Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
Broken teeth – What usually happens. Emergency treatments. How a repair can be made.
Broken teeth – Managing emergencies. Making repairs.
If you have a tooth break, certain questions will rush through your mind. You’ll wonder how badly your tooth has been damaged and if it can be repaired. You’ll be concerned about how soon your tooth will start to hurt and what your next steps should be.
That’s what we cover in this guide. We explore:
► Different ways teeth tend to break. – Did your tooth just chip a little? Or worse, did it crack, lose a filling, have a piece break off, or fracture off at the gum line?
For each of these situations, we explain how to figure out what has happened and what it could mean for your tooth.
► How different types of tooth fractures are dealt with as an emergency. – We cover this subject from two angles: a) How dentists manage a patient’s tooth pain, sharp edges, loose or missing pieces, as well as hot, cold and air sensitivity. b) First aid steps and remedies that you may be able to take on your own at home.
► Ways dentists repair broken teeth. – This aspect of this guide explores questions such as: What kind of restoration will be needed? Has the damage been too great? Which teeth can be saved?
Usually, most teeth can be repaired by placing a filling or dental crown. However, some fractures may be so severe that root canal treatment or gum surgery is required first. In extreme cases, the level of damage that’s occurred may be so extensive that a repair isn’t possible and the tooth must be extracted. Our guide explains.
FYI: The damage your tooth has experienced may have been influenced by your daily habits. This page outlines: Proactive steps you can take to minimize your risk for tooth damage. Jump
So, what’s happened to your tooth? Which scenario fits your situation?
Ways that teeth tend to break.
We’ve divided our coverage of this topic into two broad sections.
- Section 1 – The damage to your tooth is physically obvious. Examples: You can see or feel that a portion of your tooth is missing. Part of your tooth is loose but it remains attached to your gums.
- Section 2 – Your tooth has cracked but seemingly remains intact. Examples: You can visualize a crack in your tooth. You experience cracked-tooth symptoms (explained below).
Timely attention is needed.
Any tooth that shows signs that it has fractured needs to be inspected by your dentist. And in some cases, doing so promptly may play an important role in how simple or successful its repair will ultimately be.
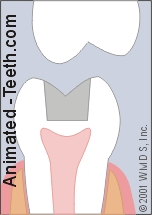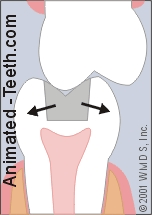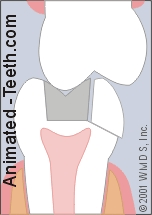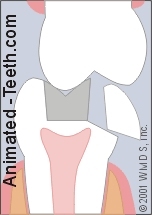
A tooth fracture where a piece has separated off.
- It could be that the event has substantially weakened the tooth. If so, not tending to it in a timely fashion may result in it fracturing further, potentially catastrophically.
As examples:
1) It may be that what’s left of the tooth is now significantly weaker than before. For example, the remaining cusps may not be able to withstand as much pressure and will fracture if stressed.
2) If a part of your tooth has broken off from around a filling, the restoration may no longer be anchored or supported adequately. And if pressure is applied to it, it may dislodge, possibly resulting in further tooth fracture.
- Hard foods might wedge in the missing piece’s void, thus splitting the tooth further.
- Since the tooth now has a part missing, dental plaque and debris that accumulates in this void may be difficult to clean away. As a result, tooth decay may form over the coming weeks and months and compromise the integrity of the tooth further.
What should you do?
The level of urgency involved will vary with each person’s case (ranging from substantial to just very little concern). Clearly, the best plan of action always involves contacting your dentist’s office and letting them determine the seriousness of your situation.
Certainly, if you’re experiencing symptoms, you’ll be more inclined to act promptly. But even if you’re not, you still shouldn’t delay in making contact with your dentist’s office.
Avoiding the use of your tooth until it can be repaired, or at least temporized, always makes a good plan. But since uncontrollable traumatic events are always possible (like while eating or sleeping), it can’t be relied upon to provide a solution.
