Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
Surgical Tooth Extractions: Why are they needed? Techniques. What to Expect.
Guide to surgical extractions.
A surgical tooth extraction is performed for complex extraction cases. Unlike a routine simple extraction, a surgical one includes additional procedural techniques that help to ensure the success and safely of the procedure.
The added steps may include raising a gum tissue flap, removing bone tissue from around the tooth, and sectioning the tooth into smaller pieces for easier removal. Surgical extractions are commonly required for impacted wisdom teeth, severely damaged teeth, teeth surrounded by dense bone, or those that have a challenging root anatomy.
This guide explores when surgical extractions are necessary, the techniques dentists use, and what to expect during the process. It emphasizes that a surgical extraction isn’t a “bad thing”—instead it’s the best way to ensure a predictable and efficient procedure while minimizing surgical trauma, which is exactly what you want. So, read on and learn what will take place.
What is a surgical extraction?
The term Surgical tooth extraction refers to the process used to remove teeth that includes additional “surgical” steps that aren’t performed during routine extractions. Routine/”Simple” extraction protocol. These added steps may include:
- Creating a gum tissue flap. – With this procedure, an incision outlining a section of gum tissue is made. The area of tissue is then reflected (peeled) back, thus providing your dentist with access to the bone tissue and/or tooth that lies underneath.
- Removing bone (ostectomy) – Trimming away bone tissue may be needed to give your dentist better access to, or a better view of, your tooth. Or it may be required to create an opening through which your tooth is taken out.
- Tooth sectioning – This is a process where your tooth is cut into pieces (“sectioned”), so it can be removed more easily.
When does a tooth extraction qualify as a surgical extraction?
When one or more of the above techniques are used, the procedure is formally categorized as a “surgical” extraction. Procedures that don’t require any of these steps are termed “simple” extractions. Surgical vs Simple example.
This page’s highlights as a video –
Subscribe to our YouTube channel.
When are surgical extractions needed?
Indications / Applications
There can be a number of situations where the nature of a tooth’s extraction is expected or discovered to be more complicated or challenging than with routine cases. And as such requires the inclusion of one or more of the above surgical techniques as a means of helping to lessen the complexity, difficulty, or risk of the procedure.
A decision to include these additional techniques might be planned, anticipated, or even an impromptu event. Situations can include:
- Severely broken or fragile teeth.
- Teeth that have challenging root morphology – Like molars (which have 2 or 3 roots) or any teeth whose roots are especially curved or exceptionally long.
- Impacted teeth. (Wisdom teeth / third molars are a common example.)
- Dense or inelastic bone tissue surrounding the tooth.
- Root tip retrieval.
Our next section discusses the difficulties and challenges that the above situations can pose for a dentist and then explains what surgical steps (gum tissue flap, bone removal, tooth sectioning) are used to overcome them. (Jump to a specific section using the links above.)
If instead you’d rather learn more about the process itself, use this link: Surgical tooth extraction procedure details.
Problem situations and their surgical solutions –
1) Broken teeth.
Many teeth are slated for extraction because much of their crown (the portion of a tooth that lies above the gum line) has been lost (fractured, broken) or severely damaged (like by decay), and now the tooth is beyond repair.
Or it’s possible that during its extraction procedure, a tooth has broken (for example, the crown of a weakened tooth might break off at the gum line), therefore leaving little of the tooth visible or accessible to the dentist.
The difficulty this causes – In cases where significant portions of a tooth are missing, the shape of the piece(s) that remains may be difficult for the dentist to grasp or manipulate with their extraction instruments.
And since these are the tools the dentist will use to remove the tooth, the dentist now has a dilemma.
Solutions for this situation.
One remedy is for the dentist to remove bone from around the pieces of the broken tooth that remain, so they’re more accessible and visible. Then, once this process has been completed, the tooth can be worked and removed using conventional extraction instruments.
How it’s done.
- In some cases, the procedure that’s used to remove the bone may be as simple as the dentist using their drill to create a trough around the tooth, thus exposing more of it.
If so, the whole process may be completed in just a minute or two, with little extra attention required for the wound because this technique has been used.
- With other cases, the dentist may find that they need more of the tooth exposed, or a greater extent of bone removed to reach where the broken bit lies. If so, a gum tissue flap will be raised, then the bone underneath trimmed away.
This scenario is a more involved surgical process than the first one. And afterward, stitches will be needed to hold the flap in place as it heals.
(See below to learn more about both of these procedures.)
2) Fragile or cracked teeth.
Beyond just having missing parts, what remains of a broken tooth may be fragile. And traumatized teeth that may still appear substantially intact, may have cracks that suggest to the dentist that they’ll fracture during the extraction process.
The difficulty this causes – Teeth are extracted by way of applying forces to them. And these same forces might be enough to break a fragile tooth. If so, the portion that remains in the tooth’s socket may be difficult to access and manipulate, thus adding greatly to the degree of difficulty of the procedure.
Solutions for this situation.
