Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
Endodontist vs. General Dentist – Who should perform your tooth’s root canal work?
Endodontist or Family Dentist – Which makes the right choice for performing your tooth’s root canal therapy?
When it comes to having a root canal, dentistry offers two options. Either your regular (general) dentist can perform your tooth’s work, or else a specialist. The formal term for a root canal specialist is “endodontist.”
This guide compares the two, offering insights into their expertise, success rates, and the types of cases best suited for each. Whether you’re prioritizing the highest level of care for a complex case or balancing cost and convenience, this page provides the insights you need to make an informed choice.
General Dentist vs. Endodontist – What differences will you encounter?
When the root canal procedure is considered in its entirety (scheduling, costs, treatment time, success rates, etc…), each type of dental professional, your family practitioner vs. a dental specialist, offers a different set of advantages.
a) Advantages associated with choosing an endodontist.
1) Greater expertise and clinical skill.
An endodontist is a dental specialist and as such has:
- All of the same schooling as your regular dentist …
- … Plus 2 or 3 years of additional training in graduate school that’s entirely focused on just performing endodontic procedures …
- … And also, however many years of being in practice where each day they only perform this one kind of work.
All combined, the above factors generally mean that an endodontist has a lot of knowledge about, and is quite expert in doing, that which they do. (More about the specialized training Details. endodontists receive.)
2) More-advanced equipment.
The range of tools and equipment that an endodontist equips their office with typically lies a full level above that which a general dentist has.
For example, most specialists use a surgical microscope to examine the interior of the tooth they’re treating. And nowadays, most probably have 3D X-ray imaging (Cone Beam CT scan) capability. ( More details about specialized Endodontic equipment. )
Equipment of this caliber isn’t needed for every case. But having it may be indispensable for diagnosing and treating teeth that pose especially unique or complex endodontic challenges.
3) A higher level of diagnostic skills.
Due to their additional years of training and use of more sophisticated equipment, an endodontist is generally considered to have greater expertise in diagnosing difficult cases and their associated dental problems.
4) Shorter or fewer appointments.
Because all they do is perform endodontic procedures, an endodontist is typically very proficient in providing treatment. That typically translates into your having shorter or having to schedule fewer appointments.
5) Higher treatment success rates.
Research studies suggest that treatment completed by endodontists tends to have a higher success rate. This is especially true for certain kinds of teeth Which ones?
And while not a true apples-to-apples comparison between a general dentist’s work vs. a specialist’s, due to their advanced training and expertise, an endodontist can offer a wider range of endodontic procedures. Ones that comparatively more difficult cases might require for a successful outcome.
This includes endodontic surgery (apicoectomy, root-tip surgery) and root canal retreatment (to correct failed treatment).
A general dentist has an obligation to refer patients out for dental work they don’t have the skill to provide. However, it’s conceivable that a general practitioner may not fully recognize situations where a more advanced procedure is needed.
6) More expertise in pain management.
It’s only logical to assume that a practitioner who has “seen it all before” will be more likely to be able to anticipate and successfully manage their patient’s pain-related problems.
b) Advantages offered by general dentists.
The benefits associated with choosing an endodontist won’t play a significant role in all cases.
That’s because not all root canal procedures pose a great challenge. And in the case where your own family dentist is more than capable of performing your work, there are certain advantages in having them do so.
A dentist performing root canal treatment.
1) Lower fees.
There’s usually a financial premium attached to the services of a dental specialist. It’s generally expected that an endodontist’s fee will be higher Root canal costs. than your regular dentist’s for the same procedure.
2) A familiar office environment for you.
Having your family dentist perform your work has the advantage that your treatment will be performed in an office you’re already familiar with, by a person you already know.
And because your dentist and their staff already know you too, they may be more accommodating with scheduling, billing, and insurance issues than an endodontist’s office might be.
3) Convenience.