1) Your tooth has fractured, a portion has come off or is loose.
Some traumatic events result in outright tooth fracture, meaning that a piece has physically separated from the remainder of the tooth. The fragment that has come loose may have:
- Broken off cleanly, resulting in a void in the tooth’s shape. (The missing part might be a part of the tooth, a piece or even all of a previously existing filling, or just a tiny chip of tooth enamel.)
- Although broken, the fractured piece may have remained tethered in place due to the fact that it is still attached to surrounding gum tissue. (The piece is loose but still remains pretty much in place.)
▲ Section references – Stefanac
Reasons why a broken tooth might, or might not, hurt.
The level of discomfort associated with a tooth that has had a piece break off will vary depending on the specifics of the situation. Here are some possible scenarios:
a) Situations where the tooth may not be painful at all.
Not all teeth that break end up hurting. Here are some explanations why:
- The fracture may just involve tooth enamel. – If a chip is relatively small or shallow, it may be confined to just the tooth’s enamel covering. This layer, which is around 98% mineral in content, has little association with the tooth’s nerve. Because of this, feeling pain, or sensitivity to hot, cold or air, would be relatively unexpected.
Chips like this are common in areas where tooth wear has resulted in the formation of a thin, brittle enamel edge. For example, minor chipping frequently takes place on the biting edges of front teeth (incisors, canines).
With back teeth (premolars and molars), since everything feels bigger to your tongue, if it discovers something that only feels like a small chip or area of roughness, it’s quite possible that its extent is just confined to the tooth’s enamel.
- The involved portion of the tooth is relatively distant from its nerve. – The closer the deepest aspect of a void created by the loss of a piece of tooth is to its nerve, the more likely it is that the tooth will experience some level of sensitivity. Responses to hot, cold or air (explained below) would be commonplace in this type of scenario.
Don’t be too surprised if the size of the void doesn’t seem to correlate with the level (lack) of discomfort you feel. It’s common that the nerve space inside a tooth will shrink in size, either due to age or in response to an event (such as advancing tooth decay or having had a filling placed).
If that’s the case, the base of a seemingly deep void may in actuality still be relatively distant from the tooth’s nerve. This situation is common with back teeth (molars, premolars) that have a long history of having a large filling in place but could also apply to any tooth with this type of history.
- The tooth may not contain live nerve tissue. – In some cases, the lack of sensation, even after the loss of a massive amount of tooth structure, might be due to the fact that the nerve inside the tooth at some point has already died. (A clue suggesting this would be if the tooth has a previous history of displaying any of the common characteristics associated with a tooth needing root canal treatment Signs / Symptoms.)
In other cases, the tooth may have already had root canal treatment completed. If so, any hot, cold, or air stimuli that reach the tooth wouldn’t be expected to trigger a response.
b) Situations where the tooth may be painful.
► Some broken teeth may be spontaneously painful.
A tooth that now hurts on its own without any provocation suggests that its pulp tissue (“nerve”) has been substantially insulted or traumatized by the event that has caused its fracture. And generally, this type of symptom doesn’t bode well for the tooth’s outlook.
- The nerve’s condition is referred to as pulpitis (meaning inflammation of the tooth’s pulp tissue). Spontaneous pain is considered a sign of irreversible pulpitis, meaning the tooth’s nerve won’t just settle down and return to a normal healthy state (which is what happens with reversible pulpitis).
It will take evaluation and diagnosis by your dentist to confirm this status. But when irreversible pulpitis is diagnosed, root canal treatment will be required before the broken tooth can be rebuilt.
With fractured teeth, a cause for the pulpal insult could include that a crack has formed that extends to the tooth’s nerve, thus providing a conduit for bacteria into this space.
- Some teeth that display spontaneous pain may ultimately seem to settle down. The explanation would be that the irreversible aspect of the tooth’s condition has progressed to the point where its nerve tissue has finally died.