With these types of situations, the dentist may decide that approaching the tooth’s procedure as a surgical one right from the start makes the best plan because it minimizes the chances of complications associated with the unpredictability of the tooth fracturing.
Here’s how performing a surgical extraction can help.
- Removing some of the bone that encases the tooth’s root(s) can make it so it can be loosened up and removed with less force, thus reducing its chances of fracture.
- The dentist may decide to section the tooth. “Sectioning” means cutting a tooth into pieces and taking them out individually.
As an example, a two-rooted molar might be cut in half. That way each piece, each having one of the roots attached, can be removed separately.
(See below for more details about these procedures.)
3) Teeth with long or curved roots.
An extraction’s level of difficulty often hinges on the configuration of its roots. (This is one reason why dentists typically recommend that wisdom teeth should be removed before full root development has occurred. Rationale / Example.)
Here are some of the root-related challenges that a tooth may pose that a dentist can manage by performing its extraction surgically:
a) Curved roots – Teeth that have especially curved, hooked, or crooked roots can be stubborn extractions. Especially in the case where the tooth has multiple roots (like molars that characteristically have 2 or 3 roots).
Due to their extreme root anatomy, the act of pulling these teeth may require the use of excessive force that can result in bone or tooth breakage.
Solutions for this situation.
Molars (including wisdom teeth, which are third molars) are frequently sectioned when pulled. Doing so is a way of transforming more challenging 2 and 3-root tooth extraction cases into simpler ones. Now, since each piece just has a single attached root, each piece can be removed using less force than if the tooth were still whole.
Additionally, with the tooth sectioned into pieces, the dentist will have the luxury of removing portions having especially curved roots individually, instead of locked together as a stubborn, difficult-to-manage unit.
(See below for more details about sectioning teeth.)
b) Long, large roots – Teeth (like eyeteeth, canines) that have relatively larger, longer roots will take more force to extract than those that have comparatively shorter, smaller ones (such as lower incisors).
And when having to extract a tooth with a longer root, the dentist doesn’t want to be placed in a position where they must apply excessive force. Doing so puts the tooth, surrounding bone, and even the jawbone at risk of fracture.
Solutions for this situation.
By removing some of the bone that encases the roots of stubborn teeth, or sectioning them into parts if multi-rooted (like when performing 2 and 3-root tooth extractions), the dentist can lower the level of force they must use, thus lowering the risk of procedure complications.
(See below for more details about these procedures.)
c) Thin, fragile roots – Comparatively longer, thinner roots will be more likely to break during a tooth’s extraction process. And this concern doesn’t just exist with small teeth. Some of the individual roots of large multi-rooted teeth can be small and fragile and therefore easily broken too (molars have 2 or 3 roots, premolars may have 2 roots).
Solutions for this situation.
In cases where a dentist fully expects that a tooth’s root(s) will break, a surgical extraction (bone removal, sectioning) may be indicated. That’s because, at the time of surgery, broken root tip retrieval can be routine but isn’t always.
For example, the layer of bone that encases the tips of the roots of upper molars can be paper-thin. So in the case where a root does break, an attempt to retrieve the piece that remains may result in it being pushed through this fragile bone and into the nasal sinus. If this occurs, this is a major complication.
(See below for more details about these procedures.)
4) Impacted teeth.
Tooth “impaction” involves the situation where a tooth has not been able to come into its normal position in the mouth. And as a result, it still lies buried by gum tissue and possibly bone tissue too.
The type of tooth that’s most likely to be impacted is the 3rd molar (wisdom tooth).
[Use this link for a graphic illustrating the different impaction types Pictures / Diagrams discussed below.]
With impacted teeth, by definition, a surgical extraction will be required. (To flap back gum tissues and remove bone when necessary to access the tooth). It’s only a question of what additional surgical steps will be needed (like sectioning a 2 or 3-rooted molar).
a) Soft tissue impactions. – This is the case where the tooth is only buried by a layer of gum tissue.
Solutions for this situation.
The dentist will need to make an incision in the overlying gum tissue and then reflect it back as a flap.
Now that the tooth has been exposed it can be removed, possibly just using routine extraction techniques. The flap is then positioned back and tacked into place using stitches.
(See below for more information about tissue flaps.)
b) Partial-bony impactions. – This classification involves teeth whose upper portion is both buried underneath the gums and partially encased by bone.
Solutions for this situation.
Just as above, the gum tissue must be flapped back so the tooth is exposed. Whatever bone stands in the way of removing the tooth is trimmed. The tooth is then removed and the tissue flap is repositioned and stitched into place.
(See below for more information about how these procedures are performed.)
c) Full-bony impactions. – With this situation, the impacted tooth is fully encased in the jawbone. (The most difficult types of wisdom teeth to remove are full-bony impactions.)
Solutions for this situation.
The same general steps taken with partial-bony impactions are performed here also, although much more bone tissue is trimmed away. And while any of the cases discussed above may, this one frequently involves the use of tooth sectioning technique to cut the tooth into smaller pieces that can then be removed individually.
