How to Identify Canker Sores and their Stages.
Canker sore (aphthous ulcer) identification / stages / pictures.
Canker sores, also known as aphthous ulcers, are a common type of mouth sore. This page provides a comprehensive guide to identifying these oral lesions.
What we cover.
With the help of pictures and diagrams, this guide explores the signs, symptoms, and typical locations of canker sores. You’ll learn how their appearance and symptoms evolve through their stages of formation and healing. Additionally, we cover lesion frequency, the number of lesions per outbreak, risk factors, and what to expect during the healing process. (Check out this page’s Table of Contents for a complete list of its topics.)
Whether you’re managing a current outbreak or looking for prevention tips, this guide is designed to help you confidently identify canker sores and understand what to expect.
How dentists diagnose canker sore lesions.
Dentists distinguish canker sores (specifically, “recurrent minor aphthous ulcers,” the common type of canker ulceration that affects 80% of sufferers) from other types of mouth sores based on these three points.
The three pillars of canker sore identification –
- Their appearance (which changes during their successive stages of formation and then healing).
- Their location and the type of oral tissue on which they’ve formed.
- The fact that they are recurrent (meaning the person has experienced them before).
Additionally, the persons’s patient history—specifically what they did or did not experience with their sores—plays a valuable role in identification and helps differentiate aphthous lesions from other types of mouth sores.
Related page: Canker sores vs. Oral herpes lesions—How to tell them apart.
Methods that aren’t routinely used for aphthous ulcer identification.
As a side note, we’ll point out that the factors mentioned above, collectively, are usually all that’s needed to make an accurate diagnosis for canker sores.
- No medical testing (e.g. biopsy, culturing) is typically involved in making a diagnosis.
- When viewed microscopically, the histologic characteristics of canker sores are non-specific, making this method of evaluation of little diagnostic value.
(Visit this page if you’d like information about The biology of canker sore formation. )
This page’s highlights as a video –
Subscribe to our YouTube channel.
Canker Sore Identification quiz – A quick way to learn the important points from this page.
https://www.animated-teeth.com/?p=172#quiz
What do canker sores look like?
A canker sore’s appearance changes as it moves through its distinct stages of development and then healing.
Canker sore stages –
Use these links for details about each specifc phase.
And as additional resources, this page features two Q&A sections that answer questions that people frequently have about identifying canker sores and understanding their stages
The stages of canker sore formation and healing.
Note: The time frames we’ve assigned to each of the stages overlap because what any one person will experience will vary.
#1 – The Prodromal Stage.
(Also referred to as the Premonitory Stage.)
Time frame: 2 to 48 hours duration.
This stage is the earliest indication of pending canker sore formation but it doesn’t involve any visible signs. Instead, what’s noticed is a tingling, itching, burning, or numb sensation in the area where the ulceration will ultimately form.
These kinds of signs are referred to as “prodromal” symptoms, meaning that they hint that something is brewing but the signs themselves are not specific to just canker sores. Other types of mouth ulcers might start out with these same general symptoms.
# 2 – The Macule Stage.
(Also referred to as the Preulcerative Stage.)
Time frame: 18 to 72 hours duration.
During this time frame, the first visible signs of the developing lesion will start to show.
- The area where your mouth ulcer will ultimately form begins to transform into a reddened circular area on the skin. (Formally referred to as an “erythematous macule.”)
- As the lesion’s development progresses, it’s possible that the macule may transform into a small, possibly whitish, papule (solid, slightly raised area).
- Toward the end of the macule stage, the tissue of the affected area will begin to ulcerate.
(This process of ulceration begins in the skin’s basal (lowest) layer and then becomes more apparent as it advances up into the more superficial layers above.)
Slideshow – Stages of a Canker Sore pictures.
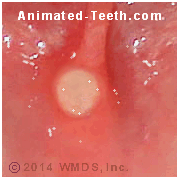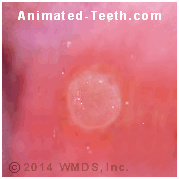
Pictures of fully formed aphthous ulcers.
#3 – The Ulcer Stage.
By this stage in its development, the lesion has transformed into a fully-formed ulceration. (View our Stages of a Canker Sore slideshow for pictures). It may continue to grow in size for 4 to 6 days.
What does a canker sore ulceration look like?
