Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
3 Key Causes of Bad Breath ( 1. Anaerobic oral bacteria 2. Smelly volatile sulfur compounds 3. Tongue film. ) and 8 Factors That Worsen It.
What’s the primary cause of bad breath?
Bad breath, medically known as halitosis, is primarily caused by anaerobic oral bacteria that produce foul-smelling volatile sulfur compounds (VSCs). These bacteria thrive in the film that accumulates on the back of the tongue and around teeth, leading to unpleasant odors.
Several additional factors can exacerbate bad breath, including dry mouth conditions (such as morning breath or xerostomia), smoking, gum disease, sinus conditions, certain foods, medical and dental conditions, and dentures.
This guide explores all of these topics in depth. Gaining an understanding of the science behind halitosis is a key step toward effective prevention and treatment. By addressing both the primary causes and contributing factors, you can improve your oral health and regain confidence in the quality your breath.
What kinds of odors come from your mouth?
Imagine the smell of rotten eggs, an animal feedlot, urine, feces, sweaty feet, and rotting meat. Now, imagine that all of these odors were mixed up into a single cocktail and you had to take a whiff.
Well, that’s pretty much what you do every time you smell someone else’s breath. The same exact compounds that cause each of those kinds of stinky smells (see list below) are found in everyone’s mouth.
And when their concentration is high enough, you’ll have bad breath. Or, if you can keep their levels to a minimum, you won’t. And there you have it. The whole subject of what causes bad breath is as simple as just that.
Bad breath is caused by smelly “volatile sulfur compounds.”
Just like humans, bacteria consume foods and in turn excrete waste byproducts. And, unfortunately, the waste byproducts produced by some types of oral bacteria are smelly sulfur compounds. And it’s these molecules that usually lie at the root of a person’s breath odors.
Some of the foulest smells you know are caused by sulfur compounds.
- The stench of rotten eggs is due to the compound hydrogen sulfide.
- The stinky smell that comes from feedlots and barnyards is created by the sulfur compound methyl mercaptan.
- The odor you associate with the ocean is partly due to the presence of dimethyl sulfide.
▲ Section references – Aylikci
In scientific terms, halitosis is caused by “Volatile Sulfur Compounds” (VSC’s) …
Dentists refer to the foul-smelling sulfur byproducts excreted as waste by oral bacteria as “volatile sulfur compounds” (VSC’s). And it’s their presence in the air we exhale that others detect as “bad” breath.
[The word “volatile” describes the fact that these compounds evaporate (transform into a gas) quickly, even at normal body temperature. It’s this property that explains how these compounds are able to escape our mouth so rapidly and easily.]
FYI: When it comes to halitosis that’s caused by oral bacteria (which is 90% of all bad breath cases), the primary VSC’s involved are usually hydrogen sulfide and methyl mercaptan.
Additional stinky compounds that may be involved …
While the VSC’s in our first list above are generally considered to be the primary causative agents of bad breath, other types of volatile molecules can play a role too.
Some of these are the compounds that are responsible (at least in part) for the unsavory odors listed below.
- Cadaverine – Urine, decaying meat.
- Putrescine – Rotting meat.
- Skatole and Indole – Human fecal matter.
- Propionic and Isovaleric acid – Sweat and sweaty feet.
- Butyric acid – Human vomit.
- Pyridine – Unpleasant fish-like odor.
It all boils down to concentration.
▲ Section references – Lourith, Aylikci
Volatile sulfur compounds are created by anaerobic oral bacteria.
Most of the compounds that cause bad breath are the byproducts of anaerobic bacteria (more specifically Gram-negative anaerobic bacteria).
The term “anaerobic” describes the fact that these types of bacteria do best in an environment that’s devoid of oxygen.
FYI – Research suggests that the human oral cavity may be home to as many as 500 bacterial species, most of which are capable of producing smelly compounds that can cause bad breath.
