Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
Cold Sores (Fever Blisters) Identification & Stages – Pictures | Signs & Symptoms | Locations | Transmission/Contagiousness
How are cold sores identified?
Cold sores, also known as fever blisters, are distinguished from other types of mouth sores by way of evaluating:
- The appearance of the sore as it progresses through its stages of formation.
- The location in which the lesion has formed.
- Laboratory testing can be performed but is not commonly used or needed.
What our guide covers.
With the aid of pictures and diagrams, this guide outlines the distinctive appearance, signs, and symptoms of cold sores at each stage: tingle, blister, weeping, crusting, and final healing. Additionally, it highlights how the location of a lesion (such as around the mouth or on the lips) is a crucial clue in confirming it as a cold sore. (Check out this page’s Table of Contents for a complete list of its topics.)
We also explain when cold sores are most contagious and cover common methods of virus transmission—both to others or even to other parts of your own body, thus allowing you to take the precautions needed to protect yourself and those around you.
A) What do cold sores look like? (The 5 stages.)
The appearance of a cold sore (fever blister) will gradually change as it progresses through the five stages of formation we outline here. The timeline for this transformation (from the first sign of lesion formation to complete healing) usually lasts between 8 and 12 days.
FYI: The stage of your sore correlates with its level of contagiousness.
#1 – The Tingle stage (Prodrome stage) – Days 1 & 2.
In most cases, the first indication a person notices of a developing cold sore is a new sensation—such as burning, stinging, itching, soreness, tightness, or swelling—in the area where the lesion will ultimately appear.
► What to look for – The area may become reddened and slightly raised (forming a papule).
► Things to know – All of these initial signs are symptoms of inflammation. (Your body’s response to the presence of the herpes virus and the tissue damage it’s starting to cause.)
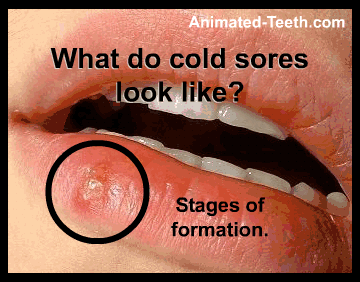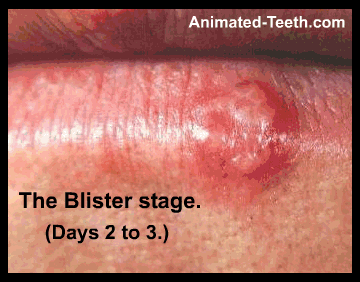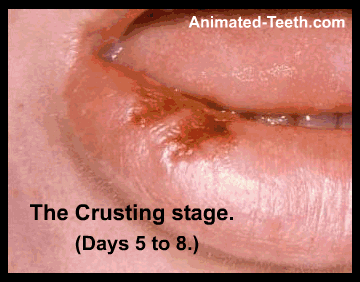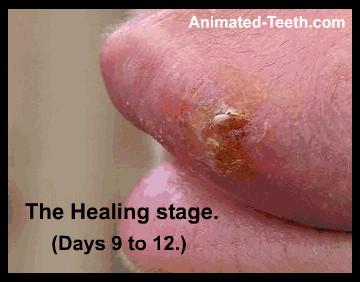
The stages of cold sore (fever blister) formation.
#2 – The Blister stage – Days 2 & 3.
► Things to know – This is the stage at which the total number of herpes virions (HSV particles) is at its highest. In general, the overall size of the developing lesion correlates with the relative number of virions present. (Hull)
▲ Section references – Hull, Opstelten
#3 – The Weeping stage (Ulcer stage) – Day 4.
The blisters that form typically rupture soon after appearing, releasing a clear fluid containing a high concentration of herpes virions. Once all of the blisters have broken, the lesion transitions into an ulceration (an open sore).
► What to look for – Immediately after the blisters rupture, the lesion appears as a shallow red ulcer (a wet, raw-looking sore), which then gradually develops a gray surface.
► Things to know – This stage of fever blister formation is typically the most painful one, as well as the most contagious one.
