Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
Additional (valid) reasons for wisdom tooth removal.
Supplementary justifications for extracting wisdom teeth.
Beyond the issues of gum disease, tooth decay, or recurring pericoronitis (infection) that we’ve covered elsewhere on our website (use the links), there are additional factors that merit consideration when evaluating the necessity of wisdom teeth removal.
This page explores these equally significant reasons for extraction. Understanding these factors is essential for making an informed decision about your treatment options.
Additional factors that may be indications for third molar removal.
- Chronic pain / Pressure / Headache.
- Poor tooth alignment or positioning.
- Cyst or tumor formation.
- Damage caused to neighboring teeth.
FYI: The list above is a subset of our master list of (valid) justifications for extracting third molars.
You may also find this page of interest: Is it always necessary to remove impacted wisdom teeth?🔗
Full details about our “additional” reasons to extract third molars.
A) Wisdom teeth that cause pain.
- The most common reason why people seek an evaluation of their wisdom teeth is because they’ve recently experienced a painful episode.
- Having pain is the most common third molar symptom, with 33% of patients reporting problems stating it. (Pogrel)
The discomfort may be nebulous in nature.
The type of pain or sense of pressure that the patient reports is often vague or indistinct.
- The discomfort is sometimes described as a radiating pain stemming from the region of the wisdom tooth (Koerner).
- In other cases, the tooth is suspected as the cause of headaches or neuralgia (intense intermittent pain associated with the path of a nerve). (Fragiskos)
▲ Section references – Pogrel, Koerner, Fragiskos
Causes of 3rd molar related pain, pressure and headaches.
Especially in the case where the symptoms experienced are vague, indistinct or distant, it will be the dentist’s goal to discover a direct relationship between the discomfort and events taking place with or in the area of the person’s wisdom teeth.
Possible causes of ‘wisdom tooth pain’ include:
- Sensations associated with the tooth’s eruption process.
- Pressure that the erupting wisdom tooth directs to adjacent nerves.
- Active pathology associated with the tooth and/or adjacent structures or tissues, including decay, gum disease, root resorption, and soft tissue irritation, trauma, and/or infection).
- Pain not directly attributable to the wisdom tooth itself, including TMJ (jaw joint) dysfunction or some type of medical condition.
Each of these possibilities is explained in greater detail below.
1) The tooth’s eruption process.
The pain that a person has noticed with their wisdom tooth may be associated with the process of it coming in (its “eruption”).
The discomfort may be intermittent or constant. Patients sometimes describe what they feel as a vague sense of pressure.
2) Pressure on adjacent nerves.
In rare cases, an impacted lower wisdom tooth may place pressure on the nearby inferior alveolar nerve (the major nerve of the lower jaw).
▲ Section references – Haq, Fragiskos
3) Non-odontogenic discomfort.
There can be situations where the pain or pressure noticed by a patient certainly seems to be centered on the region where a wisdom tooth lies. But due to the absence of obvious pathology, their dentist can’t be certain that the tooth itself lies at fault.
- One common culprit is temporomandibular joint (jaw joint, TMJ) dysfunction, including pain stemming from its associated muscles.
This scenario is especially likely if the person has a habit of clenching or grinding their teeth, or has recently experienced a period of stress.
- In other cases, the symptoms might be caused by an underlying medical condition (migraine, cardiac, vascular, or neuropathic in nature).
In a rush to find a solution …
In situations where a clear cause for the patient’s discomfort has yet to be identified, a decision might be made to go ahead and remove the tooth in question in an attempt to alleviate the patient’s condition as promptly as possible. If so, the patient must be advised that relief may not be achieved and ultimately the procedure they endured was unnecessary.
▲ Section references – Koerner
4) Common wisdom-tooth related pathologies.
Once investigated, what a person has experienced can often be directly attributed to common wisdom tooth-related issues and pathologies. This could include most any of the conditions or situations discussed further below on this page, or the following items that we discuss elsewhere.
- Common causes of pain are an infection around the tooth, or trauma to the layer of skin (gum flap) that lies over it.
- Other common issues may involve just the wisdom tooth itself, or possibly the adjacent 2nd molar too. These can include pain as a consequence of tooth decay, gum disease or root resorption.
B) Poorly positioned wisdom teeth.
Some wisdom teeth manage to erupt but nevertheless wind up with a positioning that causes, or has the potential to cause, problems. As examples …
Wisdom tooth positioning issues/problems that can be cause for extraction.
- The tooth has erupted but its alignment is “crooked.”
- The tooth has erupted as much as it will but still doesn’t adequately clear its surrounding gum tissue.
- The tooth’s positioning is such that it’s difficult to thoroughly clean.
- The tooth has supererupted.
We explain each of these deficiencies in greater detail below.
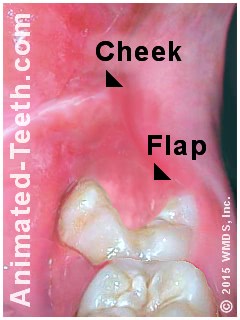
Trauma to both flap and cheek tissue in the area of a 3rd molar.
a) Crooked teeth.
b) High gums or gum flaps.
