Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
What Does a Dry Socket Look Like? – Guide to Dry Socket Appearance, Signs, Symptoms, and Healing Timeline
Guide to Dry Sockets – Signs, Symptoms, and Appearance.
It’s normal to experience some pain or discomfort after a tooth extraction, but if the pain intensifies a few days after your procedure, it may indicate that you are developing a dry socket. This common complication occurs when the protective blood clot in the tooth’s socket becomes dislodged or dissolves prematurely, exposing the underlying bone tissue and interrupting the healing process.
This guide will explain for you what a dry socket looks like, how it feels, and how what is going on differs from normal healing. You’ll learn to recognize its key warning signs, such as throbbing pain, bad breath, and its characteristic empty-socket appearance. Additionally, the guide outlines the typical timeline for dry sockets, how long they tend to last, and what to expect while your recovery progresses. (Check out this page’s Table of Contents for a complete list of its topics.)
By recognizing the signs and symptoms of a dry socket early on, you can seek treatment sooner. Doing so will minimize the amount of discomfort you experience and help to get your extraction site’s healing process back on track.
This page’s highlights as a video –
Subscribe to our YouTube channel.
What is a dry socket?
A dry socket, more formally termed alveolar osteitis, is a common postoperative complication associated with having a tooth extracted. It involves a situation where an extraction site’s healing process is interrupted (delayed) due to the loss of the blood clot that normally occupies the tooth’s empty socket.
Dry socket signs and symptoms.
The predominant characteristics of having a dry socket are:
- Throbbing (possibly very intense) pain.
- Bad breath – A foul odor and/or bad taste coming from your extraction site.
- A scenario where these events have first appeared a few to several days following your tooth extraction procedure.
How can you tell if you have a dry socket?
There’s no formal testing that’s performed to identify alveolar osteitis. Instead, your signs and symptoms are compared to what normally occurs following a tooth extraction.
a) What’s normal healing like? What usually happens after a tooth is pulled?
- In most cases, a patient will experience some degree of discomfort from their extraction site on the day of their surgery. (Hopefully, this will just be minor.)
- And then with each day that follows, the level of pain they notice gradually tapers off until it finally disappears.
- And as each day passes, the site shows continued, although very gradual, progress in healing.
b) What’s different when a dry socket begins to develop?
As alveolar osteitis sets in …
- The patient will find that their initial discomfort does gradually fade over the first few days following their extraction. (Just like with normal healing.)
But then, usually somewhere between days 2 and 4 following their procedure, their level of pain begins to intensify.
- During this same time frame, the patient may start to notice a bad taste or odor coming from their extraction site.
- On inspection, the patient will notice that their tooth’s socket appears empty. (Evidence of blood clot loss and/or disintegration.) The bony walls of the interior of the socket may be visible.
▲ Section references – Kolokythas
Here’s a recap of the above information in tabular form for comparison.
Dry socket formation vs. normal healing. – Major differences.
| Dry Socket formation. | Normal healing. |
|---|---|
| Post-op pain lessens over the first days but then gets worse. | Levels of post-op pain gradually improve each day. |
| The tooth socket appears empty. (Only some or none of the original blood clot is visible.) | The tooth socket appears relatively full. (With blood clot and developing tissues.) |
| Within the socket, regions of exposed bone are visible. | No visible exposed bone tissue. |
| Bad taste coming from the extraction site. | No associated taste. |
| Bad breath. Foul odor coming from the extraction site. | No associated breath odors. |
Dry Socket Signs & Symptoms quiz.
Worried that you may have a dry socket? Our Dry Sockets Signs & Symptoms quiz can be a quick way to figure out if you do. Learn what’s usually noticed with this complication and see if that applies to you.
https://www.animated-teeth.com/?p=235#quiz
Additional details about the symptoms associated with a dry socket.
1) What does a dry socket feel like?
Pain and discomfort.
In cases where a dry socket develops, the level of discomfort the patient notices from their extraction site typically starts to intensify on days 2 to 4 following their extraction. (48 hours following the procedure, or later.)
This detail alone is an important characteristic clue that helps to confirm for your dentist that you do in fact have a dry socket.
a) What does a dry socket feel like at first?
The first tipoff that a dry socket is starting to form is typically a gradually intensifying, frequently throbbing, pain coming from the area of your extraction site.
b) How bad can a dry socket hurt?
- The discomfort typically (almost characteristically) takes the form of a dull throbbing ache.
- What’s felt can range from moderate to severe in intensity. Using a pain scale of 1 to 10, the level of discomfort can be, at times, a full 10. Some people describe the pain as the worst they’ve ever experienced.
- The discomfort that’s felt may be constant or intermittent. If intermittent, its frequency can vary. Over time, the pain is likely to become constant.