These teeth too will require root canal treatment before they can be rebuilt. As above, it will take your dentist’s evaluation to discover that this scenario has occurred.
What should you do?
▲ Section references – Torabinejad
► Some broken teeth may be painful to biting pressure.
Experiencing this symptom may be associated with more than one scenario.
- It may suggest that beyond just being fractured (having had a piece break off) the tooth itself is cracked too.
With this scenario, when pressure is applied the cracked portions shift, thus causing pain.
- Another explanation could be that the tooth has fractured but the loose part is still attached to gum tissue and therefore hasn’t fallen off yet.
In this case, when pressure is applied, the position of the attached fragment shifts and triggers gum-tissue pain. Even after the pressure is released, the soft tissue pain may linger a bit.
In some cases, it may take biting from just the right angle to get enough pressure on the broken but still attached piece to elicit the pain. Or, sometimes it is pressure from the person’s curious tongue that causes fragment movement and pain.
(Mamoun)
- While statistically less likely, the tooth may have just happened to break coincident with having developing symptoms that signal the need for root canal treatment. If so, the pain may be a sign of that underlying condition.
▲ Section references – Mamoun, Torabinejad
► The tooth may have sensitivity to hot or cold stimuli or air.
Some fractured teeth will only hurt, or will hurt more so, when exposed to hot and cold temperature extremes like those noticed when consuming foods and beverages. Or are sensitive when air is drawn into the mouth.
And like discussed above, it’s easy enough to imagine how a tooth that has broken and now has a void that exposes its inner aspects might display signs of temporary sensitivity to stimuli.
- The situation where your tooth is irritated by thermal insult or air but then when the stimulus is removed it immediately settles back down typically suggests that its nerve is still healthy, and once a repair is made the tooth will likely be fine (reversible pulpitis).
- At the other extreme, a painful response that lingers (especially to temperature extremes) may indicate that the tooth’s nerve is compromised (irreversible pulpitis) and will require root canal treatment before it can be rebuilt.
Possible scenarios could be that the crack associated with the fracture extends to the tooth’s nerve. Or that bacteria have invaded the tooth’s nerve space via this crack and the tooth’s symptoms are associated with the degeneration of the tooth’s pulp.
▲ Section references – Torabinejad
► Broken teeth may irritate soft tissues.
- Due to the way they’ve broken, fractured teeth may have sharp edges that rub against and therefore irritate, abrade, or even lacerate soft oral tissues (cheeks, tongue, lips).
- In the case where the piece of broken tooth is loose but still attached to its associated gum tissue and therefore hasn’t come off, pain may be felt anytime pressure is applied to the piece and it shifts.
Ways dentists repair broken teeth.
It’s not always a catastrophic event when a tooth breaks. And in fact, in most cases, it usually isn’t. This can even include cases where the tooth has broken off, all of the way down right at the gum line.
a) Cases where just minor repair is needed.
- It’s conceivable that such a small portion of the tooth has chipped off that it only requires some minor smoothing using a dental drill.
Cases most likely solved using this simple remedy would be those where the entire depth of the chip is confined within the tooth’s enamel layer (described above).
- With smallish yet larger defects, just placing a small, conservative filling may make a satisfactory fix.
Bonded restorations (a type of filling that creates a bond with tooth enamel How this works.) often make an especially good choice for this type of repair because they can be placed without a need for extensive, or possibly any, tooth trimming first.
- In cases where the dentist does notice a crack in the tooth that they are repairing, a best practice, if possible, is to trim away those portions of the tooth that it involves.
It may be indicated to place a sedative filling in the tooth for a period of weeks (to make sure the tooth settles down and is OK) before placing the permanent filling.
(Abbott)
- While not the usual solution, it may be that your dentist feels that simply bonding the broken fragment back into place makes the quickest, simplest, and best color-matching repair.
Don’t expect this remedy to be offered in very many cases. But doing so can sometimes make a serviceable solution.
(Garcia)
- In rare cases, your dentist may conclude that although the amount of damage you’ve experienced so far is small your tooth now lies at increased risk for further damage.
