Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
Wisdom Teeth Cavities: Should You Fill the Tooth or Pull It?
Wisdom Tooth Decay: Should You Pull It or Fill It?
Wisdom teeth (third molars) are especially prone to decay due to their location at the back of the mouth, making them difficult to reach and clean. When a cavity develops, it raises the question: should the tooth be filled or extracted?
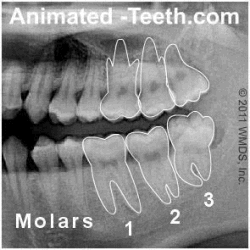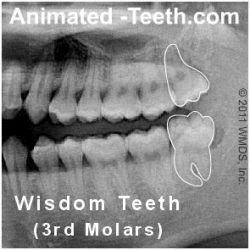
Wisdom teeth are 3rd molars and lie at the very back of your mouth.
Making the right choice in this situation hinges on several factors. This guide explores the key considerations dentists evaluate, the guidelines they follow, and the risks and benefits of both treatment alternatives.
Wisdom tooth cavities are a fairly common problem.
It only makes sense—because wisdom teeth (third molars) are located in a hard-to-reach area of the mouth, cleaning them can be extremely difficult, if not nearly impossible. As a result, plaque tends to accumulate on their surface, placing them at constant risk for tooth decay
An X-ray that shows
a wisdom tooth cavity.
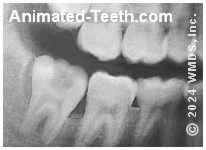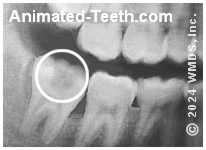
What happens if you get a cavity in a wisdom tooth?
Once a lesion has started, your dentist really only has two options. They can either recommend:
- Saving your tooth by way of placing a filling. – If you can see the cavity in your tooth, getting to your dentist’s office for evaluation long before it starts to cause any pain will increase the odds that your dentist can offer this option.
- Extracting your tooth. – Even if your tooth doesn’t display any symptoms (discomfort, pain, swelling), extracting it may still make the most reasonable or prudent option.
Pulling or filling a decayed wisdom tooth – Which makes the better choice?
As you’d expect, this decision can only be made on a case-by-case basis because, of course, everyone’s and every tooth’s situation is different.
There is, however, a core set of deciding issues and factors that dentists tend to use when making a decision about which to recommend. That’s what we discuss next.
Factors and issues. / Pros and Cons
A) When should a wisdom tooth that has a cavity be considered for extraction?
Circumstances that favor removing decayed third molars include:
X-ray showing the socket of an extracted wisdom tooth.
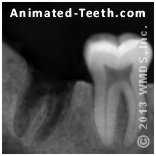
- The size of the lesion is extensive and the prognosis for the tooth is poor. – Seeing or feeling a hole in your tooth can be a sign of advanced decay. So can tooth sensitivity to hot or cold foods and beverages, or episodes of spontaneous pain.
- The dentist’s access to the tooth and/or cavity is limited. – Just like limited access can inhibit your ability to clean your tooth, it can also limit your dentist’s ability to make a successful repair.
- The position of the tooth makes it difficult to brush and floss. – Teeth that can’t be kept plaque-free remain vulnerable to continued problems with cavities (recurrent decay).
- The tooth has experienced multiple episodes of decay before. – Teeth that have been filled before remain at risk for recurrent decay if they can’t be kept plaque-free.
- The patient doesn’t possess the dexterity to adequately clean the tooth.
- The tooth holds little dental importance – Like in regard to function (i.e. chewing) or future dental work.
- The patient prefers extraction.
Print out this list for discussion with your dentist.
The remainder of this page explains considerations associated with each of the above factors. Additionally, our comments section gives some examples of how these factors are weighed in real life.
B) When should a wisdom tooth’s cavity be filled instead of extracting the tooth?
Situations that favor placing a wisdom tooth filling are …
An X-ray that shows a wisdom tooth filling.
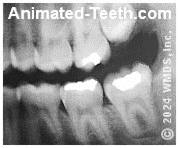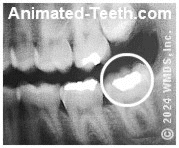
- Your dentist has adequate access to the tooth. – In many cases, wisdom tooth filling placement is a simple, straightforward affair.
- Your dentist feels that the health and outlook for your tooth following its repair seems reasonable. – Discovering wisdom tooth cavities at an early stage helps to guarantee this outcome.
- The tooth has significant dental importance – This may be in regard to function (like chewing) or the tooth might hold strategic importance for future dental work.
- The patient feels they can do a better job of keeping the tooth plaque-free. – Once aware of their historical deficiencies, a patient may be motivated to improve their oral hygiene efforts so to prevent future problems.
- The patient prefers filling placement.
Print out this list for discussion with your dentist.