- This lesion’s most basic form appears as a single, shallow mouth ulcer that has a symmetrical round or oval shape. (Note: Having multiple simultaneous lesions is possible.)
- Canker sores are typically no more than 1/4 inch in diameter (3 to 5 mm).
Diagram: The physical characteristics of a canker sore.
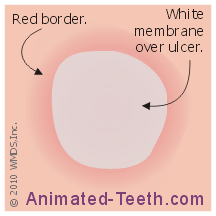
Sores have a grayish membrane-coated central ulceration with a surrounding red border. The skin around the lesion looks normal.
- The lesion’s center (the ulceration) develops a loosely attached membrane-like covering (a pseudomembrane) that can be easily dislodged.
(The membrane is pyogenic in nature, meaning it’s composed of cells, compounds, and debris originating from the inflammatory process that has caused the ulceration.)
- Initially, the membrane has a primarily yellow-white coloration. As healing ultimately progresses, it will tend to take on more of a grey-white tint.
- A border comprising a band of erythematous (reddish) tissue will surround the ulceration.
The outline of this red halo is characteristically circumscribed (well defined) and regular (not jagged).
- The skin that lies outside the lesion’s reddened border will appear normal and healthy.
Other characteristic signs and symptoms.
- Canker sores usually are painful. The level of discomfort that’s experienced may seem out of proportion with the lesion’s size.
Sufferers will frequently limit their oral movements, the types of foods they eat, and favor the sore’s surface as not to trigger pain.
- There are no distinguishing systemic features associated with minor aphthous ulcers, such as the person having malaise (generally feeling poorly) or fever.
▲ Section references – Neville, Akintoye, Chavan, Casiglia, Scully, Dunlap
Can a person have more than one lesion at a time?
Yes, outbreaks of multiple, simultaneous canker sores may occur.
- Usually, the maximum number of sores that will form at one time will be six or fewer.
- If multiple canker sores do develop, they’re more likely to be distributed as opposed to being clustered together.
- In the case where two sores do form adjacent to each other, they may combine into a single larger and irregularly shaped mouth ulcer (as opposed to the classic round or oval lesion).
▲ Section references – Neville
Are they contagious?
- No, canker sores are neither contagious nor infectious.
For more details, see this page Why canker sores are not contagious.
Where do canker sores form?
An important factor in canker sore identification is that they only form in specific areas of the mouth. (Note: For this section, we are specifically referring to “recurrent minor aphthous ulcers,” the most common type of canker sore.)
- They characteristically form on “loose” oral tissues—meaning areas in the mouth where the skin is not tightly bound to the underlying bone.
- The tissue in these locations is characteristically nonkeratinized, meaning it is a thinner, more delicate type of oral lining.
What locations are involved?
Here is where you can expect canker sores to form.
Diagram: Locations where canker sores usually form.
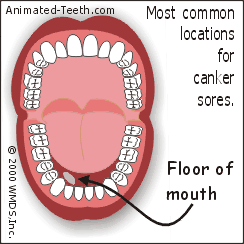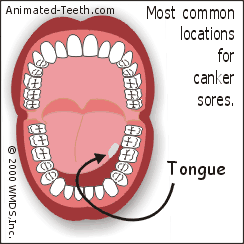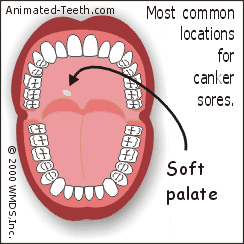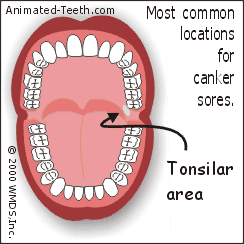
Canker ulcerations characteristically form on the “loose” tissues of the mouth.
- The inside surface of the lips and cheeks.
- The underside (ventral surface) of the tongue.
- The mucobuccal fold (the deep trough where the skin of the jawbones and lips/cheeks meet).
- The floor of the mouth.
- The soft palate.
- The tonsillar areas.
(Listed in order of locations/tissues most frequently affected.)
Less common locations.
While rare, it is possible for canker sores to form on keratinized tissues. This includes the top (dorsal) surface of the tongue, the gum tissue that surrounds a person’s teeth, hard palate, or even the border of the lips (vermilion border).
▲ Section references – Neville, Dunlap
Additional Q & A about the formation stages.
Beyond the questions we’ve addressed above, here are some additional ones that people often have.