(See below for more information about tooth sectioning.)
5) Dense, inelastic bone.
The underlying difficulty – Conditions may exist that have affected the bone that encases the roots of a tooth. This can include increased bone density (often a result of excessive tooth clenching and grinding) and age-related bone inelasticity.
Other patients may have added deposits of bone on their jaws (termed exostoses) whose presence complicates the extraction process.
Solutions for this situation.
With these cases, the use of bone removal or tooth sectioning techniques can help to reduce the level of force that’s needed for the extraction, thus making it a more controlled and predictable process.
(See below for more information about these procedures.)
6) Root tip removal.
The underlying difficulty – The outcome of a tooth’s extraction process may be such that the fractured tip of one of its roots has either been inadvertently, or possibly purposely, left behind.
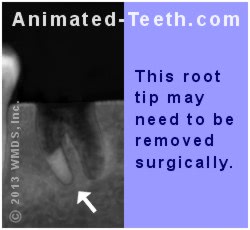
Some bone removal may be needed to retrieve this root tip.
Over time, the broken piece may remain in its original location, or possibly migrate toward the jaw’s surface. Why they move. But either way, if at some point a decision is made to retrieve the root tip, a surgical extraction will likely be needed.
Solutions for this situation.
The type of procedure needed will simply depend on the tip’s current position.
- If it now lies close to the surface of the gums, a minor incision through the overlying tissue may create enough access to flick it out.
- If the broken tip still remains encased in bone, a tissue flap and bone removal will be required to retrieve it.
Surgical extractions – Procedure details.
There are 3 basic surgical techniques that might be utilized during a tooth’s extraction. They are:
a) Tissue flaps.
A gum tissue flap is created and raised (peeled back / lifted) when the tooth or bone lying underneath needs to be accessed during the extraction procedure.
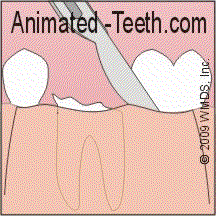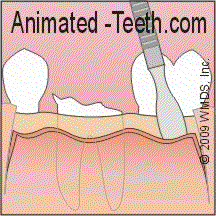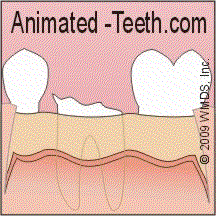
Creating a flap allows access to the jawbone surrounding the tooth.
Then, once the tooth has been removed, it’s positioned back into place and stitches are used to hold it there during the initial phases of its healing process.
Use this page “Gum tissue flaps procedure” The steps. for information about how they’re designed and made, as well as information about types of, placing, and removing stitches.
b) Trimming bone.
- Changing the nature of the extraction – By removing some of the bone that encases a tooth’s root, the dentist can change (reduce) the level of force that’s needed to loosen and remove it.
This is a positive thing because it helps to make the extraction process more controlled and predictable. When excessive forces must be used, tooth or bone fracture or jaw joint aggravation may occur.
- Access –When extracting broken teeth, surrounding bone is often removed so more of the tooth is exposed. This makes it easier for the dentist to grasp and manipulate what’s left of the tooth, thus making the extraction process more like a conventional one.
In the case of impacted teeth (like wisdom teeth), the purpose of removing bone may be as fundamental as being what’s needed to even access the tooth.
Whatever the purpose, as the dentist makes their plans one of their prime considerations will be how to keep the amount of bone they remove as limited as possible.
Trimming away bone – The process.
a) Removing bone immediately adjacent to and within the tooth’s socket.
In cases where much of the tooth is missing and what is left is its root portion in its socket, the dentist may already have the direct access they need to remove bone.
This type of situation might exist when pulling teeth that have already fractured, or those that during their extraction procedure have broken or been sectioned into pieces (see below).
What the dentist will do.
Since they already have the access they need, a dentist will often just go ahead and trim away bone tissue from around the tooth using their dental drill. Doing so can be a quick and simple way of exposing more of the tooth without making a big production out of the process.
Deeper within the socket, this same method might be used as a way of removing bone from in between individual roots, or simply creating whatever additional space is needed for better instrument access.
Issues.
One advantage of this method is that no secondary wound is created (like when a gum tissue flap is raised, see below). The trimming is primarily accomplished within the wound that would have generally existed anyway. This is favorable for the healing process.
What you’ll experience.
If your dentist does things this way, it won’t be much of an issue for you. You’ll hear the noise and feel the vibrations of the drill as it’s being used. Other than that, it should be a non-issue.
Trimming bone in this manner may take very little time. And as opposed to a separate step, it’s often just incorporated into the flow of the procedure.
Since they don’t want to remove more bone than is necessary, a dentist will frequently drill an initial amount, then try to remove the tooth. If it doesn’t come out as expected, and after evaluating why, they’ll make adjustments in their plan and trim some more.
b) Removing bone external to the tooth’s socket.
In situations where the bone that needs to be removed lies in an area covered by gum tissue, a flap will need to be raised.