The remainder of this page explains considerations associated with each of the above factors. Additionally, our comments section gives some examples of how these factors are weighed in real life.
This page’s highlights as a video –
Subscribe to our YouTube channel.
Should I get my decayed wisdom tooth filled or extracted? – How to decide.
As an introduction to this subject, here’s a list of questions people frequently have. Our answers are brief. We explain these issues in more detail in the text that follows this Q&A section.
FAQs: Quick Answers to 11 Questions About Cavities in Wisdom Teeth
Here’s a list of questions that people frequently ask. Our answers here are brief, but we explain all of these issues in more detail in the text that follows this FAQ section.
Is it common for wisdom teeth to decay?
Yes, any dentist would be quick to say that there’s nothing rare about cavities forming in a person’s third molars. Just like with any other tooth in your mouth, if dental plaque is allowed to accumulate on its surface, the tooth will be at elevated risk for decay formation. Your wisdom teeth are no exception to this rule.
Is a wisdom tooth more prone to getting a cavity?
Only in the sense that the placement of the tooth (its positioning/alignment) may make it hard, if not impossible, to properly clean. And if you can’t adequately remove dental plaque from a tooth, then it will be at increased risk for the formation of decay.
But, other than that, there is nothing about third molars that makes them any more susceptible than any of your other teeth.
What should you do if your wisdom tooth has a cavity?
Generally, tooth decay will advance over time, so if you have a wisdom tooth that has a cavity, you will need to have your dentist treat it before it has advanced to a point where it causes symptoms and/or significant problems with your tooth.
Seeking treatment sooner rather than later usually affords you and your dentist more treatment options. And if the solution chosen involves placing a filling, the cost of the repair will likely be less for a smaller (earlier) repair.
How are cavities in wisdom teeth dealt with?
Your dentist will generally have two options to offer, either placing a filling or extracting the tooth.
In deciding which makes the better plan, they’ll need to evaluate how important your tooth’s place is in your dentition (set of teeth). And if they feel it can be salvaged and it plays a valuable role, then they will recommend restoring it.
If instead, the tooth is too severely damaged, has little dental importance, or is expected to have a poor outlook (for example, experience decay again later on), they will recommend removing it.
Can a cavity in a wisdom tooth be filled?
Yes, absolutely. A third molar, just like any tooth, can have a filling placed. That assumes of course that the cavity hasn’t advanced so far that it has seriously compromised its nerve. (Signs and symptoms might include episodes of pain and/or swelling associated with the tooth.) And that the dentist has the access they need to perform their work.
Even if the tooth has been seriously compromised, it still may be possible for it to be restored. However, more extensive dental work than just placing a filling will probably be needed. And sometimes it’s hard to justify this additional cost and effort for a wisdom tooth.
Are wisdom teeth fillings harder to place?
Only in the sense that due to their positioning wisdom teeth can be more difficult for your dentist to access than other teeth. (After all, if you’ve had trouble brushing and flossing your tooth, your dentist may have difficulties with access too.)
This factor makes a great reason why you should seek treatment for your cavity while it is still just a small one.
Shouldn’t any decayed wisdom tooth just be pulled?
Yes, if the tooth’s lesion has advanced so far that salvaging the tooth is not possible. Or if some factor associated with the tooth makes the idea of restoring it questionable or ill-advised, then extraction is the only other choice.
Extraction might also be chosen if the tooth holds little dental importance or is seen as a likely source of persistent problems. (Recurrent (repeat) decay, gum disease, or the tooth increases the adjacent 2nd molar’s risk for these same issues.)
Won’t a decaying wisdom tooth just fall out?
No, that’s not a realistic expectation. As the tooth’s decay advances, you can expect it to compromise the structural integrity of your tooth, and portions of it will break off from time to time.
And, unfortunately, as the size of the lesion advances yet further, you can expect the tooth and/or its surrounding tissues to become infected. (Infection is frequently accompanied by periods of significant pain and swelling.) Almost certainly, there will finally be a point in time when your tooth will require extraction and you’ll be eager for it.
Are decayed wisdom teeth harder to pull?
No, not necessarily but possibly. If the amount of decay has compromised the tooth’s structural integrity, or the tooth’s deterioration leaves little for the dentist’s instruments to grasp or lever against, then they may have more difficulty.
But remember, most teeth that are extracted are compromised in some way. So dentists and especially oral surgeons are used to overcoming these kinds of challenges.
Is it possible that my wisdom tooth has caused a cavity in the tooth right next to it?
Yes, absolutely. And this complication (or the potential for it to happen) is a common reason why some wisdom teeth are recommended for extraction.
When it occurs, the problem lies in the fact that a factor associated with the third molar keeps the person from adequately cleaning their 2nd molar. This might be related to plaque and debris accumulation in the cavity of the decayed wisdom tooth. Or the position of the tooth (rotated, angled, tilted) of the third molar creates a “food trap” between the two teeth.
