Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
How Dentist Treat and Manage Dry Sockets.
Guide to the professional treatment of dry sockets.
A dry socket, formally known as alveolar osteitis, is a painful complication that can occur after a tooth extraction. While there is no true “cure” for this condition, professional care typically provides substantial pain relief and promotes a more favorable healing environment.
This guide outlines the steps dentists take when treating a dry socket, including the placement of medicated dressings and, when needed, the use of pain relievers (OTC or prescription). It also explains why antibiotics are rarely necessary. Additionally, we break down the common ingredients in dry socket paste (the “brown stuff” patients see) and compare professional care to DIY remedies. (Check out this page’s Table of Contents for a complete list of its topics.)
Recognizing the benefits of professional care will hopefully encourage you to seek prompt assistance from your dentist. Doing so should provide significant pain relief and pave the way for a smoother, quicker recovery.
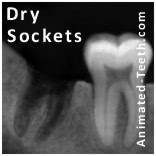
Tooth socket after extraction.
Professional treatment of dry sockets.
What your dentist accomplishes when treating your dry socket may be different than you expect.
You probably didn’t know this …
What a dentist’s care can accomplish.
The type of treatment that a dentist can offer is referred to as “palliative” care, which simply means that their efforts are directed toward the management and control of their patient’s symptoms (with pain being a primary one with dry sockets).
What they can do is implement steps that: 1) Help to keep their patient as comfortable as possible and 2) Ensure that the socket’s healing environment is as favorable as possible. This page explains how both are accomplished.
By the way, never ever be hesitant to ask for your dentist’s help.
As the provider of your care (your tooth’s extraction), it’s your dentist’s obligation to provide you with the follow-up assistance you require.
All dentists fully expect that a percentage of patients Incidence statistics. will develop dry sockets and require extra attention. So rather than delay and continue to suffer, you should contact them and take full advantage of the help they have to offer.
Can you instead treat a dry socket on your own?
Assuming that you have correctly diagnosed your condition, there are steps that you can take that can help to provide pain relief. But a self-treatment approach won’t be as comprehensive as the level of care your dentist can provide.
Home remedy solutions.
For information about the how-to’s and why-or-why-not’s of a DIY approach, use this link Self-treatment directions.
Keep in mind, however, even in emergencies where a DIY approach may be needed, it is still best used in conjunction with your dentist’s direct advice (phone contact) since they are the ones most knowledgeable about your case specifics and therefore how the information we provide applies to your situation.
This page’s highlights as a video –
Subscribe to our YouTube channel.
Dry Sockets Treatment quiz – A quick way to learn the important points from this page.
https://www.animated-teeth.com/?p=244#quiz
How do dentists treat dry sockets?
A) The initial evaluation.
As a start, your dentist will first need to establish that it’s likely that you do indeed have a dry socket.
A dry socket.
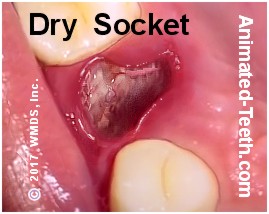
Visual inspection is a part of diagnosing a patient’s dry socket.
- They’ll quiz you about the nature of your symptoms: What are they like? Where do they seem to come from? How often do you experience them? How long do they last?
- Your dentist will also inspect your wound. (They’ll look for the situation where it appears that the socket’s blood clot has been lost and there is exposed bone tissue.)
- They’ll also want to know about the timing of the events you’ve experienced.
(In most cases, a person’s post-extraction healing will progress normally for some days before the symptoms of a dry socket See the list. begin to set in.)
B) Placement of a medicated dry socket dressing (packing).
Once your dentist determines that it’s likely that you do have a dry socket, they’ll typically then proceed with treating it using the following protocol.
The steps.
1) Cleansing the socket.
As an initial step, they’ll gently flush your extraction site with sterile water, saline solution, or chlorhexidine (a prescription antibacterial mouth rinse). They’ll then gently suction off excess fluid from the socket.
The purpose of this step is to wash away any loose debris that might inhibit the healing process or even promote the formation of a secondary bacterial infection.
2) Placing dry socket paste.
Your dentist will then smear a medicated dressing (dry socket paste) onto a piece of gauze or other type of carrier (cotton pellet, strip of iodoform gauze, dissolvable cellulose sponge).
(See below for more details about dry socket paste and carriers.)
They’ll then insert the coated carrier directly into the opening of your tooth’s socket (see animation). The insertion is performed quickly. No anesthetic is used.
