one more time. After a few minutes he came back extracted the tooth .
Through out the procedure, I was asked several times if I was ok and to raise my left hand if I felt any pain. I asked what was injected forgot the name but it was the best stuff acts quickly and lasts for hours. I have severe anxiety and not once did I feel any pain from start to finish. I was however told to breathe after it was over. Best experience I ever had with a dentist
alpj
Reply –
Not every extraction process will be totally painless. But as alpj explains, if you give your dentist prompt and accurate feedback you tip the scales far in your favor of having a pain-free experience.
Staff Dentist
Comment –
I’m Getting My teeth pulled!
I’m 10 and my teeth are pushed out front. My dentist said that I have to remove 2 top teeth and 2 bottom teeth, so they can put braces on. Can you guys tell me what happens and if it’ll hurt?? On a scale of 1-10 (1:hurts so bad-10: No pain at all) Thanks
A.S.
Reply –
We like to think that people find that the whole experience is more pleasant than they might have expected.
While our pages aren’t exactly geared toward your age group (and instead more toward adults), you might choose to read through the following pages:
What’s the extraction process like.
And if you haven’t already, you should read this entire page. It answers questions like the ones you’ve asked.
Staff Dentist
Comment –
Too much for me.
I attempted to have my tooth extracted yesterday but I could feel like a cold sensation which too me felt like pain I was given 4 injections and was told told that I couldn’t receive anymore so I rescheduled the extraction for today and was told to eat before I go in. Was the cold sensation pain or heavy pressure. I had an extraction before and didn’t feel this pain should I request to be sedated if the same pain is felt today
Danielle S.
Reply –
As mentioned above, nerve fibers that carry different types of sensations have different physical characteristics, and for that reason are affected by dental anesthetics differently.
For the most part, pain fibers that feel sharp pain (respond intensely and quickly to a painful stimulus) are the type most easily affected (conked out).
Generally speaking, this is the order of effect that local anesthetics have on nerve fibers: Pain is usually the first to disappear, then followed by the loss of cold sensation, warmth, touch and finally pressure.
Only you and your dentist can sort this out. But as you suggest, if you think that anxiety may be influencing your interpretation of events, some type of conscious sedation technique may provide a solution.
We will point out that your post itself describes the sensation as thermal, not pain. Also, your dentist’s pre-extraction testing should have included some type of poking or prodding that should have served as a test for the evaluation of loss of pain sensation.
Best of luck.
Staff Dentist
Comment –
It hurt bad.
I have just had 2 teeth out they were loose and painful I had 2 injections in my gum , when the dentist started pulling the pain was so bad I grabbed her arm ,she then went straight on and pulled the next tooth out ,it wasn’t pressure, it was as if pulling the tooth out with no pain relief , never again I have had loads of teeth out but never had pain like that its put me of for life 🙁 why would this happen ?
Susan M.
Reply –
Sorry to hear about your bad experience.
You mention that you had “2 injections in my gum,” which implies that it was expected that depositing the anesthetic directly adjacent to the teeth would numb them (that’s common for certain teeth).
You also mention your teeth were “loose and painful.” That could be a description of teeth that have an associated infection, and generally speaking the presence of infection tends to inhibit the effectiveness of local anesthetics (the solution given via dental shots).
So possibly the underlying problem lay in the fact that while normal protocol was followed, the conditions in the tissue (infection) inhibited the effectiveness of the numbing solution. That’s not an uncommon scenario. And when it occurs, there are additional ways to anesthetize teeth.
The larger issue here is that it would be expected that the dentist’s initial pain-response testing would have identified the failure. And also there seems to have been no prior agreement of patient signals, or acknowledging the signals, that pain was felt.
As this page discusses, anesthetic failure is not terribly uncommon. But a dentist can use a protocol where the failure is discovered early, and hopefully after only minimal pain has been experienced, and then corrected.
Staff Dentist
Comment –
Worried.
Hello, I am 17 and tomorrow I need to get 2 baby teeth that haven’t came out yet. I never have gotten teeth pulled before so I am a bit nervous about it. I have braces on and need the teeth removed so my other teeth that are moving can keep straightening . One tooth is worn down on top near the back and the other is very small and on the bottom front area. Will it be quick and painless ? What’s the worst that could go wrong. Thank you
Keith
Reply –
Good luck with your procedure.
Focusing on the “worst that can happen” really isn’t the way to approach a tooth extraction. In fact, that train of though can easily enough result in a self-fulfilling prophecy.
We’d like to think that this page explains how patient and dentist activities and cooperation help to keep the potential for any unpleasantness to a bare minimum. It also provides study statistics about the frequency with which patients report feeling pain.