In some parts of the country, just finding an endodontist can be a relatively difficult experience. Getting to one may require a trip to a nearby metropolitan area. Or, if one travels to your town, they may only schedule appointments on a limited number of days.
4) Treatment continuity.
Having just one person perform all of the different procedures your tooth requires can sometimes be a benefit.
For example, a tooth might have a quirk or peculiarity whose details might be difficult to communicate from one practitioner to another. Also, there may be some advantages in terms of appointment scheduling such as having more than one procedure performed during the same office visit.
General dentists vs. endodontists. – Treatment success rates.
When it comes to your tooth’s work, there’s no factor that’s more important than its ultimate success. And it seems logical to speculate that the added expertise that a specialist has to offer will favorably influence the outcome of the treatment they provide.
Statistics from the following research studies seem to confirm this, at least to some degree, and for some types of teeth more so than others.
Alley (2004)
This small study (350 cases) found a success rate of 98% for therapy performed by endodontists vs. 90% for cases completed by general practitioners.
Iqbal (2016)
Using a sample of 90 failed root canal cases, this study found that 79% of them represented work that had been performed by general dentists.
This paper also cites a study (Weiger 1998, a historic study that we don’t have access to) that determined that the success rate of endodontic therapy performed by general dentists generally runs on the order of 65% to 75%. For specialists, this number was 90%.
Lazarski (2001)
This study investigated the outcome of over 100,000 root canal cases by way of evaluating an insurance company database. Each tooth was followed over a time frame of at least 2 years.
- The study found a similar success rate for work completed by both specialists and general dentists (94% at 3.5 years).
- The paper noted however that the specialist group treated a substantially greater percentage of molars (multi-rooted teeth often having a very complex root canal system), whereas the generalist group had more single-rooted, typically easier to treat, teeth.
Burry (2016)
Also extracting data from an insurance company database, this study monitored the outcome of almost one-half million root canal cases, broken into groups of 1, 5, and 10 years following the completion of their work.
- Molars – At 5 years, molars treated by specialists had a 2% higher survival rate. At 10 years this difference expanded to 5% (84% vs. 89%).
- Incisors, Canines, Premolars – For these types of teeth at 5 years, no statistical difference was found in survival rates for cases performed by endodontists vs. dentists. At 10 years, a 1% difference in success was reported (around 91%).
▲ Section references – Alley, Iqbal, Lazarski, Burry
Do these studies suggest that some types of teeth are best treated by endodontists?
Possibly. To recap the study just mentioned (Burry), it suggests that:
- As far as 10 years out, relatively little difference is found in the success rate of cases completed by endodontists vs. general dentists for incisors, canines (cuspids, eyeteeth), and premolars (bicuspids).
- But for molars, a survival difference is apparent at longer durations (5% at 10 years out).
Those findings seem to correspond pretty well with the data in our “root canal failure rates by tooth type” tables Study findings. which seem to suggest that:
- Treatment failure is more frequent with molars (possibly more so with upper ones) than incisors and canines.
- Root canalled premolars (more so upper ones) tend to fail at a rate greater than that for front teeth (incisors and canines) but less than molars. (This is in contrast to the Burry study above which found the failure rates for incisors, canines, and premolars to all be about the same.)
Formulating general guidelines about opting for treatment by a general dentist.
Using the information above, you could draw some broad conclusions about which types of teeth are generally the easiest to treat, and therefore the best candidates for treatment by a general dentist.
It’s important to keep in mind however that the following statements are simply our conjecture, and that of course exceptions always exist.
a) Incisors, Canines, Lower Premolars.
The level of skill needed to successfully treat upper and lower incisors, upper and lower canines, and lower premolars generally seems to lie within the capabilities of general dentists in the majority of cases.
As an explanation, these are single-rooted teeth that most frequently just have a single, relatively large (and therefore comparatively easier to treat) root canal.
b) Molars.