If I have my decayed wisdom tooth extracted, will my other teeth shift?
No, this generally isn’t a scenario that you have to be concerned about. But your dentist will evaluate your specific situation for the potential for this complication before making their recommendation for extraction.
1) What you should know about cavity formation on wisdom teeth.
Cavities form on tooth surfaces where dental plaque is allowed to build up and remain for extended periods. This is true for any tooth, your wisdom teeth are no exception.
What are the special concerns about the potential for decay in wisdom teeth?
If the positioning of a third molar is such that it’s difficult or possibly even impossible to clean, it will be at increased risk for cavity formation.
This gum tissue flap interferes with cleaning this wisdom tooth.
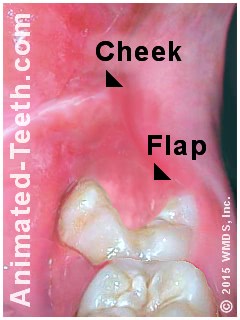
- Due to the fact that wisdom teeth occupy a position in the very back of the mouth, many 3rd molars can be very difficult to brush and floss. If maintaining adequate oral hygiene is not possible, the persistent accumulation of food debris and dental plaque that builds up frequently results in the formation of tooth decay (see statistics section below).
- Compounding this difficulty, some third molars will fully erupt but have a positioning that is angled or misaligned. (The tooth has come through the gums but its alignment is crooked.) As a result, these teeth may be extra difficult to clean or prone to trapping food.
- Impacted wisdom teeth – Some 3rd molars never fully erupt. (They remain in a position where they only poke partway through the gumline or are covered over by a flap of gum tissue (see picture above).) As a result, it may be impossible to properly clean them.
Special difficulties with impacted wisdom teeth.
As a type of worst-case scenario, some impacted wisdom teeth may be entirely impossible to clean.
This scenario involves a situation where the developmental space that exists around the crown of a partially impacted tooth (a tooth that to some degree has penetrated through the gums) has been colonized by bacteria.
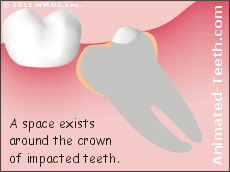
Plaque can accumulate in the space underneath the gum line.
Since this space is both minute and entirely underneath the gum line, it can’t be accessed. And as such, the dental plaque that the bacteria form will remain undisturbed and therefore has the potential to cause a cavity in the tooth.
▲ Section references – Koerner
2) Things to know when choosing between wisdom tooth filling placement and tooth extraction.
Just as you would expect, the possibility or practicality of repairing a decayed wisdom tooth simply depends on the circumstances and conditions that exist. Here are some examples.
a) Some cavities in third molars can be repaired easily enough by placing a dental filling.
- The overall size of the lesion is still relatively small. – While not a definitive test, a cavity (dark spot) that you see that causes no pain may be an indication of this.
- The lesion is located on an aspect of the tooth that’s readily accessible. – Of course, your dentist needs to be able to access the decay with their instruments to remove it.
Why would you want to opt for filling placement?
Wisdom teeth are just that, a type of tooth. There’s nothing different or lacking about them. And there’s no reason why a properly positioned one can’t function as a valuable member of a person’s dentition (set of teeth). Since you’re only born with 32, why lose any tooth that could be saved?
Why wouldn’t you want to consider placing a wisdom tooth filling?
If the repaired tooth can’t be kept plaque-free, or you’re not willing to regularly put in the effort to keep it that way, filling placement may not provide a lasting solution. (Discussed below.)
b) Sometimes wisdom tooth extraction simply offers a better solution.
In some situations, a dentist may feel that removing the wisdom tooth makes a better choice than restoring it. Here are some reasons why.
1) Repair may not be possible.
In some instances, the lesion that has formed may be situated in such an awkward location on the tooth that the dentist finds their access to it extremely limited, if not impossible.
It’s easy enough to imagine that if the area has been difficult to clean with a toothbrush and floss it would be equally inaccessible when the dentist’s instruments are used. If so, the tooth should be extracted.
2) The long-term outlook for the tooth may be poor.
Even in cases where a filling might be successfully placed, if the wisdom tooth still cannot be adequately maintained and its surface kept plaque-free, it will run the risk of developing recurrent decay.
(The term “recurrent decay” means that a new cavity has formed on an aspect of a tooth adjacent to an existing filling.)
If this scenario exists, dealing with the tooth just once (pulling it now) may make the more prudent choice.
- Teeth that experience further decay may (possibly) be more difficult to extract.
- Those that develop extensive lesions may become symptomatic (cause episodes of pain and swelling).
- Extraction offers the financial economy of knowing that you’ll only have to pay for a procedure for the tooth once.
3) Making a repair simply may not make good sense.
Just because dental work can be performed, doing so may not make a lot of sense when the amount of effort and finances required for it are considered.
