Tooth Bonding Science
How does the science of dental bonding work?
One of the hallmark characteristics of tooth bonding is the great strength with which it adheres to tooth enamel. And while you might expect that the formation of this bond is somewhat complicated, its principles are actually quite simple and easy to understand.
Here’s how tooth bonding works. It’s based on what’s referred to as acid-etch technique. A protocol that dentistry began to implement on a widespread basis in the early 1960s.
A) The tooth’s enamel is first treated with an acidic conditioner (tooth etchant).
Background
Enamel is the most highly mineralized body tissue (98% mineral content vs. 70% for bone). And this fact makes the process of dental bonding possible.
The etching process. – What does it do?
When an acidic solution is placed on a tooth’s enamel surface (animation frame #2), it will dissolve away (etch) some of its mineral content.
After this etching treatment, the enamel’s smooth surface will have been transformed into one that at a microscopic level is irregular, jagged and rough (animation frame #3).

Acidic etching gel is used to roughen up the enamel’s surface.
What kind of acid is used to etch teeth?
The most common etchant used in dentistry is phosphoric acid. 35% phosphoric acid is the most common formulation but products may range from 30% to 50%.
Etchant products usually take the form of a gel that when squirted onto the tooth’s surface tends not to run. In the early decades of bonding technique, liquid etchant was common but has since faded in popularity.
How long is the etchant left on the tooth?
The etchant is usually applied and then left on a tooth’s surface for about 20 seconds. Afterward, it is rinsed off using a water spray. This page outlines the steps of the etching process.
What does etched tooth enamel look like? – A familiar comparison.
In terms of something you are likely familiar with, etched enamel is very similar to frosted (etched) glass.
With etched glass, as you run your hand over its surface you can feel that it has a texture. That’s because, at a microscopic level, it is quite rough, just like very fine sandpaper.
You’re probably also familiar with the fact that etched glass has a dull, frosted appearance. In a similar fashion, if you dry etched enamel it shows this same distinctive frosted look too.
B) How dental bonding’s attachment to a tooth’s surface is formed.
In creating the bond between the restorative placed and a tooth’s surface, dental bonding science exploits the microscopic roughness of etched tooth enamel. Here’s how:

1) The bonding agent locks on to the enamel.
2) The dental composite, in turn, is bonded to the bonding-agent layer.
- The dentist coats the tooth’s etched surface with a liquid plastic referred to as “bonding agent” (animation frame #2 below).
- Since it’s a liquid, it’s able to seep in between the nooks and crannies of the tooth’s etched surface.
- Then, once it’s cured (hardened), because it encases the rough microscopic projections of the etched enamel, it becomes locked (bonded) onto the tooth’s surface.
The bond is a simple mechanical one.
It’s due to an interlocking of the cured bonding agent within the nooks and crannies of the etched enamel surface.
FYI –Although a simple process, acid-etch technique (etching a tooth’s enamel surface and creating a bond with it) is responsible for revolutionizing dentistry.
It’s the basis of all modern adhesive dental procedures (bonding, porcelain veneers, dental sealants, placing orthodontic brackets) and fundamentally remains little changed since its first introduction in 1955.
C) How the rest of a bonded restoration is created.
At this point, the tooth’s surface has only been covered with a very thin layer of plastic (the bonding agent) (animation frame #2).
So to give the dental restoration its needed bulk and shape, successive layers of a dental material called dental composite (see below) are added to the initial sublayer until the restoration takes its needed form (animation frame #3).
As each layer is placed, it creates a chemical bond with the bonding agent sublayer and/or a previously placed layer of composite.
Notice that we said a chemical bond is created, as opposed to a mechanical one like that which exists between the bonding agent and the etched enamel surface.
FYI –As a point of interest, the strength of the bond between a restoration and its associated etched enamel surface can exceed that of the chemical bond that holds the bulk of the restoration together.
This is evidenced by the fact that broken white fillings don’t necessarily fall out in one piece. It is just as likely, if not more so, that some remnant of the restoration will remain firmly bonded to the tooth.
Bonding to tooth dentin.
Creating a bond with tooth dentin, while similar, is a more complicated affair and one whose understanding is still evolving.
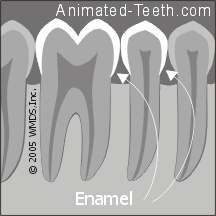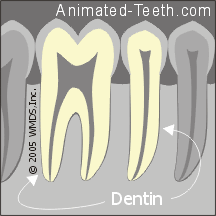
A bond can be created with both tooth enamel and dentin.
What is dentin?
- Teeth are not solid enamel. Instead, it just composes an outer covering over the part of a tooth we can see.
- If a tooth has broken, decayed, been trimmed or if its gum line has receded, aspects of its dentin component become exposed.
The science of bonding to dentin is fairly involved and beyond the scope of our discussion here (we discuss it a little bit more lower on down this page). But the fact that it is possible helps to improve restoration integrity and adhesion.
It’s all a one-step process.
As a point of interest, the steps your dentist takes when creating a bond with dentin may be essentially the same as those used with enamel. And in fact, but depending on precisely what product and protocol are used, it’s possible for them to accomplished both processes simultaneously using the same agents and materials.
What is dental composite made of?
At its core, dental composite (tooth bonding) is just a plastic compound, with this basic core referred to as the restorative’s resin matrix or unfilled resin (see “fillers” below).
In terms of an actual chemical compound, bisphenol-A glycidyl methacrylate (Bis-GMA), urethane dimethacrylate (UDMA) or trithylene glycol dimethacrylate (TEGDMA) are frequently used.
Added fillers.