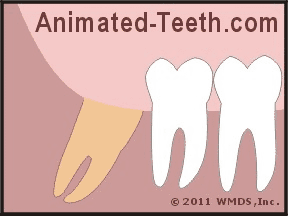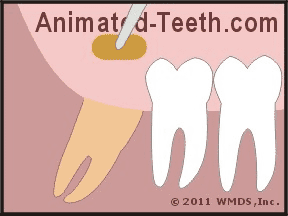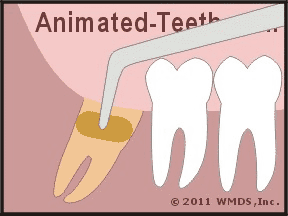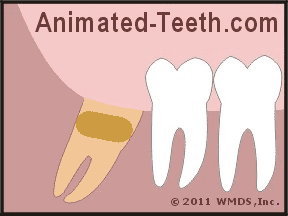
A medicated dressing is placed in the opening of the tooth’s socket.
3) Repeat dressing applications, when needed.
The medicated packing is usually renewed (removed, the socket gently rinsed, and a new dry socket paste packing placed) every 24 to 48 hours, typically for 3 to 6 days.
The exact interval that’s used will depend on your pain-relief needs, however, evaluation and retreatment should take place at least every two days. Once a day is common. Patients experiencing higher levels of pain will likely require daily treatment to remain comfortable.
4) Treatment termination.
Over time (typically 3 to 6 days), the pain caused by your dry socket should gradually subside. As it does, you’ll probably find that daily packings are no longer needed. Possibly, instead, every-other-day dressing placements may be enough to keep you comfortable.
As the level of pain continues to subside each day, a point is finally reached where OTC pain relievers (Tylenol, Advil, Motrin, Aleve, etc…) are found to be an equally effective but more convenient way to manage the dry socket’s dwindling discomfort, if something is needed at all. When this point is reached, dressing placements are terminated.
Note: Consult your healthcare professional before taking any medication to confirm that it’s safe and appropriate for your use. Use medications only as directed.
A final check of your socket.
Even when your symptoms have subsided, you’ll still need to return to your dentist’s office one last time so they can remove the last packing that was placed in your dry socket. And this is an important step to take.
An exception might be the case where a dissolvable dressing carrier has been used. You would have to confirm this fact with your dentist and follow their recommendation about what’s required.
How quickly do dry socket paste dressings work?
It’s not uncommon for a patient to experience dramatic pain relief, possibly even immediately, once dry socket paste has been placed.
Over time (usually about a day or two), the effectiveness of each medicated packing will gradually taper off. At that point, if the patient’s symptoms still persist, the dressing can then be replaced with a new one.
C) What ingredients do dry socket pastes contain?
Most dry socket pastes are composed of a mixture of compounds. Some of the ingredients typically included are:
Eugenol (extract of clove oil, an analgesic), Guaiacol or Balsam of Peru (compounds related to Eugenol), Benzocaine (an anesthetic), Iodoform (an antimicrobial agent), Chlorobutanol (an anesthetic), Butamben (an anesthetic)
The eugenol is typically the predominant or characteristic component of any dry socket paste formulation. In fact, some dentists treat cases using eugenol alone.
Commercial dry socket pastes (the brown stuff).
Most dentists tend to use commercially prepared, multi-component medicated dressings to treat cases. These products are typically thick pastes, frequently dark brown in color, that have a strong spicy-sweet odor due to their eugenol content.
What kind of carrier is the paste delivered on?
Your dentist has a number of options to choose from.
- Historically, dentists used a short strip of iodoform gauze (it has antimicrobial properties) to which paste or even just eugenol had been applied.
- A large-ish cotton pellet or a small square of gauze, either similar in size to the tooth socket’s opening, might be used.
- In some cases, a dentist will choose a dissolvable material as the carrier. Oxidized cellulose (Surgicel, which looks like gauze) or absorbable gelatin (Gelfoam/Surgifoam, which looks like a fragile piece of Styrofoam) are options.
The problem with dry socket dressings.
While we’ve already mentioned that the use of medication within the socket does not speed up the healing process, you might be surprised to learn that placing a dressing actually retards it somewhat.
- As an object, the dressing/packing is considered a “foreign body” by your body and as such interferes with the healing process.
- While beneficial in providing pain relief, eugenol is a known irritant to soft tissues and bone.
▲ Section references – Kolokythas, Bowe
These issues make this treatment a trade-off. One of creating pain relief in exchange for extending the length of the healing period, although minimally. For someone in need of this relief, this is an easy decision to make.
This phenomenon also explains why dentists don’t place dry socket dressings as a preventive measure at the time of surgery.
D) Your dentist may write you a prescription for oral pain relievers.
