Looking for information about other Dental Topics?
Full Website Index• Animated-Teeth.com •
Coronal leakage – A cause of root canal treatment failure.
Guide to Coronal Leakage.
The cause of root canal failure that you’ve never heard about.
The long-term success of endodontic therapy depends on the final restoration placed following treatment and its ability to create and maintain a durable, impermeable seal. This seal protects the tooth’s interior and completed root canal work from recontamination.
When this critical requirement is not met, a condition called “coronal leakage” develops. This complication results from bacteria and debris seeping past the tooth’s restoration, whether a crown or filling, causing reinfection of the tooth’s root canal space.
This guide examines this often often-overlooked but significant cause of root canal treatment failure. It discusses the conditions that enable coronal leakage, the risks it poses to treated teeth, practical steps for prevention, and possible treatment solutions.
Coronal leakage: What is it?
Dentists, and especially endodontists, have increasingly become aware of a problematic phenomenon that takes place with root-canalled teeth termed “coronal leakage.”
It involves a situation where oral fluids (along with the bacteria and debris they contain) find a way of leaking into and subsequently recontaminating and infecting the interior of a tooth that has previously had root canal therapy.
Why is this a problem?
The biological implications of coronal leakage are root canal treatment failure and dealing with the complications/symptoms that may accompany it (pain/swelling). Once it has occurred, the tooth will require endodontic retreatment to (once again) clean, disinfect, and then seal The procedure. the tooth’s root canal system.
How is coronal leakage prevented?
As this page explains, it’s prevented by way of …
- Placing an appropriate final dental restoration for a tooth promptly after its root canal work has been completed. One that can create an adequate seal for its work. (Frequently a permanent crown is required, in some cases, a filling may suffice. See below.)
- Monitoring the restoration (and your tooth) over the long term and replacing it if evidence appears that its seal has deteriorated or been compromised.
This page’s highlights as a video –
Subscribe to our YouTube channel.
Note: Dental-Picture-Show’s content and videos have now been absorbed into Animated-Teeth.com.
A description of the coronal leakage phenomenon.
Background.
One major goal of performing root canal therapy is eliminating bacteria and other contaminants from within the tooth’s nerve space. Why? | How?
What takes place when coronal leakage occurs.
Imagine a situation where a tooth’s endodontic treatment has been successful in accomplishing this task. But, over time, the same kinds of contaminants that were originally responsible for its problems (like bacteria and the by-products they create) once again find a way of seeping back into its nerve space (pulp chamber and root canals).
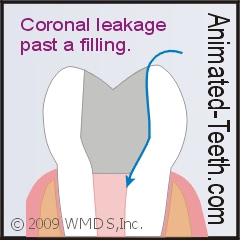
If the filling’s seal is compromised, bacteria can recolonize the tooth’s root canal system.
- The leakage may take place through a frank opening in the tooth or its filling. (Possibly some type of breakage has occurred.)
- Just as likely, what takes place may be microleakage. With this situation, the seal between the tooth and its restoration (the restoration margins) has broken down and as a result a microscopic pathway now exists into the tooth’s interior.
The problem.
Once bacterial penetration into the tooth’s root canal system has occurred, conditions inside the tooth will revert back to those that existed before its initial endodontic therapy was performed. The tooth’s previously successful work must now be considered failed root canal treatment. (Symptoms to look for.)
The fix.
Only a few treatment solutions exist. The tooth must either have conventional root canal retreatment (or possibly endodontic surgery/apicoectomy) or else tooth extraction will be required. (For more information about these options, use this link: Endodontic retreatment How successful is this? )
And that’s exactly what coronal leakage is.
Coronal leakage is a phenomenon where debris and bacteria have found a way to seep from the patient’s oral cavity, past an endodontically treated tooth’s dental restoration, and ultimately penetrate into and recontaminate and infect its pulpal space (root canal system).
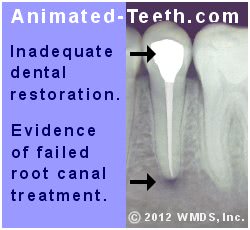
Bacteria seeping past this tooth’s defective filling has caused its root canal treatment to fail.
The term “coronal” refers to the fact that the seepage occurs through the “crown” portion of the tooth. (The part of the tooth that’s visible above the gum line.) The tooth has lost the “coronal seal” its restoration was intended to provide.