This type of scenario would apply to cases such as removing impacted wisdom teeth (where a layer of bone lies over the tooth) or removing the bone alongside a tooth (so to expose a portion of its roots, so it’s easier to remove).
What the dentist will do.
- The dentist will first need to plan and then make the incision(s) needed to create the gum tissue flap (see above). They’ll then reflect (peel) it back.
- Once exposed, the bone can then be removed (either via the use of a drill or hand instruments).
- Once the extraction has been completed, the flap is closed and tacked back into place with stitches.
Issues.
The fact that along with bone removal a gum tissue flap is raised too makes this a more involved procedure than that described above.
And because a flap is created, a higher level of surgical trauma is experienced than with routine extractions, and this will affect the duration of the healing process that follows. Extraction healing timeline.
In cases where choosing to perform this step is even remotely optional, what the dentist is trying to accomplish by doing so is to create trauma “surgically” (quickly, neatly, in a controlled manner) as opposed to via the blunt force typically created during a messy, blundered extraction (i.e. torn or bruised tissues, broken, bruised or otherwise traumatized bone and broken teeth.)
What you’ll experience.
You’ll feel pressure as the outline of the flap is scored with a scalpel and then peeled back. The procedure.
You’ll also hear the sounds and feel the vibrations and pressure created by the tools used to remove the bone (probably a drill, possibly hand chisels). But other than that, this whole process should be a non-event.
The addition of this step will mean that your extraction may take a little longer. With simple cases, just an extra 10 minutes or so. With impacted third-molar extractions (wisdom teeth), this step may be a major component of the extraction process.
After your procedure has been completed, it’s important for you to understand if you need to return to have your stitches removed or not.
Minimizing trauma to the bone.
Whichever of the above methods is used, first on your dentist’s mind will be making sure that the drill they use doesn’t overheat the bone tissue during their work. They’ll do this by flushing the site with water (or preferably saltwater) continuously throughout the trimming process.
This constant irrigation will also wash away spicules of loose bone that are created (they could interfere during healing). It also helps to keep the bone moist during the extraction process.
▲ Section references – Fragiskos, Koerner, Wray
c) Sectioning teeth.
Tooth sectioning, or “controlled tooth division,” can help to lower an extraction’s level of difficulty. By splitting (sectioning) a tooth into parts, an otherwise potentially challenging extraction, like 2 and 3-root tooth extractions (molars), can be transformed into a simpler procedure because now each part can be removed individually.
What sectioning accomplishes.
Tooth sectioning has various purposes. They include:
Sectioning a molar.
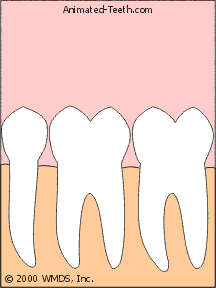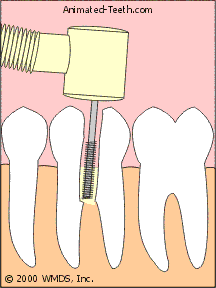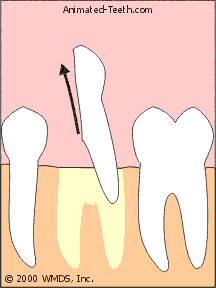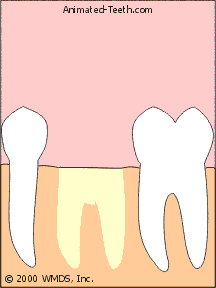
Each piece is easier to remove than the tooth as a whole.
- Reducing the level of force needed to remove the tooth. – By splitting a multi-rooted tooth into parts, each piece can be removed using less force than if the tooth were whole.
Complications that the use of excessive extraction force can potentially lead to include tooth root breakage, jawbone fracture, fracture of the maxillary sinus, jaw joint (TMJ) irritation or damage, and causing damage to adjacent teeth.
- Simplifying a tooth’s configuration. – Multi-rooted teeth that have especially curved, hooked, or crooked roots are frequently sectioned. That way each root’s path of withdrawal out of the socket can be managed individually.
Without sectioning, these types of extractions are often difficult and result in root breakage.
- Allowing smaller access. – In the case where bone tissue must be removed to gain access to impacted teeth (like wisdom teeth), sectioning the tooth into smaller portions allows it to be removed through a smaller opening (see picture below).
A smaller wound is favorable for the healing process and results in a smaller post-surgery defect (“dent”) in the jawbone.
How are teeth split up?
The dentist’s goal when sectioning a tooth is to divide it up into smaller parts. But each one must still remain large enough to be easily manipulated by their extraction instruments.
- In the case of a two-rooted lower molar, a logical place to cut the tooth is in half, right between its roots (see picture above).
- With some impacted wisdom teeth, the tooth’s crown portion may need to be cut off and removed first. Then the root portion can be sectioned and removed.
Sectioning an impacted molar.