But in particular, the following types of anaerobic Gram-negative bacteria have been identified as key producers of VSC’s.
- Bacteria typically associated with dental plaque build up around teeth – Fusobacterium nucleatum, Porphyromonas gingivalis, Tannerella forsythia, Prevotella intermedia, and Porphyromonas endodontalis.
- Bacteria typically associated with debris build up on the surface of the tongue – Veillonella, Actinomyces, Prevotella, Capnocytophaga, and Odontomyces (in populations age 70 and beyond).
- Bacteria that generate high levels of hydrogen sulfide – Peptostreptococcus, Eubacterium, Eikenella, Centipeda, Selenomonas, Capnocytophaga, Veillonella, Propionibacterium, Porphyromonas, and Fusobacterium
- Bacteria that generate high levels of methyl mercaptan – Fusobacterium, Bacteroides, Porphyromonas, Eubacterium, and Treponema denticola.
It’s possible that some types of Gram-positive oral bacteria, primarily Streptococci, may also contribute to VSC formation.
A proposed mode of action is one where these bacteria cleave off sugar chains from glycoproteins, thus reducing them to a more basic form of protein molecule that’s then available for digestion by Gram-negative bacteria.
▲ Section references – Suzuki, Calil, Danser
The key to controlling bad breath is to control the number of causative bacteria that live in your mouth.
The human oral cavity is home to hundreds of different types of bacteria. And there’s a constant battle for living space between the types that cause bad breath (which are mostly Gram-negative anaerobic ones) and those that don’t.
It’s the precise balance between these two that ultimately determines the quality of a person’s breath.
a) The role dental biofilms play.
The accumulation of biological films (the whitish coating that forms on the tongue and teeth both above and below their gum line) can tip the scales in favor of odor-causing bacteria.
- As the biofilm matures, a transition takes place where within its depths it becomes ever more oxygen-depleted, and thus an increasingly hospitable environment for anaerobic bacteria and their continued production of volatile sulfur compounds.
(This transformation takes place as quickly as during the first few days of the biofilm’s formation.)
- As more and more coating builds up on surfaces within a person’s mouth (e.g. tooth, gum tissue, and especially the tongue), these bacteria gain more and more available living space, thus putting the person at ever-increasing risk of having bad breath.
b) The role food sources play.
Most volatile sulfur compounds are the waste products created by anaerobic bacteria as they digest proteins (or more precisely, the related compounds: proteins, peptides, and amino acids).
FYI – Most specifically, studies indicate that it’s the breakdown of sulfur-containing amino acids (the building block molecules of proteins) that result in the formation of volatile sulfur compounds.
These are primarily Methionine and Cysteine. (Other sulfur-containing amino acids don’t play a major role because they are not incorporated into proteins.)
What’s the source of these proteins?
Even without having created an obvious exposure, like just having eaten something high in protein, it’s not hard for oral anaerobic bacteria to find their preferred meal.
- Some of the compounds that make up saliva are proteins.
- With lax brushers and flossers, there’s always the leftover food debris from yesterday’s meal, and the meal before that, and the one before that …
- The debris that tends to build up on the surface of the tongue (see below) is protein-rich. Major components include shed skin cells, expired white blood cells, blood metabolites, and, of course, food debris.
▲ Section references – Porter, Aylikci
High-protein foods.
Oral bacteria eat what you’ve eaten.
Since the primary food source for the bacteria that cause bad breath is protein, you can help control their numbers by limiting your intake of foods that are rich in them. More importantly, you should make sure to clean your teeth and mouth promptly after meals that have included them.
Foods that are protein-rich.
- Meat, fish and seafood, eggs, and dairy foods (milk, cheeses, and yogurt) are all obvious examples of foods that are high in protein. Most of us get about two-thirds of our daily needs from them.
- Other sources include cereal grains (and cereal grain products), nuts, and seeds from pod-bearing plants (peas, beans, and lentils).