By this point, the lesion’s rate of viral replication has passed its peak. The inflammatory response triggered by the virus and the damaged skin cells is now fully active, working to clear the affected tissue. (It’s this inflammation response—which is a normal part of the healing process—that causes the redness, swelling, and tenderness associated with cold sores.)
#4 – The Crusting stage – Days 5 through 8.
If the ulcer has formed in a location where it’s not kept wet by moisture from the mouth, it will scab over.
► What to look for – The scab typically appears as a yellowish or dark red to brown crust. It may crack or break, which can lead to bleeding.
At times when the scab has come off, you can see the amount of ulceration that remains and the pink, newly formed tissue that surrounds it.
► Things to know – The formation of the scab is often accompanied by an itching or burning sensation. Moisturizing the scab Details can help to prevent this.
#5 – The Final Healing stage – Days 9 through 12.
As time progresses, so will the sore’s healing.
► What to look for – A series of scabs will usually form over the lesion. As each one flakes off, it is replaced by the next one.
Each new scab will be smaller than the previous one, until finally, the lesion has fully resolved, typically without residual scarring.
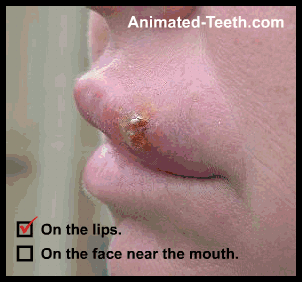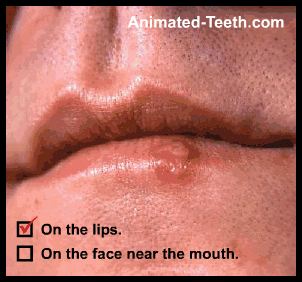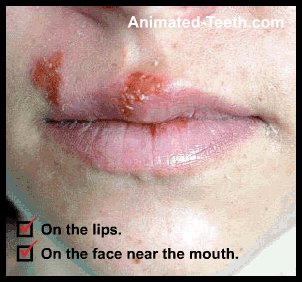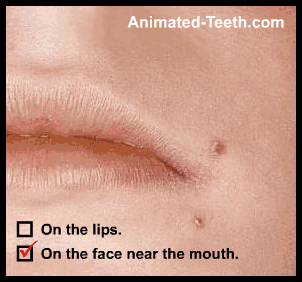
Locations where cold sores (fever blisters) form.
B) Where do cold sores form? What locations?
- On or at the edge of the lip.
- On the face, near the mouth. – Such as on the chin, lower portion of the nose, or cheeks.
This is an important characteristic that aids in the identification of recurring facial lesions as cold sores.
C) Are cold sores contagious?
Yes, during times when you have a cold sore, your potential for spreading the herpes virus should be one of your concerns.
Contact with your sore, or the fluids coming from it, or even your own infected saliva can transfer herpes virions to others, or even other parts of your own body (see below).
1) Transmission to others.
a) Direct contact.
It’s generally considered that the dominant transmission route of the herpes simplex virus involves making direct contact with the infected individual, usually via one of the following events.
- Coming into contact with the person’s herpetic lesion (direct oral skin-to-skin contact).
The transmission event could be an activity like kissing, or even just brushing your lips against someone’s sore during a hug.
As a best practice, if you have a cold sore, you should refrain from being intimate with others or participating in contact activities (e.g. wrestling, basketball, etc…). (See below for which cold sore stages tend to release the most virus particles.)
- Being exposed to another person’s infected body fluids (saliva).
While a cold sore’s level of virus replication waxes and wanes as it progresses through the stages discussed above (see additional discussion below), one must assume that any time they have a lesion that some level of virions are likely to exist in their saliva, thus making it a potential means of transmission.
- Asymptomatic viral shedding.
Asymptomatic shedding (periods when an infected person has no active lesion but their body sheds viral particles, such as into their saliva) may be responsible for transmission in a low percentage of cases. But as of yet, the exact degree to which this phenomenon actually plays a role in oral HSV transmission is not well documented.
A study that monitored healthy herpes positive (HSV 1) subjects detected asymptomatic oral shedding on 12% of days, with an average duration of 24 hours for each episode (Mertz). It’s estimated that 70% of the general population sheds HSV 1 asymptomatically at least once a month (Neville).
b) Via an intermediary.
