Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
Guide to Mesiodens / Mesiodentes – Maxillary midline supernumerary teeth.
Extra midline teeth.
Mesiodentes are extra teeth that form between a person’s two upper center teeth. And although having this condition is not extremely common, they are the most frequently occurring type of extra tooth. In many cases, a mesiodens will remain undiscovered beneath the gums and is only first diagnosed via dental X-rays or when some type of developmental abnormality (tooth crowding, spacing, or alignment issues or delayed tooth eruption) becomes apparent.
This guide explains → What a mesiodens is, what causes one to form, and how often they occur. It also covers → Types of problems these extra teeth can create, how they are diagnosed, and the treatment options available. Since management often depends on a child’s stage of dental development, we also offer guidance on when removal is typically recommended and what additional treatment, including orthodontic correction, will likely be needed. (Check out this page’s Table of Contents for a complete list of its topics.)
What is a mesiodens (mesiodentes)?
An erupted mesiodens.
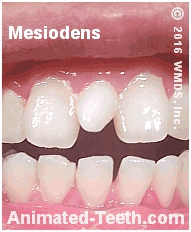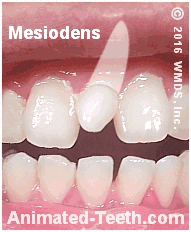
The white shadow approximates the size and shape of its root.
Mesiodens vs. Mesiodentes
If more than one midline tooth is present (which occurs in 20% of cases), the plural form of mesiodens is “mesiodentes” and applies. Also of note, the word “mediodens” can be used interchangeably with the term mesiodens.
Appearance
Most mesiodens have a conical or peg-shaped (see picture above), though they can sometimes resemble a small version of a regular tooth.
What causes a mesiodens to form?
It’s simple enough to say that all teeth, including any supernumerary ones that form, arise from tooth buds. (Tooth buds start to form in the fetus as early as 6 weeks.) Of course, the question then becomes why does the extra tooth bud for the mesiodens exist at all?
▲ Section references – Dean, Russell
Predisposing and correlating factors for mesiodens formation.
There are two issues that seem to have an association with mesiodens formation. One is heredity/genetic factors. The other is specific types of medical disorders or syndromes.
a) Is a mesiodens hereditary? What role does a person’s genetics play?
Having a mesiodens may show a correlation with a person’s family history. For example, twins, siblings, and members of multiple generations of a family line frequently all share a propensity for having an extra front tooth.
It’s also reported that males are twice as likely as females to have one form. And incidence rates are thought to vary according to race. So, heredity/genetic factors/a history of familial occurrence definitely seem to play a role in some cases.
b) What medical disorders or syndromes are associated with mesiodens formation?
Conditions and syndromes that show a correlation with the development of a mesiodens include craniofacial anomalies, such as cleft lip or palate, Gardner’s syndrome, Ehlers-Danlos syndrome, and cleidocranial dysplasia.
▲ Section references – Russell, Meighani
How common is having a mesiodens? How rare are they?
While not incredibly common, the term rare doesn’t exactly apply either. Dental studies report the following statistics about their frequency of occurrence.
- For the general population, the prevalence of hyperdontia (having supernumerary teeth) runs on the order of 0.15 to 3.9%.
The incidence rate for having a mesiodens (an extra tooth between your center two front teeth) generally runs between 0.15 and 1.9%. (Although, this statistic is reported to vary with race. The condition tends to affect males about twice as often as females.)
- Having a maxillary (upper dental arch) mesiodens is much more common than a mandibular (lower) one. 82% of cases are maxillary supernumeraries.
- This condition usually just involves having a single extra front tooth (one mesiodens). But in 20% of cases, multiple mesiodentes are present.
- One-third of people who have a mesiodens have additional supernumerary elsewhere in their mouth.
- Only about 25% of mesiodentes actually erupt into the oral cavity (meaning come through the gums, either fully or just partially) the remainder stay impacted (blocked from eruption underneath the gum line).
▲ Section references – Russell, Meighani
How do you find out you have a mesiodens?
Since between 75% to 90% of mesiodentes remain impacted (lie underneath the gum line), they often go undetected until they are incidentally discovered on dental X-rays or when a developmental abnormality, such as improper tooth alignment or spacing, becomes apparent and is investigated.
This section of our page explains how mesiodentes are diagnosed.