As an example, possibly they’ve identified what they interpret as being a significant crack in the tooth that at this stage is symptomless. If so, they may recommend the placement of a dental crown (see next section).
(Abbott)
▲ Section references – Garcia, Abbott
b) More extensive fractures.
Teeth that have larger sections missing will require more extensive work. But you don’t necessarily have to be concerned that a repair can’t be made.
Even teeth that have had a substantial portion break off are usually salvageable. This includes those that appear to be broken off flat at the gum line or even below it. And, actually, making these types of repair are probably pretty routine for your dentist.
Types of restorations that may be needed for teeth with comparatively large portions missing.
- It may be that placing a filling can provide a suitable repair. However, durability issues may be a concern with large fillings. Additionally, just placing a filling may still leave the tooth at risk for further breakage.
- Dental crown placement What is a crown? can help to reinforce and strengthen a broken tooth. And for teeth that have experienced a catastrophic event and as a result are missing a significant amount of original tooth structure, choosing this option frequently makes the smart choice.
(This page explains situations where a dental crown may make a better choice than just placing a large filling Indications / Pros & cons..)
In cases where a substantial portion of a tooth has been lost, like when broken off at the gum line, being able to successfully anchor a filling to the tooth may pose a substantial challenge. And if so, placing a crown may be the only way to successfully rebuild it.
In some cases, the only way of successfully anchoring a crown may be via elective root canal treatment and then post and core placement. What is this? (Abbott).
- The possibility does exist that the treating dentist may feel that bonding the fractured remnant back in place makes a reasonable repair.
One might anticipate that this would be the exception rather than the rule. And more likely with comparatively smaller broken pieces than larger ones. It also might be more likely with broken front teeth (incisors, possibly canines) rather than back ones (molars, premolars) where the level of chewing forces involved is greater. (Garcia)
▲ Section references – Garcia, Abbott
c) Especially problematic cases.
Certain characteristics of the way a tooth has broken may complicate its repair.
- If the piece that fractured off extends far below the tooth’s gum line, periodontal (gum) surgery will be needed.
- If the fracture has resulted in serious damage or insult to the tooth’s pulp tissue (nerve), root canal treatment will be required.
1) Cases where gum surgery is required.
This complication arises when the edges of the broken piece extend far below the tooth’s gum line and therefore involves its root (see animation).
A tip-off that this condition exists can be that a loose tooth fragment remains stubbornly attached to surrounding gum tissue.
A fracture that involves the tooth’s root.
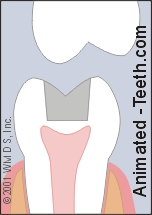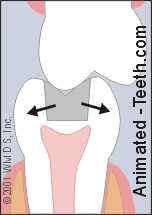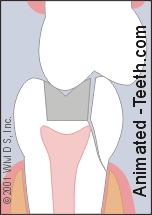
(Note: The tooth’s nerve seems involved too, see below.)
The problem.
- If the edge of the dental restoration placed to repair the damage lies too close to the bone level that surrounds the tooth, the gum tissue in that area will remain persistently irritated and inflamed.
This inflammation could result in gum recession, or even the loss of supporting bone around the tooth. Both symptoms might affect neighboring teeth too.
- If to small amount of tooth structure extends up past the level of the gum line, the dentist may not be able to adequately anchor a new restoration (crown or filling).
The solution – Crown lengthening.
A type of gum surgery termed “crown lengthening” is the solution usually used to resolve either of the issues just mentioned.
- This is a minor surgical procedure where the level of the gum and bone tissue surrounding the tooth is lowered, thus revealing more of it.
- After healing has occurred, a restoration can then be placed under more favorable conditions.
- [With teeth toward the front of the mouth (incisors, canines, possibly premolars), the appearance of the repositioned gum line must be considered before this approach is chosen.]
▲ Section references – Rosenstiel
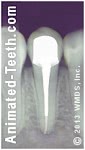
This broken tooth required root canal and a crown.