Can you pop a canker sore?
No, aphthous ulcers form from a macule (reddened area of skin), not a blister. There is never any blister to pop.
Why are canker sores so painful?
These lesions are ulcerations. The protective layer of skin that originally covered over the area of the sore has fully deteriorated thus leaving the inner layer of tissue and the nerve endings it contains exposed.
FYI: Some treatments for canker sores work by forming a protective film over the ulceration.
Do canker sores get bigger before they go away?
With “recurrent minor aphthous ulcers” (the most common type of canker ulceration), once a lesion has fully formed (usually by day 4 to 6), it’s not expected to grow in size. However, during formation, it is possible for two directly adjacent lesions to coalesce into one larger one.
Is it normal for canker sores to be yellow?
Yes. Especially during the early stages of ulcer formation, a yellow membrane can usually be seen covering its surface. Later on, this yellow coloration will typically transform to a grey-white tint.
How often do canker sores form?
Outbreak frequency.
- Once a person has experienced an initial outbreak, the probability of recurrence is high, although the frequency with which this takes place can be quite variable.
- A rate of one outbreak every 1 to 3 months might be considered typical (encompassing about 50% of people who get them). 30% of sufferers deal with their presence on a monthly basis.
That means many people will only be plagued by a few episodes a year, while others will experience nearly continuous outbreaks and therefore will never be completely free of these mouth ulcers for any extended period of time.
Incidence rates / Prevalence.
- Most sources tend to suggest that around 20% of the general population experiences canker sores, although actual reports from studies have ranged from 5% to 66%.
- A person’s first outbreak will typically take place between the ages of 10 and 20 (teen years through young adult), and then decrease in frequency and severity with age.
Lesions are most prevalent in people ages 10 to 40. 80% of those affected will experience their first lesion prior to the age of 30.
- It’s been suggested that women are more likely to experience these mouth sores than men but not all studies confirm this fact.
- A family (genetic Details) predisposition seems to exist. Children with parents who get canker sores have a 90% chance of getting them too, as compared to a 20% chance for those whose parents don’t.
- A person’s risk seems to be unrelated to race. But people who live in North America are more likely to suffer from them, as opposed to people who live in other worldwide geographic areas.
- Non-smokers and people in upper socioeconomic groups are more likely to experience outbreaks.
▲ Section references – Akintoye, Woo, Ship, Ship, Chavan, Neville
#4 – Canker sore healing stages.
Time frame: 4 to 14 days duration.
The Healing stage time frame.
Canker sores (specifically, recurrent minor aphthous ulcers) characteristically heal within just a few to several days. This characteristic can be useful in helping to confirm the kind of mouth ulceration a person has.
How long should it take for a canker sore to heal?
- A sore will usually heal within 4 to 14 days, although some can heal in as little as 3 to 5.
- The pain associated with a lesion will usually begin to subside around day 3 or 4.
- In most cases, the healing process reaches completion uneventfully and results in no residual scarring.
When should I be concerned about a canker sore?
Any ulcer that has not healed within a 2-week time frame should be evaluated by a dentist. This is for two reasons.
- One is for proper lesion differentiation. (Is the mouth ulceration you have really a canker sore?)
- The other is because there is another larger, more problematic form of aphthous ulcer that characteristically does have an extended healing time frame and its needed management is different than with routine canker sores.
Canker sore appearance during its healing stages.
- The process of new skin growth (epithelialization) will start off at the edges of the ulcerated area and then, as days pass, advance from all directions until finally the wound’s entire surface has been covered.
- As this epithelialization process takes place, the original yellow-white color of the sore will take on a grey-white appearance.
- As the newly formed tissues mature (the surrounding edges of the wound will be at a more advanced state than its center), the skin will begin to take on a more normal pink coloration and the size of the lesion will continually shrink down.
- The reddened border of the original wound will remain obvious during the early stages of the healing process. As the wound’s new skin tissue matures, the border’s redness will gradually fade. Once complete healing has finally occurred, the skin’s normal coloration and appearance will return.
▲ Section references – Woo, Casiglia, Scully
How can you tell that your canker sore is healing properly?
As long as the changes you notice with your lesion’s healing progress stay within the time frame and appearance parameters just discussed, you can assume that all is going well.
Reasons for concern.
Any events that vary from what’s described above should trigger some concern and is a reason to consult with your dentist.