- Many deserts (cakes, pies, yogurt) often are surprisingly protein-rich. (Often due to egg white or nut content.)
Make sure to clean your mouth after meals.
Keep in mind, if you’ve eaten a meal that contains high-protein foods, and you fail to clean your teeth and mouth thoroughly afterward How to., you’ve created the type of prolonged food source that’s ideal for the proliferation of the kinds of bacteria that produce the smelly volatile sulfur compounds that are responsible for bad breath.
Where do the types of bacteria that cause halitosis live?
As discussed above, anaerobic bacteria do best in environments that are devoid of oxygen. And due to this fact, they’re typically found in the greatest numbers in the hidden recesses of the mouth. This includes:
- The deep grooves, micro-furrows, and crypts found on the dorsal surface (top side) of the tongue.
- Areas in between teeth, and those spaces (termed periodontal pockets, see below) that form as a result of gum recession and bone damage caused by gum disease.
- They’re also found in thick debris films, such as the coating that’s frequently found covering the back portion of a person’s tongue.
(Takeaway: You may have noticed that two of the locations in the list above involve the tongue. That’s why tongue cleaning plays such a vital role in controlling bad breath. How to do it.)
a) The dorsum of the tongue.
For the vast majority of people, most of the bacteria that produce the smelly volatile sulfur compounds responsible for their bad breath odor live on the dorsum (top surface) of their tongue.
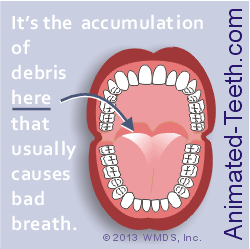
The most common cause of halitosis is debris buildup on a person’s tongue.
In fact, studies suggest that roughly 4 times as many bacteria (100 vs. 25) tend to attach to a single skin cell on the tongue as compared to other areas of the mouth.
▲ Section references – Yaegaki
Where on the tongue?
Think back to the breath testing experiments Self-testing. we outlined on the first page of this topic.
- While the smell emanating from the anterior portion of a person’s tongue can be unpleasant, it usually isn’t the primary source of their breath problems.
- The most common odor-producing region of the tongue is its posterior (back) portion.
Do this check.
Go to a mirror, stick your tongue out, and take a look. You’ll probably see some amount of coating on your tongue’s surface (see picture).
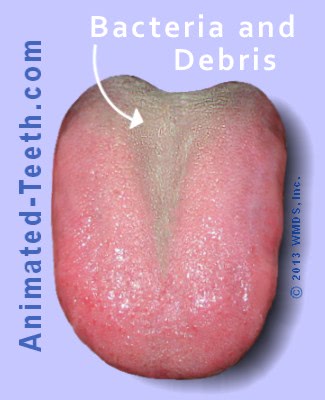
Smelly debris accumulation on the back part of the dorsum (top side) of the tongue.
For most people, this film, or more precisely the anaerobic bacteria that live in it, is the fundamental source of their breath odor.
Details.
Color.
Texture.
The further back you look (toward your throat), the heavier the layer will usually be. (Researchers sometimes use the following terms to categorize the appearance of the film: dry, slippery, dry and rough, prickly and furred.)
The level of buildup will vary.
The amount of coating that forms can be influenced by the anatomy of the person’s tongue. For example, people who have a deeply grooved or furrowed tongue may find that they accumulate more coating than those whose surface is smoother.
Other factors can play a role too. For example:
- Age – Older people tend to have more accumulation due to age-related factors such as:
1) Reduced salivary flow. 2) Decreased dexterity resulting in an inability to perform tongue cleaning. 3) Changes in the type of taste buds present (some kinds trap debris more so than others). 4) Changes in the type of bacteria present.
- Periodontal disease – People who have gum disease tend to have a thicker accumulation (and more breath problems too, see below).
▲ Section references – Danser
The amount matters.