An example.
While admittedly different than just placing a filling, some wisdom teeth that have advanced lesions may require extensive dental work to restore them (root canal treatment and dental crown placement).
The number of appointments and amount of finances needed to complete this level of treatment can be extensive. And success rates for root canal treatment performed for wisdom teeth can be questionable.
With these considerations in mind, and for cases where the wisdom tooth has little strategic importance (with chewing or as a support for other dental work), wisdom tooth removal likely makes the more practical choice.
3) A wisdom tooth may put adjacent teeth at risk for cavities.
When third molars don’t fully erupt into normal alignment, their positioning may result in the formation of what’s referred to as a “food trap.” (A trap for dental plaque and food debris between the wisdom tooth and the next tooth forward, the 2nd molar, as shown in our animation.)
If the space between a wisdom tooth and its neighbor can’t be kept clean, a cavity may form.
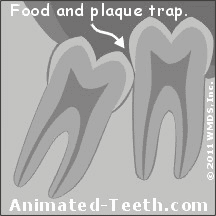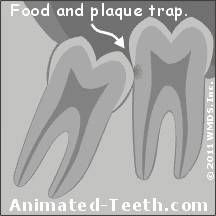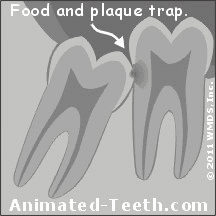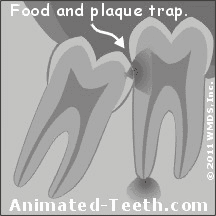
Advanced lesions can cause nerve tissue death, with extraction or root canal then being required.
If the accumulation of matter that builds up in this space (dental plaque, trapped food debris) can’t be cleaned out thoroughly, which is frequently the case, not only will the wisdom tooth be placed at much greater risk for developing a cavity but so will the 2nd molar.
A lose-lose outcome.
The worst-case scenario for this type of situation is one where decay has formed on both teeth to such a great extent, or in such an inaccessible location, that neither can be repaired and as a result, both must be extracted.
Another dire outcome would be one where it may still be possible to salvage the 2nd molar but only after performing root canal therapy and placing a dental crown.
Generally speaking, it’s one thing for a person to lose a wisdom tooth (a kind of tooth that a large percentage of people function just fine without). But when a second molar (typically considered a much more valuable tooth) is needlessly lost or severely damaged, it’s a tragedy.
4) How often do problems with tooth decay occur?
What does research show?
Here are the findings of some studies that have evaluated wisdom teeth and their incidence of cavity-related problems.
Study #1:
Title: Occlusal caries experience in patients with asymptomatic third molars.
- This study evaluated the decay rate of asymptomatic, erupted wisdom teeth. (In this case, Erupted = Teeth that have been able to come into place normally, or at least fairly close to it.) All participants had one or more wisdom teeth.
The study determined that for subjects 25 years and older, 39% of them had at least 1 wisdom tooth that had a history of decay (either active or repaired).
Lower wisdom teeth were more likely to be affected than upper ones (24% vs. 18%).
Study #2:
- This large study evaluated over 3800 impacted wisdom teeth. The findings of this report were that 2 to 3% of the lower ones, and roughly 7.3% of their adjacent second molars, had cavities.
– Since fully impacted wisdom teeth (which have limited potential to decay) were included in this study, one would have to assume that the decay rate for partially erupted lower impacted wisdom teeth would be greater than the numbers stated above.
Study #3:
Title: Diseases and lesions associated with third molars. Review of 1001 cases.

The space between this wisdom tooth and neighbor can’t be cleaned.
- Linden evaluated a group of patients ages 13 to 75 years who collectively had over 2800 wisdom teeth removed. In regard to these extracted teeth, 7% had cavities, as did 42% of their adjacent 2nd molars. (Our picture shows an extensively decayed 2nd molar.)
– The numbers above quite possibly were skewed by the fact that the study group was composed of patients whose wisdom teeth were removed for a reason, including the diagnosis that decay was present. In normal populations, the rate might be expected to be lower.
Study #4:
Title: Third molar caries experience in middle-aged and older Americans: a prevalence study.
- Fischer determined that, for a population of 52 to 74-year-olds, the incidence of tooth decay on third molars strongly correlated with the decay rate the person experienced with their other teeth.
– This suggests that, in regard to making a determination about how significant the risk of third molar tooth decay complications might be for you, you should first consider what your cavity rate has been in general.
What can you do to prevent wisdom tooth cavities?
Circumstances associated with the formation of cavities in wisdom teeth are no different than with any other type of tooth. If the tooth’s surface can’t be kept plaque-free, the potential for decay formation always exists.
For further details about the decay process, here are links to our pages that explain How and why cavities form and how dentists detect cavities on X-rays Pictures | Diagrams.