Your tooth may sustain additional damage.
Beyond just the failure of its root canal treatment, when coronal leakage occurs your tooth may suffer additional consequences.
Recurrent decay.
The accumulation of bacteria inside your tooth, especially over the longer term, can result in the formation of tooth decay. If this condition is not discovered early on (which is possible if no discernable symptoms have formed), it may cause significant tooth damage.
Research findings about coronal leakage.
While the concept of coronal leakage has been known for over 100 years, it’s only since the 1990s that it has received widespread attention and study.
a) How often does it occur?
Nowadays it’s considered a significant factor in causing root canal failure. For example, a study by Hoen evaluated 337 failed endodontic cases and determined that 13% of them involved complications with coronal leakage.
However, with any one case, coronal leakage may be only one factor of several that are involved. Here’s an explanation.
A study by Gillen applied statistical analysis to data collected from published research. The findings of the report were:
- Teeth having both adequate-quality endodontic therapy and final dental restorations had a 2.8 greater success rate than teeth having adequate treatment and inadequate restorations. (Inadequate restorations allow coronal leakage to occur.)
- Teeth having both adequate-quality endodontic therapy and final dental restorations had a 2.7 greater success rate than teeth having inadequate treatment and adequate restorations.
Together, these findings imply that:
- Placing a suitable restoration can play an important role in protecting the outcome of a tooth’s therapy.
- But a well-sealing restoration alone can’t overcome problems created by low-quality endodontic work.
That conclusion isn’t necessarily surprising. But it does reinforce the fact that each and every step of a tooth’s treatment is important and interrelated.
▲ Section references – Hoen, Gillen
b) How quickly can coronal leakage occur?
Although a tooth’s root canal system does receive an “endodontic” seal during its procedure (by way of the dentist compacting gutta-percha inside the tooth How this is done.), the integrity of this seal isn’t able to resist the continued assault of contaminants that takes place when coronal leakage occurs.
Research findings.
- A study by Torabinejad determined that the recontamination of a tooth’s entire root canal system may occur in as little as 2.5 to 6 weeks.
- A more recent study by Eliyas found that bacteria can physically recolonize the full length of a tooth’s sealed root canal system in as little as a few days.
Even worse, this same study determined that endotoxins, irritating chemical compounds produced by bacteria, can cause contamination of the tooth’s root canal space even more quickly than the microorganisms themselves.
▲ Section references – Torabinejad, Eliyas
Understanding how concerns about coronal leakage might affect your tooth’s treatment timing and planning.
A) Coronal leakage as it pertains to temporary dental restorations:
Once your root canal therapy has been completed, your dentist will need to place some type of temporary restoration that will create a seal that protects your tooth’s work until that point in time when a permanent one can be placed.
They have a lot of temporary restorative materials to choose from like glass ionomer cement, traditional dental cement, resin-based materials, and proprietary restoratives.
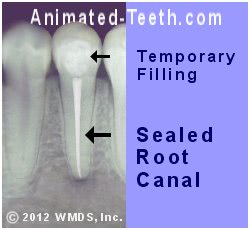
Replacing a temporary filling promptly helps to protect your root canal work.
Exactly what kind of temporary restorative is placed isn’t as important as your understanding of the interim/nonpermanent nature of this filling and being aware of the time period over which it can be expected to maintain its seal without concerns about it deteriorating and leaking. You’ll need to ask your dentist for details but it may be as little as 3 weeks. (AAE)
FYI: This detail is important to know in case scheduling difficulties crop up and your original treatment plans must be delayed.
B) Coronal leakage as it pertains to permanent dental restorations:
Generally speaking, following the completion of your tooth’s endodontic therapy, you must not delay. Your tooth’s “final” restoration should be placed as soon as is reasonably convenient. (In other words, don’t drag your feet in scheduling this procedure.)
Exactly what time period is appropriate will be based on the type of interim (temporary) restoration your dentist has placed and the time frame over which they feel they can predictably rely on the seal it creates. Strict compliance with their recommendation is important.
Needed characteristics of final restorations.
In regard to the properties that the permanent restoration that’s placed for your tooth will need to have, here’s what it must be able to accomplish:
- Be capable of creating a barrier able to prevent seepage/leakage past it.
- Be durable enough that this seal is maintained, even as the tooth functions under extreme conditions.
- Offer protection for the tooth so the seal is not compromised due to tooth fracture.