Research has shown that there’s a direct correlation between the amount of coating on a person’s tongue and the total number of bacteria that are present (more coating = more bacteria = higher levels of smelly volatile sulfur compounds). And in fact, the tongue can be home to literally billions of individual bacterial organisms.
As you can probably guess, when the anaerobic bacterial load on a person’s tongue is reduced (like by cleaning it), there’s usually a direct correlation (an improvement) in the quality of their breath. (That’s why tongue brushing or scraping Directions. plays such an important role in curing halitosis.)
The Winkel Tongue Coating Index.
As a way of documenting their patient’s status, some dentists use the Winkel index to quantify what they find.
The Winkel Tongue Coating Grid.
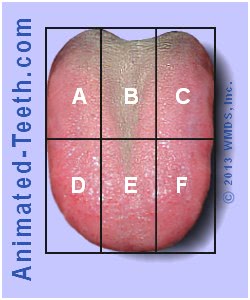
The greatest amount of coating is usually found in sections B, followed by A and C. Sections D, E, and F usually have the least.
Using the Winkel system:
- An imaginary grid consisting of 6 rectangles is mentally superimposed over the patient’s tongue (see picture).
- Each section is then rated from 0 to 2 based on the amount of coating present.
- All of the individual scores are then totaled to give an overall rating ranging from 0 (no coating) to 12 (a very heavily coated tongue).
▲ Section references – Danser
b) Bacteria that live around teeth.
The anaerobic bacteria that cause bad breath frequently find a home in places around your teeth too.
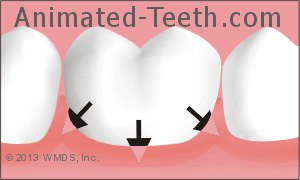
Odors can come from bacteria living below the gum line.
The evidence.
When you floss, you may notice that your floss dredges up a foul odor or taste. This odor is often most noticeable as you floss between back teeth.
These locations are places where anaerobic bacteria have found a home. The bad taste and smell you get (due to the smelly volatile sulfur compounds they have created) are proof of this fact.
The role of gum disease.
Even in relatively healthy mouths, anaerobic bacteria are able to find suitable (oxygen-deprived) places to live. These types of locations are, however, even more numerous and available in the mouths of people who have periodontal disease (gum disease).
Healthy vs. diseased gums.
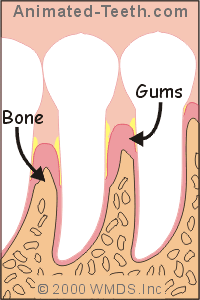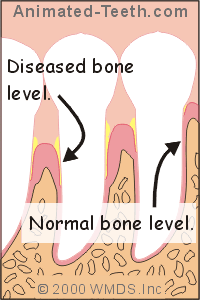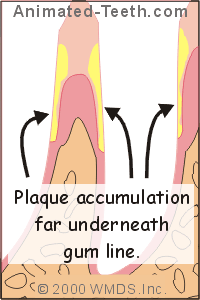
Gum disease causes deep pockets that are hard to clean.
Pocketing.
That’s because advanced gum conditions result in damage to the gum and bone tissue that surrounds a person’s teeth, the outcome of which is the formation of deep spaces termed “periodontal pockets.”
These recesses can be difficult, if not impossible, to clean. And that makes them an ideal undisturbed anaerobic environment for the types of bacteria that cause bad breath. (For more details, this link explains the halitosis / gum disease relationship. It’s role. in greater detail.)
Contributing issues & risk factors for bad breath.
As important as it is to understand the fundamental underlying cause of halitosis (anaerobic bacteria and their production of volatile sulfur compounds), there are also important bad breath co-factors (issues and conditions) that tend to tip the scales in favor of your developing halitosis or a worse case of it. They include:
- Dry Mouth (morning breath / xerostomia)
- Smoking
- Gum disease
- Sinus conditions
- Foods
- Medical and Dental conditions.