Here are some suggestions about things you can do:
Wisdom tooth cavity prevention- Steps to take.
- Make sure to thoroughly brush and floss your wisdom teeth. Realize that doing so may take extra effort. Brushing tips. Flossing tips.
- Using an electric toothbrush may help to make your brushing sessions more effective. Powered toothbrushes: Best Sonicares Best Oral-b’s
- Visit your dentist for regular checkups. The goal is to detect and repair developing tooth decay as early as possible.
- Use Fluoride Toothpaste, it really does help to prevent cavities. If decay formation has been a problem for you, your dentist may recommend using a prescription fluoride product.
- If your dentist makes a valid case for extracting your wisdom tooth (like those discussed above on this page), take their advice. Lose it.
Last reviewed: February 16, 2025
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Chu F, et al. Prevalence of impacted teeth and associated pathologies–a radiographic study of the Hong Kong Chinese population.
Fisher E, et al. Third molar caries experience in middle-aged and older Americans: a prevalence study.
Koerner KR. Manual of Minor Oral Surgery for the General Dentist. Chapter: Surgical Management of Impacted Third Molar Teeth.
Linden W, et al. Diseases and lesions associated with third molars. Review of 1001 cases.
Shugars DA, et al. Occlusal caries experience in patients with asymptomatic third molars.
Video transcription.
Welcome to Animated Teeth.com and our page that discusses factors that need to be considered when making a decision about what to do with a wisdom tooth that has developed tooth decay.
As you’re probably aware, it’s relatively commonplace for a person to have their wisdom teeth extracted. So, when you have a third molar that has a cavity, doesn’t it make sense to just go ahead and have it pulled?
Well, that may make the best plan for many cases but it’s not the best one for all. And as an explanation, the remainder of this video will outline factors your dentist will need to evaluate before coming to a conclusion about how to advise you.
To start, we’ll mention that just because a tooth is a wisdom tooth doesn’t mean that it’s not a valuable member of your dentition and should be saved if possible.
Yes, the diminutive size or oddball shape of some third molars may render them functionally useless. As can poor positioning, like the case where the tooth only pokes part way through your gums.
But those circumstances certainly don’t exist with all wisdom teeth and many might be missed immediately if extracted, or might have played an important role in rebuilding your mouth in the future if adjacent teeth are damaged or lost.
So, your dentist must weigh the importance of your tooth both in terms of the role it plays now and how it might be useful in the future. And, generally, and especially in the case where the needed repair is just a simple filling, a dentist will typically be inclined to encourage you to keep any tooth possible.
In deciding to save your tooth, an important factor that must be examined is why it developed decay in the first place. Was it simply due to lax oral home care? Wisdom teeth are positioned in the very rear of your mouth where they’re hard to see and access. And when it comes to brushing and flossing, they often receive second-rate care. Of course, you can always improve.
In contrast, it may be that the tooth’s circumstances cause special challenges. For example, maybe the tooth-gum relationship forms a space that’s hard or even impossible to clean. Or maybe the tooth’s alignment is reasonable but still irregular enough that food and debris tend to trap.
Situations like these may result in aspects of the tooth that are predisposed to persistent dental plaque accumulation. And if so, recurrent decay, meaning the formation of a new bout of decay after a previous cavity has been repaired, may seem a likely scenario to your dentist and therefore tip the scales in favor of them recommending tooth extraction.
Exactly what process will be needed to fix your tooth will also need to be weighed. For example, is it even possible for your dentist to make a successful repair? After all, teeth that are hard for a person to reach when cleaning can be a challenge for their dentist to access too.
If the needed dental work is extensive and expensive, does the current or potential value of the tooth warrant this level of care? Additionally, wisdom teeth sometimes have aberrant anatomy. And that can make the outcome of some procedures, like root canal treatment if needed, less predictable. So, clearly, your dentist will have a lot of treatment issues to consider before advising you one way or the other.
In passing, we’ll mention that for small cavities the cost of placing a filling vs. extracting the tooth will probably be fairly similar. That’s because the cost of pulling an erupted wisdom tooth, meaning one that has come through the gums into fairly normal positioning, shouldn’t be any more than any other tooth. For more details, look for our website’s pages that discuss fees for both fillings and extractions.
Beyond all that we’ve discussed, there is, of course, the issue of what you personally prefer to have done. If a decayed wisdom tooth has debatable importance and a questionable long-term outlook, you may want to be done with it once and for all. However, if you lean toward this option despite your dentist’s encouragement to the contrary, it’d be smart to let them run through their arguments again because once your tooth is gone it’s gone forever.
With that advice, we’ll wrap things up. Don’t overlook reading this video’s associated webpage for more details and more thorough arguments on both sides of this issue. And good luck in making your decision and having your procedure. Goodbye.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
Cavity in wisdom teeth. Pull them?
