Will you need antibiotics before having your tooth pulled?
You may need to take antibiotics before having your tooth pulled.
Circumstances and safety concerns associated with some extraction cases will require that the patient must take prescription antibiotics prior to having their procedure performed.
How many days of antibiotics are needed before an extraction?
What’s needed will vary according to the specific issues and concerns associated with the patient’s case. In some situations, the course of antibiotics will need to be started a few days before the person’s procedure. For others, a one-time, same-day dose will provide the antibiotic coverage that they need.
Common reasons why antibiotic treatment is needed prior to tooth extraction.
Here’s a list of the most common reasons why a patient might require pretreatment with antibiotics before having a tooth pulled.
Take antibiotics as directed.

Report any bothersome symptoms immediately.
- The patient has a medical condition or issue that requires the use of prophylactic antibiotics (antibiotic premedication).
- The tooth slated for extraction has an associated infection with swelling that needs to be managed before it can be removed.
- Coverage with antibiotics is considered necessary to help prevent post-extraction infection.
Note: In the vast majority of cases, a patient’s risk of developing an infection following their tooth extraction is considered low and therefore the use of prescription antibiotics is not typically indicated.
Following our discussion of the above topics, this page also addresses antibiotic safety concerns and answers a dozen FAQs about antibiotics taken for tooth extractions.
1) Extraction cases requiring antibiotic premedication for medical reasons.
Some medical conditions or issues place the patient at risk of developing a bacterial infection as a consequence of having their tooth pulled.
What’s the concern?
For these patients, bleeding that occurs during their procedure can provide an entry point into their body for bacteria. The bacteria can then spread via their bloodstream (termed a bacteremia). The bacteremia can result in the formation of infection at (typically) distant locations, like in the heart or bone joints.
Antibiotic prophylaxis.
When the patient’s risk for this scenario is considered high, it will be mandatory for them to take “prophylactic” antibiotics before their tooth extraction can be performed. Especially in sequelae involving the heart, not doing so could be life-threatening.
Medical conditions where antibiotic premedication may be required before tooth extraction.
- Patients with certain cardiac conditions (heart problems). – Mitral prolapse with regurgitation, damaged or scarred heart valves (like damage from rheumatic fever), heart valve defects, congenital heart disease, congenital heart defects, cardiac (heart) transplant, hypertrophic cardiomyopathy, a previous history of infective endocarditis/bacterial endocarditis.
- Patients who have artificial objects that have been placed in their bodies. – Prosthetic heart valves, heart valve repair with prosthetic materials (rings, cords), joint replacements/prosthetic joints (knee, hip, etc…), renal dialysis catheters.
- Medical conditions that affect host susceptibility to infection. – Some medical issues place a person at higher risk of developing infection. This includes uncontrolled or poorly controlled diabetes, having chemotherapy or immunosuppressive therapy, and end-stage renal disease.
Print this list for discussion with your dentist about your risks.
Only your dentist can decide if pre-op antibiotics are indicated.
Our list above is not all-inclusive and is purposely vague. Research findings, as well as the opinions of the doctors and organizations who evaluate them when formulating current guidelines, are constantly evolving.
Current opinion about prophylactic antibiotic use.
The current trend in opinion is one where antibiotic premedication is utilized less frequently than in previous decades. This revision is based on the findings of more recent studies, many of which suggest that taking the antibiotic provides little benefit for the patient while leaving them at risk for adverse reactions to the antibiotic itself (see discussion below).
So, if you have a history of having taken antibiotics in association with dental work or specifically extractions, you should feel free to quiz your dentist. But their reasoning is probably based on (possibly different) current guidelines for responsible antibiotic use. Additionally:
- Don’t be surprised if your dentist feels that they must consult with your physician before they decide that prophylactic antibiotics are, or are not, needed.
- In cases where the patient is already taking an antibiotic for other reasons, the usual protocol is that a different one is chosen for use with their upcoming dental procedure.
▲ Section references – Koerner
Antibiotic prophylaxis – What regimen is used?
The regimen used for your antibiotic prophylaxis before your oral surgery will be tailored to you. Generally, it will take the following form.
How many days of taking antibiotics is required?
In most instances, only one day. The chosen antibiotic is typically taken as a single dose, 1 hour prior to the patient’s extraction procedure.
Additional details.
- The antibiotic that’s most frequently used is amoxicillin. In cases where an allergy to it is a concern, clindamycin is usually chosen as the alternative.
- Even if you are currently taking antibiotics for other reasons, your dentist will probably feel that taking an additional dose of a different antibiotic is needed.
- The precise regimen that’s used with your case will, of course, be dictated by your dentist. They may feel a need to consult with your physician before making a decision.
How long after taking antibiotics can your tooth be extracted?
In the case of single-dose (premedication) antibiotics, after waiting an initial hour, a tooth has typically been taken out within 2 to 3 hours of your having taken your medication.
2) Managing existing tooth infections with pre-extraction antibiotics.