- The pain may remain localized to just the extraction site, radiate to other portions of the jaw, or even extend to other areas on the same side of the patient’s head such as the ear or temple, or possibly even the eye or neck. Experiencing headaches is also reported.
- The pain usually reaches its most intense/highest pain scale level around 72 hours post-extraction (Bowe). The pain may be so debilitating that it causes loss of sleep and affects the person’s ability to function.
c) How long does dry socket pain last?
On average, the discomfort usually runs for 4 to 8 days. That means you’ll likely need attention from your dentist to stay comfortable. How dentists treat dry sockets.
During this time period, there can be times when the pain you experience can be quite severe (a pain scale rating of 9 or 10). Toward the latter days of your ordeal, however, your discomfort will gradually taper off and finally just disappear.
What does a dry socket feel like to your tongue?
As your tongue explores your wound, you may be able to ascertain that the tooth’s socket seems empty and open. (Due to the loss of its blood clot.) You may be able to feel the sharpness of the socket’s exposed bony surfaces.
2) What does a dry socket look like?
A picture of a dry socket.
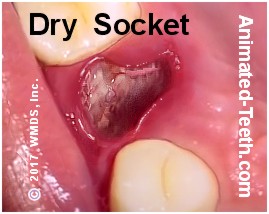
Note the loss of the socket’s blood clot and exposed bony interior.
- The tooth’s socket will appear empty instead of being filled in with a blood clot or granulation tissue (new developing tissue) like with normal healing.
(In many cases, the emptiness of the socket isn’t readily apparent because it’s filled with saliva, or accumulated food and debris.)
- The exposed bone of the walls of the empty socket is visible. It may be partially covered with a gray/yellow layer of necrotic tissue or other debris.
- The gum tissue immediately surrounding the extraction site shows signs of being inflamed (red, tender, puffy).
How does a dry socket’s appearance compare to normal healing?
- With normal healing, the tooth’s socket remains substantially filled. (First with the blood clot that forms and then with the developing tissues that arise from it.)
- No exposed bone is visible.
- The contours of the extraction site continually become more and more rounded as the bone and soft tissues of the wound gradually heal over.
3) What do dry sockets smell and taste like?
Characteristic signs of having a dry socket include noticing a bad taste in your mouth and having bad breath (halitosis).
The compounds that create this odor and taste are the byproducts of the breakdown of necrosing tissues, blood cells, and accumulated food debris harbored in the depths of the socket. Additionally, the waste products of oral bacteria that thrive in this type of environment are well known for producing offensive tastes and odors.
The odor that’s noticed is usually just described as foul or possibly even putrid. The taste of a dry socket might be described as foul, sour, fishy, or metallic.
4) Additional signs and symptoms associated with dry sockets.
- The lymph nodes in your jaw or neck (on the same side of your body as your wound) may feel tender and enlarged. (A sign of the body’s inflammation response to conditions associated with the dry socket’s formation.)
- Dry sockets are typically not associated with the presence of fever, swelling of the surgical region, or obvious signs of infection, local or systemic. (This last point is an important one to note. It explains why antibiotics are not usually indicated in the treatment of alveolar osteitis.)
▲ Primary reference sources for entire Characteristics section – Kolokythas, Bowe, Noroozi
5) How often do dry sockets occur?
Statistics show that experiencing alveolar osteitis is a relatively common post-extraction complication. Although, by far, it’s most common following wisdom teeth removal.
An impacted lower third molar slated for extraction.
The potential for dry socket formation is a concern with these extractions.
- For routine tooth extractions, the chances of experiencing a dry socket run on the order of 1 to 4%.
- They’re much more likely to occur with lower tooth extractions than upper ones.
- In general, surgical extractions (like impacted wisdom tooth removal) have a tenfold higher incidence rate.
- As many as 38 to 45% of mandibular (lower) wisdom tooth extractions (see picture) are complicated by the subsequent formation of a dry socket.
- With all tooth extractions considered collectively, a dry socket is the most common post-surgical complication.
▲ Section references – Cardoso, Bowe
6) Dry socket timeline.
How long does it take for a dry socket to form?
Characteristically, symptoms don’t start to appear any sooner than 2 to 3 days following your extraction. 95% of dry socket cases are apparent within the week following the patient’s procedure. (Kolokythas)
How long do dry sockets last?
Once a dry socket has set in, it usually takes about 7 to 10 days for the extraction site’s healing process to get geared up again and create new granulation tissue that then starts to cover over and protect the socket’s exposed bone. As this process advances, you can expect your symptoms to begin to subside. (Noroozi)
How long do they hurt?
The pain from a dry socket usually lasts for 4 to 8 days. At times, the pain may be quite intense. But as the healing process finally manages to make progress, the discomfort will finally taper off.