- Top on the list of issues that should be investigated is if the mouth ulcer you have is indeed a canker sore (“recurrent minor aphthous ulcer”), as opposed to a lesion due to a different cause.
- If your ulceration is determined to be an aphthous one, your dentist should then determine if instead of a “minor” lesion it is a “major” one. And therefore a type of sore that needs an extended time frame and possibly more aggressive management to resolve.
Additional Q & A about the healing stages.
Beyond the questions we’ve addressed above, here are some additional ones that people often have.
Do canker sores hurt more when healing?
No, once the full extent of the ulceration has formed, your sore’s healing will begin and the level of pain associated with it should start to improve.
The new reparative tissues will first start to form around the edges of the lesion and then continue to close in over its entire surface as days pass. As the size of the raw, uncovered portion of the ulceration continues to diminish, the level of pain associated with the lesion should diminish.
How long does the pain of a canker sore last?
Hopefully, the level of discomfort you notice will start to subside by days 3 to 4. Although, complete resolution of pain won’t occur until that point when the healing process has advanced enough that the exposed tissues of the lesion are finally covered over and protected.
What color do canker sores turn when healing?
It’s normal for the original yellow-white color of the ulceration to transform to a grey-white tint. This is a sign of primordial skin tissue formation.
How do you know when a canker sore is healing?
As the process of forming new skin over the lesion progresses (epithelialization), its surface will start to take on a grey-white tint.
Since the edges of the ulceration will mature sooner than its center, this area will be the first to return to a more normal pink coloration. As new skin forms over more and more of the sore’s surface, the amount of pain the lesion causes will diminish.
How many days does it take for a canker sore to go away?
This will depend on the initial size of the ulceration and ultimately how involved its healing process will be.
With small sores, it’s possible that resolution may occur as quickly as just several days (3 to 5). But with relatively larger lesions, expect that it may take as long as two weeks.
What happens if a canker sore goes untreated?
In the vast majority of cases, no treatment is required for a canker sore and its healing will occur uneventfully and without scarring.
FYI: Most over-the-counter treatments for aphthous ulcers are only palliative in nature. (Only aimed at reducing pain levels and maintaining a healthy wound as opposed to speeding up healing.)
“Major” aphthous ulcers.
Canker sores like we have described above are formally termed “recurrent minor aphthous ulcers.” They are the type of canker lesion experienced by 80% of sufferers.
Beyond these “minor” lesions, there’s another type of aphthous ulcer referred to as “major aphthae” or Sutton’s ulcers. And in comparison to the minor variety, these “major” canker sores are large, deep ulcerations whose healing is characteristically slower and more painful.
Characteristics.
- Unlike minor aphthae, the major kind forms on all types of oral tissues (both keratinized and nonkeratinized tissues). They frequently form on the lips, soft palate, or fauces of the throat.
- They can approach 1/2 inch (or more) in diameter and may cause regional or even facial swelling.
- Their healing usually takes between 10 and 40 days. However, it may take some months (even as new ulcers are forming).
- Residual scarring is common.
▲ Section references – Chavan, Neville
Looking for more information?
If you’re still not clear about what kind of mouth sore you have, you may find this page helpful or reassuring: Canker vs. Herpes sores – How to tell them apart.
Since canker sores are recurrent by nature, consider this page—Triggers for Canker Sore Outbreaks—which offers insights that may help you minimize future episodes.
If you need help managing a current outbreak, select from our other Canker Sore Guides, which cover home remedies, OTC products, and prescription treatments.
Last reviewed: April 26, 2026
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Akintoye SO, et al. Recurrent aphthous stomatitis.
Casiglia J. Recurrent aphthous stomatitis: Etiology, diagnosis, and treatment.
Chavan M, et al. Recurrent aphthous stomatitis: a review.
Dunlap CL, et al. A guide to common oral lesions.
Neville BW, et al. Oral and Maxillofacial Pathology. Chapter: Allergies and Immunologic Diseases.
Scully C, et al. Oral medicine — Update for the dental practitioner Aphthous and other common ulcers.
Ship J, et al. Recurrent Aphthous Stomatitis.
Ship II. Epidemiologic aspects of recurrent aphthous ulcerations.
Woo S, et al. Recurrent Aphthous Ulcers: A Review of Diagnosis and Treatment.
Video transcription.