Beyond placing a dressing, your dentist may also write you a prescription for an analgesic (pain pills), or explain the use of a non-prescription alternative.
Analgesics are seldom effective in controlling the (possibly extreme) discomfort from a dry socket on their own.

While not a cure, pain relievers may aid in controlling dry socket discomfort.
They are typically only used as an adjunct (supplementary approach) after the placement of a medicated paste has been completed (as described above) and it’s been determined that some residual level of pain remains.
E) Taking antibiotics is not usually indicated.
Dry socket formation involves a scenario where an extraction site’s healing process has been interrupted due to the loss of its blood clot. An active bacterial infection is typically not involved. For this reason, the use of antibiotics is not usually indicated.
Legitimate considerations.
There can be reasons why a dentist might feel that their use is required. This could include cases where the patient is immune-compromised, or where the dentist finds strong evidence that systemic or secondary bacterial infection is involved.
Common practices.
Despite best-practice recommendations, it’s estimated that somewhere between 20 and 50% of dentists (a number that varies by country) continue to routinely prescribe antibiotics for their dry socket patients (Vessal).
While seemingly prescribed with the patient’s best interests at heart, the indiscriminate, purposeless usage of antibiotics instead only serves to increase the person’s risk of complications (like experiencing an allergic reaction), while offering just minimal potential for benefit.
▲ Section references – Vessal, Kolokythas
How do you know when your dry socket is “cured”?
As the healing process of your extraction site progresses Healing timeline. and new soft tissue gradually fills in your tooth’s socket and covers over its sensitive bony walls, the amount of discomfort that you notice will gradually fade away.
Since a dentist’s treatment steps are just palliative in nature, they can be discontinued at any point when the level of your symptoms has subsided enough that they’re no longer an issue.
At this point, you can expect your extraction site to continue on and finally complete its normal healing process Healing stages..
Other than a final check that there are no dressing materials still left in your socket, there’s no special follow-up care that’s needed after your symptoms have disappeared.
Remember, treatment for dry sockets is just palliative and not a true cure.
As explained previously on our pages, a dry socket involves the situation where an extraction site’s healing process has been delayed due to the loss of its blood clot.
Over time, the wound can still be expected to go ahead and heal on its own. It’s just that it will take longer and be more painful than it would have been otherwise. (Related content: How long do dry sockets last?)
Placing a packing like described on this page doesn’t speed things up. Instead, it simply helps to reduce the amount of discomfort that you experience while your (now prolonged) healing process takes place.
If you think you have a dry socket, don’t hesitate to ask for your dentist’s help.
All dentists know that there’s always a chance that after an extraction a patient will develop a dry socket. And although there are risk factors See the list. that tend to influence their rate of occurrence, actually experiencing one can usually just be chalked up to bad luck.
For this reason, once you’ve asked, you’ll probably find that your dentist is quite sympathetic to your situation and will be very accommodating in providing assistance. They fully expect that some percentage of their patients will require additional attention and understand that it’s their obligation to provide this follow-up care when it’s needed.
Study: Time from first symptoms to seeking treatment.
We couldn’t help but notice the following statistics mentioned in a study by Bowe [linked above]. This paper stated that for their group of study subjects:
- The duration that elapsed between the date of extraction and the initial onset of dry socket symptoms ranged from one to three days.
- The time that elapsed between symptom onset until presenting to their dentist for treatment was four to six days.
- By the time the patients reported for treatment, all classified their pain as severe.
These numbers make one think that patients may generally be hesitant to seek post-op assistance. However, they also suggest that those who seek attention promptly will likely save themselves a day or night of severe discomfort. So don’t be hesitant to contact your dentist if you find the nature of your socket’s healing process has changed.
Looking for more information?
If you’ve read this page, hopefully you’re onboard with seeking care from your dentist. However, in the case that you are really jammed up, we do have a page that discusses DIY dry socket remedies. Just keep in mind that professional treatment is always considered more effective, more appropriate, and that considering self-care doesn’t mean that you shouldn’t still contact your dentist.
If instead you’re looking for additional background information about alveolar osteitis in general, consider these pages: What are dry sockets? Why do they form? and Risk factors for dry sockets.
Last reviewed: April 18, 2026
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Bowe DC, et al. The management of dry socket/alveolar osteitis.
Kolokythas A, et al. Alveolar Osteitis: A Comprehensive Review of Concepts and Controversies.
Vessal G, et al. Study of antibiotic prescribing among dental practitioners in Shiraz, Islamic Republic of Iran.
Video transcription.
Hello, and welcome to Animated Teeth.com and our page that discusses the treatment of dry sockets, or, as your dentist would say, alveolar osteitis.