How much is your wound’s healing process delayed?
In general, you can expect that the healing of your extraction site Normal healing timeline. will be delayed on the order of a week or longer.
How do you know when your dry socket is over?
A dry socket is a set of symptoms associated with interrupted (delayed) wound healing. As conditions within the extraction site correct themselves and get back on track, the symptoms produced by the site’s irritated tissues will gradually subside.
Once your symptoms have disappeared, it’s expected that this complication has run its course and your healing process will continue on to completion.
▲ Section references – Noroozi, Kolokythas
7) How are dry sockets treated?
Pain relievers on their own (over-the-counter pain medications and even prescription narcotics) are seldom fully effective in managing the discomfort associated with a dry socket.
Treatment.
The most effective treatment for pain associated with a dry socket is one where the patient’s dentist inserts a special paste (medicated dressing), daily if needed, directly into the wound How that’s done.. In a pinch, there are some home remedy methods Instructions that can be used to provide pain relief.
Then in conjunction with that treatment, over-the-counter medications (like aspirin, Advil/Motrin/ibuprofen or other nonsteroidal anti-inflammatory drugs (NSAID)), or prescription medications if needed, are used to control whatever level of discomfort continues to persist.
8) Etiology – Why do dry sockets form?
Dry socket risk factors.
Research and clinical observation have identified a number of factors that correlate with a patient’s risk for developing alveolar osteitis. They include:
- Previous history of dry sockets. | Extraction difficulty. | Failing to follow aftercare instructions. | Cigarette smoking/Tobacco products use. | Taking birth control pills. | Age. | Tooth location.
Understanding these factors can be useful in preventing this condition. Our Dry socket risk factors page provides greater details about them.
That’s why following your dentist’s post-operative instructions is so important.
As noted above, failing to follow your oral surgeon or dentist’s instructions (especially those that address blood clot formation and retention) places you at an increased risk of experiencing this complication.
For more information, our pages Post tooth extraction instructions – First 24 hours. Next day and beyond. cover this subject in detail.
The cascade of events associated with dry socket formation.
The exact pathogenesis of the formation of alveolar osteitis is not fully understood but it is known that the following factors are involved.
1) The blood clot is lost.
A course of events takes place where the blood clot that normally forms in a tooth’s socket following its removal isn’t properly retained. It either:
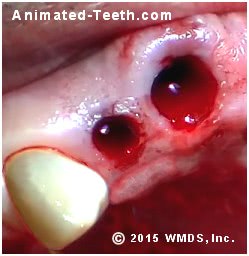
The blood clot that begins to form immediately after an extraction is an important part of the healing process.
- It disintegrates by way of a chemical process termed fibrinolysis.
(Fibrin is a tough fibrous protein whose formation is triggered by the clotting process. Pieces join together to form long strands that then crosslink with others. As this process continues, and the web that’s formed snares platelets, it develops into what’s referred to as a blood clot.)
It’s hypothesized that the compounds responsible for this fibrinolytic activity may come from the socket’s bone itself, either as a consequence of infection or as a result of trauma created during the extraction process. (Noroozi)
- It is dislodged by an event or activity.
(Common scenarios involve loss of the clot as a result of vigorous swishing, rinsing, spitting, or the creation of a sucking action, like when drinking using a straw.)
▲ Section references – Noroozi
2) The wound’s healing is interrupted/delayed.
The lost blood clot would have played an important role in the healing process of the extraction site. However, due to its loss, the progress of the socket’s healing is interrupted (delayed).
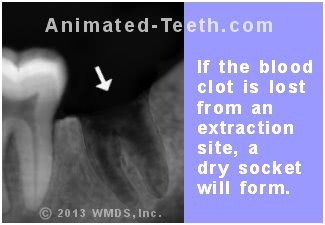
If the blood clot is lost, the socket’s bony interior is exposed instead of protected.
3) The socket’s bone tissue becomes exposed.
The clot would have also covered over and protected the bony walls of the tooth’s empty socket as it heals. Now that it’s been lost, the walls are exposed and become irritated, resulting in (possibly intense) pain and sensitivity.
Looking for more information?
If you’ve read this page, it seems likely that you suspect that you have a dry socket forming. If so, we suggest that you read this page next: How dentists treat dry sockets.
As an alternative, we do have a page that discusses DIY dry socket remedies. But keep in mind that professional treatment is always considered more effective, and appropriate.
If instead you’ve read this page because you have an upcoming extraction (like the removal of an impacted wisdom tooth) and are concerned about possible complications then, then read this page: Risk factors for dry sockets. Its information may save you some discomfort.
Last reviewed: April 18, 2026
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Bowe DC, et al. The management of dry socket/alveolar osteitis.
Cardoso CL, et al. Clinical concepts of dry socket.