2) Cases where root canal treatment will be required.
- Clearly, your tooth’s level of symptoms (pain especially) will hint to you that a nerve problem exists or is developing, although not all teeth that require root canal treatment display obvious signs.
- Other than that, it’s not really possible for a layperson to know, just by looking at their tooth, whether this step will be required or not. Even teeth that seem to be broken off even with the gum line may not have a complication involving their nerve, whereas much smaller-looking fractures do.
How dentists temporize fractured teeth and manage their symptoms.
Until that time when arrangements can be made to permanently repair your tooth, your dentist will take steps to help alleviate whatever symptoms you are experiencing. If direct attention from them is not possible, they may instruct you on how to perform steps on your own using OTC (over-the-counter) products.
Tooth pain.
Anti-inflammatory medications.
In some cases, a tooth’s discomfort may be associated with a condition termed “reversible pulpitis” (reversible nerve inflammation). This involves a state where the tooth’s pulp tissue is healthy (this includes that it has not been directly affected by the fracture), just temporarily irritated due to the level of trauma the tooth received when it fractured.
In treating these types of cases, a dentist may suggest the use of an NSAID medication (non-steroidal anti-inflammatory drug). You may be familiar with this drug class as a pain reliever. But just as important they can help to prevent/minimize/reduce the level of the tooth’s pulp tissue inflammation, and therefore the complications it brings during the nerve’s attempted recovery.
- Examples of NSAIDs include: ibuprofen (Motrin, Advil), aspirin, naproxen (Aleve). (Each is available as an OTC product.)
- As an example of an adult’s use of ibuprofen with the goal of settling down the level of pulp tissue inflammation, with the added benefit of controlling discomfort: 200 to 400 mg every 6 hours for the first 1 or 2 days following the event.
▲ Section references – Haas, Hargreaves
Of course, when any type of medication is considered, its appropriateness for use by the patient must be evaluated. A common issue of concern is the potential for NSAIDs to create gastrointestinal problems. Also, taking NSAIDs may inhibit the blood clotting process, a factor that would need to be known/considered/managed by the person’s dentist in the event that the tooth’s extraction is indicated.
Temporary / Sedative fillings.
- Some types of temporary filling materials have anti-inflammatory and anesthetic properties. As such, they can be used to help sedate/soothe/aid in the recovery of teeth experiencing reversible pulpitis (healthy but irritated pulp tissue, the cracked or fractured portion of the tooth has no direct connection with the pulp).
- As an added benefit, the placement of the filling seals and protects the tooth from added insult, like that experienced with hot or cold foods and beverages. The filling may also help to protect oral soft tissues from irritation from sharp edges.
The kind most commonly placed by dentists is a mixture of zinc oxide (powder) and eugenol (liquid). It’s the very low level of eugenol that seeps from the restoration through tooth tissues (dentin) toward the tooth’s pulp that provides the benefits. (Abbott, Markowitz)
A dentist will trim away portions of the fractured tooth that have associated pathology (cracks, decay, etc…). The temporary filling is then placed and the tooth is monitored over a series of days and weeks as its recovery is evaluated. (Abbott)
▲ Section references – Markowitz, Abbott
Initiating root canal treatment.
In cases where the above possibilities either can’t, aren’t expected to, or aren’t an appropriate means for controlling the pain from the fractured tooth, a dentist will initiate root canal therapy.
(These situations would be classified as involving irreversible pulpitis, meaning cases where the level of nerve tissue insult/inflammation that exists is so great that recovery to a healthy state is not possible.)
If for whatever reason root canal treatment is indicated but not opted for, the only other appropriate option is to extract the tooth.
Prescription pain relievers.
In cases where direct (hands-on) attention from your dentist isn’t possible, they may prescribe a narcotic (prescription) pain reliever for you.
Unlike NSAID products, narcotic compounds only help to control pain. They have no anti-inflammatory effect. Using them is simply a temporary means of keeping a patient comfortable until more definitive treatment can be performed.