My dentist says fillings on wisdom teeth don’t work and that I need two pulled. What do you think? Is that true?
Mellie
Reply –
It’s not really for us to second guess what your dentist thinks makes the best treatment plan for you. After all, they have actually examined your teeth and we have not.
Without question the blanket statement “fillings on wisdom teeth don’t work” isn’t accurate. But we think you’ve misinterpreted what’s been said.
Wisdom teeth aren’t any different than any other kind of tooth. So yes, absolutely, fillings can be placed in them.
What may make fixing a cavity/placing a filling in one a poor choice often has to do with the wisdom tooth’s positioning in the mouth.
If the dentist doesn’t have adequate access to the part of the tooth that has developed the cavity, fixing it can be difficult to do correctly, and sometimes not possible at all.
Another consideration associated with the tooth’s positioning is how well you brush and floss it. If you can’t keep it plaque free, then the dentist may feel that the risk of a new cavity forming on the tooth (after a first filling has been placed) is high. If so, possibly the less troublesome solution is simply to extract the tooth.
In your case, you state that two of your four wisdom teeth have cavities. That implies that you do have difficulty in keeping them clean. So as with the second scenario, possibly the simpler, less costly, less troublesome, etc… solution is to simply have yours taken out.
Read through this page above, we explain these points in greater detail.
Staff Dentist
Comment –
Wisdom teeth filling
Wisdom teeth have more roots than regular molars, so harder to numb, plus my wisdom was broken, Dr built it up and filled it 4 mos ago, but it’s really sensitive, eat even really use it much & I’ve developed infection twice and had to take a course of antibiotics both times. Going back to have it pulled now, cause it’s constantly a nuisance and I’m tired of taking pain medications almost every day. I suggest just having them pulled from the get go.
Marcy
Reply –
We’ll agree that due to their location that wisdom teeth can be difficult to clean, leaving them vulnerable, as in your case, to decay and infection. And we agree that in terms of function (like eating), most people do just fine without having their 3rd molars.
We’ll take issue on the points that wisdom teeth have more roots than regular molars (they may but don’t usually). And the actual number of roots shouldn’t usually have any bearing on the difficulty with which it can be numbed up.
Best of luck with your extraction. It sounds like a good plan for you.
Staff Dentist
Comment –
Fillings in wisdom teeth.
Hi I am 25 and the lucky owner of four almost perfectly erupted wisdom teeth. But also the owner of fillings in all four wisdom teeth. Short after the eruption I had cavities, which my dentist chose to drill and fill – I was not questioned. But he said that it was difficult to dry the teeth and therefore he needed to prepare silver fillings and not composites like (the too many fillings) I have in my other teeth. The silver fillings are about 2/3 of the upper chewing surface but are so far back in my mouth that they are not visible – unless if I open wide, so that is OK with me. Dentist says that the fillings should be very long lasting if I brush thoroughly
Flemming
Reply –
Just like your dentist’s treatment suggests, well-positioned wisdom teeth can be valuable teeth to have and there is no reason to extract them.
What we really like is that for the repair they saw the advantage of placing amalgam fillings (not as technique sensitive to place). And yes, your silver fillings should last as long or longer than your composite ones. Not every dentist still places amalgam (the primary filling material for back teeth in decades past, that has now fallen out of fashion primarily because it is not white in color).
Your words about your general decay rate (historic/current) is a concern. Keep in mind that filled teeth can get cavities if you don’t clean them properly. This would especially be a continued concern with hard to reach wisdom teeth.
You should read our pages that cover tooth decay, just so you have a better idea of why it forms and how to prevent it. It will save you a lot of grief over your lifetime.
Staff Dentist
Reply –
Thanks for your comments on fillings in my wisdom teeth.
Hi, thanks a lot for your comments. Nice to hear that my dentist took a good decision when he filled my wisdom teeth with amalgam fillings.
Yes, I wrote that I have (too many) fillings which might indicate a concerning decay rate. The story behind is, that during my teenage years I was eating lots of sugar, sweets and candies and drinking soda, while I was not brushing my teeth frequently and thoroughly. So, within two or three years I got 12 cavities drilled and filled with composites, so happy it is not visible I had all these cavities!! That was about 10 years ago, and since then, I have only had the mentioned cavities in my four wisdom teeth, bringing me at totally 16 fillings (which I think is far too many for a 25-year-old).
Thanks for the links to tooth decay pages – I certainly learned that my fillings are not lasting forever and need to be redone at some point in time, probably due to “recurrent” decay, which you also mention in your comments. That was an eye-opener to me and placed some major concerns in my head, especially because I have so many fillings – obviously I can’t ignore the recurrent decay risk. I still have a “sweet tooth” to satisfy, but nowadays I am taking very good care of my teeth. Therefore, I hope my high decay rate is historic and under control and that my recurrent decay risk is limited. I trust my dentist is checking all my fillings at my regular dental checkups, so that any recurrent decay is detected and fixed early so that my fillings (amalgams and composites) will be lasting for many years ahead.