The types of mesiodentes – Classifications.
Mesiodens are categorized according to variations in their morphology (size, shape, and structure).
Eumorphic.
This designation simply means that the extra tooth has a relatively normal appearance. (It just looks like having an extra front tooth.)
Dysmorphic.
This term applies when the tooth is abnormal in size and/or shape.
- A common example is that the tooth appears much more conical than its adjacent teeth. (It looks more like an extra eyetooth rather than a central incisor, see our picture above.)
- At an extreme, a mesiodens may bear very little resemblance to a normal tooth at all (referred to as a “dysmorphic mass”).
▲ Section references – Meighani
What kinds of problems are associated with having a mesiodens?
As an extra tooth that has no intended location of its own, its physical presence frequently affects the normal course of events taking place with neighboring teeth, most commonly the adjacent central incisors.
The kinds of complications that may result include abnormal tooth development (misshapen roots, root resorption, cyst formation). And the disruption of normal tooth eruption (ectopic or delayed eruption, tooth misalignment).
a) Impacted or delayed tooth eruption.
How does a mesiodens interfere with the eruption of neighboring teeth?
Having one of these extra teeth is the most common reason for the delay, or even total failure, of a person’s maxillary central incisors (their two upper center front teeth) to come in. And, in fact, checking for a mesiodens is always at the top of a dentist’s list when this kind of abnormality is first realized.
It’s the physical presence of the extra tooth that causes the problem. It acts as an obstacle that the adjacent erupting central incisors can’t negotiate past. This kind of interference occurs in 26 to 52% of cases when an extra front tooth is present.
b) Abnormal alignment or spacing (diastema) problems.
How does a mesiodens cause crooked teeth?
The presence of one of these extra teeth, whether it comes in (erupts) or not, can cause the adjacent central incisors to be displaced, rotated, or have a gap between them (a diastema). Studies suggest that tooth displacement (alignment irregularities) occurs in 28 to 63% of mesiodens cases.
It’s the physical presence of the extra tooth that’s the problem. Nature must find a way to fit three teeth into the space intended for just two. The only way that’s possible is to shift them out of normal alignment.
c) Tooth root aberrations.
How does a mesiodens cause root abnormalities?
When the extra tooth is present, it may physically encroach upon the space intended for either of the adjacent central incisors’ roots. And this may affect them either during their formation or afterward.
Root dilaceration (extreme root curvature) is one possible outcome. Root resorption (the presence of one tooth causing the root of another to dissolve away) is also possible, although rare.
d) Ectopic tooth eruption.
Irregular/unexpected mesiodens eruption may occur.
Rather than just coming in along with a person’s other teeth, extra front teeth are sometimes grievously misaligned and erupt ectopically (come in at an abnormal location or position). This can include the person’s palate or even their nasal cavity.
e) Cyst formation is possible.
▲ Section references – Russell, Meighani
Treatment and management of mesiodentes cases.
We start this section by answering several frequently asked questions about having a mesiodens and what is generally suggested as treatment. Then, following those answers, we provide more detailed information about how cases are handled for people of different age groups and are at different stages of dental development.
General FAQs about how a mesiodens case is usually handled.
a) Does a mesiodens tooth need to be removed?
Yes, it is an extra front tooth and as such has no place in a person’s dentition (set of teeth). Its presence typically interferes with adjacent teeth, especially the central incisors, and prevents them from coming in and/or aligning properly. Even if a mesiodens finds a way of erupting, its abnormal size and shape will spoil the appearance of the person’s smile.
b) When should a mesiodens be removed?
The timing of its extraction should be adjusted according to the patient’s stage of dental development, which is generally a function of their age.
Some of the factors a dentist juggles when making this decision are: 1) Is the patient old enough to tolerate the procedure? 2) Timing their surgery for when developing adjacent teeth are least likely to be damaged. 3) Performing the work before it has caused significant dental complications.
c) How is a mesiodens tooth removed?
Removal typically involves the situation where the tooth still lies fully embedded within the jawbone. (None of the tooth is visible.) As such, it must be removed via “surgical” extraction. (A process where overlying gum tissue is reflected back and bone is removed so accessing the tooth and removing it are possible.)
In cases where the tooth has instead erupted (has come through the gum line, either fully or partially), performing a conventional extraction may be possible. However, eruption only occurs in about 20 to 25% of cases.
d) Is it painful to have a mesiodens removed?