Kolokythas A, et al. Alveolar Osteitis: A Comprehensive Review of Concepts and Controversies
Noroozi AR, et al. Modern concepts in understanding and management of the “dry socket” syndrome: comprehensive review of the literature.
Video transcription.
Hello, and welcome to Animated Teeth.com and our page that discusses dry sockets, their signs and symptoms, and appearance. Using this video, we’ll highlight some of the primary points we cover that we feel you should know about when sorting through this subject.
This page’s coverage is divided up into a few subsections.
Since it’s usually the timing of the patient’s symptoms that leads to making a diagnosis, we cover that first. And compare what’s experienced to normal post-extraction healing.
Then, while less diagnostic, we discuss the appearance of a dry socket, and compare that to what’s seen with normal healing.
This page also explains why dry sockets form, how often this complication tends to occur, and how long it usually lasts.
We should point out that this isn’t our primary page that discusses treatment for this condition. We instead have two companion pages that cover that. One explains how dentists treat alveolar osteitis, the formal name for a dry socket. The other discusses the possibility of self-treatment.
As far as signs and symptoms go, what’s reported by the patient, and especially their mention of the timing of events, is usually the cornerstone on which a dentist bases their diagnosis.
The standout characteristics of a dry socket are throbbing pain, which can be very intense, and possibly a foul breath odor. But the most important point is this. These symptoms don’t start to appear until some days, usually 2 to 4, following your procedure. That’s the key, the timing.
To recap that point, with normal post-operative healing, the patient can expect that as each day passes, the discomfort they notice from their extraction site will continually, gradually diminish.
With a dry socket, pain levels will start to subside for a few days but then start to ramp up. And associated halitosis may be noticed. And if the person can see in their tooth’s socket, they will probably discover that it seems empty. The blood clot that was noticed previously now seems at least partially missing.
Here’s a comparison of normal vs. alveolar osteitis in tabular form.
In regard to discomfort, the classic description of dry socket pain is “dull and throbbing.” It may be constant or intermittent. Its intensity can vary but at times may be debilitating. The pain may seem focused at your extraction site or can extend into portions of your head and face.
Unfortunately, there is no cure for a dry socket, it simply needs to run its course, which typically takes 4 to 8 days. In the meantime, the most effective means of controlling your discomfort comes from treatment from your dentist, so let them know you need help.
If you can see into your extraction site, the classic description of a dry socket is one where the socket looks empty. If it doesn’t, it may still contain a portion of the blood clot that had formed or it may be full of food and debris.
If you can see the socket’s bony walls, they may be covered with a gray-yellow layer of necrotic debris. Your gum tissue around the opening will be red and puffy, which are signs of inflammation.
With normal, uneventful healing, no exposed bone will be visible. The tooth’s socket will appear substantially filled in.
At this point, you’re probably wondering why dry sockets form. They’re a situation where the extraction site’s healing process is interrupted and therefore delayed.
The crux of the problem lies in the fact that the blood clot that formed immediately following your extraction has become compromised, either disintegrated by chemical mediators or dislodged. And since it provides the scaffolding for the continued progress of the healing process, your socket finds itself back at square one, although now with exposed irritated tissues.
While developing a dry socket isn’t routine, it’s certainly not uncommon. Comparatively more difficult or involved extractions tend to be more frequently associated with their formation, especially removing lower impacted wisdom teeth.
There are other risk factors too, including a previous history of having a dry socket, tobacco product use, possibly increased age and taking oral contraceptives, and, drum roll please, not following your dentist’s aftercare instructions. Look for our supplemental page, shown here, that discusses these issues in more detail.
There’s a lot more information on this page than we’ve covered in this video, so make sure to read through it. However, as advice to you if you’re currently experiencing a dry socket, by far it’s your dentist’s care that will be most effective in controlling your pain. So, as your extraction provider who is also obligated, and probably very eager, to provide you with postoperative assistance, be sure to take advantage of their services. Good luck.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
Pain and odor post 8 days
I received resorbable sutures after having all four wisdom teeth extracted. It has been a week since the surgery and I have a terrible odor/taste in the back of my mouth constantly. Most similar to a fishy smell. This smell is accompanied by pain from the cheeks to the jaw on both sides of my face. Without ibuprofen and Tylenol it is unbareable. I am taking amoxicillin and prednisolone but have about finished the he round of anitibiotcs prescribed. How normal is any of this?
Jt
Reply –
What you need is evaluation by your dentist. Even via initial telephone contact they should be able to develop a fair idea of what is going on and what type of attention you require.
As you’d expect, the usual course of events would be one where pain diminishes with time. Some of what you report seems consistent with a common postoperative complication referred to as a dry socket. That might explain what is going on. Your dentist will need to make that determination.
Staff Dentist