While the long-term failure rate of molars treated by general dentists is relatively low (16%), the added expertise that an endodontist can provide apparently provides a benefit (11% case failures), especially when the long term is considered (both statistics cited here involve a 10-year interval). (Burry)
Additional factors that favor considering having an endodontist perform your tooth’s work.
- Of all of the different kinds of teeth, molars are the type most likely to experience failure. (Per our tables link above, likely comprising 46% to 58% of all failed cases).
- Per the Lazarski study cited above, it seems that molars are the type of tooth most commonly referred by general dentists to specialists for treatment.
[It would be our conjecture that this implies that endodontists typically treat more difficult cases (the cases that general dentists refer out), and therefore their overall failure rate of 11% mentioned above might be lower if it only included cases having a similar level of difficulty as those treated by general dentists.]
- Per our reference below, choosing a dentist who is a recent dental school graduate may not make the best choice for providing molar endodontics.
As an explanation, molars have the most complex root canal anatomy. That includes the greatest number of roots and the largest number of individual root canals What’s normal? | Variations, many of which are characteristically small and often branched thus making them difficult to locate and treat.
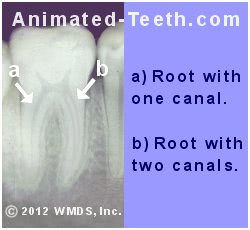
Molars can be difficult to treat because they have multiple roots and canals.
All things considered, and in the sense of erring on the side of caution, electing to have an endodontist complete your molar’s work seems to make a reasonable first choice. However, from a strictly statistical standpoint, either type of provider (specialist or general dentist) is likely to create a successful outcome.
c) Upper Premolars
Judging the necessity of a specialist’s care for upper premolars is somewhat difficult to determine.
- Our Burry reference above found no statistical difference in outcome for premolars in general (upper or lower) when treated by either type of practitioner (and actually calculated a slightly lower success rate for specialists, 90% vs. 91%).
- However, two of our failure-by-tooth-type tables linked above suggest a higher failure rate for premolars in general, and one of them for upper premolars in particular.
As an explanation: 1) upper premolars may have one or two roots and 2) one, two, or more root canals. This variability makes treating them less straightforward.
Just like for molars, in the case of upper premolars, it seems that electing to have an endodontist complete your tooth’s work makes a reasonable first choice (for erring on the side of caution). Although from a strictly statistical standpoint (according to the studies we’ve cited), either type of provider is likely to be able to produce a successful outcome.
▲ Section references – Lazarski, Burry
Special circumstances.
a) Troublesome teeth.
Of course, none of the above general guidelines should apply to teeth where your dentist has identified factors that suggest that the level of skill needed to complete its work lies beyond their capabilities.
Whether this fact is identified before or during the treatment process, it only makes sense that the tooth’s work should be referred to an endodontist for completion.
b) Strategically important teeth.
We’d also suggest that in cases where a tooth is vitally important from a standpoint of associated dental work, and that tooth’s root canal treatment seems even remotely challenging, that a referral to an endodontist as a way of helping ensure the most predictable outcome makes sense.
As examples, this type of scenario might include teeth that (currently do or will in the future) support a dental bridge or removable partial denture. Or teeth whose replacement by an implant might pose challenges.
c) Retreatment success rates.
The point of making sure that your tooth is in the right hands initially is an important one because beyond just the added cost and inconvenience, if a tooth’s work fails and retreatment is then needed Possible options., the success rates associated with this work are generally lower than for a tooth’s original treatment.
Rates run lower on the order of 6 to 8% for conventional retreatment (just repeating the tooth’s original work, the method used in most cases) and 22% when surgical intervention is needed. (Elemam)
A common difficulty associated with retreatment is that its success has been hampered by issues arising because of previous mismanagement of the case. Iatrogenic factors. (The assumption here would be that this scenario is more likely associated with treatment performed by a general dentist.)
So especially with vitally important teeth, doing whatever is needed so treatment is completed to the highest standards the first time makes the most prudent choice, by far.
Endodontists typically use more advanced equipment.