No, pain during your procedure shouldn’t be a factor. Your dentist will numb you up just like with any other tooth extraction.
Afterward, your potential for post-extraction pain will generally correlate with the level of surgical trauma created during your procedure. Patients undergoing more involved surgeries (like removing an unerupted/impacted mesiodens) tend to experience greater postop pain.
e) How much postop recovery time is needed following mesiodens removal?
The amount of rest and recuperation you’ll require will depend on how extensive your procedure has been.
Following a simple, routine extraction (like when removing a small erupted mesiodens), taking the remainder of the day off is usually adequate. But aftercare for surgical extractions may require a day or two of rest and recovery.
f) Are braces needed after mesiodens removal?
Frequently, yes. The fact that the extra tooth was originally present typically disrupts normal dental development. In turn, this often results in the patient’s adjacent teeth being crooked or possibly not coming in at all. As such, orthodontic treatment is frequently needed to guide them into proper alignment.
In some cases, however, especially if tended to at the proper point in the patient’s dental development, simply removing the offending tooth may allow nature to follow its normal course with the patient’s teeth then correcting on their own.
Details about treating a mesiodens case – According to age group.
The treatment plan required for a mesiodens will need to vary according to the age (stage of dental development) of the patient. Here are some examples.
a) For very young children.
Unerupted mesiodentes discovered in very young children are typically left alone for the time being. A part of the concern is that the surgical process needed to remove them could damage the adjacent developing permanent central incisors.
b) For children with mixed dentition.
Once a child has first entered the mixed dentition stage (a point where their first permanent teeth should have started to come in), a dentist may recommend that the extra tooth should be extracted.
- Performing surgical intervention at this point may help to promote the “spontaneous” eruption of the permanent incisors. (The situation where the teeth come in on their own unassisted. In contrast, sometimes even after removing the extra tooth the incisors still don’t erupt, and therefore require orthodontic assistance.)
- Removing the tooth during this stage/age may allow the erupting permanent teeth to achieve a more normal alignment.
However, during this period of dental formation, there is a risk that the surgical process needed to extract the extra tooth might result in damage to the forming roots of the neighboring central incisors.
c) For older children and adolescents.
Wait and watch.
In cases where the mesiodens has been identified early on (like via x-ray examination), a decision may be made to just keep the child’s situation under observation.
- As their growth and development continue, the supernumerary tooth may erupt, therefore making the oral surgery associated with its removal less of an ordeal.
- The permanent incisors may erupt too, although they’ll likely be malpositioned and therefore require orthodontic intervention.
- The presence of the mesiodens may prevent the permanent incisors from erupting. Due to this failure, the baby teeth above them may be retained (don’t fall out as expected).
Extracting the mesiodens.
The dentist may plan to only observe the child’s situation until that point when more complete root formation (2/3rds to 3/4ths, as determined by dental x-rays) has occurred. (The root formation of upper central incisors is generally expected to be completed by ages 9 to 10 years.)
At this point, the surgical process of removing the embedded supernumerary is less likely to result in damage to these, now almost completely formed, teeth.
As for the type of practitioner that should remove the supernumerary, the patient’s pedodontist (pediatric dentist) or general dentist may feel they have the skill set needed to remove the tooth. This would be common in the case of an erupted mesiodens. For those that remain impacted, a referral may be made to an oral surgeon.
Difficulties associated with this approach.
The forces that cause tooth eruption tend to diminish with age. And that means that the later in life that a mesiodens is extracted, the more likely it is that the patient’s central incisors won’t go ahead and come in on their own (erupt spontaneously).
If spontaneous eruption is ultimately able to occur, it may take some months or years following the removal of the offending extra tooth. And for this reason, after its extraction, the dentist will need to periodically monitor the incisors via x-rays to get a hint of what progress they are making.
Assisted orthodontic eruption.
In cases where it appears that the incisors have adequate space in which to come in but haven’t shown any progress within the last 6 to 12 months, the dentist may determine that they need assistance.
This typically consists of exposing the unerupted teeth (a minor oral surgery procedure) and then attaching some type of orthodontic appliance (braces) to them, so to assist and guide them into place.
An erupted mesiodens.