- Dentures
As you read through the explanation of each of these issues, take notice of how many of them directly relate to:
- Conditions that promote the growth of oral bacteria.
- Situations that make it more difficult to clean those areas where oral bacteria reside.
These issues are important because they’re the actual reasons why you have bad breath. The co-factors discussed below just help to set the stage for them.
Contributing factors for halitosis –
A) Dry mouth.
Morning breath.
Everyone, even including people who don’t really have much of a mouth odor problem, probably notices that their breath is least pleasant in the morning when they first wake up. (As opposed to the term “bad breath,” the words “sour” and “stale” are often used to describe what’s noticed.)
This occurs because during the night a person’s mouth tends to dry out, due to their body’s natural tendency to lower their flow of saliva as they sleep. And if you snore or sleep with your mouth open, it tends to aggravate this situation even more.
In most cases, morning breath can be expected to disappear after a person has performed their morning oral hygiene and has had a chance to rehydrate their mouth.
Similar conditions.
- This same type of drying/souring event is often noticed by teachers, lawyers, or anyone else who must speak for extended periods of time.
- People who routinely breathe through their mouth, are fasting, or else find themselves stressed (these situations tend to reduce salivary flow), may find they have a chronically dry mouth and thus persistent problems with breath malodor.
Why oral moisture is so important.
An explanation for the dry-mouth phenomenon lies in the fact that oral moisture helps to keep a person’s mouth clean.
- The presence of oral fluids encourages us to swallow. And with each swallow we take we expel bacteria from our mouth, as well as the food and debris on which they feed.
- Oral moisture dilutes and washes away the smelly waste products (volatile sulfur compounds) that oral bacteria produce.
- Saliva is the body’s natural mouth rinse. It contains compounds that kill bacteria and buffer their stinky waste products.
So, when our mouth dries out, each of these mechanisms is inhibited to some degree, with the net result being one where the conditions for bacterial growth are enhanced, while the neutralization of their odoriferous VSC waste products is diminished.
B) Xerostomia.
▲ Section references – Quirynen
Common causes.
Medicines – Xerostomia can be a side effect of taking certain types of medications.
This includes antihistamines (allergy and cold medications), antidepressants, blood pressure agents, diuretics, narcotics, or anti-anxiety medications may all be contributing factors to this condition.
Age – As a person gets older, a condition of chronic mouth dryness may become more and more of a problem.
That’s because a person’s salivary glands tend to work less effectively as they age, and the composition of the saliva they produce changes too.
Gum disease as a complicating factor.
People who have xerostomia are at greater risk for developing gum disease and the breath issues that come with it (see our next section).
A part of this risk is associated with the relatively dried-out nature of the person’s dental plaque, thus making it more difficult to remove. Also, some level of the protection that saliva provides (such as washing away and buffering oral bacteria and the VSC’s they produce) is lost too.
C) Smoking.
You’re probably familiar with the odor of people who have “smoker’s breath.” As it turns out, dealing with it is difficult because the smoking habit both causes and promotes halitosis. Here’s how:
Cigarette smoke contains VSC’s.
The odor of bad breath is caused by a class of molecules collectively referred to as volatile sulfur compounds (VSC’s). And in the case of smokers, not only does their breath contain some level of VSC’s that have been produced by oral bacteria but it also contains additional levels derived directly from their cigarette’s smoke.
That means that short of quitting smoking, there’s no cure for smoker’s breath. Although, practicing immaculate oral hygiene (and thus reducing the level of intra-oral VSC’s produced) may help to minimize it.
Ways smoking aggravates breath problems.
Smoking dries out oral tissues.
The dry-mouth conditions associated with smoking typically correlate with an increased level of biofilm formation (tongue coating and a buildup of deposits around the teeth).

Smoking aggravates breath issues.
- The film itself provides increased living space for the kinds of bacteria that cause bad breath.
- And the buildup of biofilm around teeth places the person at greater risk for developing gum disease.