Flemming
Comment –
Help.
what would cause a wisdom tooth to decay right INSIDE the gum?
KG
Reply –
There are two issues to know about:
1) Tooth decay can form on any tooth surface where dental plaque is allowed to build up and persist.
2) The gum line (the place on a tooth where the gums tissue attaches) is the same on all teeth. So even though a wisdom tooth may look like it is buried in gum tissue, where its gum tissue actually attaches to it is further below the gum’s surface. This means there can be a lot of empty space that exists between a tooth and its surrounding gum tissue.
(The illustration above on this page shows an extreme of that situation. The space that surrounds the buried wisdom tooth is shown in a tan color.)
If that space fills in with dental plaque, and since you can’t effectively brush a tooth buried in gum tissue, a cavity may form.
Staff Dentist
Comment –
Bottom right side wisdom tooth.
My bottom right wisdom tooth is fully through my gum and has a cavity. I’m having pain especially when it touches the top tooth. I’m having it removed but am worried. Will it be easily extracted since it’s fully out of the gum? Or will the cavity cause a problem?
AS
Reply –
Extracting a wisdom tooth that is fully erupted can be as routine as extracting any other molar.
The concern with advanced decay is that it might have compromised the structural integrity of the tooth. A common scenario would be one where the crown portion (the part of the tooth above the gum line) fractures or comes off during the extraction process.
1) The X-ray of your tooth that your dentist took would give them an idea of the extent of the decay. If it was especially extensive, it seems that they might have made some comment.
2) Just because a tooth breaks during its extraction process doesn’t mean that it will then be difficult to remove. Having a tooth break is common, fairly routine and doesn’t necessarily add to the degree of difficulty of the procedure. It may, but it absolutely doesn’t always. With a two-rooted molar with divergent roots, the crown coming off could conceivably make the extraction easier (because that event would facilitate removing each root independently).
Staff Dentist
Comment –
Non-impacted wisdom tooth removal.
Tooth #32 is not impacted and looks like a normal molar in X-ray in terms of positioning but it has a very large internal cavity. It didn’t bother my until I stopped using Sensodyne toothpaste. Then pain alternated between wisdom tooth and second from last molar in upper jaw where I had a crown put on about 5 months ago. Pain decreased and stopped once I started using Sensodyne and Listerine mouth wash about 2 weeks ago. Dentist said I should have it removed but he doesn’t do that. Do I need to have it removed if it is not impacted and not causing pain but has large internal cavity?
HSM
Reply –
If the wisdom tooth has a cavity in it (especially a very advanced one) and that situation cannot be corrected (by placing some type of restoration, possibly root canal treatment would be needed too), then the only alternative is to have the tooth extracted.
As the cavity increases in size over time, you place yourself at increasing risk for experiencing an acute episode (infection, pain, swelling). And the advancing cavity will only further weaken the tooth, and therefore possibly making it’s removal more difficult.
It’s not possible for the products you mention to provide a solution for active decay.
That’s not to say there is no question that your discomfort isn’t caused by the upper tooth. That’s for your dentist to determine. But no good will come from your leaving #32 unattended.
Staff Dentist
Comment –
Wisdom tooth deteriorating.
I’m 43, I have one wisdom tooth left & it was halfway under the gum & halfway out, kind of slanted. I’ve had no problems with that tooth until the last couple of years. The tooth has been coming out in pieces so there was just a shell. It has come down to the remainder of the tooth which is barely a rigid area above the gum & nothing but a hole in the middle that catches all kinds of food.
Steph
Reply –
What you seem to describe is an impacted, partially erupted wisdom tooth (“halfway under the gum & halfway out, kind of slanted”) … That also has a large carious lesion (cavity) … (“The tooth has been coming out in pieces so there was just a shell”).
For teeth that are extensively decayed, and 1/2 submerged under the gum line, the possibility of restoring the tooth (decay removed, filling placed) seems doubtful. Pending your dentist’s decision, it would seem your only solution lies with having the tooth extracted.
Staff Dentist
Comment –
Rotten wisdom tooth.
My wisdom tooth is fully grown above gums but rotten and hollow and half broken off. It recently tonight started hurting severely and draining a white chunky stubstance. I used a whole tube of maximum strength orajel trying to aleiviate the pain. And now the tooth hole is filled with the white substance. I plan on going to the dentist as soon as possible. What do you think?
Cassidy
Reply –
At this stage, it seems quite possible that you have an active infection associated with your tooth. Quite possibly rather than originating in the tissues that surround your tooth (pericoronitis), the infection’s origin is instead inside the tooth’s nerve space (related to the very advanced decay that you describe).
Pus coming from an infection is white in color, however we are less familiar with it being described as “chunky.”