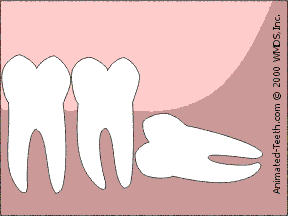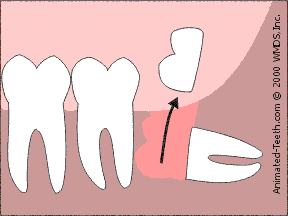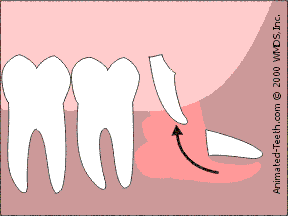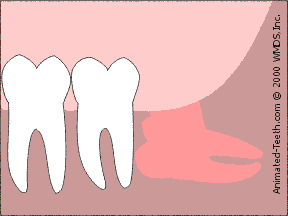
By sectioning the tooth into parts, less bone removal is needed.
How does a dentist section a tooth?
Nowadays, teeth are usually sectioned using a dental handpiece (drill). [In the past, teeth were broken into parts using a mallet and chisel.]
- During this process, the dentist will continuously flush the working area with water.
This removes any chips or fragments that are created. It also helps to keep the amount of bone-traumatizing heat that’s generated during the process to a minimum.
- After the tooth has been sectioned, the individual pieces are teased out using conventional extraction instruments (forceps and elevators).
- The pieces may be interlocking, so sometimes it takes getting the first one out before the others follow more easily.
What you’ll experience.
Sectioning a tooth into pieces typically does involve cutting into its pulp chamber and nerve tissue. The good news is that since your tooth has already been numbed for its extraction, you won’t feel it as it does.
- You will hear the sound of the drill and feel the vibrations it creates as it works.
- In some cases, your dentist may cut your tooth most of the way through but not all. They’ll then split the two halves apart by wedging a tool in between them. If so, you’ll feel a little bit of pressure as it’s applied, and then a snap as the two parts separate.
Other details about surgical extractions.
Yours may be planned or unplanned.
As beneficial as the surgical steps we discuss on this page can be, no dentist will choose to include them in their patient’s extraction process unless they feel sure they are needed. As examples:
- During your pre-treatment examination, your dentist may discover reasons why they feel a surgical extraction should be planned right from the start. Examples of these reasons are given at the top of this page.
- Your dentist might observe clues that hint that surgical steps will be needed but they choose to hold off on them until they have further proof.
For example, the pre-op x-ray that’s been taken of your tooth Yes, one will be needed. may suggest that the bone encasing its roots is quite dense. Finding the tooth very difficult to loosen during the initial stages of your extraction process would confirm this fact for your dentist. If so, they might immediately switch to the use of a surgical approach.
- As a last scenario, the nature of the routine extraction that your dentist expects might suddenly change. For example, the crown of your tooth might snap off at the gum line. If so, a switch to a surgical approach would be likely.
Don’t be frightened of the idea of having a surgical extraction.
As a patient, the last thing you want is for something unexpected to happen during your tooth extraction. Or for the process to be more difficult than it needs to be (including the healing process).
Implementing surgical steps with your procedure generally means that it will go more quickly and predictably, and likely result in less overall surgical trauma, than if the potential undesired events did occur.
Try to think of having a surgical extraction as a form of insurance, in the sense that it places your dentist in a position where they have more control. Thus helping to guarantee that your entire experience will be as pleasant and uneventful as it can be.
Details about: “Simple” (routine / “non-surgical”) tooth extractions. What they’re like. ▶
Last reviewed: February 21, 2025
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Ahel V, et al. Forces that fracture teeth during extraction with mandibular premolar and maxillary incisor forceps.
Fragiskos FD. Oral Surgery (Chapter: Surgical Tooth Extraction)
Koerner KR. Manual of Minor Oral Surgery for the General Dentist. (Chapter: Surgical Extractions)
Wray D, et al. Textbook of General and Oral Surgery.
Video transcription.
Hello. Welcome to Animated Teeth.com and our page that discusses surgical tooth extractions.
It seems likely that anyone would have some confusion about what the term surgical extraction actually means. After all, pulling any tooth is considered oral surgery.
Well, dentists and the coding system that’s used for filing dental insurance claims generally categorize extractions into two broad groups.
One is simple extractions. This term applies to most procedures and refers to the situation where the tooth being pulled holds a relatively normal position in your jaw and the steps needed to remove it are straightforward and routine, like the case where a dentist can grasp the tooth with extraction forceps and then wrestle it on free.
The term surgical extraction applies when some type of additional steps are required. Exactly what’s needed will be different with each case but some common examples are raising a gum tissue flap, removing bone from around the tooth, or dividing the tooth into sections so each piece can be removed separately.
As a starting point in explaining further, you might wonder what kind of situations might warrant a surgical extraction.
Well, removing impacted teeth or a residual root tip, like one left behind during a previous extraction attempt, are common examples.