Both of these factors (discussed further below) are associated with oral malodor.
Other important pages –
Smokers tend to have worse oral health status.
In cases where this is true, the person’s failure to adequately brush and floss their teeth and clean their tongue will simply result in increased levels of the types of bacteria that cause bad breath living in their mouth.
D) Periodontal (Gum) disease.
Gingivitis and periodontitis (two forms of gum disease) are frequently the underlying cause of a person’s breath odor.
Ask any dentist, the smell coming from the mouth of a person with active periodontal disease (an advanced form of gum disease) can be so distinctive that a dentist can correctly diagnose their condition even before they begin their examination.
▲ Section references – Quirynen
Who’s at greatest risk for odors associated with gum disease?
- Gingivitis (inflammation of gum tissue) routinely occurs in all age groups when proper oral home care (brushing and flossing) is not practiced.
- Periodontitis (inflammation of both gum and bone tissue) is typically more prevalent in “older” age groups (such as age 35 and beyond).
That means that statistically speaking, the older we get the more likely it is that we have a gum condition that will affect our breath quality.
- It’s also considered that breath odors associated with periodontitis (the condition more likely in older adults) are more pronounced than with gingivitis.
- There’s also some evidence that the severity of the gum disease case correlates with odor levels.
- Dentists sometimes use the BANA test How it works. as a method of diagnosing halitosis cases caused by the bacteria that cause gum disease.
How gum disease affects your breath.
- It’s both the waste products of the microorganisms that cause gingivitis and periodontitis, and the by-products associated with the inflammation that they create, that produce the volatile sulfur compounds that cause breath malodor.
Additional factors with periodontitis.
Healthy vs. diseased gums.

Periodontal disease can result in pocket formation around teeth.
- Advanced forms of periodontitis typically result in serious damage to the bone that holds teeth in place.
As it occurs, deep spaces form between the teeth and gums (termed “periodontal pockets,” see illustration), and they provide the ideal anaerobic living environment for the types of bacteria that cause bad breath.
- Research has found that the amount of odor-causing coating that’s present on the tongues of people who have periodontitis is greater than on those who don’t (as measured by weight).
Studies have also determined that the level of volatile sulfur compounds coming from this film is four times greater for people who have periodontal disease than in control groups.
▲ Section references – Suzuki, Sanz
▲ Section references – Pham
E) Sinus conditions.
Sinus conditions can cause breath odor problems.
1) Postnasal drip.
One of the symptoms of upper respiratory infections and allergies can be a postnasal drip. This discharge falls onto the back portion of a person’s tongue, by way of the opening that lies behind the soft palate.
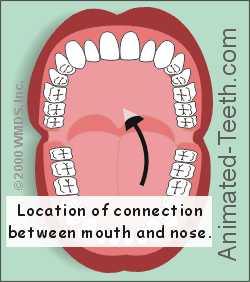
Discharge from the sinuses into the mouth can aggravate breath problems.
The discharge itself frequently has a foul taste and smell. What’s worse, the bacteria that cause bad breath can use it as a food supply, thus helping them to multiply and produce higher levels of VSC’s.
2) Dry mouth.
As an aggravating factor, people who have sinus conditions will often have a stuffed-up nose too, and therefore will tend to breathe through their mouth.
The drying effect of doing so tends to create an environment that promotes bad breath (discussed above). Additionally, sinus sufferers are likely to take antihistamines, a type of medicine that’s known to cause mouth dryness (see above).
Other upper respiratory infections.
Tonsillitis (an infection of the fleshy pieces of tissue on each side of your throat) or pharyngitis (infection of the throat itself) can be the source of breath odor. As a tip-off that this is the case, you may notice a sore throat, difficulty with swallowing, or enlargement of the lymph nodes in your neck or under your jaw.
▲ Section references – Quirynen
F) Medical conditions.