Since narcotics do nothing on their own to aid in the recovery of a tooth’s pulp tissue, in cases where that possibility exists (reversible pulpitis), they are sometimes prescribed in combination with an NSAID.
Temporizing loose but still attached tooth fragments.
In some cases, a person’s tooth may have fractured but the part that has separated hasn’t come completely loose yet.
What you may notice.
- Usually, the piece that’s fractured hasn’t fully separated because it still has an attachment to gum tissue that tends to hold it in place.
- Frequently the patient won’t experience pain unless they bite down on (or otherwise manipulate) the piece, thus causing it to shift. It’s possible that the discomfort noticed is actually coming from the gum tissue rather than the tooth.
Temporization.
- They can either attempt to temporarily splint the tooth back together.
Preparing (trimming down) the tooth and then placing a temporary dental crown could accomplish this goal. Possibly bonding the broken piece back into place might also serve as a temporary solution.
- Or they can remove the fragment, and then place some type of filling (see below).
Removing the broken part.
- With small pieces, a dentist may be able to just twist the loose part off with their fingers. (If your piece is a nuisance, and is extremely loose and just flapping in the breeze, your dentist may instruct you to do the same.)
- With more stubborn or larger fragments, they may need to use dental forceps (pliers) or an elevator How extraction instruments are used. to get hold of, or pry off, the piece.
Depending on how extensively the gum tissue has been attached, you can expect that there will be some minor bleeding (best controlled with finger pressure onto a pad of moist gauze) and soreness after the fragment has been removed.
While probably not of great importance, your dentist can learn details about the way in which your tooth has fractured from the broken bit, like how much of the tooth at a level below the gum line is involved.
Numbing your gums.
Numbing up the gum tissue attached to the loose fragment may or may not be needed. If it is, dabbing on a topical anesthetic gel or liquid (benzocaine, available OTC) may suffice. If not, then the use of a local anesthetic (a dental injection) will be necessary.
Temporizing missing tooth parts.
Especially if your broken tooth is sensitive (like in response to hot and cold foods) or has sharp edges, your dentist will fill in the missing fragment’s space by placing a temporary dental filling.
Temporary fillings for tooth voids.
- As discussed above, a common choice is zinc oxide and eugenol paste (available OTC).
As alternatives, for teeth that show (incisors, canines, premolars) a dentist may place some type of restorative (dental composite usually) that matches the color of the tooth more closely.
Or they may choose a material that has the ability to adhere to tooth structure (glass ionomer or composite), possibly allowing it to be placed without a need to trim/reshape the tooth first.
- If they can’t provide direct (hands-on) attention, a dentist will sometimes instruct their patient on how to place dental wax, or possibly zinc oxide and eugenol paste, (both available OTC) in their tooth’s broken area as a temporary measure to alleviate both tooth sharpness and thermal sensitivity.
Your tooth will remain at risk.
Of course, even after any type of temporary repair has been made for your tooth it will remain fragile and vulnerable to further breakdown.
The tooth must be favored so the level of pressure it’s exposed to doesn’t damage it further (like when you’re eating). As a way of helping to minimize the amount of force that the tooth receives, your dentist may trim it so it’s slightly shorter (referred to as “taking the tooth out of occlusion or contact”).
2) Your tooth has cracked but no piece has come off or become mobile.
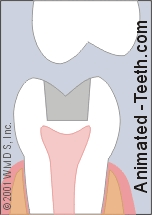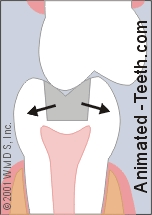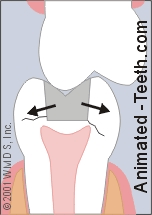
This tooth has cracked but no piece has come off.
▲ Section references – Abbott
a) Cases where a tooth has cracked – Some pain or discomfort is felt.
Cracked teeth can be sensitive. When biting pressure is applied, if a portion of the tooth on either side of the crack shifts (even ever so minutely), a painful response can be triggered.