Actually, we have two pages on our website that discuss this subject. This one that explains how dentists treat this complication. The other discusses possibilities with self-treatment.
Without question, your better hope of finding substantial relief comes from your dentist. And as your treatment provider, they have an obligation to assist you with whatever post-operative complications you encounter. Usually, you’ll find they have a genuine eagerness in following through with their work and take pride in seeing that you’re taken care of. So, be in touch with them.
As a first step, your dentist will need to establish that it’s likely that you do indeed have a dry socket.
We have a separate page and video that discusses the usual signs and symptoms of this complication. So, here we’ll just mention that arriving at a correct diagnosis is usually pretty easy for them based on a combination of the symptoms you’ve noticed and their timing.
So, if you’ve called and spoken to them, or even just your presence at their office a few days after having had your extraction, well, they’ll have a strong, probably correct, suspicion about what your problem is.
As a bit of negative news, we’ll point out that your dentist doesn’t really have a cure to offer. A dry socket involves a situation where normal extraction site healing has been interrupted and therefore delayed. And no one can do anything about that. Your body simply needs time to regroup and get the healing process back on track.
Until that happens, you’re left experiencing the pain associated with exposed, irritated, and inflamed extraction site tissues. Fortunately, however, these symptoms are something your dentist can do something about.
Dry socket treatments are palliative in nature, meaning their focus is helping you manage the pain you’re experiencing until that point in time when your body’s healing process has resolved your condition.
This treatment usually takes a dual approach. First, it always involves placing medication inside your socket that characteristically, and amazingly, is able to provide substantial relief. As a second front, they may utilize oral pain relievers, either prescription or nonprescription, depending on your needs.
Of the two, it’s the medication, typically a paste, that your dentist places inside your dry socket that’s the most effective in making you feel better.
Exactly what’s in the concoction, typically just called “dry socket paste,” can vary depending on its source, either self-formulated by the dentist or a purchased product. But all of these kinds of pastes are usually similar in the fact that they include the ingredient eugenol.
Eugenol is also called “oil of cloves,” like the spice. And FYI, its smell is one of the main odors usually associated with dentist offices.
What the dentist does is this. They’ll first gently rinse the debris out of your socket. And, by the way, getting a good look into it like this helps them to confirm their diagnosis of alveolar osteitis.
They’ll then put some of their dry socket paste on a carrier, like a small piece of gauze or cotton, and then they’ll tuck that down into your socket using a pair of dental tweezers. And yes, doing that step might hurt for a split second.
Once finished, they’ll send you on your way. The onset of relief can be quite rapid, possibly amazingly so. The idea is you’ll stop by and they’ll remove and replace the medicated cotton every day or two until your symptoms subside.
As we said previously, this treatment doesn’t cure or speed up the dry socket’s healing. It just provides pain relief. So, it’s repeated as needed to keep you comfortable but not beyond.
As a second front, your dentist may discuss the use of oral pain relievers with you, either prescription or nonprescription. But typically, these are only used for additional pain relief, and, once again, only as needed.
Often, the placement of the paste alone is all that’s required to manage your discomfort. In contrast, the use of pain pills by themselves is frequently ineffective.
As one last point, keep in mind that a dry socket is typically a situation involving interrupted and delayed healing, without the presence of infection. So, for that reason, the use of antibiotics is not usually indicated.
Hopefully this video has convinced you that seeking your dentist’s assistance is the key to finding dry socket relief. So, go ahead and let them know that you need their help. They’d be disappointed if you didn’t. Good luck and goodbye.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
Dry socket healing progress
Hello! I had my lower right wisdom tooth extracted three weeks ago. A week later I went back to the dentist due to dry socket which he treated by an alvogyl dressing. Then another week I went back again for a follow up and the dentist renewed the dressing. The hole in the gum is not closing and I can still see the dressing inside. I rinse my mouth with warm salt water after every meal, 3-4 times a day.
I am still only eating soft food because after eating solid food I feel a slight pain near the extraction site, otherwise I don’t feel any pain. I think the gum is slightly swollen on the outer side. I am just wondering how long the gum will take to close up.
A Jady
Reply –
You need to report to your dentist so they can evaluate your situation.
The alvogyl is usually placed on a dressing, that may or may not be a material that dissolves away on its own. If not, it must be removed. If it is, and now a week later you still see some type of object in your socket, the situation should be evaluated by your dentist. The presence of alvogyl in the socket beyond the time frame it is needed will delay healing.
The hole itself will fill up from the bottom, as opposed to initially closing over at the top, so it’s expected that you’ll may see some remnant of a hole for quite some time.
Staff Dentist