Pretreatment antibiotics aren’t usually required when extracting infected teeth for healthy patients. However, cases involving teeth that have caused extensive swelling may require management before the tooth can be pulled. And this management may need to include the use of pre-extraction antibiotics.
How dentists manage swollen infected teeth that need to be extracted.
You might be surprised to learn that managing tooth-related swelling due to the presence of infection via the use of antibiotics only is never your dentist’s first choice. And the presence of swelling or other signs of infection doesn’t necessarily dictate that antibiotics should be used.
Instead, what’s required is that your dentist takes steps that will aid in resolving the swelling associated with your tooth as quickly and predictably as possible.
The preferred approach for managing swelling due to infection.
Whenever possible, utilizing a hands-on approach makes the best plan when dealing with tooth-associated swelling.
One method involves “incising and draining” the infected tissues. To do so, the dentist will make an incision in the swollen tissues which then allows the pus they contain to drain out. The infected tissues may be allowed to drain for some days before the patient’s extraction procedure is then performed.
In some cases, the patient’s signs of infection and level of associated swelling may be such that the dentist determines that going ahead and extracting the tooth still makes a permissible choice. If so, the pus held by the swollen tissues will then drain out via the extraction wound.
Antibiotic therapy may still be indicated.
Even when a hands-on approach is implemented, a dentist may determine that a course of oral antibiotics is still indicated. Doing so can aid in more fully, possibly more quickly, resolving the tooth’s infection and tissue swelling before its procedure.
In these cases, a regimen of 7 to 10 days of taking oral antibiotics is common, with the patient’s tooth being extracted on one of the last few days of the treatment course.
Diffuse swelling may not offer an opportunity for drainage.

Pretreatment antibiotics may be needed.
The last resort for dealing with swelling due to infection.
Related page – We now discuss this topic more fully here: Issues associated with Pulling infected teeth. – Including in the presence of swelling.
What pretreatment antibiotic regimen is used with infected tooth extraction cases?
How many days of taking antibiotics is required?
A total course of 7 to 10 days of taking antibiotics is typical, with the patient’s extraction procedure taking place towards the end of their antibiotic therapy.
How long after you start taking your antibiotics can your tooth be extracted?
Taking 4 or 5 days of oral antibiotics prior to the day of your extraction is common. The remainder of your medication is then taken, as directed, to completion, during the following days.
Additional details.
- Tooth-associated infections typically respond well to penicillin, amoxicillin, clindamycin, or metronidazole.
▲ Section references – Hupp
Extraction of an infected tooth.
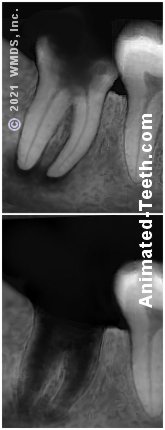
3) The use of antibiotic therapy to prevent postextraction infections.
Some patients may wonder if it’s necessary or routine to take antibiotics prior to oral surgery as a measure to prevent the risk of infection and associated complications following an extraction.
In most cases, taking antibiotics to prevent post-extraction infection is not indicated.
Potential complications associated with the use of antibiotics include: allergic reactions, systemic side effects (diarrhea, nausea, vaginitis, etc…), development of bacterial drug resistance.
What does the research say?
There is relatively little published literature about using antibiotic treatment to prevent postoperative infections after non-wisdom tooth extractions.
A review that did try to investigate this subject (Lodi), but fell short, did conclude that even with wisdom tooth extractions (see below) included in the pool, the incidence rate of post-extraction infection was 1 out of 13 cases.
Considerations with using pretreatment antibiotics to prevent postextraction infection.
As possible factors to consider, we’ll mention the following points.
- The incidence rate of postoperative infection generally rises in relationship to the duration/extensiveness of the patient’s extraction procedure. For example, it is very common for a dentist to utilize preoperative antibiotics with impacted wisdom tooth surgeries, especially lower ones.
[The highest post-extraction infection rate is associated with removing lower impacted wisdom teeth. Studies have placed this number at up to 12% of cases (O’Connor).]
- In cases where the use of antibiotics is indicated but not previously planned for, your dentist has some options.
Taking oral antibiotics as little as 1 hour before your procedure may provide adequate coverage. They may administer systemic (I.V.) antibiotics. They may apply the antibiotic topically (place it in your extraction site immediately following your tooth’s removal).
▲ Section references – O’Connor
What else is important to know about taking antibiotics?
Antibiotic safety concerns and issues –
a) You must follow your dentist’s instructions.
When antibiotics are indicated for an extraction procedure, you must adhere to your dentist’s instructions regarding their usage. Failing to take your medication as directed may render it ineffective. As examples:
- Taking single-dose antibiotic premedication too close to the time of your appointment may not give it enough time to distribute into your bloodstream for your procedure. As a result, your appointment may need to be delayed or rescheduled.
- Individual doses of multi-day antibiotic therapy must be taken reasonably close to their suggested intervals so the antibiotic is maintained at an effective therapeutic level in your bloodstream.
- Multi-dose regimens must be continued, as directed, even during the days after your tooth extraction. Doing so helps to prevent antimicrobial resistance and to make sure your infection is brought fully under control.
b) Make sure to report symptoms and side effects to your dentist.