In both of these cases, the tooth or root remnant can’t be directly handled and removed because it lies underneath the gum line. Extra steps will be needed to create access.
Other examples can include severely broken teeth, like those broken off at the gum line and therefore are difficult for the dentist to get leverage on with their instruments. Or teeth that seem fragile and are expected to break, possibly problematically, when using a conventional extraction approach.
As a last group, some teeth that require a surgical procedure are generally intact and do have a relatively normal positioning in the jawbone. But as a complication, they are anticipated to be difficult to remove.
This might be because they have exceptionally long, curved, or divergent roots. Or their surrounding bone tissue is exceptionally dense.
As far as what additional procedural steps might be needed during a surgical extraction, here’s an example that illustrates the need for three common ones, raising a gum tissue flap, removing bone tissue, and sectioning the tooth.
Our animation here illustrates a lower impacted wisdom tooth. It still lies fully underneath the gum line and, in fact, is entirely encased within the jawbone. As yet another challenging feature, the tooth has an abnormal orientation in that it lies on its side.
As a process, it’s pretty obvious what the dentist will need to do to get at the tooth. They’ll first flap open the gum tissue to expose the bone underneath. They’ll then remove the least amount of bone possible that still gives them adequate access to the tooth below.
As a final step, and one you probably don’t have any familiarity with, to get the tooth out more easily, and through a more conservative opening in the bone, the dentist will section the tooth, meaning they will cut it into preplanned pieces so each one can be removed separately.
So, with that case, it’s pretty obvious why all of those steps are needed. But why would a surgical extraction be needed for a tooth that’s already come through the gums?
Well, take a look at this next animation. The tooth is fully erupted. Its roots aren’t exceptionally long or curved. But maybe the dentist has already tried to muscle this tooth out and they just can’t get it to budge. As an explanation, maybe the bone tissue surrounding it is exceptionally dense.
At this point, the dentist’s concern would be that if they use an even greater level of force the tooth may break and that could complicate the procedure. A solution could be to section the tooth in half so they can address their efforts to just one root at a time. Divide and conquer.
With this case, the act of sectioning the tooth changes the previously attempted simple extraction into a surgical one. Changing course in midstream isn’t uncommon if difficulties are encountered. But different than with our impacted tooth example, no gum tissue flap or bone removal is needed to create access. The dentist will just drill directly into the tooth to cut it in half.
As another example of a surgical extraction, here’s an animation that shows a severely broken tooth. With this case, there simply isn’t enough exposed sound tooth structure for the dentist’s instruments to get leverage on to remove it.
As a solution, if a gum tissue flap is raised, the dentist can then trim away some of the surrounding bone, so to lessen its grip and expose more of the tooth so the dentist has more to work with. Maybe the dentist will even section the tooth into two, like with our last example.
So, the steps taken here, while the same as with our impacted-tooth example, are implemented differently. But it’s still a surgical extraction.
So, now you know some of the steps that might be taken during your procedure and why. But there’s one last point we’d like to cover.
Some people might cringe at the idea that their tooth requires surgical extraction. And we get that concern. After all, having one probably sounds like a whole different ballgame than what you likely expected.
But what you’d be overlooking, especially in cases where the need for a surgical process isn’t so clear to a layperson, is this. It’s not just that your dentist has concluded that the additional steps will help them get your tooth out more easily. They’re also trying to ensure that your extraction process creates as little surgical trauma as possible. This is important because your healing process and its risk for complications will be influenced by what has occurred during your surgery.
Yes, incising gum tissue, removing bone, and sectioning a tooth will create trauma. But that which occurs during a poorly planned, difficult simple extraction can be expected to be greater.
This can include traumatizing surrounding bone tissue due to an inordinate amount of prying at or rocking back and forth on a tooth that is reluctant to yield. Or bruising or even tearing soft tissues in an ad hoc attempt to gain better access or visibility. Not to mention that the degree of difficulty of the extraction can be significantly raised if some type of unfavorable tooth or bone breakage occurs.
The fact is, the dice were already cast long before your dentist informed you that you needed a surgical extraction. Evidently your tooth has challenging characteristics. And planning to remove it surgically is your dentist’s opportunity to improve your procedural experience and minimize your potential for post-operative complications. So, try to see things in that light.
With that, we’ll conclude this video. Our page contains many more details about surgical extractions, so be sure to give it a read. Good luck with your procedure. Goodbye.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
Surgical broken tooth extraction.
I have a broken tooth that needs to come out. The tooth doesn’t hurt but the dentist says that what’s left is so decayed that a crown can’t be placed. My dentist says that a surgical extraction is needed and that I need to take sedation medication for it. I’m scared, this seems like a big process.
Kelly M
Reply –
Your situation seems to be one where tooth extraction seems to be the only option. If so, you should look at your dentist’s pre-treatment planning of your extraction as a surgical one a very positive thing.
A dentist with less clinical expertise might first attempt your extraction as a conventional (simple) one, only to fail.