A part of the difference in treatment success suggested by the studies above, especially with difficult-to-treat teeth like molars, may have to do with the more sophisticated equipment that an endodontist typically has. Two examples that stand out are:
Surgical microscope. – This instrument is used to scan the interior of a tooth in search of tiny root canals or cracks.
( Missed canals Details. and cracks in roots Details. are two of the most common reasons for endodontic failure. A study by Hoen suggests that 42% of failed cases involve missed canals. )

An endodontist using a surgical microscope.
Using their high-powered microscope, an endodontist can inspect a tooth’s interior with much greater precision and thoroughness. This helps to ensure a successful case outcome.
Cone Beam Computed Tomography (CBCT, Cone Beam CT scan) – This method of taking X-rays gives a 3D representation of the patient’s teeth and surrounding jawbone. The details this kind of imaging reveals can be a big aid in evaluating, diagnosing, and treating teeth that have especially challenging root canal systems.
Since general dentists only perform endodontic dental procedures as a portion of their daily caseload, they usually have trouble justifying the high cost of these types of specialized high-end equipment.
Additional considerations in deciding between a general dentist vs. an endodontist.
a) Shorter appointments.
All other issues being equal, it only stands to reason that a practitioner who specializes in providing a single kind of treatment will be more adept at completing it than one who only performs that type of work occasionally.
Beyond just operator skills, equipment that can expedite the treatment process will typically be a must-have for an endodontic office, whereas for a general dentist purchasing them may not be cost-effective.
A study by Wong found that the amount of time needed for a tooth’s treatment correlated (decreased) with: 1) greater operator experience and 2) the use of optical magnification. Both of these are factors more likely associated with treatment provided by specialists.
A general dentist may be able to offer better treatment continuity.
It shouldn’t be overlooked that just having one person perform all of your tooth’s work may offer the advantage of being able to combine some of your needed procedures into a single appointment. As examples:
- Your dentist might be able to begin your tooth’s root canal treatment during the same appointment when its need for treatment was diagnosed.
- At the completion of your endodontic procedure, your dentist might be able to place, or at least begin the process of placing, your tooth’s final restoration. The advantage is that there would be less risk of coronal leakage A cause of failure. occurring or in the case of a fragile tooth that requires strengthening How crowns reinforce teeth., tooth fracture.
b) Pain management.
While there’s no reason why any dentist shouldn’t be able to control a patient’s discomfort Steps they can take., since handling “hot” (painful) teeth is such a routine matter for endodontists, they might be better at anticipating or controlling pain-related complications.
It’s also conceivable that a specialist’s office might offer a wider range of anxiety control and sedation techniques Common options. for use with your procedure.
c) Has your dentist considered a referral?
No doubt, most patients simply follow the advice of their dentist in deciding who will perform their tooth’s root canal work. But this requires that they have been objective in weighing the quality of care they can provide versus what is required for the satisfactory completion of your case.
Terms that come into play when making a decision are “standard of practice” (technical details about how your procedure is performed) and “standard of care” (a comparison to what other practitioners would do).
A major tenet of the latter is that the dentist must provide a level of treatment that serves their patient’s best interests and protects their health. And while that doesn’t necessarily mean that the treatment they provide must be successful, their decision to take on a case must conform with what other general practitioners within the same community would choose to do. As examples:
- These terms would be defined differently for localities where the services of an endodontist are readily available vs. those where they are not.
- There would be less latitude involved in interpreting these terms in cases where the dentist simply did not want to refer out cases that could generate income for their practice, or where the dentist chose not to use a protocol that conforms with modern endodontic standards.
What does it take to become an endodontist?
Exactly what it takes to be credentialed as a root canal specialist varies by state and/or country. The usual requirements are that the person has:
- Completed a dental degree. – This means that an endodontist has the exact same basic training as your general dentist, in all fields of dentistry.
- Completed an advanced training program. – This typically involves 2 to 3 years of additional schooling.