The product you mention contains benzocaine, a topical anesthetic. Topicals are typically only effective in numbing up the surface of the gums. If you have an infection (whatever the location), that’s probably not going to provide a lot of relief.
Your solution lies with your dentist. One would guess that an extraction is in your future. Your dentist may need to place you on antibiotics before that can be done. You should describe your situation to them when you contact them. If they feel antibiotics are indicated, possibly they can phone your pharmacy so you can get started with them as soon as possible.
Staff Dentist
Comment –
Tooth filling for wisdom teeth.
Im 39 years and went to see a dentist due to having severe pain on both lower sides of my wisdom teeth. She checked and found cavity and that both 2 wisdom teeth were rotten. It was my first Dentist visit since I was born I think, however she numbed the right hand side lower gums, drilled the rot out and put white fillings. Sshe never prescribed anything or booked me off, so I assumed that I would be good to go back to work after my one hour lunch. But since then I’m experiencing a throbing or poking feeling and teeth sensitivity on the side that the procedure was performed. So I went back to ask if there is some meds she can give me, she re-checked me and couldn’t find anything wrong. She was so upset and scolded me saying she doesn’t believe that I’m in pain but I honesty am feeling pain both when my mouth is closed or open. What could be wrong
Mrs. Mangoza
Reply –
As guesses, and situations your dentist could explain further for you …
1) Related to the presence of decay and/or the placement of a filling, a tooth’s nerve tissue sometimes displays signs of having been traumatized. The throbbing you mention might be a sign of that.
The tooth’s condition (inflammation of the nerve tissue) is generally classified as “reversible” or “irreversible.”
With the former case, the tooth will settle down. To help, a dentist will sometimes recommend the use of an OTC anti-inflammatory pain reliever, which aids with controlling pain and settling the irritated nerve tissue down more quickly.
“Irreversible” cases are those where the nerve doesn’t recover because it has been traumatized too much. (The “severe” pain you had initially might be a sign of that condition.) Irreversible cases lead to the need for root canal therapy or tooth extraction.
While a dentist can’t know which way a case will resolve, they will have an opinion based on what they observed when working with the tooth (like how extensive the decay was, what your symptoms were and currently are).
If this is what’s going, it would seem your dentist expects that your situation is the “reversible” kind and the tooth should settle down. You might quiz them about the use of an anti-inflammatory analgesic to aid this process. And of course, if the tooth doesn’t improve, you need to let them know too.
2) The placement of “white” (dental composite) fillings is sometimes associated with post-operative tooth sensitivity. We don’t really have a page that explains that situation, but just Googling those terms should provide you with sources of information so you can judge if instead that seems to be what’s going on with your tooth.
Good luck.
Staff Dentist
Comment –
Hole in wisdom tooth.
In the last month, I happened to pick broken chips of my lower left wisdom tooth out of my moth on two different occasions. The tooth is fully erupted with a thin flap of skin, though it had always had cracks and fissures since it’s eruption (which was protracted and painful). Since the past month I get constant pain, (even on drinking room temperature water) and lodgement of food particles. Do you advise a filling or an extraction?
Sandra
Reply –
Only an evaluation by your dentist can determine what makes the right choice for your tooth. Beyond quizzing you and direct examination, they will also probably need to take an X-ray to fully diagnose your case.
Short of having almost any of that information, it seems you are describing a tooth that has very advanced tooth decay:
1) It’s at a point where its structurally unsound enough that portions have started to fragment off (here’s our page about broken teeth). So much of the tooth is now missing that it accumulates/retains debris.
Generally, that doesn’t sound like a tooth that’s in need of just a “routine” filling (a procedure where there’s minimal concern about the outcome for the tooth’s nerve or the longevity of the restoration). (Here’s a discussion about rebuilding seriously compromised teeth with a filling vs. crown.)
2) The fact that the tooth has pain suggests that the decay has advanced close enough to the tooth’s nerve tissue to irritate it. If the nerve tissue is at a point where it has been significantly traumatized, the tooth would require root canal treatment before rebuilding it would be possible.
You state “constant” pain but it’s hard to interpret what you mean. The worst case would be the situation where the pain often/typically occurs on its own. If instead it only occurs in response to a stimulus (like the water you mention), then that possibly poses a more favorable outlook for how affected the nerve tissue is. Once again, only your dentist can determine this (here’s more information about endodontic pain characteristics).
4) You also mention an associated flap of skin that covers the tooth, which very likely could be the reason why you can’t clean it properly and the decay has started. If so, that would need to be trimmed away (if that can provide a long-term solution), otherwise you would be at risk of the same set of events occurring again.
In the case where a wisdom tooth is seriously compromised, its needed repair will be extensive, and after repair it will still remain at risk for a recurrence of problems, then yes, and especially on the recommendation of your dentist, the more practical solution may be to extract the tooth.
Staff Dentist