As a dental restorative, the physical properties of a composite’s core resin matrix (unfilled resin) leave a lot to be desired. As a remedy, fillers and modifiers are added by the manufacturer. The result is the white putty-like compound you see your dentist applying to your tooth.
- Filler particles are added to enhance characteristics such as strength, wear resistance, consistency (handling properties), translucency, polishability, color and dimensional stability when setting.
- Just which of these characteristics are needed most will vary according to the application for which the restorative is used. And to accommodate these different circumstances, a manufacturer will offer a number of product formulations that have been tweaked accordingly.
As examples, a dental composite used to make fillings for back teeth would need to excel in its strength and wear resistance characteristics. For front teeth, color (shade options), translucency (light handling characteristics) and polishability (smoothness, sheen) would be properties that would be more of a concern.
- Compounds frequently used as fillers include barium/lithium-aluminium glass, borosilicate glass containing zinc/strontium/lithium, crystalline silica, silicone dioxide, zirconium oxide and/or zirconia-silica, with the size of the particles (e.g. macro, micro, nano, hybrid) being an important characteristic of the composite.
Filler particle size seems to especially influence a composite’s mechanical strength, wear resistance, polishability and polymerization shrinkage (dimensional change when setting) characteristics.
Variations and advances in acid-etch technique.
What we’ve outlined above describes a dentist’s use of acid-etch technique in its most basic form. And while that may be the exact protocol that your dentist follows, related to a more thorough understanding of the process involved (primarily associated with bonding to dentin), coupled with the introduction of new single-step products, a slightly different clinical routine may be followed. Here are some possibilities:
Total-etch vs. selective-etch vs. self-etch.
a) Total-etch.
This refers to a protocol where the etching gel is placed over the entire tooth preparation (the part of the tooth receiving the dental restoration). The main disadvantage of using this method is related to the possibility of creating postoperative tooth sensitivity (a tooth that has sensitivity after its filling has been placed).
The sensitivity is typically associated with the tooth’s dentin (etching enamel essentially never creates tooth sensitivity). But it’s not that the dentin has been exposed to the etchant but instead that following this step and prior to restoration placement the dentin is not adequately protected/sealed. If it has been (usually by placing a glutaraldehyde-containing treatment), post-op sensitivity should not be a problem.
b) Selective-etch.
With this technique, the etching gel is selectively placed on just those portions of the tooth preparation that are composed of enamel. The exposed dentin surfaces are left unetched but are sealed prior to the completion of the restoration placement.
The potential for postoperative sensitivity is less with this technique but failing to etch some enamel surfaces could be a possibility.
c) Self-etch.
This technique involves the use of specially developed self-etching bonding agents. The application of the product both etches the tooth’s surface (a self-limiting process that etches both enamel and exposed dentin) and serves as the bonding agent (and primer for the dentin too). It’s applied as a single step.
The use of this type of product has advantages (it’s quicker, more controlled/predictable dentin treatment, typically results in less postoperative tooth sensitivity) but may not be effective in etching some enamel surfaces (those not previously freshened up by trimming them with a dental drill).
Which etching method makes the best choice?
Clearly, this is a decision that can only be made by your dentist. There is less potential for the creation of postoperative sensitivity with the selective-etch and self-etch techniques. But when proper protocol is followed, each method can be used successfully. (Christensen 2013)
▲ Section references – Christensen
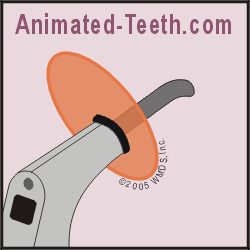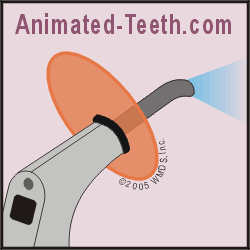
A dental curing light shines blue light that sets dental composite.
Light curing.
Curing light units.
Dental “curing lights” are hand-held units that produce visible spectrum output (light) that lies within a specific wavelength range. Usually, this is blue-colored light that has a wavelength between 420 and 450 nm.
Page references sources:
Christensen GJ. Which technique is best — total-etch, self-etch, or selective-etch?
All reference sources for topic Dental Bonding.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
No etching.
My dentist said they don’t etch teeth any more. They say it causes tooth sensitivity.
KL
Reply –
If your dentist is placing “dental bonding” there absolutely is an acid-etch step involved. It’s a fundamental aspect of bonding technique. But instead of etching the tooth as a separate step, they may be using a combination product that serves as both the etchant and bonding agent.
Due to your comment, we’ve added a new “total-etch, selective-etch and self-etch” section above. It discusses the relationship of these tooth-etching techniques with the potential for creating postoperative tooth sensitivity.
Staff Dentist
Comment –
broken bonding
I had a bonding veneer placed on my tooth and a part of it has come off. My tooth is rough but otherwise seems ok. What is the next step?
patty b
Reply –
From your words and description, we’re assuming that the type of veneer you’ve had placed is 100% composed of dental bonding (dental composite). The type of restoration that would be placed during a single dental appointment.
If so, what you describe is similar to what we explain on this page. It’s quite possible for the strength of the bond between the etched enamel surface and dental composite to be stronger than the internal strength of the bonding itself.
That would explain the roughness you still feel on the surface of your tooth. Some of the composite is still attached to your tooth.
While it’s disappointing that the failure has occurred, it should be an easy fix. It may be that your dentist can even just bond a new layer of restorative directly onto that portion of the dental composite that’s still attached to your tooth (with just minimal or no tooth drilling required).
The most common reason for the failure would be some type of “bite” situation (hopefully rare) where the forces applied exceeded the strength capabilities of the composite. For this restoration to be successful over the long term, you may need to watch out for creating this type of situation (by being careful about how you bite things or what type of objects you bite against).
Staff Dentist