In your case, as positives, baby teeth are typically smaller than their adult counter parts. So removing them is often easier. Also, numbing baby teeth generally offers less of a challenge for the dentist than many adult teeth. So you have that going for you too.
As far as the “quick” question, we have a page that discusses how long it takes to get a tooth pulled. Good luck.
Staff Dentist
Comment –
Shots hurt.
I’ve had teeth pulled before and felt the usual pressure as they call it but no pain, other than injections to numb, until today. I had a broken tooth that had to come out. Was given the injections to numb which numbed one side. I begin to get concerned because the area around the gum was not numb but he gave more injections right before pulling and those injections hurt worse, however the numbing began instantly.
Vic
Reply –
You state:
… Was given the injections to numb which numbed one side. I begin to get concerned because the area around the gum was not numb …
We’re guessing this was a lower back tooth. If so, the purpose of the first injection the dentist gave (a manidibular block) was to numb the broken tooth and jawbone. The soft tissue to the side of the tooth is serviced by a different nerve.
Numbing both nerves at the same time would mask from the dentist if mandibular block injection had been effective or not, hence the needed wait time between the two shots. And if that second injection involved an area of “tight” tissue, yes it could pinch.
Staff Dentist
Comment –
What to expect?
I am due to visit my dentist tomorrow for check up 10 days ago my tooth broke off and all u can see is a filling it is next to my eye tooth it was a heavy filling i have a tiny wee stub of tooth left at top i also have receding gums and a lot of sensitivity an feel extremely anxious am i going to feel a lot o pain and will the filling just break as theres no enamel to grip onto.
Hg
Reply –
The whole basis of dental anesthesia is that it has its affect on the nerve that runs to your tooth at a point before it ever reaches inside of it. So what you visualize probably has very little, if anything, to do with whether or not your dentist can effectively numb up your tooth.
You mention you have receding gums. Generally that should be a positive thing for a tooth extraction (the tooth is possibly encased in a lesser amount of bone than it was previously).
If there is little actual tooth structure for the dentist’s forceps to grasp, they will no doubt rely more heavily on the use of their dental elevator for the removal of the tooth. If that proves difficult, they may need to take some surgical steps. That however is a positive event because it means by doing so (if needed) they will remove the tooth less traumatically.
You state: am i going to feel a lot o pain
A patient’s mind set almost always has the ability to trump the reality of their situation. You might ask your dentist about the use of conscious sedation for your procedure so you are more relaxed. For example, the use of laughing gas is a technique that can often be elected for right at the time of the appointment.
Staff Dentist
Comment –
Tooth extraction did not hurt at all.
One of my infected – yes – tooth was pulled out recently and got stiched. It was done very efficiently and no pain at all. The only thing was that the dentist had to drill the tooth first, i guess in pieces? so probably to take it out more easily. Nowadays the young dentists that I visit are such a good professionals and the systems are so developed, that there is nothing to be worried about. They even have relaxing music to calm down, and some dentists even sing to get the atmosphere more softer. But if they could do something for the sound of the drills then the experience would be even better, and people would not be so afraid to pay a visti to dentist every year.
Pia
Reply –
Thanks for posting about your positive extraction experience.
As points of clarification for anyone reading:
Infected teeth are routinely extracted. It’s simply a matter of the activity/extent of the infection and how its presence might affect the procedure or pose the patient for post-op complications, which is a judgment call made by the dentist.
You state “the dentist had to drill the tooth first, I guess in pieces.” Here’s more information about that process. It’s referred to as “sectioning” a tooth.
In regard to the sound of the drill, historically dental drills were air-pressure driven. And the air turbines in them have a characteristic whine. With electric handpieces, the sound that’s produced is less so. Sometime in the future, probably all dentists will use electric handpieces.
Staff Dentist
Comment –
Tooth extraction this week, and will it hurt?
I’m having a tooth extraction tomorrow on my second molar. I’m 14 and my teeth take a long time to come out so this tooth is the last one, but it just won’t come out. I loosened it so much where it is slightly loose now, although I feel like it has a huge root and strong one as well. My question is, since it has a huge root and it’s a molar, will the extraction hurt?
Peter
Reply –
There are really multiple issues you’ve brought up.
One is how easily your tooth will come out. No matter how it seems to you, a baby tooth won’t prove much of a challenge to your dentist who is used to pulling adult teeth. But even so, that issue doesn’t correlate with the level of pain felt.
The issue of potential for pain has to do with tooth numbing. With routine extractions, the nerve itself is numbed up totally exterior to the tooth, so whether it has a long or short root, isn’t really a factor.
A long or short root can correlate with the amount of extraction pressure needed to remove the tooth. But as this page discusses, feeling pressure is different than feeling pain.
You should do fine.
Staff Dentist