What types of restorations can meet these requirements?
After an evaluation, your dentist will make a recommendation as to what type of restoration they feel should be placed. (We discuss factors related to making this decision here: Rebuilding teeth after root canal treatment. Options.)
Generally speaking, one of three alternatives might be utilized.
1) Placing a dental crown.
Without question, the fit of a permanent crown over its tooth typically creates a superior and lasting seal. And for teeth that require strengthening/protection from fracture, placing this kind of restoration makes the right choice.

A dental crown can establish an excellent seal but not all root-canalled teeth require one.
2) Placing a filling.
Not all root canalled teeth require the protection of a crown. If after its endodontic treatment has been completed the tooth remains primarily intact, the placement of a dental filling has been shown to create an adequate seal. (Eliyas 2015)
Composite resin (dental bonding, a white filling) or else dental amalgam (metal or silver filling) are the most common materials used.
For the most part, the kinds of teeth that can meet the needed conditions for a filling are those that before their endodontic treatment had no or just a very small dental restoration, and no significant damage from tooth decay or breakage.
3) Patch the tooth’s existing crown.
In the case where a tooth’s root canal work has been performed through an opening drilled through its existing permanent crown Explained, it may be possible that a satisfactory seal can be created by filling the tooth’s access cavity with dental restorative (amalgam or bonding).
Which type of restoration makes the best choice for preventing coronal leakage?
In terms of creating a predictable and lasting seal for a tooth that will help to ensure its treatment’s long-term success, there is no question that placing a brand-new dental crown following a tooth’s endodontic therapy makes an excellent choice, especially in the case of molars.
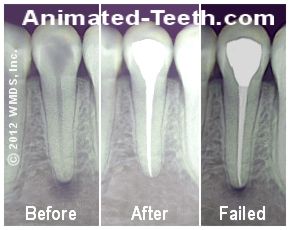
Coronal leakage due to an inadequate final restoration (a filling in this case) could explain this case’s treatment failure.
But this procedure may be judged too aggressive (in terms of the amount of tooth structure lost) for teeth that don’t otherwise require the benefits that a crown can provide (see “rebuilding” link above). If so, placing a filling may be considered appropriate.
Choosing to patch the hole in an existing crown (through which the tooth’s root canal treatment has been performed) with a filling makes the least predictable choice. We explain the reasons why here. Pros / Cons
What symptoms can you expect with coronal leakage?
Once seepage into your tooth’s root canal system has occurred, you have the potential to experience any of the wide range of symptoms normally associated with endodontic infection.
Common symptoms.
- Tooth sensitivity or discomfort. – Intermittent or persistent pain, either triggered or spontaneous. Throbbing pain. Sensitivity to pressure (like biting on the tooth).
- Tooth abscess. – The presence of swelling (intermittent or persistent). Development of a pus pimple (gum boil) next to your tooth (formally termed a fistulous tract).
- Additional symptoms of tooth infection. – Noticing a bad taste in your mouth or having a bad breath odor.
FYI: This link covers the topic of failed root canal symptoms What to look for. in greater detail.
How do you know if your root canal is leaking?
Other than noticing some of the symptoms mentioned above, there’s really no way for you to know that a problem exists.
If you do notice signs that your tooth or its filling has deteriorated or broken (possibly a change you see or feel with your tongue), you should let your dentist know because these kinds of events may allow seepage. Even if your dentist can’t document that they have, the changes that have occurred may be reason enough for them to suggest upgrading or replacing your tooth’s current (deteriorating) restoration.
What’s next?
We have lots more information about difficulties with root-canalled teeth.
Last reviewed: January 22, 2025
Author: Paul Cotner, DMD — retired dentist.
Published by: WMDS, Inc. — owner of Animated-Teeth.com.
Educational information only — not a substitute for professional dental care.
Page references sources:
American Association of Endodontists (AAE). Coronal Leakage.
Eliyas S, et al. Restoration of the root canal treated tooth.
Gillen B. et al. Impact of the Quality of Coronal Restoration versus the Quality of Root Canal Fillings on Success of Root Canal Treatment: A Systematic Review and Meta-analysis.
Hoen MM, et al. Contemporary Endodontic Retreatments: An Analysis based on Clinical Treatment Findings.
Torabinejad M. et al. In vitro bacterial penetration of coronally unsealed endodontically treated teeth.