Instead of that (which involves you sitting through the failed attempt, creating additional tissue trauma, extending the length of your procedure, etc…), your dentist has identified that surgical steps are needed. By doing that right off the bat, your procedure will be quicker and less eventful, both during your procedure and the healing process that follows. Those are all very positive things.
As far as the use of the medication for your procedure goes, it’s not uncommon that some type of sedation method is used with surgical extractions. And in your case you clearly state you are scared about the procedure, so that seems a reasonable thing to do. In general terms, using it helps you to be more relaxed, and gives your dentist a more compliant/cooperative patient. Once again, these things are all positive. Good luck.
Staff Dentist
Comment –
Difficult tooth extraction.
My wisdom tooth was extracted a week ago and lots of pain I have had for the last two days. It was a very stuff extraction process due to its location and I heard him complain of one root that was still in place after the extraction but later on lost its whereabouts. Am back to the hospital and AwAiting an x Ray to be done to rule out any remnant roots. Am worried about her competence.
Joseph O.
Reply –
Since we obvious know nothing about the circumstances involving your situation, it’s not possible for us to state anything specific. In our response, we’re making the assumption that the treatment was provided by a general dentist.
Any dentist will tell you that what it takes to actually complete a procedure (level of skill or expertise) may be different that what they initially thought would be required. With the question then becoming, was their level of expertise one where they should have suspected that the procedure would be difficult (like noticing telltale signs on an x-ray).
For anyone else reading in preparation of an extraction, about all you can do is ask the dentist bluntly: Is this a type of extraction you routinely perform? Is this the type of extraction that general dentists routinely refer to an oral surgeon? Is there anything about the tooth or situation that might indicate that referral would make a good choice?
Make it clear to them that the process and outcome of the procedure are as important to you as factors such as cost or convenience, and that you are open to the idea of being referred if that makes the more predictable procedural choice.
Joseph, we hope you have a quick recovery. While you don’t mention, we assume that your having a dry socket has been ruled out as the problem.
Staff Dentist
Comment –
Hollowed out tooth.
I was told 2 years ago when I went back to have a tooth removed I would have to see a specialist in case it broke. I was told roots were right at my sinus cavity. Does that sound right?
tt
Reply –
Your dentist seems to anticipate that the same paper thin layer of bone both encases your tooth’s roots and serves as the floor of your sinus. As such, this fragile bone may break off and stay attached to the tooth when the tooth is removed, thus necessitating some type of repair. Or if a root breaks off during the extraction process, when trying to to retrieve it it may get pushed through the thin bone and into the sinus, thus necessitating yet another procedure to retrieve it from there.
As bad as all of that sounds, what is difficult for a general dentist accomplish is often fairly routine for an oral surgeon to prevent and/or handle. Your dentist simply wants you in the most capable hands possible if complications arise. But they certainly don’t know for a fact that they will.
Per your question: Yes, sectioning the tooth, or removing bone from around the tooth as described above, may be an appropriate technique to use with your tooth to lower the risks associated with its extraction (either making tooth fracture or sinus floor fracture less likely). But only the person extracting the tooth can determine if that is needed.
Staff Dentist
Comment –
Surgical Tooth Extraction
Good day,
Can surgical tooth extraction be done with just dental shots only to numb the area, without any form of sedation? Thank You.
Elle
Reply –
Yes, and that’s probably the norm. The use of sedation has to do with helping the patient tolerate the procedure (fear, long procedures, and such). If those issues don’t apply, then it’s not needed.
Here’s a link to our page that discusses sedation.
Staff Dentist
Comment –
Fast Tooth Extraction – Hammered it loose
Had a tooth extracted yesterday. Upper right #12 or #5. It was 1/2 decayed, couldn’t be repaired, saved.
Without warning, my dentist used some kind of hammer, mallet, to loosen tooth from bone without breaking it into pieces. I was shocked & traumatized with the amount of pressure I felt….OMG…luckily, I was numbed up enough so I felt no pain.
I still can not believe that this dentist was hammering, 2-3-4, hard blows to my tooth. I don’t know how he did it. I had never even heard of such a procedure. I’m wondering, why isn’t this procedure described anywhere, & if it’s not common procedure, are there any side affects to my jaw, mouth, etc., that I should be watching for? I also hope that the teeth on each side did not get whacked with all that hammering force, pressure.
Geeeeezzzz….???
L.R.
Reply –
Historically it was common for dentists to use a mallet and chisel to section teeth (cut them into multiple pieces for easier removal).
When air turbine dental drills became widely used in dentistry (1960’s), they became the preferred choice for this task. [That’s not to say that using a (air driven) drill necessarily makes a better choice. But it does create a more pleasant patient experience.]
While we can imagine that oral surgeons still use a mallet and chisel for some purposes and situations, it’s not so common for a general dentist to do so.
We will mention that teeth #5 and #12 are sometimes two-rooted teeth. So possibly the dentist did have sectioning in mind. However, doing so for these teeth isn’t necessarily common practice.