The use of antibiotics may trigger side effects and these must be reported to your dentist or other healthcare provider immediately so they can assist you with them.
1) Allergic reactions.
Some people experience an allergic reaction to antibiotics. This will vary with the specific medication taken. Cross-sensitivity is possible, so all previous reactions you have experienced must be reported to your dentist.
The reaction may take the form of a skin rash, itching, or swelling. More severe cases may include fever, joint pain, and inflammation. At an extreme, anaphylactic shock may be triggered. It may be life-threatening and requires immediate emergency assistance.
2) Additional side effects.
Other unwanted effects of antibiotics can include nausea, vomiting, diarrhea, and yeast infections. These side effects may range from just mild to severe. Report what you experience to your dentist or healthcare provider so they may monitor your condition and assist you with your symptoms.
c) Responsible antibiotic use is important.
Some patients hold the mistaken opinion that the use of antibiotics with their extraction case holds few consequences other than providing an extra layer of protection for them. In reality, however, your dentist must weigh your case’s needs in light of antibiotic stewardship and responsible use.
Beyond potential (harmful) side effects for you the patient whenever antibiotics are involved (discussed just above), prescribing them only when necessary and in appropriate doses helps to reduce the development of antibiotic resistance and helps to safeguard the effectiveness of these medications for future use. And not just for you but for us all.
Some quick FAQs about taking antibiotics for a tooth extraction.
We’ve covered these issues in our text above but for succinct clarity on these frequently asked questions, here are some quick and simple answers.
Is 5 days of antibiotics enough for a tooth infection?
If the tooth is slated for extraction, 5 days of antibiotics may be enough for your procedure to be performed. Then, afterward, it would be expected that your dentist would have you continue on with them for another 2 to 5 days, for a total of 7 to 10 days of antibiotic therapy.
Is it bad to not take antibiotics before a tooth extraction?
No, most certainly, not all tooth extractions require the added use of antibiotic treatment. In fact, most don’t. Taking them when they are not needed is risky and irresponsible. Only your dentist can determine if they are needed.
Should I take antibiotics prior to a tooth extraction?
If you have consulted with your dentist and they have prescribed them then, yes, it is imperative to take them as directed. However, self-prescribing (like using left-over antibiotics) is likely to be risky, irresponsible, and ineffective behavior.
Can a dentist pull an infected tooth without antibiotics?
It’s all a matter of degree. Dentists routinely pull teeth that have low-grade infections. However, a tooth that displays more severe symptoms, like pronounced swelling, will probably require some type of infection management (possibly including antibiotic therapy) before it can be removed.
Why do I need to take antibiotics before a tooth extraction?
The two most common reasons are to manage an acute infection associated with the tooth that interferes with performing your extraction comfortably and safely. Or else, to prevent systemic postoperative complications associated with the bacteremia (bacteria in your bloodstream) that follows a tooth extraction.
Will a tooth extraction site heal without antibiotics?
Yes, the vast majority do. Developing a new infection after a tooth extraction is not a common event.
Separately, in cases where an active infection has been associated with the tooth and antibiotics were started prior to its extraction procedure, they are typically continued on for a few days afterward and this will help to promote a more favorable healing environment.
How long does it take for antibiotics to clear a tooth infection?
In the case of a necrotic tooth that requires extraction, they won’t ever. The source of the infection lies inside the tooth where the antibiotics can’t reach. However, once the tooth has been pulled, the remnants of the infection remaining in the tissues can then resolve.
Do you have to finish antibiotics before a tooth extraction?
Not necessarily. It’s common for a dentist will feel that they can remove a tooth after around 5 days of antibiotic treatment. The remainder of the prescribed medication is then taken during the following days for a total of 7 to 10 days of therapy.
What happens to a tooth abscess after antibiotics?
In the case of a tooth extraction, once the tooth has been removed, your body with the assistance of the antibiotic will clear up and heal the infected tissues.
What if I forgot to take my antibiotics before having my tooth extracted?
In the case of active infection, and if it hasn’t otherwise resolved on its own, your appointment will probably need to be postponed.
In the case of taking antibiotic premedication (often a single dose regimen), the serious postoperative systemic complications it was intended to prevent may occur. They may be life-threatening.
Can you still have a tooth infection after finishing antibiotics?
In the case of a necrotic tooth that’s going to be pulled, yes, you still do. The focus of the infection is inside the tooth where the antibiotics don’t have an effect. But your situation is better because the antibiotic helps to control the effects of the infection in the tissues that surround your tooth.
Page references sources:
Koerner KR. Manual of Minor Oral Surgery for the General Dentist. Chapter: Infections and Antibiotic Administration.
Hupp J, et al. Contemporary Oral and Maxillofacial Surgery. Chapter: Infections
Lodi G, et al. Antibiotics to prevent complications following tooth extractions.
O’Connor N, et al. Incidence of deep fascial space infections following lower third molar removal.
All reference sources for topic Tooth Extractions.