The oral pathology textbook by Regezi states: “the spread of infection through airborne
droplets, contaminated water, or contact with inanimate objects is generally undocumented.” (Our research of this subject ran across numerous studies stemming from the 1980s and 1990s that in their day had postulated these as transmission routes.)
This same opinion seems to be supported by the other reference sources we’ve used for this page, all of which portray the dominant route of transmission of oral herpes as being either infected saliva or contact with active lesions, as opposed to intermediary objects.
c) Further considerations.
▲ Section references – Mertz, Neville, Regezi, Arduino, Ayoub
2) Transfer to other body parts.

Always wash your hands after touching a cold sore.
- Herpes simplex can cause herpetic whitlow, a painful infection of the fingers.
- A herpesvirus infection of the eye can result in corneal blindness.
(If you wear disposable contact lenses and their contamination is suspected (like by handling them after touching a sore), then throw them away. To avoid this issue, you may choose to wear your glasses when you have a cold sore.)
- Being intimate with others can cause infection of your partner’s genitals.
3) Other best practices for preventing viral spread.
- Don’t touch or pick at cold sores. Only touch them when treating them.
- Dab medication on a lesion rather than rubbing it in, so not to disturb the sore.
- Wash your hands (soap and water) after treating a lesion. And washing them repeatedly throughout the day makes a good practice too.
When are cold sores the most contagious?
Virus particles are present during all stages of cold sore formation. And for that reason, each and every stage should be considered to be contagious.
a) Wet lesions are the worst.
The most contagious stage of a cold sore is when its blisters rupture (the Weeping stage). This is because the liquid contained in these blisters holds literally millions of herpes simplex virions.
b) Scabbed lesions, less so.
As a cold sore continues to run its course, the number of virus particles present in it diminishes. Usually, by the time a scab has formed (the Crusting stage) the number of virus particles has lessened dramatically.
Concerns with at-risk persons.
Some people are at greater risk for herpetic infections and associated complications than others. And for this reason, they should be given special consideration.
This includes people with immature immune systems (newborn babies) or compromised ones (such as chemotherapy or HIV patients).
All of the basic precautions used to prevent the spread of the herpes virus need to be vigilantly practiced when these types of individuals are involved. Parents/caretakers need to establish rules about what type of contact is allowed with those in their charge.
Statistics involving newborns.
Herpes infections involving newborn children can be a serious matter, with possibly multiple organ systems being affected, and even risk of the infection causing death.
In the vast majority of cases (90%), the virus is passed to the child from their mother during delivery (whether or not she currently has any signs or symptoms of infection). Fortunately, a newborn’s risk of experiencing a herpetic infection is a low-percentage event (involving far less than 1% of newborns), and usually a manageable condition when treated (however 60% of untreated cases result in death).
▲ Section references – Rettner
Looking for more information?
Certain treatments can aid with cold sore prevention or management: Prescription Medications | OTC & Home Remedy Solutions
Once you’ve had a cold sore, you’ll probably have others in the future. This page discusses Triggers for Cold Sore Breakouts.
Or, use this link to view all of our Cold Sore (Fever Blister) Guides.
Last reviewed: April 25, 2026
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Arduino PG, et al. Herpes Simplex Virus Type 1 infection: Overview on relevant clinico-pathological features.
Ayoub HH, et al. Characterizing the transitioning epidemiology of herpes simplex virus type 1 in the USA: model-based predictions.
Hull CM, et al. Novel Composite Efficacy Measure To Demonstrate the Rationale and Efficacy of Combination Antiviral–Anti-Inflammatory Treatment for Recurrent Herpes Simplex Labialis.
Rettner R. Deadly Kiss: Can a Baby Contract a Lethal Virus from a Cold Sore?
Mertz G. Asymptomatic Shedding of Herpes Simplex Virus 1 and 2: Implications for Prevention of Transmission.
Neville BW, et al. Oral and Maxillofacial Pathology. Chapter: Viral Infections.
Opstelten W, et al. Treatment and prevention of herpes labialis.
Regezi JA, et al. Oral Pathology: Clinical Pathologic Correlations. Chapter: Vesiculobullous Diseases.