This may cause the tissue to become chronically inflamed (reddened, sore and swollen, like the “flap” tissue in our picture).
In some cases, the excess tissue can be successfully trimmed away. In others, it may tend to grow back over time. (It depends on the tooth to jawbone relationship that exists.) If your dentist determines that the latter is the likely outcome for your situation, then the tooth will need to be extracted.
c) Supererupted third molars.
Wisdom teeth that don’t have an opposing tooth to bite against often supererupt (poke through the gum tissue further than normal).
These teeth may cause tissue irritation or trauma. Their abnormal positioning may interfere with jaw movements, or create traps between teeth where food and debris tend to accumulate. Teeth having this problem should be extracted.
d) Teeth that are hard to clean.
Some wisdom teeth occupy a position that makes them very difficult to brush and floss. If so, both they and their neighboring tooth are placed at increased risk for complications with tooth decay and gum disease. And for that reason, they should be removed before problems develop.
C) Cysts and tumors.
While not an especially common occurrence, cysts or tumors can arise from the retained developmental tissues associated with an impacted wisdom tooth.
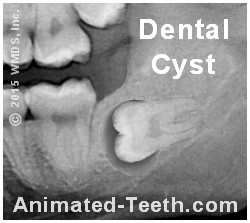
It is the size of the tissues that surround this tooth that suggest cyst formation.
Identification and treatment.
A tooth’s associated pathology is most often discovered via x-ray examination. Once identified, the tooth should be removed and its cyst or tumor evaluated histologically (microscopic evaluation) by a pathologist for identification.
Monitoring impacted wisdom teeth.

Misdirected eruption can trigger the resorption of adjacent teeth.
D) Root resorption of neighboring teeth.
When they fall out, they look as though they don’t have a root. That’s because as the permanent tooth underneath erupted, its presence caused the baby tooth’s root to resorb (dissolve away).
▲ Section references – Hupp
Last reviewed: February 17, 2025
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Fragiskos FD. Oral Surgery. Chapter: Surgical extraction of impacted teeth.
Haq Z. A survey of reasons for surgical removal of impacted mandibular third molar in armed forces personnel at Afid, Rawalpindi.
Hupp J, et al. Contemporary Oral and Maxillofacial Surgery. Chapter: Principles of Management of Impacted Teeth.
Koerner KR. Manual of Minor Oral Surgery for the General Dentist. Chapter: Surgical Management of Impacted Third Molar Teeth.
Pogrel MA, et al. American Association of Oral and Maxillofacial Surgeons White Paper on Third Molar Data.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
Scheduled for extraction tomorrow
2 wisdom tooth to pull by tomorrow.. is it safe to pull a tooth while im suffering severe pain on all left side jaw,ears and head?
Jam
Reply –
Possibly. In many cases having the extraction could be the right solution. In other circumstances, like when a tooth has an associated infection, the extraction process may need to wait until the secondary issue is brought under control but certainly not always.
You should touch base with your dentist’s office and let them know what’s going on. They can then quiz you about the pain that you notice and decide what’s needed, and what the timing of your extractions should be.
As a courtesy, you should contact them as much ahead of time as possible. They have set aside appointment time for you and now if you don’t need it (or just less of it) they should know so they can see other patients that require attention.
Staff Dentist
Comment –
extract tooth in lower jaw
I am 42 years old and have in the extra teeth lower jaw. It is always an abstraction for my tongue while speaking. the tongue is cut due to touching of teeth while speaking. I find difficult when i speak because it gives lots difficulty.
amar 1
Reply –
Like this page discusses, a very legitimate reason to remove a wisdom tooth is because its position in the jaw is such that it disrupts normal function. You should bring this problem to your dentist’s attention. Quite likely they will recommend the tooth’s extraction.
Staff Dentist
Comment –
Wisdom tooth cutting back of my cheek
I am 25. Last year, I got a wisdom tooth on the upper left side. It is partially erupted. Never had a problem cleaning it. But day before yesterday when I woke up in the morning I felt a slight pain at the back side of my left cheek. On closer inspection, I noticed that it was caused by the wisdom tooth slicing across the cheek. It made it difficult (but not so much) for me to completely open my mouth. Yesterday I rinsed my mouth twice with salt water. The pain seems to be fading now. Should I be worried about my tooth? Will it cause trouble in future if I don’t get rid of it?
PS
Reply –
You simply need an evaluation by a dentist. They’ll advise you as to what should be done with your tooth and if your current infection needs any management by them.
As far as the tooth’s outlook, as discussed above, a big question is whether the tooth’s partially erupted status is permanent or transitory. If it’s expected that the tooth will never fully come into proper position, despite your comment “Never had a problem cleaning it.”, as the illustrations on this page show, it’s not really possible to thoroughly clean a partially erupted tooth, so there’s always the potential that the same problem will occur again at some point.
While we’re not entirely clear on this statement: “caused by the wisdom tooth slicing across the cheek.” It’s not uncommon for an upper wisdom tooth to come in at an (improper) angle where its cusps scrape and irritate the patient’s cheek. If a tooth is both partially erupted and has a poor alignment, extracting the tooth is a common solution but it will take your dentist’s evaluation to decide if that is indicated.
Staff Dentist