Hello. Welcome to Animated Teeth.com and our page that explains how to identify canker sores through their different stages of formation.
In this video, we’ll share pictures, graphics, and checklists taken from our website that make it easy to figure out if what you’re experiencing may be a recurrent minor aphthous ulcer. Which by the way, is the formal term your dentist uses for routine canker sores.
When it comes to identification, there are three primary issues to pay attention to. One is the lesion’s overall appearance, which of course, will vary as it passes through its different stages.
Another, and really unique diagnostic feature, is the sore’s location. Recurrent minor aphthous ulcers characteristically only form on a certain type of oral tissue that’s only found in specific parts of the mouth. And the third factor is that most people will find their situation familiar. Meaning they remember having this kind of lesion before.
We’ll start off by covering the issue of lesion location. Canker sores, the recurrent minor form, which is the most common type, only form on tissue referred to as loose mucosa.
To understand what kind of tissue this is, put your finger between your lower lip and teeth and then slide it on down as far as it will go. Down here, in the deepest part of the trough that lies between your cheek and jawbone, you’re touching unattached, or loose, oral mucosa. The word mucosa as used here means skin tissue that lines the inside of your mouth.
If you look in a mirror, you’ll find that this same kind of loose tissue lines the entire inside of your lips and cheeks. And on the jawbone side, you’ll probably find that it only runs about halfway up. Then, closer to and surrounding your teeth, you’ll normally find that the loose tissue transforms into a very dense and tightly bound type of gum tissue, which, correspondingly, dentists refer to as attached mucosa.
Loose mucosal surfaces are only found in certain locations in the mouth. This includes the inside of your lips and cheeks, the floor of your mouth, the underside of your tongue, your soft palate, and the area of your tonsils. So, if the sore you’ve noticed is developing somewhere else, it probably isn’t a routine canker ulceration.
Besides being some other type of mouth sore, it could be possible that what you have is a more aggressive form of aphthous ulceration that sometimes does form in additional locations, like along the side of the tongue. But in regard to distinguishing recurrent minor aphthous ulcers, the common, routine form of canker sore, forming on loose mucosal surfaces is the diagnostic rule.
As far as appearance goes, when you first feel the tingle of a canker sore starting to come on, you may not be able to see much of anything. At most, you might discover an area of slightly raised reddened skin where your sensations are coming from. So, during the early stages of development, like the first 3 days or so, aphthous ulcer identification still leans heavily on the location factor.
With time, more fully developed canker sores do take on a very characteristic appearance. These two pictures show examples.
What you’re looking at is a shallow sunken ulceration in the surface layer of the skin that has developed a grey-white pseudomembrane. That means a non-attached covering that just lies on the sore’s surface and is easily dislodged. It’s made up of leftover debris from the inflammatory process that created the ulceration.
Surrounding the lesion, you’ll see a reddened border that’s an indication of the inflammation process going on inside the area it encompasses. Outside that ring, the adjacent tissues will look pink and normal.
Additional identifying characteristics include a small size, only a quarter of an inch across or so. Usually, just one sore will form at a time, although an outbreak of a few simultaneously is not uncommon.
And, yes, canker sores are painful when touched or bumped. So, expect that and be careful with your lip movements and activities, like eating. Usually after 3 or 4 days, the level of pain they cause diminishes significantly.
Also, routine canker sores are just a local phenomenon. The person does not experience systemic symptoms like malaise or fever. Usually the sore has healed uneventfully and without scarring within a week or two.
The third pillar of canker sore identification is that the lesion you see is similar to what you’ve experienced before.
Of course, anyone person will have to experience an initial breakout. But after that, you can expect sores to recur sometime in the future. This might be on the order of a few times a year but, of course, everyone’s mileage will vary.
We have an associated page that discusses triggers and factors that tend to correlate with canker sore outbreaks and their frequency, like certain foods, stress, product ingredients, genetic factors, etc…, so look for it.
Also, we have several pages that cover the issue of canker sore management, including prescription, over-the-counter, and home remedy solutions. So, look for them too. And, of course, we must mention that this page contains additional information not included in this video, so give it a read.
As one last point, we’ll mention that your dentist usually bases their diagnosis for routine canker sores on the exact same factors that we’ve discussed in this video. They don’t biopsy or medically test, they just make observations and ask you questions. So, making an accurate determination is usually just that simple and easy. And now you know how to do that yourself. Goodbye.