Some medical issues are known to be associated with oral malodor. If a person’s breath issues persist after they have consulted with their dentist and have tried the usual simple solutions (that almost always work), then a consultation with their medical doctor may be indicated.
Your doctor will, of course, know what types of conditions to look for. But in general, they will evaluate you for problems associated with your respiratory (pulmonary or bronchial), hepatic (liver), renal (kidney), endocrine (glands that produce hormones), and gastrointestinal (stomach and intestine) systems.
Non-oral causes.
Medical conditions and medications are categorized as “non-oral” causes of bad breath.
And while these factors may be an aggravating or even the fundamental cause of a person’s problems, in the majority of cases the origin of breath odors is the oral cavity and it should be evaluated first.
▲ Section references – Danser
G) Foods.
Everyone knows that certain foods and beverages have a reputation for causing bad breath. Some of the most notorious ones are garlic, onions, alcohol, and spicy foods in general.
How foods can cause bad breath.
- When we eat, our digestive system breaks down the food we have consumed into its component molecules. And as it happens, some of them have a very unpleasant odor.
- As these molecules are created, they are absorbed into the bloodstream so they can be distributed throughout the body as nourishment.
- As our blood travels through our lungs, some of these molecules are released into them. As a result, as we exhale, they are expelled along with our breath.
“Non-oral” bad breath.
While experiencing this type of condition can be annoying and embarrassing, it’s really just “temporary” or “transient” halitosis.
It’s classified as another type of non-oral malodor, meaning that the source of the person’s breath problems doesn’t originate in their mouth.
Solutions.
This type of bad breath will resolve on its own, typically within 48 hours or so, as your body completes the process of breaking down and utilizing, or else excreting, the smelly compounds. You can control this type of malodor simply by avoiding or minimizing your consumption of the offending types of foods.
H) Dental conditions.
- Active infections, like those associated with abscessed teeth, partially erupted wisdom teeth (Pericoronitis), or dental implants (Periimplantitis), can all lie at fault.
- Teeth that have large voids (possibly due to decay or fracture) may trap enough bacteria and debris that they become the source of foul odors.
Bacteria associated with infected teeth can be the source of breath odors.
I) Dentures.
Dentures (complete dentures, full dentures, partial dentures, etc…) can have a big influence on the quality of a person’s breath.
How to test for denture breath.
Try this test to see if your dentures might be the source of your breath odors.
- Remove your dentures and place them in a baggie.
- Seal the baggie shut and let it sit for about four or five minutes.
- Now, crack the baggie open and take a whiff.
For better or worse, that’s what your breath smells like to others. Use this link for more information about the causes of denture breath and how to remedy it.
Now that you know about the different factors that have caused your bad breath. Our next page outlines the plan that’s needed for an effective halitosis cure. 3 goals to meet.
Last reviewed: January 08, 2025
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Aylikci BU, et al. Halitosis: From diagnosis to management.
Calil CM, et al. Effects of stress hormones on the production of volatile sulfur compounds by periodontopathogenic bacteria.
Danser MM, et al. Tongue coating and tongue brushing: a literature review.
Jiun IL, et al. Association Between Oral Hygiene Status and Halitosis Among Smokers and Nonsmokers.
Kenney EB, et al. Oxidation reduction potential of developing plaque, periodontal pockets and gingival sulci.
Lourith N, et al. Oral malodour and active ingredients for treatment.
Pham TAV, et al. Clinical trial of oral malodor treatment in patients with periodontal diseases.
Porter SR, et al. Oral malodour (halitosis).
Quirynen M, et al. Characteristics of 2000 patients who visited a halitosis clinic.
Rosing CK, et al. Halitosis: An overview of epidemiology, etiology and clinical management.
Sanz, M. et al. Fundamentals of Breath Malodour.
Suzuki N, et al. Induction and inhibition of oral malodor.
Yaegaki K, et al. Examination, Classification, and Treatment of Halitosis; Clinical Perspectives.