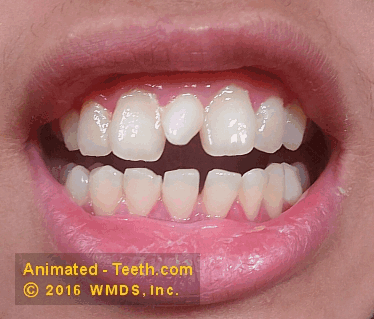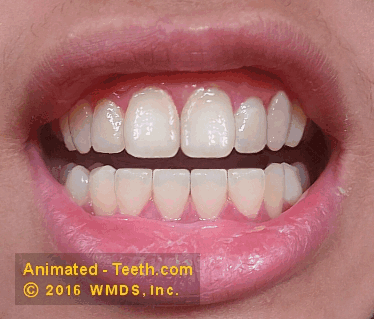
Treatment includes extracting the mesiodens and then performing orthodontic treatment.
Orthodontic treatment.
Whether this treatment can be accomplished via the use of fixed braces (metal wire and brackets) or removable orthodontic appliances will vary according to the specifics of the case.
d) Adults / Cases discovered late in life.
It may be that even though a mesiodens is present, the person’s permanent teeth have still been able to come into place satisfactorily. If so, a decision might be made that the unerupted extra tooth should not be removed but instead only monitored.
▲ Section references – Dean, Russell
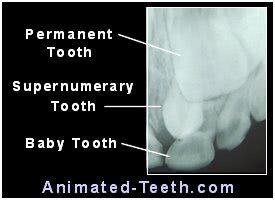
This periapical x-ray reveals the presence of a mesiodens (supernumerary tooth).
How is a mesiodens usually discovered?
In most cases, these extra teeth are first identified via radiographic (x-ray) examination.
That’s because about 75 to 80% of mesiodentes don’t erupt (pierce through the gums) and therefore can’t otherwise be seen or confirmed. (Although, developmental abnormalities noticed with adjacent teeth may hint that a buried extra tooth exists.)
What kind of x-ray is needed?
Since a mesiodens occupies a position directly adjacent to a person’s other front teeth, discovering one is possible using pretty much any type of dental x-ray that’s taken to visualize this area. This would include periapical or maxillary-occlusal radiographs (somewhat common views to take). Or a panoramic (full-mouth) radiograph or cone-beam computed tomography (CBCT) scan.
However, it’s common that detection at an early age is frequently hampered by the fact that the anterior (front) portion of the jaw isn’t always included in routine x-ray evaluations of young children. As a result, x-ray pictures that would easily reveal the presence of a supernumerary tooth aren’t taken.
Other methods of diagnosis.
a) Baby tooth mesiodens discovery.
Deciduous supernumeraries frequently do erupt. But due to their normal-looking appearance, and the fact that young children often aren’t seen by a dental professional, they are frequently overlooked and have come in and ultimately fallen out without ever having been identified.
A simple tooth count is one way they can be discovered in a child’s primary dentition. (The normal number of deciduous teeth is 20.)
b) Permanent tooth mesiodens discovery.
It’s fairly common that a search for the presence of a mesiodens in a person’s permanent dentition isn’t begun unless the patient’s permanent central incisors (one or both) are late in erupting, or else have come in but are displaced in position and/or alignment.
Additional tip-offs include that the primary (baby tooth) incisors have been over-retained (haven’t fallen out on schedule, usually at around age 6 to 7 years). Or else that the permanent incisors have erupted ectopically (have come in in an abnormal location).
Looking for more information?
One tip-off that your child has a mesiodens is that their expected pattern of tooth eruption and exfoliation has become disrupted. Use our link to find out what’s normally expected so you can compare.
Many mesiodentes patients will require orthodontic treatment to correct the tooth alignment issues caused by their condition. Nowadays you have a number of different types of orthodontic systems to choose from.
FYI, another type of supernumerary tooth is the 4th molar (these are extra wisdom teeth). If you’d like to learn more about them, use this link: Supernumerary wisdom teeth.
Last reviewed: April 18, 2026
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Dean JA, et al. McDonald and Avery’s Dentistry for the Child and Adolescent. Chapter: Development and Morphology of the Primary Teeth.
Meighani G, et al. Diagnosis and Management of Supernumerary (Mesiodens): A Review of the Literature.
Russell KA, et al. Mesiodens — Diagnosis and Management of a Common Supernumerary Tooth.