Signs and symptoms of a cracked tooth.
- The tooth gives a sudden sharp pain in response to biting pressure.
- The pain subsides immediately once the biting pressure has been released, possibly eliciting another sharp painful response as you do.
- You may not feel the pain every time you close down. Sometimes it takes biting or biting on something, at just the right angle, to trigger the response.
- You may or quite possibly not be able to visualize the crack or feel it with your tongue.
b) Cases where a tooth has cracked – Little or no pain is felt.
Not all cracked teeth produce consistent symptoms. In fact, in some cases, it can be very difficult for the dentist to diagnose exactly which tooth lies at fault.
- It may take some time, including investigating on your own at home, to identify which tooth is the culprit.
- Tooth cracks can be exceedingly difficult, if not impossible, to visualize. Dentists sometimes apply a dye that seeps into cracks to make them more obvious.
- It can be difficult to identify a crack on routine dental x-rays. To be visible, the crack would have to lie in perfect alignment with the orientation of the x-ray machine’s rays. While possible, having this alignment occur isn’t so common. (Mamoun)
Identifying cracks, especially those that extend into a tooth’s root, typically involves taking multiple x-rays from different angles and comparing them. Sometimes advanced 3-D imaging is needed.
- Hairline cracks that can be visualized but produce no symptoms are often just tooth enamel craze lines that require no attention other than being monitored by your dentist over time. (Abbott 2009)
The textbook by Rosenstiel states that hairline cracks not subject to excessive loading (i.e. heaving chewing forces) can often go untreated. Simply monitoring them during routine dental recall appointments typically proves sufficient to identify newly developed signs and initiate corrective measures.
▲ Section references – Abbott, Mamoun, Rosenstiel
While identifying the problem tooth is of great importance, identifying the crack itself is somewhat less so. Even if the crack can be identified, knowing its full extent or nature usually isn’t possible.
The dentist simply treats the tooth based on the way they interpret the evidence they have. They then proceed with additional treatment solutions if the tooth’s symptoms continue or change.
How dentists repair cracked teeth.
There’s a range of solutions that a dentist can use to treat cracked teeth.
Minor cases.
If your symptoms are just minimal, it’s possible that your dentist may determine that your tooth requires little or no treatment. Sometimes just buffing the tooth down so it’s a tiny bit shorter than its neighbors (so it receives less biting pressure) provides a lasting solution. (This is referred to as “taking the tooth out of occlusion.”)
When more major repair is needed.
Especially in the case where your symptoms are persistent or severe, your dentist will need to provide some type of fix.
- It’s possible that placing a filling as a repair might suffice. This would be more likely in the case where the dentist feels they have identified the crack and anticipates that they understand its full extent.
During restoration placement, it would generally be the dentist’s goal to trim away those portions of the tooth in which the crack lies.
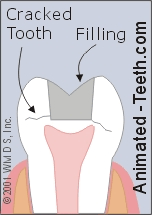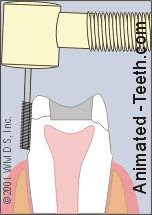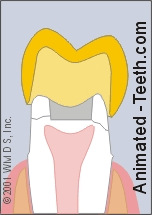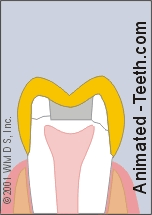
A crown acts as a splint that holds a cracked tooth together.
- In cases where the extent of the crack can’t be interpreted or the patient’s symptoms are severe, the dentist may feel that a dental crown should be placed.
Doing so will help to splint the tooth together so its cracked parts can’t shift and cause pain. This same splinting effect can also help to prevent the crack from progressing further.
- In some cases (often those that are most painful), the dentist may determine that the crack reaches deep into the interior of the tooth and involves its nerve. If so, before a dental crown can be placed, root canal treatment will be required. Why?
Or root canal may be needed because the tooth’s nerve tissue has been too traumatized by its ordeal and is not able to recover (irreversible pulpitis).