Usually, an endodontist must limit the scope of their practice to just performing endodontic procedures. (As an example, that means they can’t be the one to place a new dental crown on your tooth after its root canal work has been completed.)
Board Certification
Being “board certified” is a separate credential. It’s issued by a country’s governing association for that specialty. In the USA, it means that the endodontist has passed a set of examinations (oral, written, case presentation) overseen by the American Board of Endodontists.
Professional organizations.
Just as many dentists choose to join the American Dental Association (ADA) for professional, educational, and social purposes, an endodontist and even general dentists may choose to join the American Association of Endodontists (AAE). Doing so has no bearing on their qualifications as a practitioner.
Comparing the level of training of endodontists vs. general dentists.
a) Dental school training.
The amount of experience that a new dental graduate (DDS, DMD) has in performing endodontic care might be less than you’d expect.
One study (Woodmansey) polled the directors of US and Canadian dental school (predoctoral) endodontic programs. 60% of the schools provided a reply.
- On average, the total number of root canal cases completed by students before graduating was just 6. (It would be our conjecture that these would tend to be simpler, more straightforward cases.)
- When asked if they felt their graduating students were competent to treat molar cases, 36% of directors responded “yes,” 36% “no,” and 28% were uncertain.
b) Graduate program training.
We ran across a position paper written by the European Society of Endodontology stating what they considered the minimum criteria they felt appropriate for specialists’ training. (Gulabivala)
It stated that its recommendation was that a graduate student should spend 60% of their training in clinical activity, with a minimum of 180 cases (teeth) treated during the course of a 3-year program.
A 2007 standards paper published by the American Dental Association states that 40 to 60% of a student’s training should involve clinical practice, although no set number of treated teeth is mentioned. We should also state that this paper states that a period of 2 years of training is adequate.
Either way and as you would expect, the level of training and experience accumulated by endodontists during their schooling far exceeds that provided to general dentists.
▲ Section references – Gulabivala, Woodmansey
What’s next?
We have more to share about having root canal therapy.
Last reviewed: January 21, 2025
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
Alley B, et al. A comparison of survival of teeth following endodontic treatment performed by general dentists or by specialists.
Burry JC, et al. Outcomes of Primary Endodontic Therapy Provided by Endodontic Specialists Compared with Other Providers.
Elemam RF, et al. Comparison of the success rate of endodontic treatment and implant treatment.
Gulabivala K, et al. Accreditation of postgraduate speciality training programmes in Endodontology. Minimum criteria for training Specialists in Endodontology within Europe.
Hoen MM, et al. Contemporary Endodontic Retreatments: An Analysis based on Clinical Treatment Findings.
Iqbal A. The Factors Responsible for Endodontic Treatment Failure in the Permanent Dentitions of the Patients.
Lazarski MP, et al. Epidemiological evaluation of the outcomes of nonsurgical root canal treatment in a large cohort of insured dental patients.
Wong AW, et al. Treatment time for non-surgical endodontic therapy with or without a magnifying loupe.
Woodmansey K, et al. The Landscape of Predoctoral Endodontic Education in the United States and Canada: Results of a Survey.
Comments.
This section contains comments submitted in previous years. Many have been edited so to limit their scope to subjects discussed on this page.
Comment –
Regular dentist vs. Endontist
My dentist tells me I have a tooth that needs root canal and has scheduled an appointment for me. I have friends who have had bad experiences with their root canals and tell me I should go to a specialist. How do I decide what to do?
JM
Reply –
From just the standpoint of the outcome of the work performed, it’s easy enough to assume that your case is in more predictable hands with an endodontist.
An endodontist has all of the same training as a dentist, plus at least two additional years of schooling/clinical work concerning just root canals. Plus in their practice that’s the only kind of treatment they preform, for years on end. It’s hard for a general dentist to compete with those credentials.