You mention that the tooth was extensively decayed, implying that there was little tooth structure for extraction forceps to grasp. From that, we’re assuming your dentist drove their tool into the ligament space between the tooth and bone (like how a dental elevator is used, although usually just with hand pressure), thus the tooth came out.
Since we know so little about your procedure, we won’t second guess your dentist’s choices.
Generally a dentist will be concerned about the level of forces applied, for fear of breaking bone, pushing the tooth beyond it’s socket (like into the sinuses) or traumatizing adjacent teeth. No doubt your dentist had factored these issues in.
As far as what to watch for, we have a page that describes the expected healing process after extractions. If you notice anything that diverges from that, you should be in touch with your dentist for evaluation.
If there was any major bone breakage, we’re assuming your dentist would have identified that at the time of your procedure. Any small fractures might not be identified, but would also likely just heal uneventfully on their own (with no one ever knowing they really existed).
In general, the sharp edges of tooth fracture should be apparent now. Sensitivity issues associated with cracked teeth or traumatized tooth nerves would also be expected to be apparent this time frame.
Longer term, bone fracture issues will have shown themselves and/or healed. It’s possible that trauma to teeth during the extraction might lead to future problems (need for root canal, tooth breakage, the expansion of small cracks created during the extraction process) but all of those things would be essentially impossible to directly correlate to events during your procedure.
Staff Dentist
Comment –
Tooth cutting.
Went to dentist yesterday. Dentist told me that there is very small place to pull your tooth so I will have to grind other tooth to make space for extraction. Please advice, I am phobiatic to doctors and dentist is like a nightmare for me.
What can be done?
Hemant Bhave
Reply –
Without knowing a single thing about how your tooth is positioned, about all we can state is the following:
Here’s a quote from Hupps textbook of oral surgery:
“… crowded or otherwise malposed teeth may present difficulty in positioning the usually used forceps onto the tooth for extraction. When access is a problem, a different forceps may be needed or a surgical
approach may be indicated.”
Our point here is that no mention is made of making changes to the adjacent teeth. Trimming down the tooth being extracted would be a harmless option. Or removing the tooth via a surgical procedure, possibly involving sectioning it into pieces that are easier to withdrawal from the cramped confines, would be a common approach too.
With difficult cases, like yours seems to be, a referral to an oral surgeon might be indicated.
Staff Dentist
Comment –
Horizontally Impacted Wisdom teeth.
Hello, my dentist has diagnosed me as having lower horizontally impacted wisdom teeth. He has thus recommended a surgical procedure involving sectioning. He also mentioned that there is a risk of nerve damage in such procedures, but was quick to also mention that my risk is quite low as the nerves are adequately distant from the teeth. I am however curious; how much distance is adequate distance? Also, would taking nerve rehabilitating medication immediately after the procedure improve my safety chances? And professionally, would you remove one tooth at a time or both?
PS: One of them though in the same impacted position, does not have an negative symptoms at the moment.
Isaac Simbwa
Reply –
We don’t really have any information to share about a specific distance that might be considered safe. The bone itself is compressible, so beyond just the absolute thickness of bone that exists, the way the tooth is handled during the extraction (amount pressure applied to the tooth while working it loose, what the tooth’s path of withdrawl is (which would be different for straight or curved roots) would be important too). Obviously your dentist is taking this into consideration by choosing to section the tooth. Doing so helps to reduce the level of concern associated with these issues.
We’ll also state that it’s only with 3D x-ray imaging that the distance could even be measured, which is a type of imaging that most general practitioners don’t usually have. So, if your dentist does, all the more reason that their opinion is quite informed about your situation.
You don’t really mention if the dentist you have consulted is an oral surgeon. One would anticipate that the skill and experience level of an oral surgeon would tend to reduce the chances of complications like paresthesia. If your dentist is a general dentist, you might bluntly ask if there are any reasons why they might feel that a referral to an oral surgeon is indicated for your case.
In regard to medications, we have little to share other than what is stated here. If you’ll notice, we only discuss the use of anti-inflammatory drugs. Commenting on the benefits of using other types of drugs lies beyond scope of our website.
As far as whether to remove 1 or both teeth (left and right lower 3rd molars). The extractions are essentially unrelated. If you can tolerate both procedures, and enough time is set aside to do both without constraints, and your dentist feels that doing so is appropriate, then you might follow their advice. The advantage of doing so is that you only go through one healing process, not two separate ones. Good luck with your procedure(s).
Staff Dentist
Comment –
Extra teeth growing in my mouth.
Good day,
I have experience allot of pain m,I have 4 extra teeth growing in the front bottom teeth on the curves , It has been extremely painful.
Could you please tell me what procedure they will have to do for that.
Tonia
Reply –
On YouTube, I see a video titled “surgical extraction of fully impacted supernumerary canine.” From your description, one would think your procedure would be similar to what’s shown.
For background information about extra teeth, here’s our page about supernumeraries.. Best of luck with your procedure.
Staff Dentist