- It’s possible that even after placing a dental crown and performing root canal treatment the tooth’s symptoms will continue or new ones crop up. If so, the tooth will need to be extracted.
As examples: 1) Crown placement may not provide enough splinting effect that the tooth’s cracked segments are prevented from shifting when pressure is applied. 2) The crack may be colonized by bacteria. If so, they will cause a persistent infection that can’t be resolved.
▲ Section references – Abbott
How dentists manage and temporize cracked teeth.
Just as with broken ones, a dentist’s initial treatment of a cracked tooth will be to attempt to alleviate the patient’s pain and stabilize the tooth.
Reducing the tooth.
In cases where symptoms are relatively minor, the dentist may just buff the tooth down so it receives less biting pressure (take it out of occlusion).
Doing so can provide enough relief for the tooth that its symptoms subside. It can also help to reduce the risk of further tooth damage (crack propagation).
Temporary restoration placement.
When symptoms are more severe, the dentist may feel that they need to place some type of restoration promptly.
- They may remove the tooth’s permanent filling, trim away the portion of the tooth they interpret as being involved with the crack, and place a temporary restoration. As explained above, if the type selected has sedative properties it may help the tooth to settle down and avert pulp tissue (nerve) damage.
- In other cases, the dentist may feel that the tooth requires the protection of a crown promptly. If so, they may begin the crowning process The steps of the procedure. so a temporary one can be placed immediately. And like discussed above, they may choose a cement that has sedative properties.
Anti-inflammatory medications.
As discussed above, a dentist may recommend taking an NSAID medication. Doing so can both help to control the patient’s pain and be instrumental in helping their tooth’s nerve to recover from the insult it has received.
Allow your tooth some rest.
No matter what treatment has been provided, giving your tooth some rest will almost certainly be recommended.
Continually testing your tooth (like by biting on it) may only serve to aggravate or damage it further. Simply staying off it may substantially increase the odds that your tooth’s traumatized nerve will be able to recover from its ordeal.
Last reviewed: February 03, 2025
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Abbott P, et al. Predictable management of cracked teeth with reversible pulpitis.
Garcia FCP, et al. Tooth fragment reattachment techniques-A systematic review.
Haas BA. An Update on Analgesics for the Management of Acute Postoperative Dental Pain.
Hargreaves K, et al. Drugs for pain management in dentistry.
Lynch CD, et al. The cracked tooth syndrome.
Mamoun JS, et al. Cracked tooth diagnosis and treatment: An alternative paradigm.
Markowitz K, et al. Biologic properties of eugenol and zinc oxide-eugenol: A clinically oriented review.
Rosenstiel SF, et al. Contemporary Fix Prosthodontics. Chapter: Periodontal considerations.
Stefanac SJ, et al. Diagnosis and Treatment Planning in Dentistry. Chapter: Patient Examination and Diagnosis.
Torabinejad M, et al. Endodontics. Principles and Practice. Chapter: Longitudinal tooth fractures.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
Revealing more of the tooth.
I had a root canal 19 months ago but don’t have the crown yet because my dentist says there isn’t enough room to put it on. It’s my back lower left molar, #18 I think. My wisdom teeth were removed many years ago. I have to see a specialist who will cut my gum, and I’m afraid maybe the bone too? The dentist said it will take 6 weeks to heal before he can put the crown on after. Is this surgery really necessary? Is there an alternative?
Rachel S.
Reply –
What you seem to describe is referred to as crown lengthing. That link describes why it is needed.
When it is needed, there is no alternative. It seems your dentist feels that it’s important to have it done, hence their waiting for you has delayed their treatment of your tooth, which, depending on the type of temporary restoration that’s been placed, usually isn’t ideal.
Youtube no doubt has a number of videos showing the procedure. “crown lengthening periodontist” would probably be good keywords to use. Look for one showing the procedure for just a single tooth (like your situation).
Admittedly it is a surgical procedure but is also a comparatively minor and routine one.
Staff Dentist