As an example and as we discuss above, seemingly the success rate of molar treatment by general dentists and endodontists is similar. However, since it’s expected that endodontists are generally referred comparatively more difficult cases, one could speculate that if given the same population of teeth to work on that the success rate of treatment by specialists might be even higher.
That by no means is to say that a general dentist can’t provide expert care or that all teeth require a specialist’s level of skill. But it is fair to say that a general dentist might not have the expertise or equipment to be able to recognize when the task at hand lies beyond their capabilities. Or a general dentist may discover this fact in the middle of treatment, when the issue of referral becomes more complicated.
We’d generally have the opinion that when it comes to root canal treatment the best shot should be taken first. Beyond just the issues associated with dealing with treatment failure, the expertise with which the tooth’s original treatment was performed (or lack thereof) can affect the outcome of retreatment.
Having said all of that, in real life issues like cost, endodontist availability, patient convenience, insurance coverage, etc… certainly all come into play too. And most certainly they may affect what is determined to make a reasonable choice.
With your situation, express your concerns to your dentist. Ask if there are any issues about your case that might suggest that treatment by a specialist might be needed.
It’s their professional obligation to you to explain all of your treatment options to you, and that includes who might make the best choice for treating your case. Good luck.
Staff Dentist
Comment –
“Survival”
You use the term “survival” in the same context as “success,” but it’s unclear what you mean by survival. Do you mean survival of the tooth or “survival” of the root canal procedure (meaning that the root canal hasn’t failed after X years)? I haven’t seen “survival” used before in the latter way, as in “survival” of a medical/dental procedure.
Scott
Reply –
Our choice in the use of the word “survival” above was based on the wording found in the study that the associated information was taken from (Burry 2016, see page references link above).
Per that paper: “Survival of an endodontically treated tooth has been defined as continued presence and painless function.”
Staff Dentist
Comment –
Endodontist wait time.
Can things be safely left ? For example I have a fistula and gum boil caused by abscess at bottom of a molar tooth. My dentist has offered choice of him doing it in a few days or waiting 3 weeks to see a specialist endodontist. Which would you advise. I want to wait but the idea of an infection inside for so long worries me. What are average waits to see an endodontist ? ( I am in UK but curious about wait times anywhere)
Greg
Reply –
A scenario that sometimes applies is this. You’d have to quiz your dentist to know if it applies in your case.
1) “a fistula and gum boil” (technically a sinus tract) are often associated with teeth that are necrotic (contain no live nerve tissue).
2) With necrotic teeth, a common cause of acute flare-up is when the infection inside the tooth becomes active and produces increasing levels of pus. This causes tissue swelling. It also causes a buildup of pressure that can cause pain symptoms.
3) When a sinus tract is present, the pus instead can vent off. If so, there will be no significant buildup of pus, thus minimal symptoms.
In regard to timing, it’s your dentists obligation to take whatever steps they feel are necessary to minimize the potential that you will experience problems/added complications during the waiting period when definitive treatment can be performed (whoever provides that treatment). In light of the scenario describe above, possibly they feel that as-is the tooth represents low-risk for the 3-week period.
While we don’t know your situation, but especially considering that your dentist seems to feel that it is appropriate, a 3-week wait doesn’t seen unreasonable and probably (almost certainly) lies within what frequently occurs (with initial treatment, when needed, from your dentist as discussed above).
The only research paper that we could find that specifically discussed the issue of waiting periods for an endodontist’s attention involved the situation were few endodontists were available. In that case, and while no doubt not ideal, a substantial number of cases were being managed during a 30 to 90-plus day waiting period.
While no one could know for certain (without having some historic of x-rays, or your having first noticed the sinus tract at some point previously), most dentists would probably guess that the additional 3-week period while your tooth is associated with infection is short compared to the length of time the tooth’s original endodontic problems first started.
The larger question to us would be who can best treat your tooth. We’re not so sure that by their recommendation that your dentist isn’t implying that an endodontist might make the better choice.
Staff Dentist
